Abstract
Purpose: To compare 2 methods of fixation for maintenance of alignment during healing of valgus tibial osteotomies.
Methods: We performed a retrospective chart and radiographic review of valgus tibial osteotomy cases of staple fixation supplemented by a postoperative cast and of blade plate fixation for maintenance of femoral–tibial alignment during healing of the osteotomy.
Results: Both groups (staple- and-cast, n = 16; plate, n = 28) were similar in terms of age, preoperative alignment, extent of osteoarthritis and degree of intra-operative correction. Between-group differences in the maintenance of femoral–tibial alignment during healing were not significant. In both groups there was a strong correlation between degree of bone contact at the osteotomy site and maintenance of alignment (p < 0.005). In cases done with the plate, 90% of osteotomies with good or excellent bone contact maintained alignment during healing; with poor or fair bone contact, 75% had loss of alignment > 5° during healing. There was a trend toward a greater incidence of delayed or non-union with plate fixation compared with staple fixation that did not reach statistical significance. All of these cases of delayed/non-union had loss of femoral–tibial alignment > 5° during healing.
Conclusion: As a result of this study, we have modified our surgical technique. We now use intra-operative fluoroscopy for optimizaiton of bone contact, and we have reverted to the less invasive staple method for fixation of tibial osteotomies.
Valgus tibial osteotomy is an effective surgical procedure for medial compartment osteoarthritis of the knee in young, active patients. According to research, long-term success of an osteotomy depends on the postoperative alignment of the limb. Coventry1,2 stressed the importance of overcorrecting the mechanical axis of the limb to ≥ 5° of valgus in order to obtain good results. Several papers3–7 have reported that correction of the femoral–tibial angle to between 6° and 14° of anatomic valgus gives good or excellent results in the majority of cases. In contrast, correction to less than 5° of valgus has a high incidence of failure (63%) at 5-year follow-up.8
Staple fixation of tibial osteotomies has had good clinical success; but as a method of internal fixation, staples suffer from some theoretical drawbacks. Staple fixation depends on point concentration of force, which is not biomechanically rigid. Additional postoperative fixation, usually a cast or brace, is therefore required, which precludes physiotherapy for range of motion until it is removed.
A plate system has better strength of biomechanical fixation, which may allow for earlier weight-bearing and can allow for continuous passive motion immediately after surgery. Plate fixation also has theoretical drawbacks: the increased dissection required may have an increased risk of soft-tissue complications. The degree of risk related to peroneal nerve injury, compartment syndrome or infection from this is unknown.
The Chandler® blade plate system used in this study (Chandler, Depuy, Warsaw, Ind.) is a modification of the semitubular tension-plate methods devised by Brunner and Weber.9 It comprises a blade plate, which is inserted into the proximal tibial fragment, and 2 screws that cross the osteotomy site and provide 4 cortices of fixation in the distal fragment.
Our goal was to compare the results of blade-plate fixation with staple fixation in the maintenance of femoral–tibial alignment during the healing phase of osteotomy.
Methods
The senior author (J.P.W.) used staple fixation supplemented by a postoperative cast for 19 osteotomies from January 1990 through September 1991. Of these cases, complete preoperative, postoperative and 1-year follow-up radiographs were available for 16. Patients with staple fixation wore a long-leg cast that allowed partial weight-bearing for 6 weeks after surgery. The senior author then changed his surgical technique to use a Chandler blade plate for fixation of osteotomies, which he used in 32 sequential osteotomies from October 1991 through December 1994. These patients did not wear a postoperative cast and were allowed early range of motion and partial weight-bearing for 6 weeks. Twenty-eight knees in 25 patients of the plate group had complete preoperative, postoperative and 1-year follow-up standing radiographs.
All patients had medial compartment osteoarthritis of the knee. A transverse proximal fibular osteotomy was performed in all cases, with no use of intraoperative fluoroscopy. The surgical technique was similar for both groups: a transverse incision and laterally based closing wedge osteotomy made in the metaphyseal portion of the upper tibia. A surgical jig was not employed.
A single observer (M.M.H.) assessed all radiographs. Preoperative radiographs and those obtained 1 year after surgery were full-length standing views; the image taken immediately after surgery was a standing view centred on the knee. Preoperative images were assessed in a blinded fashion for extent of arthritis and 3 alignment variables: femoral–tibial, femoral–transcondylar and tibial plateau–tibial shaft angles. Radiographic extent of arthritis was graded according to our previously described method,10 which entails measuring the medial and lateral joint space and observing the presence of osteophytes and sclerosis of the bone. (It was not possible to assess postoperative and follow-up radiographs in a blinded fashion, since the fixation method was visible.)
Postoperative radiographs were assessed for the percentage of bone contact at the osteotomy site. Values from the anteroposterior and lateral views were multiplied to provide a surface-area percentage of bone contact. Bone contact was rated as excellent if it exceeded 75% of the cross-sectional area; good if 50%–75%; fair if 50%–25%; and poor if < 25%. For example, an osteotomy with 70% bone contact according to an anteroposterior film and 70% on lateral view would be graded as achieving fair contact (70% × 70% = 49%).
Preoperatively, both groups had similar demographic variables and radiographic extent of osteoarthritis (Table 1). There was a trend for the plate fixation group to be somewhat younger, but this did not reach statistical significance (p = 0.07). Both groups had similar degrees of preoperative malalignment, with a mean femoral–tibial angle of 2° varus. The radiographic extent of osteoarthritis, as measured by the presence and size of osteophytes and the preoperative joint space, was similar in the groups. Patients in both groups had similar degrees of intraoperative corrections and similar values for postoperative femoral–tibial alignment.
Demographics, by fixation method
Loss of alignment during healing of the osteotomy was defined as the difference between the 1-year follow-up and the initial postoperative phase. We analyzed loss of alignment based on groups based on method of fixation and degree of bone contact. SYSTAT (Systat Software Inc., Point Richmond, Calif.) was used for statistical analysis.
Radiographs and clinical charts were reviewed to identify complications, which were analyzed by fixation-method group. They included loss of femoral–tibial alignment of 5° or more during healing of the osteotomy; non-union or delayed union of the osteotomy; infection; and failure of fixation, defined as staple pull-out or subsidence of the blade plate or fracture of the screws.
Results
Average postoperative alignment was 8.0° (standard deviation [SD] 3.3°) valgus in the plate group and 8.7° (SD 3.3°) in the staple group. After 1 year of recovery, the mean femoral–tibial alignment was 4.7° (SD 5.7°) for the group with plates and 6.3° (SD 3.8°) for the group with staples. Hence, the plate group lost an average of 3.3° (SD 5.4°) of alignment, whereas the staple group lost 2.4° (SD 3.2°). Alignment at 1 year of follow-up and loss of alignment during healing did not differ significantly (p > 0.67). One-quarter or so of cases showed a loss of alignment ≥ 5° during healing with either osteotomy method (Table 2).
Maintenance of alignment by method of fixation, no. of patients
The amount of bone contact at the osteotomy site did not differ significantly between the groups (Fisher’s exact test, p > 0.67), but did correlate strongly with maintenance of femoral–tibial alignment during healing (p < 0.001). In 85% of all our cases with good or excellent bone contact, alignment was maintained during healing of the osteotomy, compared with 64% with poor or fair contact (p = 0.009; Table 3).
Maintenance of alignment by bone contact at the osteotomy site, no.
When examined by group (Table 3), this dependency of maintenance of alignment during healing on the degree of bone contact at the osteotomy site held true for cases done with plate fixation, but not for those done with staple fixation. Ninety percent of plate fixations with good or excellent bone contact maintained alignment, along with 57% of those with poor or fair bone contact (p = 0.004). In contrast, 23% of staple fixations lost 5° or more of femoral–tibial alignment despite good or excellent contact at the osteotomy site. Unfortunately, our study lacks the power to establish whether the plate method was more effective than staple fixation for maintaining alignment when the bone contact was good to excellent.
Two of the 28 cases with plate fixation and none of the 16 cases with staple fixation had non-union (Table 4). In the plate group, the cases of non-union led to loss of alignment of ≥ 5°; both required additional operative procedures with bone grafting and revisions of the plate to effect healing. There was also 1 case of delayed union in the plate fixation group. Staple pullout occurred in 2 cases in the staple fixation group, and subsidence of the plate into the osteotomy site in 1 patient in the plate fixation group. Other complications in the plate fixation group included 1 patient who developed a partial peroneal nerve palsy and 1 who developed a deep wound infection. Hence there was a trend for the plate group to have a higher incidence of complications, but this difference was not statistically significant (p = 0.20).
Complications by fixation method
If maintenance of alignment during healing is used as the criterion for success of the osteotomy, then fixation failed in 12 of 44 cases (27%). This overstates the incidence of clinical failure. Chart review of these 12 patients was performed at least 2 years and an average of 4.8 years after surgery. At that interval, only 5 of the 12 patients with loss of alignment were noted to have had clinical failures such that they required revision to a total knee replacement. Most of the 12 patients who had a loss of alignment had a valgus femoral–tibial alignment at 1 year of followup, and hence they were improved in comparison with their preoperative function.
Discussion
The tension-band (Chandler) blade plate is intended for fixation of tibial osteotomies. Our retrospective radiographic review of its use suggests some areas of concern. The plate system was effective at maintaining alignment for 90% of subjects when there was excellent bone contact at the osteotomy site, but was not effective at maintaining alignment if contact was less than 50% of the cross-sectional area at the site. Three-quarters of patients with poor bone contact had loss of alignment during healing of the osteotomy. This may be related to the geometry of the plate and the fact that it does not extend distally down the lateral cortex of the tibia. With poor bone apposition, the screws can toggle in the plate, causing loss of reduction. The biomechanics of this plate have not been well described, which warrants further research.
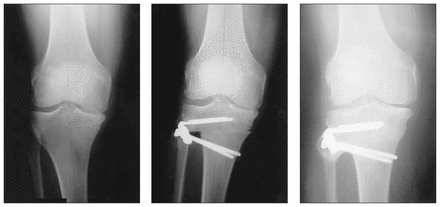
In the radiographs (Fig. 1, Fig. 2), the second set demonstrates a case of plate fixation with good position of the implant, but only a fair degree of bone contact. The osteotomy healed with collapse of the medial bone and clinically significant loss of alignment. The patient underwent a total knee arthroplasty, 18 months after the osteotomy.
Radiographs of a patient’s knee before (left), immediately after (centre) and 1 year after high tibial osteotomy. Bone contact in this case was excellent, and alignment was maintained over the course of healing.
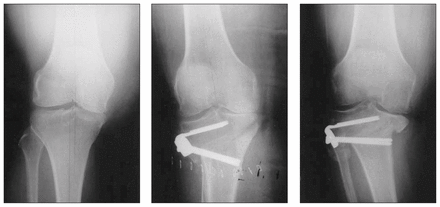
Radiographs before, immediately after and 1 year after a high tibial osteotomy. The amount of bone contact in this case was poor, and femoral–tibial alignment was lost during healing.
A high incidence of failure of blade-plate fixation for tibial osteotomies has been reported in the literature. Koshino and associates6 reported “sinking” of the osteotomy site of up to 9 mm in 67 of 134 knees. This occurred more commonly in elderly patients with osteoporosis.6
In our series, there were 2 cases of non-union and 1 case of delayed union in the plate fixation group. The non-unions ultimately resulted in loss of femoral–tibial alignment ≥ 5°. This incidence of non-union was not statistically different from the staple group, but did represent a trend toward an increase in this complication. It appears that the plate, although not rigid enough to always maintain alignment, may have sufficient rigidity to prevent some minor settling at the osteotomy site and may therefore predispose to non-union. With delayed or non-union complications, the osteotomy had rotated around the laterally based blade plate and drifted into the varus position. In contrast, when staples pulled out of the bone, there was no laterally based fulcrum, so these osteotomies settled without changing the femoral–tibial alignment. Our incidence of non-union is somewhat higher than the 0–1% reported with other types of blade plates.6,11
One patient with a plate fixation developed an intra-operative partial peroneal nerve palsy. Another in that group developed a deep postoperative infection, which ultimately resulted in loss of alignment during healing of the osteotomy. It is unknown whether the additional dissection required for insertion of the plate contributed to these complications. Other authors have examined the effect of blade-plate fixation on postoperative complications: when Hoffman and coauthors11 compared blade-plate fixation to cast immobilization without staples, they found a lower incidence of transient nerve palsy, wound infection and loss of correction in the former group.
Although plate systems may have some benefits in terms of better postoperative ambulation and range of motion, 2 studies found no clinical difference in outcomes for plate versus staple fixation.
Hee and associates12 presented their data from a retrospective study of 223 knees with high tibial osteotomy. When 74 osteotomy patients (97 knees) who had buttress plate fixation were compared with 97 patients (126 knees) with staple fixation, they found no clinical differences. Both groups had similar mean postoperative Hospital for Special Surgery (HSS) knee scores. The incidence of wound infection was significantly higher among those fixed with a buttress plate (9 of 97 v. 1 of 126 cases; p < 0.05), but no statistical difference between groups was found for incidence of non-union or recurrence of varus deformity. Their conclusion was that buttress plating had no significant advantage over staple fixation for high tibial osteotomy.12
Similarly, when Pascher and co-workers13 retrospectively compared plate fixation with staple and supplemental cast fixation, they found that the staple group had a slightly increased bone healing time. At a mean of 5.7 years of follow-up, the staple group had slightly better HSS scores and patient satisfaction, with no between-group difference in the rate of complications. They concluded that staples were less invasive and had comparable clinical results.
A major limitation of our study is a lack of prospective data on clinical outcomes and patient satisfaction with the 2 different procedures and postoperative protocols. In addition, our study sample was not large enough to show statistical significance between the different methods of fixation. Power analysis calculation determined that 108 cases per group would be required for the study to have 80% power to assess for a statistically significant differences in loss of alignment between groups.
In our study, the most important factor for maintenance of alignment was not the fixation method, but rather the degree of bone contact at the osteotomy site. When contact there was excellent or good, the majority of cases maintained alignment. A trend for the plate to be more effective at maintaining alignment than the staple and supplemental cast when bone contact was excellent or good did not reach statistical significance. A power analysis established that 405 cases would be required to show significance for this trend.
As a result of this study, we have modified our surgical technique to include intra-operative fluoroscopy to try to optimize bone contact at the osteotomy site. Our experience with the Chandler blade plate was that it had a trend towards a higher incidence of delayed or non-union. Since the literature does not support the existence of better clinical outcomes for plate fixation, we have reverted to the simpler staple method of fixation for tibial osteotomies.
Acknowledgement
This study was supported by an educational fellowship from the R. Samuel McLaughlin Foundation.
Footnotes
Competing interests: None declared.
- Accepted September 1, 2004.