Nine out of every 10 abnormal biliary–enteric communications are the result of perforation caused by gallstones from the gallbladder or common bile duct (CBD) into the duodenum; the remaining one is the result of peptic ulcer, tumour, trauma or other local abnormalities. 1 In the case we present here, 2 different biliary–enteric fistulas were found.
Case report
Twice in January 2003 we treated a 66-year-old man for recurrent severe bleeding from a duodenal ulcer by endoscopic injection of polidocanol. After the second intervention, he suffered acute but mild pancreatitis. One year later, he presented with abdominal pain in the right upper quadrant and intermittent cholestasis. The cholangio-MRI showed cholecystolithiasis and stenosis of the CBD and was consistent with chronic pancreatitis. Endoscopic cholangiopancreatography (ERCP) was attempted, but the papilla of Vater could not be cannulated. A laparoscopic cholecystectomy was performed. Cholangiography done intraoperatively showed a choledochoduodenal fistula distal to the CBD stenosis (i.e., between the stenosis and the papilla). Postoperatively, a guidewire was placed endoscopically through the fistula opening, allowing definitive access to the CBD and successful stenting of the stenosis. Nine months later, the patient again suffered from cholestasis due to occlusion of the stent. The stent was replaced. Seven months after this, the patient was readmitted because of diarrhea, bloating and pain in the right upper abdominal quadrant after a high fat meal. The elevated liver function test results indicated cholestasis.
Because of the recurrent episodes of cholestasis, indicating the failure of stenting, and because of the undefined nature of the CBD stenosis, the patient under-went bilioenteric diversion.
The preoperative ERCP confirmed the choledochoduodenal fistula located about 3 cm proximal to the papilla of Vater (Fig. 1, Fig. 2). Proximal to this fistula, a 2–3-cm long filiforme stenosis was cannulated. During the operation, a 3-cm long cystic duct was prepared. Around this, a cavity extended to the caval vein, with connection to a duodenal diverticulum. The cavity was surrounded by granulomatous tissue indicating chronic inflammation. The clip once used for closure of the cystic duct remnant was displaced. The duodenal diverticulum was resected. The CBD and the cystic duct were removed. A Roux-en-Y hepaticojejunostomy was established.
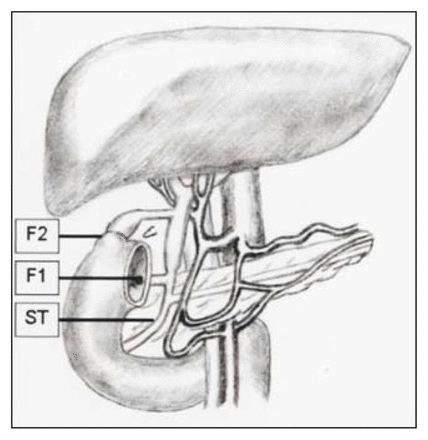
Schematic overview of the patient’s anatomy at the time of the hepaticoduodenostomy. F1 = choledochoduodenal fistula, F2 = cystic duct remnant–duodenal fistula (missing clip beside), ST = site of stenosis of the common bile duct.
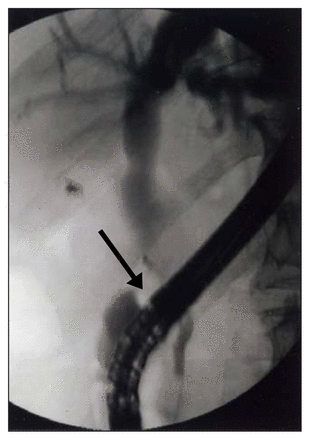
Endoscopic retrograde cholangiopancreatography shows the situation after laparoscopic cholecystectomy and before hepatico-duodenostomy. The fistula is located behind the endoscope (arrow).
Postoperatively, the cholestasis diminished, and the patient has been asymptomatic ever since.
Discussion
In our patient, the choledochoduodenal fistula was most probably caused by the initial endoscopic polidocanol injection. We believe that this treatment established a connection to the CBD, since the choledochoduodenal fistula ended in the niche of a healed ulcer. The consequent pancreatitis suggests either direct toxic tissue damage or duct damage from the polidocanol or an obstruction of the papilla of Vater. However, a perforation of the duodenal ulcer with a choledochoduodenal fistula cannot be ruled out. The consequence of the inflammatory process was a choledochoduodenal fistula and a postinflammatory choledochal stenosis.
The second fistula was found between the cystic duct remnant and a duodenal diverticulum. We hypothesize that bile leakage allowed by the missing clip on the cystic duct led to chronic inflammation around the cystic duct remnant followed by fistula formation. Earlier publications described fistulization of a cystic duct remnant after calculous obstruction of the remnant,2 but neither in the cholangiogram obtained during cholecystectomy nor in the final operation were any calculi detected in our patient. The repeated introduction of biliary stents might also have irritated the cystic duct remnant in the sense that the catheter might have been pushed too far, causing erosion of the cystic duct.
Although asymptomatic biliary–enteric fistulas are not treated, there are 2 options for the treatment of symptomatic patients3,4: temporary biliary decompression with stenting and permanent hepaticodigestive bypass.
In our case, the patient’s complaints were due to recurrent cholestasis rather than to the fistulas. A Roux-en-Y hepaticojejunostomy with tension-free end-to-side connection of the hepatic duct to the jejunum was performed. The surgical approach was chosen after about 1 year of therapy with a hepaticoduodenal pigtail stent that left the patient symptomatic owing to repeated occlusions. Operative therapy solved the problem of recurrent abdominal pain and diarrhea. At the same time, the 2 fistulas were excised.
The hepaticoduodenostomy itself is not to be regarded as a fistula as long as the Y part of the jejunum measures at least 50 cm. The more likely complication is cholangitis. However, we hope that this treatment does not induce a new fistula, because a fistula is a rare complication of biliary–digestive anastomosis with choledochoduodenostomy (with consective reflux cholangitis).
Acknowledgements
We thank Dr. Niklaus Schaub for his valuable input and excellent cooperation in the preparation of this case note.
Footnotes
Competing interests: None declared.
- Accepted September 6, 2006.