Boerhaave’s syndrome: postemetic esophageal rupture
Esophageal perforation secondary to the barotrauma of forceful vomiting accounts for 10% to 15% of perforations of the thoracic esophagus. 1 Typical clinical symptoms include retrosternal pain, accentuated by swallowing, and dyspnea, which can arise as the mediastinal pleura ruptures and massive effusions ensue. Acute awareness of the patient at risk for esophageal perforation and rapid diagnosis of this condition are of utmost importance because death is directly proportional to the time to definitive treatment.
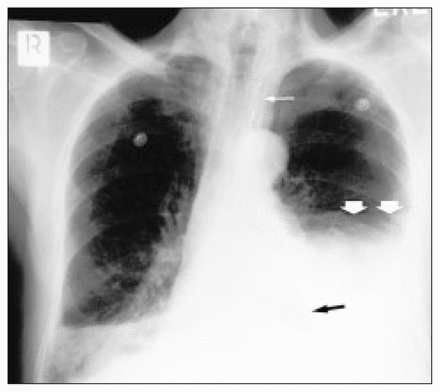
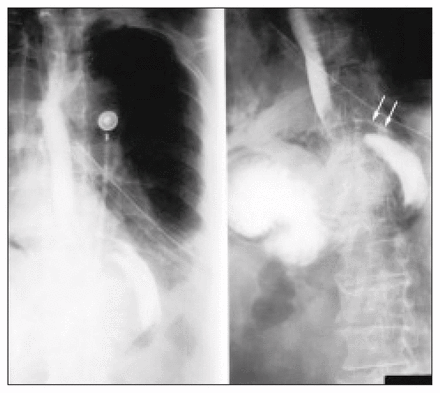
The diagnosis of thoracic esophageal perforation can be made in the majority of cases with a plain chest radiograph. Pathologic findings are present in 90% of chest radiographs obtained at presentation. In this case, chest radiography revealed a large left effusion with concurrent pneumothorax and pneumomediastinum (Fig. 1, large white arrows) in addition to a smaller right effusion. A gastric bubble is identified in the mediastinum suggestive of a hiatal hernia (Fig. 1, black arrow). In a review of cases of Boerhaave’s syndrome, common radiographic findings on plain chest x-ray films include pleural effusion with pneumothorax in 51%, pneumomediastinum in 30%, pleural effusions without pneumothorax in 25%, and pulmonary consolidation in 14%.2 However, in 12% of cases the diagnosis of esophageal perforation cannot be made from the plain radiographs and further diagnostic imaging may be required.3 A contrast esophagogram, as in this case (Fig. 2, arrows), cannot only confirm the suspected diagnosis but also provide an exact location and indicate the degree of rupture, both of which may help dictate management. Although surgical repair with wide mediastinal drainage remains the mainstay of treatment, small, well-contained perforations seen on the contrast esophagogram that drain freely back into the esophagus in patients with no signs of systemic inflammation have been successfully managed nonoperatively. 4
At thoracotomy this patient was found to have a 2-cm long linear perforation of the esophagus 2 cm proximal to the gastroesophageal junction. In addition he had a significant paraesophageal hernia with no compromise of the gastric wall. The esophageal perforation was repaired over a T-tube with wide mediastinal drainage. Elective repair of the paraesophageal hernia was delayed until after the acute septic episode had resolved.