Abstract
Background: Several systemic factors, including jaundice, long-term corticosteroid therapy, diabetes and malnutrition, increase the risk of anastomotic dehiscence. The local application of molgramostim (recombinant human granulocyte-macrophage colony stimulating factor) has been reported to improve impaired dermal wound healing. Since jaundice, one of the systemic risk factors for anastomotic dehiscence, causes significant impairment of anastomotic healing, we hypothesized that locally injected molgramostim could improve the healing of bowel anastomoses in bile-duct-ligated rats used as an experimental model for jaundice.
Methods: Eighty-six Sprague–Dawley rats were randomized into 4 groups of 20–22 animals each as follows: group 1 — colonic anastomosis only; group 2 — laparotomy followed 7 days later by colonic anastomosis; group 3 — common-bile-duct ligation (CBDL) followed 7 days later by colonic anastomosis (control group); group 4 — CBDL followed by colonic anastomosis with locally applied molgramostim. Laparotomy was performed under anesthesia in group 2 rats. In groups 3 and 4, laparotomy was followed by ligation and dissection of the common bile duct. After 7 days, colonic anastomosis was performed; in group 4 rats, molgramostim (50 μg) was injected into the perianastomotic area. On postoperative day 3, rats were killed, and the bursting pressures and hydroxyproline levels measured. Two rats from each group were selected for histopathological examination.
Results: The mean bursting pressure in group 4 was significantly higher than that in group 3 (37.8 v. 30.5 mm Hg [p < 0.01]). The mean hydroxyproline level in group 3 was significantly lower than that of the other groups (2.7 v. 3.1–3.5 mg/g tissue [p < 0.01]). On histopathological examination, specimens from group 4 rats showed an increased mononuclear cell population and a smaller gap on the anastomotic line than those from group 3.
Conclusion: The local injection of molgramostim improves healing of the impaired wound in rats subjected to CBDL.
Several systemic factors, including ischemia, jaundice, infection, diabetes mellitus and malignant lesions, increase the risk of poor healing in colonic anastomosis.1 Obstructive jaundice causes serious pathologic and biochemical changes associated with increased postoperative morbidity and mortality.2 The condition also can result in impaired hepatic, renal and systemic immune functions.3 In experimental studies, jaundice lowers the bursting strength of abdominal wounds, decreases the rupture strength of skin wounds, adversely affects the migration of fibroblasts in wound healing4–8 and reduces the migration of reticuloendothelial cells.9 Immune dysfunction has also been demonstrated and may be due to cytokine production by macrophages or abnormal hepatocyte-Kupffer cell dysfuctions.9 In oncologic surgery, gastrointestinal cancers and their lymphadenopathies cause bile duct obstruction necessitating internal drainage of the bile. In clinical and experimental studies jaundice has emerged as one of the adverse risk factors in wound healing.4–11 Wound dehiscence occurs in 2%–4% of jaundiced patients and incisional hernia in 10%–12%.2 Postoperative death has varied from 10%–30% in patients with obstructive jaundice.6–10 Leading risk factors for death in these patients have been identified as wound infection, septicemia, intra-abdominal abscesses, increased wound dehiscence and anastomotic leak.7–11
Recombinant human granulocyte-macrophage colony stimulating factor (molgramostim) has been shown to induce hematopoietic progenitor cells in myeloid and erythroid lineages to proliferate and to stimulate mature monocytes/macrophages and neutrophils. 12 Furthermore, it has been shown to enhance the migration and proliferation of endothelial cells and to promote keratinocyte growth.13,14 Animal studies have also shown that local application of molgramostim to wounded areas results in an increase in granulation tissue and breaking strength of incisional wounds, resulting in a faster wound healing.15–22 For this reason, some have suggested the use of molgramostim therapy in some patients with non-healing ulcers.23
We hypothesized that molgramostim may have beneficial effects on impaired healing of colonic anastomosis in jaundiced rats. Thus, we studied the effects of locally applied molgramostim on the healing process in rats that had common-bile-duct-ligation (CBDL) as an experimental model for jaundice.
Methods
Our procedures were in accordance with the Guide for the care and use of laboratory animals (National Institutes of Health Publication no. 86-23, revised 1985).
Eighty-six male Sprague–Dawley rats were randomized into the following groups:
Group 1: colonic anastomosis (n = 22)
Group 2: laparotomy and colonic anastomosis (n = 20)
Group 3: colonic anastomosis in rats after CBDL (control group; n = 22)
Group 4: colonic anastomosis in rats after CBDL plus 50 μg of molgramostim (n = 22).
Rats were brought into the laboratory 24 hours before the operation, and housed in separate cages. Investigators were blinded to groups during surgical procedures. All animals were anesthetized with intramuscular injections of ketamine (40 mg/kg; Ketalar, Parke Davis, Pfizer, Istanbul, Turkey) and xylasine (5 mg/kg; Rompun, Bayer, Leverkursen, Germany). After laparotomy in the rats from groups 3 and 4, the common bile duct was ligated and dissected. All components of anastomotic healing were studied in the significantly jaundiced rats in these 2 groups.2 In group 2, only laparotomy was performed. After 7 days, the rats in all groups were anesthetized. A 4-cm median laparotomy was performed and the left colon transected (without resection of a segment) by a transverse circumferential incision 5 cm proximally to the peritoneal reflection, taking care to preserve the marginal arteries. The bowel was restored by an end-to-end anastomosis with 6 interrupted, inverting sutures of 6-0 polypropylene (Prolene; Ethicon, Edinburgh). In group 4, 0.5 mL of molgramostim (from the solution of 100 μg/mL; Novartis Pharma, Basel) was injected subserosally into the perianastomotic area by multiple injections. We applied 50 μg molgramostim as recommended in our earlier studies in which molgramostim was used on anastomotic wounds.24,25 Anastomoses were performed on postoperative day 7 after CBDL to allow the development of significant jaundice. Subsequently, the abdominal incision was closed with 2 layers of continuous 4-0 silk sutures. Postoperatively, the rats were fed a diet with rat chow and water ad libitum.
On postoperative day 3 before bursting pressures were measured, 2 rats from each group were randomly selected for histopathological examination of anastomotic tissue. Investigators were blinded to groups, repeat laparotomies were made under anesthesia, and blood samples were taken to measure the serum bilirubin levels and the leukocyte count. Intraabdominal adhesions were separated gently, and a 6-cm segment of colon centred by the anastomosis was resected; the rats were then killed. In the remaining rats, the distal parts of the segments were closed with 2-0 silk sutures. The proximal parts were attached to an intraluminal pressure manometer (monitoring kit L978-A07; Abott, Slingo, Ireland). The segments were filled with isotonic NaCl solution with continuous infusion (4 mL/min). The rising intraluminal pressures were monitored and the bursting pressures noted.
Determination of hydroxyproline levels
A segment of tissue measuring 0.5 cm (30–50 mg) was resected from the anastomosis, frozen to −25°C, and then sent immediately for evaluation of hydroxyproline levels. The tissue samples were placed into hydrolysis tubes. 50 mM of potassium phosphate buffer, pH 7.0, and equal volume of concentrated hydrochloric acid were added to each tube, and the samples were hydrolyzed at 110°C for 16 hours. The pH of the samples was adjusted to 8.5 with diluted sodium hydroxide and oxidized at room temperature with chloramine-T solution. After 4 minutes, Ehrlich’s reagent was added to the tubes. The colour was allowed to develop at 60°C for 25 minutes and the absorbency at 560 μm was determined by the method of Bergman and Loxley.26 The hydroxyproline concentration was calculated as μg/mg wet weight tissue.
Histopathological examination
For the histopathological examinations, 1 cm of tissue sample from the injection site was kept in 10% buffered formalin solution and stained with hematoxylin–eosin.
Statistical analysis
The distribution of bursting pressure and hydroxyproline values was normal and their variances were homogeneous. Therefore, 1-way analysis of variance with the post-hoc Tukey test was used for the statistical analysis. Because multiple comparisons were made, the Bonferroni correction was performed and the criterion for significance was accepted as p < 0.016. The statistical analyses were performed with use of a statistical program (SPSS 10.0, Prentice Hall, NJ).
Results
The mean values of total bilirubin levels in the control (group 3) and molgramostim-treatment group (group 4) were 235 μmol/L and 226 μmol/L respectively. The differences of mean values for leukocyte counts and total bilirubin levels between groups 3 and 4 are statistically not significant, indicating that both group of animals were equally jaundiced.
The mean values of the bursting pressures and hydroxyproline levels of the groups are presented in Table 1. The values for bursting pressures and hydroxyproline levels in groups 1, 2 and 4 were significantly higher than those in group 3 (p < 0.001, Table 1). On the other hand, the differences of mean values for bursting pressures and hydroxyproline levels between groups 1, 2 and 4 were statistically not significant.
Bursting pressures and hydroxyproline levels in control and treatment groups. Values are means and standard deviations
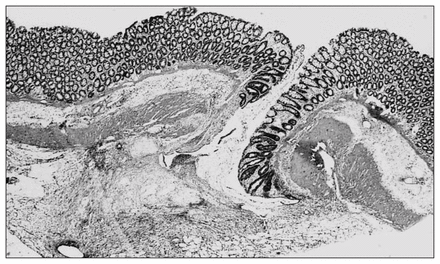
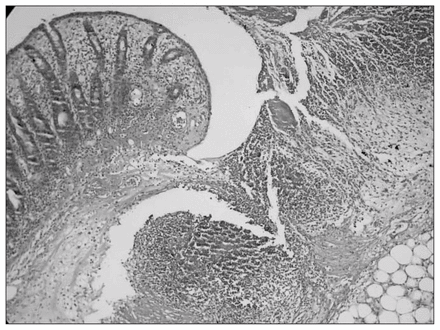
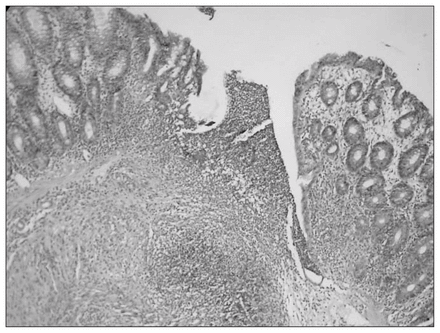
Sections of specimens taken from colonic segments of anastomotic areas are presented in Figure 1, Figure 2 and Figure 3. In Figure 1, histopathological examination of a section from a group 1 rat indicates that the anastomotic defect is nearly filled with granulation tissue and there is no gap in the submucosal layer. In Figure 2, a section of colonic segment from a group 3 rat, there is a large gap in the submucosal layer and an abscess has formed near the anastomotic line. In addition, the mononuclear cell population in the anastomotic area is sparse in this specimen. Figure 3 demonstrates a section of colonic segment from a group 4 rat injected with molgramostim. The mononuclear cell population is increased, and the gap on the anastomotic line is smaller than that in group 3.
Cross-section of a specimen from a rat in group 1 (colonic anastomosis only) demonstrates normal anastomotic wound healing on postoperative day 3. The gap between the anastomotic edges is filled by granulation tissue (hematoxylin–eosin stain; original magnification ×10).
Cross-section of the anastomosis in a rat from group 3 (colonic anastomosis after common-bile-duct ligation) demonstrates impaired anastomotic wound healing with a significant gap in the submucosal layer. There is an abscess formation in the anastomotic area. Mononuclear cell infiltration is decreased (hematoxylin–eosin stain; original magnification ×20).
Cross-section obtained on postoperative day 3 of the anastomosis from a rat in group 4 (common-bile-duct ligation [CBDL] followed by colonic anastomosis and injection of 50 μg molgramostim) indicated that the gap at the anastomotic line is smaller than that in the group with CBDL only. The mononuclear cell population is also increased (hematoxylin–eosin stain; original magnification ×20).
Discussion
In gastrointestinal surgery, impaired wound healing and anastomotic dehiscence are important problems. Obstructive jaundice is known to compromise both hepatic and systemic immune functions, and it has been reported that immune system defects in phagocytic and neutrophilic functions may occur.3 Also, there is a functional disorder of the reticuloendothelial system, which plays a role in the immunologic response and is important in the synthesis of monocytes, neutrophils and prostaglandins.3 Furthermore, pathologic conditions caused by obstructive jaundice, including renal insuffiency, cardiovascular changes and coagulation disorders, may cause additional deleterious effects on the healing of anastomoses. Obstructive jaundice has been shown to reduce the number of fibroblasts present in healing wounds6,7 and to decrease the migration of reticuloendothelial cells and fibroblasts into the wounded area.6,8 In addition, delay in angiogenesis, which adversely affects the collagen deposition, has been reported to occur in rats with obstructive jaundice.2,6–8 In line with these earlier results, hydroxyproline levels, which indicate the amount of collagen in the wounded field, and the bursting pressures, were decreased significantly in the CBDL group (group 3).
In cancer patients, granulocyte-macrophage colony stimulating factor (GM-CSF) is widely used during the treatment of neutropenia caused by chemotherapy. Beneficial effects of GM-CSF have been reported in the treatment of several clinically and experimentally impaired dermal wounds such as venous ulcers, Adriamycin extravasations and radiotherapy-related dermal complications.27,28 Recent studies suggest that the stimulation of cell infiltration by GM-CSF in the injection area induces collagen synthesis by fibroblast activation, increases the population of keratinocytes and Langerhans cells, enhances the proliferation of endothelial cells and induces their migration.29,30 GM-CSF also has immunologic, hematologic and inflammatory effects. It has been reported to increase the population and function of monocytes-macrophages3 and to induce proliferation and differentiation of monocytes of large macrophage-like cells.31,32 In support of these findings, compared with control group, increased mononuclear cell infiltration observed in our histopathological specimens from molgramostim-treated animals (Fig. 2, Fig. 3). The action of GM-CSF on monocytes-macrophages, which may be relevant to enhanced antimicrobial activity, include increased phagocytosis and oxidative metabolism, an increased number of Fc receptors, release of chemotactic factors and stimulation of mechanisms for killing intracellular viruses, fungi, bacteria and protozoa.12,32 Because of these effects, GM-CSF has antimicrobial and antitumoral effects and enhances wound healing.12,32
In our earlier studies, we found that GM-CSF significantly improves anastomotic wound healing in rats undergoing long-term steroid and intraperitoneal 5-fluorouracil treatment. 24,25 We also found that in intra-operatively radiated rats, GM-CSF had beneficial effects on the wound healing in ischemic colon segments and anastomoses.33,34
Although there are multiple parameters, including bursting pressure, bursting wall tension and tensile strength,35 with which to observe the intrinsic resistance of an anastomosis, we have chosen bursting pressure as a mechanical parameter since this approximates clinical conditions closely, especially in the early phase of wound healing.36 In addition, we measured the diameters of anastomoses after bursting and found that there were no statistically significant differences among the groups.
Although systemic administration of GM-CSF has been shown to have no effect on wound healing,21,24 it significantly improves dermal-wound healing when it is applied locally. For example, various routes of local molgramostim application (subcutaneously around the wound, incubated with skin grafts and applied topically in sterile water) have been demonstrated to induce rapid wound healing and decrease the time to total wound closure.15–17 Although in some studies, intraperitoneal or systemic administration of GM-CSF was reported to be ineffective on the healing of intestinal anastomoses,37,38 it is likely that due to the intraperitoneal adhesions, the intraperitoneal use of the drug may not have access to the anastomotic area, and local concentration of the drug may not reach a level required for a healing effect. In line with this suggestion and earlier studies, systemic application of GM-CSF was also found to be ineffective in our previous study.24 However, after subserosal injection of GM-CSF into the anastomotic line of the intestinal wall, a significant improvement in the healing process of the anastomotic wound was found.
Compared with the control group (group 3), bursting pressures and hydroxyproline levels were significantly higher in rats from group 4 in which GM-CSF was injected perianastomotically, indicating a beneficial effect on the healing of anastomotic wound. Although the exact mechanism of the GM-CSF effect is currently unknown, multiple factors likely play roles. First, it has been reported that GM-CSF reverses neutrophil and macrophage functions, which have been damaged in jaundice. Second, GM-CSF increases the number of fibroblasts in the periphery of the anastomotic area, causing an increase in the amount of collagen in the healing area. Finally, GM-CSF has been reported to have antimicrobial and neovascularization effects on application sites.12,39 All of these effects may reduce the increased infection risk in rats that had undergone CBDL. Also, GM-CSF has been used clinically in patients with coronary artery disease due to its neovascularization effects.39 Combinations of these factors may contribute to the beneficial effects of GM-CSF application observed in this study.
Conclusion
The local application of molgramostim significantly improves healing of the impaired bowel anastomosis in rats after CBDL.
Acknowlegement
We thank Ms. Mary Pfeiffer of NIDA/NIH for reading the manuscript.
Footnotes
Competing interests: None declared.
- Accepted May 18, 2004.