Abstract
Background: General surgery in Canada varies from single system subspecialty practice in large centres to multisystem broad-based practice in smaller communities. We have attempted to determine whether Canadian training programs in general surgery are appropriate for these varied practices.
Methods: A questionnaire was circulated to members of the Canadian Association of General Surgeons to collect demographic data and information about community size and patterns of practice. We also sought the source of training for general surgical subspecialties and other surgical specialties if applicable.
Results: Surgeons in smaller communities performed significantly more subspecialty and other specialty surgical practice than do surgeons in larger communities. Much of the training for this practice comes not from the primary fellowship but from senior colleagues in the community. Surgeons in smaller communities feel less well prepared than their colleagues in larger communities and are less likely to take additional fellowship training.
Conclusion: These results have important implications for surgical educators and manpower planners.
The practice of general surgery in Canada varies widely: according to the size of the community, availability of other surgical specialists, the training and interests of community practitioners, available resources and the particular needs of individual communities. Most of the training of Canadian general surgeons takes place in university tertiary care centres. University general surgeons tend to confine their elective surgery to a relatively narrow subspecialty field. It would certainly be very uncommon for a university surgeon to practise in other surgical specialties such as plastic surgery, orthopedic surgery or urology. On the other hand, surgeons in smaller nonuniversity centres are frequently called on to deal with surgical problems that are usually managed by other surgical specialists or subspecialists.
We undertook this study in an attempt to determine patterns of practice relative to community size and whether Canadian surgical training programs prepared their trainees adequately for their current practices.
Methods
The Canadian Association of General Surgeons (CAGS), a national organization representing a wide spectrum of general surgeons in Canada, has approximately 1300 members in every province. They issue a biannual newsletter containing items of interest to its membership.
In the winter edition of 2002, a questionnaire was circulated with the newsletter to the full membership. It contained questions on the following:
demographic information, including age, gender, community size, practice type, call pattern
the country and university of training
whether the surgeon had post-fellowship training
procedures performed in other specialties such as plastic surgery, obstetrics and gynecology, orthopedic surgery and urology
procedures performed in the general surgical subspecialties of head and neck, vascular and thoracic surgery
the places of training for practice in these other specialties or subspecialties (i.e., in the primary fellowship, taught by a senior colleague, self taught, course or preceptorship and other)
how well the primary fellowship prepared surgeons for their current practice on a 5-point Likert scale.
The questionnaire also gave respondents the opportunity to provide open-ended comments.
Statistical analysis was performed with use of the SPSS-11 program employing cross tabulation and χ2 analysis. A p value of less than 0.05 was considered significant.
Results
Of the approximately 1300 questionnaires circulated, exactly 250 (approximately 19.2%) (207 men, 43 women) responded by the cut-off date.
Demographic data
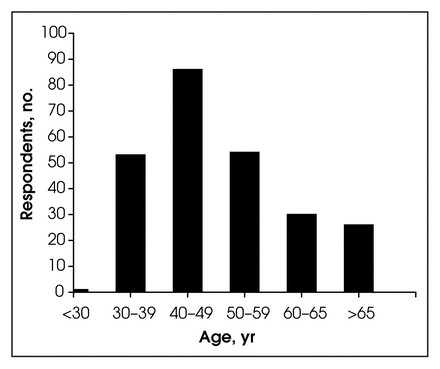
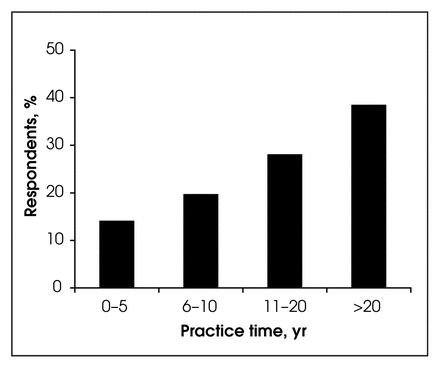
The highest number of respondents were in the 40–49 year age group (Fig. 1), and almost 40% had been in practice for more than 20 years - (Fig. 1). Almost two-thirds of respondents practised in communities with a population greater than 100 000 (Table 1), 12.6% in communities of 50 000–100 000 people, and 22.2% in communities of less than 50 000 people. Because of small group numbers, communities of less than 50 000 people were combined for the purposes of analysis. Of the 250 respondents, 184 (73.6%) practised in a group setting within the same community and 56 (22.4%) were in a solo practice (the remaining 10 did not submit a response).
Age distribution.
Demographic characteristics of questionnaire respondents*
Location of training
Over 90% of respondents received their surgical training in Canada (Table 1).
Post-fellowship training
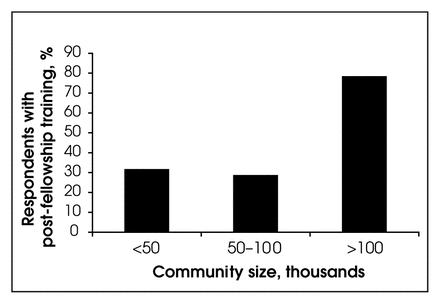
Of the 240 surgeons who responded to this question, 148 (61.7%) had trained beyond their basic Canadian fellowship (Table 1). However, when analyzed by size of community, 126 (78.2%) of 161 respondents from the communities of over 100 000 obtained post-fellowship training. In communities of less than 50 000 and between 50 000 and 100 000, 17 (30.9%) and 9 (29.0%) respectively obtained post-fellowship training (p < 0.001) (Fig. 3).
Years in practice.
Size of community in which those who had post-fellowship training practised (n = 240).
Other specialty practice
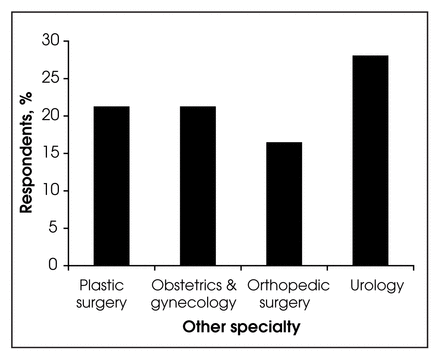
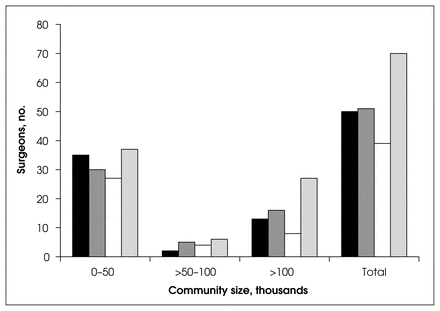
Approximately 20% of overall respondents performed some procedures in plastic surgery or obstetrics and gynecology. Of 248 who responded, 39 (15.7%) performed orthopedic surgery; and 70 (28.23%) performed some urologic procedures (Fig. 4). However, when broken down by size of community (Fig. 5), the majority of this other surgical practice took place in communities of less than 50 000, and this difference was statistically significant (p < 0.001) for all specialties.
Rate of other specialty practice.
Size of community according to surgical specialties other than general surgery. p < 0.001 for all specialties. Black = plastic surgery, dark grey = obstetrics and gynecology, white = orthopedic surgery, light grey = urology.
Subspecialty practice
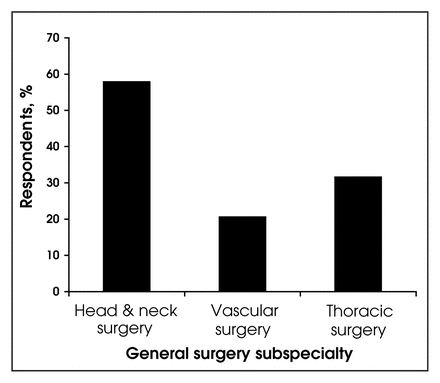
Of the 250 respondents, 143 (57.2%) performed some head and neck surgery, 51 (20.4%) performed vascular surgery and 78 (31.2%) performed some form of thoracic surgery (Fig. 6). Once again, the size of community influenced the rate of subspecialty practice, with a higher rate of vascular and thoracic surgery in the intermediate-size communities with a population of between 50 000 and 100 000 (Fig. 7). This may reflect the fact that intermediate-size communities provide regional referral services in these subspecialties.
Rates of general surgery subspecialty practice.
Size of community according to general surgery subspecialty practice. p values for subspecialties are as follows: head and neck surgery (black bars) <0.001, vascular surgery (white bars) <0.007, thoracic surgery (grey bars) <0.009.
Sources of training
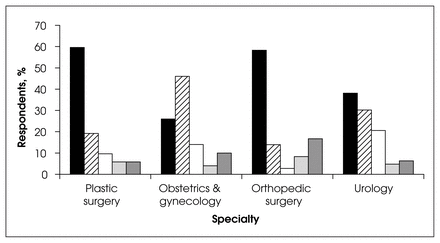
Of the other surgical specialties, the primary fellowship provided training for almost 60% of those practising plastic or orthopedic surgery (Fig. 8). For obstetrics and gynecology, the most important source of training was from a senior colleague; 46% of those practising received the training from a senior colleague in the community. For urology, 38.1% stated they received their training during the primary fellowship and 30.2% from senior colleagues (Fig. 8).
Sources of training for other specialties. Black = fellowship training, diagonal lines = senior colleague training, white = self trained, light grey = course or preceptor training, dark grey = other training.
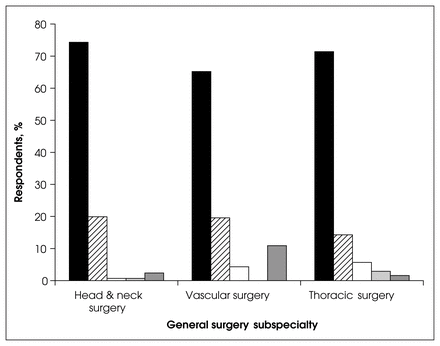
For general surgical subspecialties, the primary fellowship provided the surgical training for head and neck surgery in 74.3%, for vascular surgery in 65.2% and for thoracic surgery in 71.4% (Fig. 9). However, a significant proportion of respondents practising in the subspecialty areas (14%–20%) received their training from senior colleagues.
Sources of training in the subspecialties of head and neck surgery, vascular surgery and thoracic surgery. Black = fellowship training, diagonal lines = senior colleague training, white = self trained, light grey = course or preceptor training, dark grey = other training.
Preparedness for practice following primary fellowship
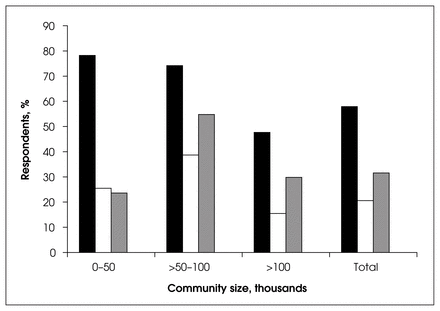
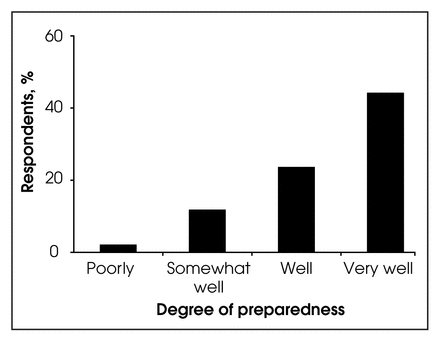
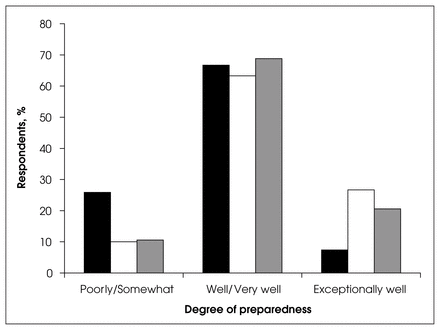
Overall Canadian general surgeons felt they were well prepared by their basic fellowship training. Over 86% indicated they were well, very well or exceptionally well prepared for their current practice (Fig. 10). However, looking at preparedness versus community size (Fig. 11), we found that respondents from communities of less than 50 000 people were much more likely to indicate that they were only poorly or somewhat well prepared for their current practice (25.9%) compared with those in communities with a population greater than 100 000 (10.6%). This difference was statistically significant (p < 0.015). (There was no significant difference in degree of preparedness in relation to age of the respondents.) The approximately 20% response rate is a potential criticism, although 250 surgeons provides a reasonable sample.
Opinions of respondents with respect to how the primary fellowship prepared them for practice.
Preparedness for practice according to community size. Black = <50 000, white = >50 000–100 000, grey = >100 000.
Discussion
This study has some limitations. It may be that those who feel less comfortable with their current practice are more likely to respond to the questionnaire, thus biasing the result. Not all general surgeons are members of CAGS, although the CAGS membership includes the majority of certified specialists in most provinces. There is also significant interprovincial variation in patterns of rural and regional care. For example, in Western and Northern Canada a significant volume of surgical care is still provided by general practitioners1 and noncertified foreign-trained surgeons who would not be members of CAGS. Nevertheless the data from this study indicates that a significant number of Canadian-trained general surgeons provide subspecialty and other surgical specialty services, particularly in smaller communities. Many of these community surgeons were not adequately prepared for their current practice by their primary fellowship programs and acquired the necessary skills in the community. Although they have broader and more varied practices than their urban counterparts, the respondents from smaller communities were significantly less likely to take additional fellowship training. They were also more likely to feel less than well prepared by their primary fellowship for their current practice.
Any discussion of nonurban surgery for Canadians begs the question: What is the optimum model for surgical care in rural and regional Canada? Some would argue that the best solution is to regionalize all surgical care. This would allow everyone to be treated by appropriately trained specialists or subspecialists who had sufficient volumes of cases to ensure competence. Certainly there is compelling evidence that, at least for certain complex cases, there is a clear volume–outcome relationship.2,3 The information for other common types of surgery is either lacking or unclear, but there is certainly a concern that hospitals or practitioners with very small volumes are unlikely to provide as good results as high-volume centres or surgeons.4
Others may advocate a more decentralized model in which at least some basic surgical care is provided in small, rural hospitals, often by general practitioners. Although CAGS has endorsed add-on surgical skills for family practice, including minor surgery and the resuscitation of the critically ill and injured, the organization has opposed cavitary surgery by anyone other than certified surgeons.5
There is a considerable body of evidence that demonstrates an inadequate supply of general surgeons to meet current attrition rates.6–8 There is diminishing interest in general surgery as a career, related mainly to the associated poor lifestyle.9 All these factors will favour the development of regional centres with concentrated services.
Given our vast geographic area and varying political climate, it is unlikely that we will develop in Canada a “one size fits all” model of regional surgical care delivery. Community needs will continue to vary by size, availability of other specialists and proximity to larger regional and tertiary centres. Surgical skill sets may need to be tailored to those of individual communities and may cross traditional specialty and subspecialty lines. Certainly the data from this study indicate that this is the case. It would seem reasonable to suggest that if Canadian-trained surgeons are going to provide broad surgical services in small- and medium-size communities they should be provided with the necessary skills to address community needs within their formal training programs. This concept is in keeping with the increasing demand that medical schools have a sense of social accountability that responds to the needs of the communities served.
If we accept that we need more general surgeons with broader skills to serve rural and regional communities the next obvious question is: How do we design an appropriate curriculum? Other countries, particularly those with broad geographic areas similar to ours, including the United States, Australia and South Africa, have grappled with this question. 10–13 Suggestions have varied from a year of training in a rural centre within the structure of a general surgery program to a 2-year post-fellowship training position.
No single fixed model is likely to be successful, and we would suggest that one of the characteristics of rural training programs must be that they are sufficiently flexible to adapt to community needs. The curriculum should provide not only the appropriate content (e.g., senior level rotations in specific specialties or subspecialties), but also they must provide the appropriate context. At least some of the training should take place in rural and regional communities if we are to convince residents that this is a legitimate and valued career option.
Specific objectives need to be developed that define what is appropriate for a community based generalist and what should be referred to the traditional specialist (e.g., in orthopedics the generalist might perform closed reductions and some defined open procedures but would refer total joint replacements).
The level of training should be sufficiently advanced to allow residents to become technically competent in specific procedures as defined by the objectives. It should be at the senior resident level or as part of specifically and objectively defined post-fellowship training.
If community or surgeons’ needs change over time there should be an opportunity for defined “fellowships” or mini-sabbaticals (ranging from weeks to months), which would allow community surgeons to acquire new skills in an academic environment.
Finally, opportunities should be created for continuing professional development of community surgeons. This must recognize the unique broad nature of their practice. Ultimately community surgery should be recognized as a distinct subspecialty, which requires a breadth of surgical skills rather than the depth of practice of focused subspecialists found in university centres. Recognition and support of this subspecialty will enable them to acquire and maintain skills that cross a broad range of traditional surgical specialties and subspecialties.
Conclusions
Canadian-trained general surgeons provide a broad range of surgical services, particularly in smaller, nonuniversity centres. Canadian training programs frequently fail to prepare their residents for this type of practice. The challenge to Canadian universities is to provide programs with the following characteristics: they should be flexible and responsive to community needs; they should provide not only appropriate objective-based content but must promote the context of rural and community surgery; the training should be at an appropriate senior residency or post-fellowship level; continuing professional development opportunities should be available appropriate to the recognition of community surgery as a distinct subspecialty with varied cross-specialty needs.
Footnotes
Presented at the annual meeting of the Canadian Association of General Surgeons, London, Ont., Sept. 19–22, 2002
Competing interests: None declared.
- Accepted April 2, 2004.