Abstract
Background: A multidisciplinary tracheostomy team was created in 2005 to follow critically ill patients who had undergone a tracheostomy until their discharge from hospital. Composed of a surgeon, surgical resident, respiratory therapist, speech-language pathologist and clinical nurse specialist, this team has been meeting twice a week for rounds involving patients who transitioned from the intensive care unit (ICU) to the medical and surgical wards. Our objective was to assess the impact of this multidisciplinary team on downsizing and decannulation times, on the incidence of speaking valve placement and on the incidence of tracheostomy-related complications on the ward.
Methods: This study was conducted at a tertiary care, level-1 trauma centre and teaching hospital and involved all patients who had received a tracheostomy during admission to the ICU from Jan. 1 to Dec. 31, 2004 (preservice group), and from Jan. 1 to Dec. 31, 2006 (postservice group). We compared the outcomes of patients who required tracheostomies in a 12-month period after the team was created with those of patients from a similar time frame before the establishment of the team.
Results: There were 32 patients in the preservice group and 54 patients in the post-service group. Under the new tracheostomy service, there was a decrease in incidence of tube blockage (5.5% v. 25.0%, p = 0.016) and calls for respiratory distress (16.7% v. 37.5%, p = 0.039) on the wards. A significantly larger proportion of patients also received speaking valves (67.4% v. 19.4%, p < 0.001) after creation of the team. Furthermore, there appeared to be a decreased time to first tube downsizing (26.0 to 9.4 d) and decreased time to decannulation (50.4 to 28.4 d), although this did not reach statistical significance owing to our small sample size.
Conclusion: Standardized care provided by a specialized multidisciplinary tracheostomy team was associated with fewer tracheostomy-related complications and an increase in the use of a speaking valve.
Tracheostomy is a common procedure in the intensive care unit (ICU) and is being performed with increasing frequency in critically ill patients.1 This trend is partly owing to the development of the percutaneous technique as well as to evidence supporting early tracheostomy decreasing the duration of mechanical ventilation.2
With more tracheostomies performed on patients in the ICU, a greater number of patients are being discharged from the ICU to medical and surgical wards with tracheostomy tubes in situ. Since the advent of the percutaneous technique, these patients no longer benefit from the follow-up of the operating surgeon and surgical team. Often they are lost to follow-up on transfer from the ICU. Ward staff with varying levels of experience are then required to assume the responsibility of tracheostomy care. However, serious tracheostomy-associated complications exist (e.g., tube blockage causing respiratory failure, respiratory infection, hemorrhage). These complications must be prevented as well as recognized and managed promptly on the wards. Complications, such as death from tube blockage, have occurred at our institution and have been reported at others.3,4 These adverse events underscore the need for specialized knowledge and regular follow-up in the care of patients with tracheostomy tubes.
To better meet the complex care needs of patients transferred with a tracheostomy tube from the ICU to the wards, a multidisciplinary tracheostomy team was created at the Montreal General Hospital. The team follows these patients on medical and surgical wards until they undergo decannulation or are discharged from hospital.
This study was designed to assess the impact of a dedicated specialized multidisciplinary service on tracheostomy care outcomes (downsizing, decannulation, speaking valve use) and the incidence of tracheostomy-related complications.
The tracheostomy team
The Montreal General Hospital is a level-1 trauma centre with a 24-bed ICU. Patients with a tracheostomy tube can be discharged from the ICU to medical or surgical beds on 5 different floors.
Prior to the development of the team, tracheostomy care decisions were left to the discretion of the original admitting service. Furthermore, these decisions about downsizing and decannulation were not necessarily made with the input of the surgeon who performed the procedure. Daily care plans, such as suctioning schedules, were optimized by respiratory therapists only when called by nurses, whose experience with tracheostomies was variable. The management was inconsistent, and tracheostomy-related complications were occurring owing to poor follow-up.
To help improve this situation, the tracheostomy service was piloted in the summer of 2005. By March 2006, it consisted of a general surgeon, a general surgery resident, a respiratory therapist, a speech-language pathologist and a clinical nurse specialist. Since then, the team has been meeting twice weekly to discuss patients with tracheostomy tubes who have been transitioned from the ICU to medical and surgical wards. Decisions regarding downsizing, decannulation, changes to daily tube care (e.g., increased suctioning) and use of a speaking valve are discussed and communicated in written progress notes to the treating team of doctors and nurses. The specific roles of each team member are detailed in Box 1.
Roles of tracheostomy team members
Staff surgeon
Head of the team
Coordinates the team’s activities
Resident
Responsible for bedside rounds
Performs decannulation and downsizing with the assistance of the respiratory therapist
Respiratory therapist
Performs a bedside check of the tracheostomy tube, the oxygen delivery system and the spare emergency tracheostomy tube
Discusses daily tracheostomy care issues with the nursing staff, patient and family
Speech-language pathologist
Assesses the patient’s ability to tolerate a speaking valve (i.e., assess level of consciousness, airway protection, phonation, management of secretions)
Provides recommendations regarding speaking valve use and/or augmentative communication strategies
Clinical nurse specialist
Assists with discharge planning
Coordinates family meetings
The team is actively involved in the management of ward patients with a tracheostomy until the time of decannulation or discharge from hospital. Whereas most tracheostomies are performed by surgeons/intensivists from the tracheostomy team, the timing of the tracheostomy is at the discretion of the attending ICU physician and the admitting physician.
Methods
Two groups were compared in this study. A historical control group comprised all patients who had received a tracheostomy from Jan. 1 to Dec. 31, 2004, before the implementation of the tracheostomy service (preservice group). The second group included all patients who had received a tracheostomy from Jan. 1 to Dec. 31, 2006, after the implementation of the service (postservice group). Patients were identified using the ICU records database as having received a tracheostomy during their admission to the ICU. Chart review identified which patients were transferred to medical and surgical wards with a tracheostomy tube in situ. The Research Ethics Board of the Montreal General Hospital approved the study protocol.
For both groups, we collected data through manual chart review, which included reviewing progress notes of the medical, surgical, nursing, respiratory therapy and speech-language pathology staff as well as relevant consultation reports and operative notes. When possible, we correlated the data with information found in the prospectively collected ICU database. For the postservice group, data were also correlated with a separate prospectively collected data set kept by respiratory therapy and speech-language pathology staff. Also, separate records from the speech-language pathology department were used to supplement and corroborate the dates of speaking valve use in the preservice group.
The information collected included sex, age, admitting diagnosis, Acute Physiology and Chronic Health Evaluation (APACHE) II scores, the indication for tracheostomy and the type of tracheostomy. We also recorded the dates of tube changes, decannulation, speaking valve placement, discharge from ICU, return to the ICU for respiratory decompensation and discharge from hospital.
We noted tracheostomy-related complications occurring while the tube was in situ. The complications included tube blockage, displacement, accidental decannulation, cuff rupture, ostomy site ulceration or cellulitis, respiratory infection, bleeding, calls for respiratory distress and death. Respiratory infection was identified by documented initiation of antibiotics for new positive sputum cultures, consolidation on chest radiographs or clinical suspicion of respiratory infection. Calls for respiratory distress included any urgent call to medical, surgical and nursing staff or a respiratory therapist, with a documented drop in oxygen saturation to less than 88%.
Statistical analysis
We performed our statistical analysis using the SAS System, version 8.2 (SAS Institute). Patient characteristics at baseline were summarized using proportions or means and standard deviations (SDs) as appropriate. We used Student t tests or Wilcoxon rank-sum and Kruskal–Wallis tests to compare clinical variables between the preservice and postservice groups for normally and non-normally distributed data, respectively. We used a multivariate Cox hazard regression model to identify factors associated with the placement of a speaking valve while controlling for the effect of the factors already known to affect recovery, such as age and traumatic brain injury. Variables with bivariate significance (p < 0.10) were entered into the regression. For this analysis, the hazard ratio (HR) and 95% confidence interval (CI) for each significant variable are presented.
We performed a subgroup analysis in the traumatic brain injury group in whom time to downsizing and decannulation was assessed in relation to whether the patient was followed by the tracheostomy service. A similar subgroup analysis was performed for patients who received care on nonsurgical wards. We considered results to be significant at p < 0.05.
Results
Study population
Over the 12-month period preceding the creation of the tracheostomy service (preservice group), 48 patients received tracheostomies. In the 12-month period afterwards (postservice group), 89 patients received tracheostomies. From the postservice group, we excluded 7 patients because they were managed independently by otolaryngology (n = 6) or thoracic surgery (n = 1) staff. We excluded 9 patients from the postservice group because in the first 2 months a respiratory therapist was not present regularly at the biweekly tracheostomy team meetings. We included in our analysis a total of 86 patients (32 in the preservice group and 54 in the postservice group) who were discharged with tracheostomy tubes from the ICU to medical and surgical wards.
Demographic and clinical characteristics
As presented in Table 1, the only significant difference between the 2 groups with respect to demographic and clinical characteristics was the proportion of tracheostomies performed with an open technique.
Demographic and clinical characteristics of patients who received tracheostomies before and after the establishment of a multidisciplinary tracheostomy team
Of the 32 patients in the preservice group, the indications for tracheostomy were as follows: expected prolonged ventilator dependence (n = 21), improved pulmonary toilet (n = 8), head and neck procedures (n = 2) and upper airway compromise (n = 1). Of the 54 patients in the postservice group, the indications for tracheostomy were expected prolonged ventilator dependence (n = 52) and improved pulmonary toilet (n = 2).
Complications
Under the new service, there was a significant decrease in the number of patients with tube blockage and in the number of calls on the wards for respiratory distress. No difference was found with respect to technical complications (displacement, accidental decannulation, cuff rupture), in ostomy site complications or in the rate of respiratory infection. Mortality was similar in both groups. Of all 86 patients, 1 patient in the preservice group died from unexpected respiratory failure (aspiration). There was no significant difference between groups in the number of patients who returned at least once to the ICU for respiratory decompensation (Table 2).
Complications among patients who received tracheostomies before and after the establishment of a multidisciplinary tracheostomy team
Tracheostomy downsizing and decannulation
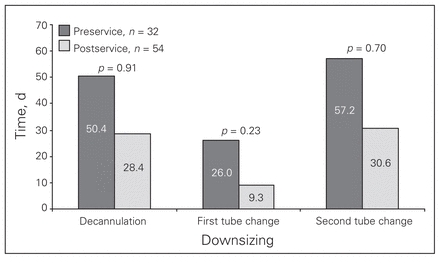
In the preservice and postservice groups, respectively, 59.4% and 68.5% of patients underwent decannulation (p = 0.48). In the postservice group, there was a trend of decrease in the mean (and standard deviation [SD]) number of days to first downsizing (26.0 [SD 76.7] to 9.3 [SD 10.9], p = 0.23), in days to second downsizing (57.2 [SD 128.7] to 30.6 [SD 27.4], p = 0.70) and in days to decannulation (50.4 [SD 98.6] to 28.4 [SD 26.0], p = 0.91; Fig. 1).
Comparison of downsizing and decannulation times in days between patients before (preservice) and after (postservice) the establishment of the multidisciplinary tracheostomy team.
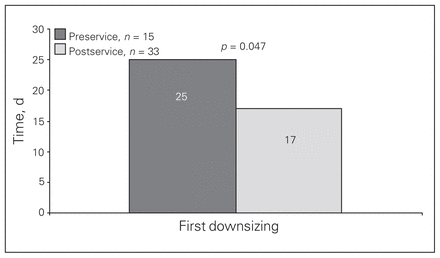
We performed subgroup analyses for patients who sustained traumatic brain injuries (n = 48). There was a significant decrease in the number of days to first downsizing (24.5 [SD 12.5] to 16.6 [SD 10.1], p = 0.047; Fig. 2). This finding was confirmed through Cox regression analysis, which showed an increased HR for reduced time to first tracheostomy tube change for the postservice group compared with the preservice group (HR 2.4, 95% CI 1.2–5.0, p = 0.023). When adjusted for age, the type of tracheostomy and APACHE II score, the HR remained significant (HR 2.62, 95% CI 1.02–6.71, p = 0.045). There was no significant decrease between the groups in time to decannulation.
Comparison of time to first downsizing in patients with traumatic brain injuries before (preservice) and after (postservice) the establishment of the multidisciplinary tracheostomy team.
We also performed a subgroup analysis for patients who received care on nonsurgical wards (n = 20). Time to downsizing and decannulation were not significantly different after the tracheostomy service was established.
Speaking valves
The proportion of patients in the postservice group who received a speaking valve increased from 19.4% (95% CI 8.9%–35.3%) to 67.4% (95% CI 53.4%–77.8%; p < 0.001). Unadjusted Cox hazard regression analysis revealed an increased HR for speaking valve placement under the tracheostomy service (HR 4.8, 95% CI 2.0–11.6, p < 0.001). When adjusted for age, the type of tracheostomy and the presence of traumatic brain injury, the HR was 4.60 (95% CI 1.55–13.60, p < 0.001).
Discussion
This study was designed to analyze the impact of a specialized multidisciplinary service dedicated to the care of patients with a tracheostomy tube. The main findings were that the tracheostomy service resulted in fewer calls for respiratory distress, fewer events of tube blockage, more frequent use of speaking valves and a trend toward shortened time to downsizing and decannulation.
Complications
There are very few reports on dedicated tracheostomy services and their effect on outcomes in patients admitted to hospital. Norwood and colleagues3 describe a respiratory therapist–led team that followed patients from tracheostomy tube placement in the ICU through to discharge from hospital. With a study population size similar to ours (ward patients: n = 20 in the preservice group, n = 51 in the postservice group), they found a significant decrease in all tracheostomy-related complications (blockage, tube displacement, wound infection). Our results are consistent with their findings of decreased complications, although we did not find a significant decrease in all complications. It is possible that our study was not sufficiently powered to demonstrate these differences. Since biweekly progress notes from the tracheostomy team provided more rigorous written documentation, complication underrecording may have been greater in the preservice group than in the postservice group.
The smaller number of calls for respiratory distress and events of tube blockage that we observed after the establishment of the tracheostomy service are important improvements. We attribute these decreases first to better daily tube care. Under the tracheostomy team, there are more frequent evaluations by respiratory therapy staff who then directly communicate any recommendations to the nursing staff. Second, the education provided by the tracheostomy team leads to a better understanding of tracheostomy-related issues by residents and nursing staff. Finally, more appropriate downsizing schedules set by the multidisciplinary team may also explain the improvement. For instance, inappropriately early downsizing in a patient who has substantial secretions that would be better handled with a larger tube intuitively increases the likelihood of respiratory distress and tube blockage.
We feel that the expertise of the respiratory therapist, speech-language pathologist and physicians on the tracheostomy team is as critical to improving care as regular structured assessments. Less resource-intensive interventions, such as a checklist for nurses and treating physicians, might reduce complications; however, the full tracheosomy team is essential for teaching and developing appropriate care plans.
Tracheostomies were performed more frequently with the percutaneous technique in the postservice group. When compared with open tracheostomy, the percutaneous technique has been associated with lower wound infection rates, equivalent rates of clinically relevant bleeding and equivalent rates of pneumonia.1,5 A larger proportion of percutaneous tracheostomies would not, however, account for a difference in the number of calls for respiratory distress or events of tube blockage.
Downsizing and decannulation times
Whereas we have no strict protocol for downsizing and decannulation, it is our standard practice to downsize the tracheostomy tube before decannulation. Before starting corking trials, we prefer to downsize (usually to a 6-French gauge cuffless tracheostomy tube) to allow for sufficient airflow and improved secretion clearance around the tracheostomy. In certain cases, if there is not enough air flow with a 6-French gauge, we may downsize to a 4-French gauge before decannulation. Of all 86 patients in our study, only 3 went directly to decannulation without downsizing.
The decision to decannulate is made on a case-by-case basis. Before decannulation, patients must have sufficient neurologic capacity to protect their upper airway, be able to manage their secretions and tolerate corking trials. If an operative intervention is expected, decannulation is delayed.
We found that time to downsizing and decannulation decreased after implementation of the tracheostomy service. In a study with a larger sample size, this trend could have shown significance. Furthermore, the subgroup analysis of patients with traumatic brain injuries did show a significant decrease in time to first downsizing. This was confirmed with Cox regression analysis, adjusted for age, type of tracheostomy and APACHE II score. We believe that the decreased time to downsizing and decannulation is a result of more appropriate and timely downsizing and decannulation schedules set by the tracheostomy team. In another study of an intensivistled tracheostomy team, Tobin and Santamaria4 reported a significant reduction in decannulation time from ICU discharge.
We hypothesized that patients on nonsurgical wards would benefit the most from the tracheostomy team. However, with a minority of patients on medical wards (n = 20), the small subgroup size may have limited our ability to detect a significant difference in downsizing and decannulation times.
Speaking valve use
The presence of a speech-language pathologist on the team is the major factor accounting for the increase in speaking valve use, as demonstrated in both univariate and multivariate analysis. Patients are known to the speech-language pathologist as soon as the procedure is performed, so evaluations are undertaken earlier. Also, more physician and respiratory therapist input during tracheostomy service rounds helps the speech-language pathologist gauge a patient’s likelihood to tolerate a speaking valve. In patients who immediately tolerate corking after downsizing, there is no need for a speaking valve. However, in our patient population with a high proportion of traumatic brain injuries and borderline level of consciousness, we often have patients who may not tolerate corking but do well with a speaking valve. Although not formally validated, we feel that speaking valve use as soon as appropriate improves patient quality of life.
Conclusion
Making decisions about tracheostomy management requires specialized knowledge. Prior to the establishment of our institution’s tracheostomy team, variable experience levels existed among the medical and nursing staff responsible for the care of patients with tracheostomy tubes on wards. Such a scenario can lead to inconsistent management with the potential for serious complications. With a tracheostomy service, daily tube care can improve through regular expert evaluation and through education of the medical and nursing staff. With a specialized service, decision-making is centralized to those with the required expertise, which leads to more consistent evidence-based management. However, even among those clinicians with experience in tracheostomy care, Stelfox and colleagues6 reported that significant variability in opinions existed concerning the appropriate timing for decannulation. This is true in part because guidelines for tracheostomy management do not exist. Forming a tracheostomy team creates the working group necessary to develop institutional practice guidelines based on current available evidence. A team also provides a platform facilitating research evaluating particular tracheostomy care practices.
While a prospective study with a larger population is required, our study shows that closer follow-up and more consistent management provided by a specialized multidisciplinary tracheostomy team has a favourable impact on tracheostomy care at a large university hospital.
Acknowledgements
We thank the tracheostomy team members: respiratory therapists Caroline Cleary, Josée Gendron, Margaret Moon, Chester Moran, Chantal Rioux and Costa Voutsinas; speech-language pathologists Alena Seresova and Judith Robillard Shultz; clinical nurse specialists Nathalie Rodrigue, Zenith Jiwan and Nancy Tze; and ICU database managers Dr. Ash Gursahaney and Josée McMurray.
Footnotes
Competing interests: None declared.
Contributors: Drs. de Mestral, Fata, Razek and Khwaja designed the study. Dr. de Mestral, Ms. Fong and Ms. LeBlanc acquired the data, which Drs. de Mestral, Iqbal and Khwaja anazlyed. Drs. de Mestral, Iqbal and Khwaja wrote the article. All authors reviewed the article and approved its publication.
- Accepted February 2, 2010.