Abstract
Objective: To assess the hypothesis that empyema thoracis (ET) is a problem often not optimally treated. Long delays in diagnosis are common, long hospital stays are typical and recovery with surgery is relatively rapid.
Design: A chart review.
Setting: The Regina Health District associated hospitals, a tertiary referral centre.
Patients: The charts of 34 consecutive patients having primary respiratory tract disease and seen during the 6-year period Apr. 1, 1991, to Mar. 31, 1997, were identified.
Outcome measures: Patient presentation, time until diagnosis of ET, number of radiologic investigations, microbiologic features, treatment methods, postoperative course and mortality.
Results: The mean delay in diagnosis, defined as the time of admission to the time of correct diagnosis, was 44.2 days (range from 0 to 573 days) and the mean delay until thoracic surgery referral was 47.4 days (range from 0 to 578 days). On average each patient underwent CT 10.1 times, had 2.6 percutaneous drainage procedures and 2.0 chest tube insertions. The mean time from the first percutaneous chest drainage to the date of diagnosis was 29.8 days (range from 0 to 564 days). Of the 26 patients who underwent CT, the mean time from the first CT of the chest to the date of diagnosis was 9.5 days (range from 0 to 75 days). Cultures of pleural fluid grew no organisms in 17 patients; in the remaining 17 patients cultures grew 23 different microorganisms. Of 26 patients who were referred for surgical opinion, 18 underwent decortication; 8 were not considered to be surgical candidates. Pathological examination showed 17 cases of inflammatory empyema and 1 case of mesothelioma (unrecognized clinically). The mean length of hospital stay postoperatively was 15.2 days.
Conclusions: Early suspicion of ET facilitates its treatment, resulting in fewer investigations and shorter hospital stays. When percutaneous drainage does not eliminate pleural effusions, empyema must be considered. Recovery from surgical decortication is rapid in comparison with the typical protracted preoperative hospital course.
Empyema thoracis (ET) is a problem that has been recognized by physicians for centuries.1 Although several mechanisms can result in an ET, including trauma, esophageal disease or iatrogenic injury, an infected parapneumonic effusion is the commonest cause.2–5 Resulting problems include decreased pulmonary function and the local and systemic sequelae of active, ongoing infection.
The presentation of empyema can vary from nonspecific, constitutional symptoms to fulminant sepsis. This fact, along with a lack of awareness, can make the diagnosis of ET difficult. There are typically long delays in diagnosis, resulting in multiple, redundant investigations and procedures and, hence, a delay in treatment. 2,6,7
Aggressive therapy is necessary to manage the advanced stages of ET. The ultimate aim of therapy is to control sepsis while maximizing pulmonary function. Once the empyema becomes organized, percutaneous drainage techniques and systemic antibiotics are ineffective. Late referral to a thoracic surgery unit, common in patients with an organizing empyema experience, lengthens hospital stays and, more importantly, increases the risk of complications.2,7
Method
This study was a case review over a 6-year period (Apr. 1, 1991, to Mar. 31, 1997) at the Regina Health District associated hospitals. The Regina Health District serves as the tertiary referral centre for a population of approximately 500 000. A total of 54 cases of ET were identified. Of these, 20 were excluded because they were of traumatic, esophageal or iatrogenic origin. Data collected from the remaining 34 cases included demographics, presenting symptoms, important dates (date of admission, correct diagnosis, surgical procedure, discharge), radiologic investigations, microbiologic features, antibiotic therapy and surgery.
The delay in diagnosis was defined as the interval between the date of diagnosis of pleural effusions and the date of diagnosis of ET. The delay to the time surgical consultation was sought was defined as the period between the date of diagnosis of pleural effusions and the date when surgical consultation was first considered. The time from the first percutaneous chest drainage to the date of diagnosis as well as the time from initial chest computed tomography to the date of diagnosis are both self-explanatory. Nonsurgical patients were defined as those who were never referred to the surgical unit or who were assessed and considered to be inappropriate surgical candidates due to severe, life-threatening concomitant cardiopulmonary disease, uncontrolled neoplasm or dementia. The length of postoperative hospital stay was defined as the period between the date of surgery (decortication) and the date of discharge or the date of death. An inhospital death was considered to be death within 30 days of operation.
Patients
The patients were referred from within the Regina Health District or from surrounding rural centres. Referrals were made from primary, secondary and tertiary levels. Diagnosis was made from symptoms, signs and radiologic examination, and in many cases was confirmed by percutaneous drainage. Pathology reports from surgical specimens confirmed the diagnosis.
Individual patients experienced a wide variety of investigative procedures and diagnostic tests. Patients with a long delays in diagnosis tended to have more diagnostic and therapeutic interventions. Postoperatively, patients were either discharged home or to their local hospital.
Results
Thirty-four patients were identified with empyema from a primary respiratory tract infection. They ranged in age from 29 to 94 years (mean 62.3 years). Twenty-five (74%) were male. Only 13 (38%) patients did not have a smoking history. Common presenting symptoms were cough, chest pain, dyspnea and pyrexia (Table 1).
Presenting Symptoms in 34 Patients Suffering From Empyema Thoracis
Six (18%) patients initially presented to a primary care physician, 13 (38%) to a secondary care centre and 15 (44%) to a tertiary care centre. For those who presented first to primary care, there was a mean delay to the correct diagnosis of 169 days, compared with 16 days for secondary care and 19 for tertiary care (Table 2). When the initial presentation was to primary care, the mean delay before a surgical consultation was sought was 147 days.
Level of Health Care in Relation to Initial Presentation and Delayed Diagnosis in Patients With Empyema Thoracis
The delay in diagnosis ranged from 0 to 573 days (mean 44.2 days). Patients were hospitalized for the duration of the delay. The delay to the time when a surgical consultation was sought ranged from 0 to 578 days (mean 47.4 days). Numerous diagnostic and therapeutic procedures, including chest radiography, chest computed tomography information radiologically guided tube and chest tube insertions, were carried out (Table 3). The mean time from the first percutaneous chest drainage to the date of diagnosis was 29.8 days (range from 0 to 564 days). Of the 26 patients who underwent CT, the mean time from the first chest CT to the date of diagnosis was 9.5 days (range from 0 to 75 days).
Radiologic Procedures Done and Chest Tubes inserted Before the Correct Diagnosis Is Reached in Patients Having Empyema Thoracis
Twenty-six patients were referred for surgical opinion: of these, 18 were considered suitable for decortication; 8 were considered to be unsuitable surgical candidates. For the surgical patients, the mean time to the correct diagnosis was 55.7 days. Eighteen patients underwent decortication, 3 (17%) of them in the intensive care unit preoperatively. Intraoperative blood loss was recorded for 13 of the cases and averaged 863 mL (range from 200 to 2000 mL). Fifteen (83%) patients in the intensive care unit postoperatively had a mean stay of 5.3 days (range from 2 to 31 days). Four (27%) of them required inotropes and 7 (47%) required mechanical ventilation. The mean duration of chest tube drainage was 12.4 days. The mean length of postoperative hospital stay was 15.2 days. One patient (6%) had a wound infection. Pathological examination of the surgical specimens confirmed 17 cases of inflammatory empyema and 1 case of mesothelioma.
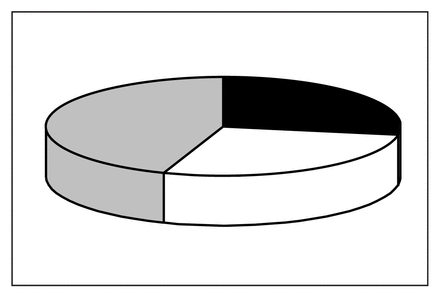
Microbiologic examination revealed a diverse group of organisms (Fig. 1, Table 4). Unlike the preantibiotic era when Streptococcus pneumoniae was the predominating organism, an extensive number appear to be involved in empyema.8
Distribution of culture findings from patients who underwent decortication for empyema thoracis. Black = culture negative, white = single organism, shaded = polymicrobial.
Organisms Grown From Culture Specimens of Pleural Fluid Aspirate or Operative Specimen in 34 Patients Having Empyema Thoracis
Of the 18 patients who underwent decortication, 2 (11%) died in hospital, 1 of empyema and 1 of mesothelioma. There were 4 confirmed deaths (50%) in the 8 patients judged unsuitable for surgery (2 of uncontrolled sepsis), and there were 2 confirmed deaths (25%) from sepsis in the group of 8 who were never referred for a thoracic surgery opinion.
Discussion
This study focused on parapneumonic ET. ET related to esophageal rupture and perforation, trauma and iatrogenic injury were eliminated because ET secondary to these causes is comparatively easy to detect and typically does not result in the same delay in diagnosis as in patients with parapneumonic empyema.
Although ET is relatively common and is associated with a significant morbidity and mortality, there appears to be a lack of awareness of the disorder. The diagnostic criteria for ET can be confused. Many different classification schemes have been designed. The majority of studies have classified ET into 3 to 7 stages.9–11 Three stages — exudative, fibropurulent and organizational — is the most common.12 All of the patients in this study were in the organizational stage.
The delays to diagnosis and surgical consultation were unacceptably long and increased morbidity, particularly as these patients were hospitalized for the duration of their diagnostic testing and subsequent treatment. This resulted in a protracted clinical course with several ramifications. Patients typically experienced an excessive number of investigations (Table 3), which did not appear to contribute to their care and potentially exposed them to risks associated with invasive procedures. Consumption of medical resources that do not positively influence patient recovery, or palliation is a consideration during these times of constrained medical care. The detrimental effect of unresolved sepsis and compromised respiratory function on quality of life, including loss of livelihood, is difficult to quantitate but is another consideration.
The lack of awareness was not apparent at just 1 but at all 3 levels of health care in Saskatchewan (Table 2). It appears that patients from secondary or tertiary care environments are less frequently referred to a thoracic surgery service. This may be because of a growing tendency to treat empyemas medically and a reluctance in seeking surgical consultation.13
In this study, the diagnosis was based on blood determinations, chest radiography and CT. Thoracentesis could have been helpful to distinguish a simple pleural effusion from a loculated, fibrous empyema. We suggest that if thoracentesis fails to drain the pleural effusion completely, a repeat tap should not be performed but rather further imaging by CT should be done to better visualize the thoracic cavity. Some studies suggest diagnosis and treatment of ET according to the biochemical analysis of pleural fluid aspirates. 11,12,14,15 In this study population, fluid analysis was not useful; biochemical results did not change the management of these patients. The long delay in diagnosis may have allowed cases of early stage pleural sepsis to proceed to an organizing stage. However, there are no data to support this. There are no widely accepted biochemical definitions of empyema, with different authors having different criteria.16–18 The relatively short length of time between the initial CT and the date of diagnosis supports the use of chest CT, which can easily reveal a multiloculated mass indicative of ET.
The goal of treatment is to control sepsis while maximizing pulmonary function. Early chest tube placement is important to establish a route for drainage19 but often is not a definitive measure. The treatment of choice is a highly debated issue; however, the definitive treatment for a thick fibrous pleural peel that is trapping underlying lung is decortication. 3,9,20–23 Thoracoscopic treatment has been promoted as a successful, noninvasive treatment for empyema; however, chronic, organized empyemas, as experienced in the Regina Health District, appeared to be unsuitable for a thoracoscopic approach. Thoracoscopy may be an option for early stage disease.
In regard to the surgical patients, there was a relatively short postoperative recovery period compared with the prolonged preoperative clinical course. The death rate for surgical patients was 11%, for those never referred was 25% and of those who declined surgery was 50%. Despite the small number and retrospective study design, the data from this study suggest a trend that in multiloculated empyema, nonsurgical treatment results in higher death rates. The data are “soft” but confirm a previous notion that early surgical intervention is the optimal treatment for multiloculated empyema.24
Of the nonsurgical patients, 10 were lost to follow-up. Considerable effort was made to locate and determine the disposition of these patients. Attempts were made to locate them through hospital records, the local health districts, and the Saskatchewan Ministry of Health from medical billing records. The constant flux of medical practitioners in Saskatchewan, worst at the primary care level, and a minimal standard of medical record-keeping appears to be responsible.
In summary, symptoms of ET include cough, dyspnea, pleuritic chest pain, general malaise and weight loss. Signs of ET include fever, decreased respiratory movement, decreased width of intercostal spaces, dullness to percussion, decreased air entry and bronchial breathing. Important investigations include a complete blood count and differential, blood cultures, chest radiography, CT with contrast, diagnostic thoracentesis and chest tube drainage.
From this study, we conclude that patients who have organized, parapneumonic empyema do indeed experience long delays in diagnosis. There appears to be a lack of awareness of the disorder, particularly at the primary care level; however, this is also present at the other levels of medical care. Patients endure multiple radiologic investigations and procedures. Long hospital stays are typical. Recovery with surgery is relatively quick compared with the protracted preoperative hospital course.
Footnotes
Presented in part at the 67th annual meeting of the Royal College of Physicians and Surgeons of Canada, Toronto, Ont., Sept. 25, 1998.
- Accepted April 12, 2000.