Schwannomas (neurilemomas) are benign neurogenic tumours arising from Schwann cells of the peripheral nerve sheath. These tumours have a predilection for the head and neck, extremities and posterior mediastinum.1 Only 3% of schwannomas occur in the retroperitoneum, constituting approximately 4% of all retroperitoneal tumours.2 They occur without gender predominance in the 20- to 50-year age group and are associated with von Recklinghausen’s disease in 18% of cases.3 Malignant change is exceedingly rare; however, malignant tumours have been reported, although they are usually associated with von Recklinghausen’s disease.3,4
The cellular schwannoma is a well-recognized variant of schwannoma that, because of its cellularity, mitotic activity and occasional presence of bone destruction, is misdiagnosed as malignant in over 25% of cases.3,5 Over 100 cases of cellular schwannoma have been published, with a recurrence rate of less than 5% and no development of metastastic disease.3 These tumours have a predilection for deep structures: the paravertebral region of the retroperitoneum (32%), pelvis (21%) and mediastinum (23%).5
We describe the management of 2 patients with presacral cellular schwannoma. The diagnosis was made preoperatively from clinical and radiologic findings, and core-needle biopsy results. Despite the rarity of these tumours it is important that the diagnosis be considered preoperatively by the surgeon and the radiologist interpreting the scans, as well as the pathologist examining the core-needle biopsies. The diagnosis of this benign entity may influence further treatment by limiting surgical invasiveness and avoiding unnecessary adjuvant therapy.
Case reports
Case 1
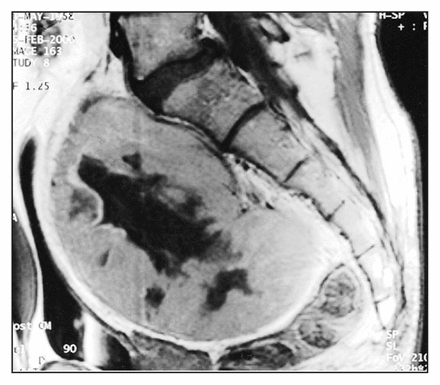
A 41-year-old man complained of low back pain for 6 months. He reported some urinary urgency but no gastrointestinal or neurologic symptoms. A large pelvic mass could be palpated. Rectal examination similarly demonstrated a large, smooth, nonmobile, retrorectal mass. There was no postanal dimple or sinus tract. No café-au-lait spots or neurofibromas were noted. Computed tomography revealed a solid, heterogeneous pelvic mass 14 × 11 × 11 cm in diameter containing small areas of calcification and having a well-defined contour. The mass extended into the right anterior sacral foramen, which was widened, but there was no bony destruction. Magnetic resonance imaging confirmed these findings (Fig. 1). A CT-guided biopsy performed at the referring hospital was inconclusive, but a transrectal core-needle biopsy under antibiotic coverage was consistent with a cellular schwannoma. Through a midline laparotomy incision, a 20 × 14 × 11 cm, well-circumscribed pelvic mass was found in contact with the sacrum. It was excised completely, sparing the right S2 nerve root from which it presumably originated. Blood loss was estimated to be 5 litres, primarily from the sacral venous plexus. The histologic appearance was that of a benign cellular schwannoma. The patient had a smooth recovery and was discharged 7 days postoperatively. There was no sign of recurrence 1-year postoperatively.
Case 1. Magnetic resonance image showing a large heterogeneous presacral mass with well-defined margins.
Case 2
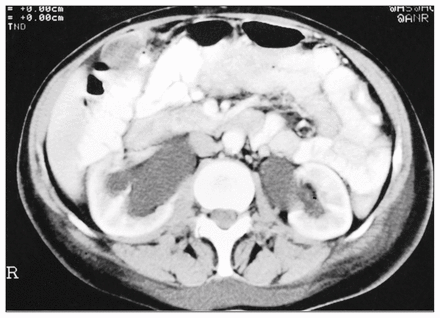
A 70-year-old woman presented with abdominal discomfort associated with a palpable abdominal mass of several months’ duration. Findings on a review of systems were negative except for right leg swelling. A large pelvic mass was palpable through the abdominal wall on vaginal and rectal examinations. A discrete left breast mass was similarly palpated. Ultrasonography revealed a pelvic mass thought to be of ovarian origin. An exploratory laparotomy revealed a large retrorectal pelvic mass. An incisional biopsy was compatible with retroperitoneal fibrosis or the wall of an inflammatory aneurysm. CT revealed bilateral hydronephrosis and a large, well-defined retrorectal tumour with a low-density centre and amorphous calcification in its wall (Fig. 2). The signal intensity of the mass on MRI was equal to abdominal muscle on T1-weighted images but higher on T2-weighted images. Angiography demonstrated important vascularization of this mass from the internal iliac arteries. The patient was referred to the Royal Marsden Hospital where a core-needle biopsy of the pelvic mass through the posterior fornix demonstrated a cellular neoplasm with cells strongly reactive for S-100 protein, consistent with a benign cellular schwannoma. At laparotomy, an encapsulated 20 × 14 × 8 cm, smooth, yellow tumour was found adherent to sacrum but without bone destruction. No nerve root was grossly evident. The tumour was completely excised. Because of profuse bleeding from the presacral veins and damage to a tributary of the right internal iliac vein, the pelvis was packed and the abdomen closed. The packs were removed 72 hours later without further bleeding. Total blood loss was 5 litres. Microscopy demonstrated an encapsulated spindle cell neoplasm with dispersed foamy macrophages, dystrophic calcifications, a mitotic count of 1 per 20 high-power fields and a strong diffuse reactivity for S-100 protein consistent with a benign cellular schwannoma (Fig. 3). Postoperatively, the patient suffered an external iliac vein thrombosis and pulmonary embolism, for which a transjugular filter was inserted and anticoagulation therapy initiated. Following her laparotomy, the patient underwent a wide local excision and axillary clearance for an invasive ductal carcinoma. She was well without any sign of recurrence 2-years after resection of the schwannoma.
Case 2. Computed tomogram with contrast showing bilateral hydronephrosis secondary to a presacral mass.
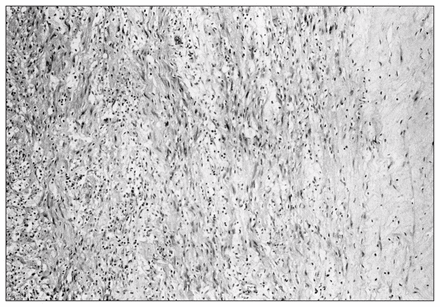
Case 2. Photomicrograph showing a cellular schwannoma consisting of wavy spindle cells and scattered foamy macrophages, with a visible capsule (right).
Discussion
In the pelvis, a schwannoma usually develops from the sympathetic system represented by the hypogastric plexus or from the spinal nerves that form the sacral plexus.6 Modes of presentation are typically nonspecific, including abdominal or pelvic pain or mass, gastrointestinal symptoms, urinary symptoms secondary to stasis, back and radicular pain. Because of their location, tumours generally reach a large size before detection.1,6 As demonstrated in our second case, bilateral hydronephrosis due to obstruction of the ureters, along with leg edema secondary to compression of the iliac vessels is also possible. The stigmata of von Recklinghausen’s disease should be sought at presentation as these patients are at increased risk for malignant peripheral nerve sheath tumours (MPNSTs). Patients may initially seek treatment from a surgeon, gynecologist or urologist, and low back pain may prompt initial evaluation by an orthopedic or neurosurgeon. An association between schwannomas and other malignant tumours has been described in up to 16% of cases; the most common cancers include skin, breast and gastrointestinal tract.7 Our second patient presented with a synchronous breast carcinoma.
Schwannomas are solid and well-circumscribed, encapsulated masses. Large schwannomas (> 8 cm) often undergo cystic degeneration due to necrosis or hemorrhage.6 Neither tumour size nor mitotic activity has been found to reflect malignant behaviour2 yet schwannomas may erode into adjacent bony structures.4 This is best described with cellular schwannomas in which atypical clinical features such as bone erosion and local recurrence may be misconstrued by the clinician or radiologist as a malignant tumour. 5 Atypical histologic features found with cellular schwannoma often suggest the diagnosis of MPNST, fibrosarcoma or leiomyosarcoma to those unfamiliar with this entity. Staining for S-100 protein is an invaluable adjunct in making the diagnosis, particularly with material from core-needle biopsy. It is rare for MPNSTs and other soft-tissue tumours to show strong, diffuse immunoreactivity for S-100 protein; such a staining pattern suggests cellular schwannoma.3 In certain cases, electron microscopy can be helpful in diagnosis.8
CT and MRI scans confirm the presence of tumour and provide valuable information about its exact anatomic location in relation to spinal roots, the sacral canal and adjacent viscera.1 There are no specific radiologic features associated with schwannomas, but the following findings are highly suggestive: a well-demarcated round or oval mass with heterogeneous contrast enhancement due to cystic and hemorrhagic changes;9 presence in the region of a known nerve ganglion or pathway; calcification and cystic change in a large tumour;10 iso- or slightly hyperintense signal intensity on T1-weighted images compared with muscle and high signal intensity on T2-weighted images.11,12 Asymmetry in size and attenuation, irregular infiltrative borders and internal heterogeneity without contrast suggest MPNST rather than schwannoma.13
The CT scans of the 2 patients described, showing a pattern of cystic degeneration and calcification within the tumour, are suggestive of pre-sacral schwannomas. They do not demonstrate the irregular borders and diffuse necrotic areas often found with soft-tissue sarcomas, nor the homogeneity and absence of cystic or hemorrhagic changes seen with other benign neurogenic tumours. According to some, MRI seems to offer better resolution and more specificity than CT and can better delineate the tumour from the adjacent anatomic structures. 12,14 Arteriography has been suggested as part of the standard preoperative work-up because of the hypervascularity of schwannomas and the possibility of preoperative embolization. 4,6 We do not perform preoperative arteriography because most of the intraoperative bleeding originates from the presacral venous plexus and trauma to the surrounding vasculature, which is not significantly diminished by tumour embolization.
Core-needle biopsy provided the preoperative diagnosis in both our patients. This was true despite a negative CTguided biopsy in the first patient and a negative incisional biopsy in the second, both performed before referral to our hospital. Our success with this method is in stark contrast to all previously published reviews in which core-needle biopsy is discouraged.1,4,11 The reasons cited include the high rate of inconclusive results, the potential for diagnosis of a malignant neoplasm leading to more aggressive and potentially harmful treatment, and complications such as infection or hemorrhage from a hypervascular tumour.15 Tumour dissemination in the case of a malignant tumour also remains a theoretic possibility. Laparotomy and frozen-section have, therefore, been recommended as the diagnostic procedure of choice.4,11,16 In the context of an exploratory laparotomy as in our case 2, an erroneous diagnosis might have been avoided with a deeper incision through the thick capsule in order to obtain representative tissue. However, we feel that there are several advantages to performing a core-needle biopsy preoperatively in patients with probable schwannomas based on clinical and radiologic findings. The advantages include the exclusion of other conditions such as lymphoma, metastases and primitive neuroectodermal tumours, requiring nonsurgical therapy, the possibility of planning a less radical operation with the diagnosis of a benign tumour, thereby saving spinal nerve roots and adjacent viscera, and easy accessibility for biopsy through vagina or rectum. A pathology department with an interest in soft-tissue tumours and the interpretation of core-needle biopsies are essential.
The extent of resection remains debated in the literature. Some authors advocate complete surgical excision that may include adjacent viscera with negative soft-tissue margins.11,17 It is their belief that malignant disease can never be excluded, and the potential for malignant transformation of retained tumour, recurrent growth and pain necessitate a more radical excision. The treatment of choice, however, is local tumour excision avoiding unnecessary sacrifice of a functionally important nerve if possible.4,7 The rationale is based on the low rate of local recurrence, even with a portion of the capsule remaining intact, and the rarity of malignant transformation found with benign schwannomas. Once bone invasion is ruled out, a transabdominal approach provides better exposure and is better tolerated by patients than a transsacral approach. Intrasacral schwannomas presenting as expansile presacral masses are optimally treated by a synchronous abdominosacral approach.16 Sufficient blood products should be made available because schwannomas are highly vascular and intraoperative blood loss may be substantial. Ligature of the vascular pedicles including the medial and lateral sacral arteries, and branches of the lumbar and internal iliac vessels has been advocated to limit blood loss;18 however, this is extremely difficult with very large tumours limiting exposure.
Although schwannomas constitute a small percentage of all pelvic tumours, physicians should be acutely aware of this condition and look for the typical features of schwannomas on CT and MRI, as well as perform core-needle biopsy to prove the diagnosis preoperatively. An awareness of the cellular schwannoma variant and the propensity for its misdiagnosis is imperative. In this way, a simple excision can be performed without wide resection with tumour-free margins, which is essential in the surgery of malignant peripheral nerve tumours and other sarcomas. Inappropriate institution of adjuvant radiotherapy and chemotherapy may also be avoided in this manner.
- Accepted June 21, 2001.