Abstract
Background: Patient recall of information about procedures, including risks and benefits and potential outcomes, is often insufficient. We sought to determine whether a multimedia educational tool enhances the informed consent discussion for elective neurosurgical procedures by increasing patient knowledge of the procedure.
Methods: Adult patients from a single neurosurgical site eligible for 4 neurosurgical procedures (lumbar spine or cervical spine decompression for degenerative disease, craniotomy for brain tumour or trigeminal neuralgia treatment) were offered enrolment. Patients were randomly assigned to either the control arm (standard consent discussion) or the intervention arm (review of an e-book containing information tailored to their disease/injury plus standard consent discussion). Participants completed a 14-item questionnaire before and after the consent discussion.
Results: Questionnaires were completed by 38 participants, 18 in the control group and 20 in the intervention group. The mean age was 62.2 (standard deviation [SD] 13.6) years and did not differ significantly between the 2 groups. The mean baseline questionnaire scores were similar for the control and intervention groups (20.4 [SD 7.3] v. 20.6 [SD 6.7]). However, the mean scores on the follow-up questionnaire were significantly different between the 2 groups (20.2 [SD 4.0] v. 23.2 [SD 4.9], p = 0.02). There was no change in the scores on the 2 questionnaires in the control group, whereas, in the intervention group, the mean score was significantly higher after the intervention (p = 0.03).
Conclusion: The use of an electronic booklet appears to improve patients’ knowledge of their surgical procedure. The use of multimedia booklets in clinical practice could help standardize and optimize the consent process, ensuring that patients receive the relevant information to make a truly informed decision.
The informed consent discussion is an essential element in the development of the surgeon–patient relationship. It is not only a legal requirement but also a process through which a surgeon must enable a patient to make an autonomous health care decision. The ethical principles of autonomy and right to self-determination are fundamental concepts in this process.1
Informed consent is required across surgical specialties so that patients understand enough about the proposed procedure to make an educated decision as to whether they elect to proceed. However, this notion implies that the surgeon provides the appropriate amount of information to allow full understanding of the procedure and alternatives, and that the patient grasps the content of the information provided. In current medical practice, with less time, fewer resources, increasing subspecialization and more complex procedures, thoroughly educating patients becomes a challenge. The Canadian Medical Protective Association reports that 21% of all legal cases and those involving the Royal College of Physicians and Surgeons of Canada have concerned issues surrounding informed consent.2 Of these cases, 65% involved a surgical case, with 79% resulting in unfavourable outcomes for the surgeon.
It has been shown that, despite physicians’ best efforts to thoroughly transfer knowledge of the procedures, tests, risks, benefits and potential outcomes, this is often insufficient. In a prospective study, Krupp and colleagues2 investigated processing of information by patients undergoing neurosurgical procedures and found that retention of knowledge regarding potential risks was less than 20% only 2 hours after a standardized consent discussion. Similarly, Muss and colleagues3 reported that one-third of patients with cancer receiving chemotherapy were unable to name the drugs they received, and a substantial proportion were not aware of the purpose of chemotherapy or its potentially lethal complications. They also reported variability in the ability of patients to remember adverse effects despite standardized information delivery and standard questions used in the interview.
Incomplete understanding of a procedure limits patient autonomy and negates the basic principles of informed consent. The aim of this study was to evaluate whether using a multimedia educational tool with custom-made interactive booklets enhances patients’ knowledge before their decision to undergo surgery.
Methods
Study design
This study was approved by the Research Ethics Board at Sunnybrook Health Sciences Centre, Toronto. The study randomly allocated participants to either the standard consent (control) arm or the e-consent (intervention) arm. It was conducted from September 2014 to October 2016.
Participants
Eligible adult patients were offered enrolment through an urban outpatient neurosurgical clinic at Sunnybrook Health Sciences Centre. Patients who were referred for surgical consultation for one of the following elective neurosurgical procedures were offered participation: 1) lumbar spine decompression for degenerative disease, 2) cervical spine decompression for degenerative disease, 3) craniotomy for brain tumour or 4) trigeminal neuralgia treatment. Patients were eligible for inclusion if they were appropriate surgical candidates based on imaging and clinical history, had the cognitive capacity to consent, understood and spoke English or had an accompanying interpreter, and had no previous consultation for an elective neurosurgical procedure.
Protocol
Following the surgeon’s review of referral information, imaging and medical history, consent for research participation was obtained by the study coordinator. Participants were then randomly assigned in a 1:1 ratio to either the standard consent (control) arm or the e-book plus standard consent (intervention) arm by a research coordinator using a Web-based randomization tool (www.randomizer.org/). The surgeon was blinded as to group allocation.
All participants completed a 14-item questionnaire before the encounter with the surgeon (Fig. 1). We created the questionnaire based on research evaluating patient knowledge following informed consent discussions in cardiac surgery.4 Each question was rated on a scale of 0 to 3, with higher scores reflecting more detailed answers. Questions were tailored to each surgical procedure, and responses provided a measure of general comprehension about the disease or injury, surgical approach, risks of morbidity/mortality, expectations for recovery, postoperative pain and alternative options.
Excerpt of cervical spine decompression questionnaire.
Participants allocated to the control group then had a routine discussion with the surgeon regarding the surgical procedure in which the rationale, process, potential risks and benefits, and alternative options were reviewed. Participants allocated to the intervention group reviewed on a mobile tablet (iPad, Apple Inc.) an e-book containing information tailored to their disease or injury. They were given 7–10 minutes to review the material, after which the standard consent discussion with the surgeon took place.
After the consent discussion with the surgeon, all participants completed a second questionnaire with the same 14 questions in a new sequence to evaluate retention.
E-book
We used an existing iPad application (iBooks, Apple Inc.), content from a standard neurosurgical textbook5 and the surgeon’s training to develop interactive multimedia content for the selected procedures. Each e-book included comprehensive yet plain-language explanations of the disease or injury, potential surgical intervention and rationale, risks and benefits, recovery times and alternative treatments. The e-books incorporated pictures and short videos (Fig. 2). The content covered the most frequently asked questions patients have during standard interviews for surgical consent, as determined by the clinical experiences of 3 surgeons (L.D. and 2 other staff neurosurgeons from Sunnybrook Health Sciences Centre). The preliminary development of the tool was done in English; translation into other languages is intended for future versions. The e-books were pilot tested among student volunteers with no medical training. Based on their feedback, wording was reduced where necessary for brevity.
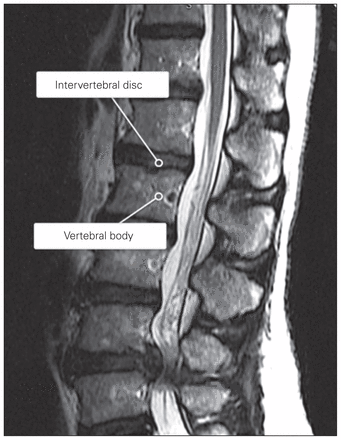
Sample e-book depiction of degenerative disc disease, lumbar spine.
Sample size and statistical analysis
This investigation involved patients from a single neurosurgical site. To evaluate the utility of the pilot e-book, a feasibility sample of 40 participants was planned.
We performed statistical analysis using Stata 14 (Stata-Corp). Descriptive analysis was conducted. Continuous variables are presented as means with standard deviations (SDs), and dichotomous data as frequencies and percentages. We compared means using 2-tailed t tests (unequal variance), and the level for accepting statistical significance was set at 0.05. Variables were compared within groups and between groups. We analyzed questionnaire answers individually and as total scores.
Results
Questionnaires were completed by 38 participants, 18 (47%) in the control group and 20 (53%) in the intervention group (Table 1). The mean age was 62.2 years (SD 13.6 yr) and did not differ significantly between the 2 groups. Twenty participants (53%) were men. The diagnoses are shown in Table 1.
Participant characteristics and baseline questionnaire scores
The mean baseline questionnaire scores were similar for the control and intervention groups (20.4 [SD 7.3] v. 20.6 [SD 6.7], p = 0.5]). However, the mean scores on the follow-up questionnaire were significantly different between the 2 groups (20.2 [SD 4.0] v. 23.2 [SD 4.9], p = 0.02). Within-group comparison of the scores on the baseline and follow-up questionnaires indicated no change in the control group (p = 0.8), whereas, in the intervention group, the mean score was significantly higher after the intervention (p = 0.03).
Discussion
Obtaining informed consent for surgical procedures or invasive diagnostic tests is mandatory for health care practitioners. It is the legal and ethical responsibility of the treating physician before any health care intervention, whether for clinical or research purposes. Patient autonomy is a basic assumption of proper informed consent6 and can be defined as “the capacity (of a person) to govern herself, to make choices … unimpeded by the choices and goals of others.”7
Thorough and appropriate delivery of information to ensure patient understanding is vital to the consent process. Studies have shown that retention of information is often insufficient and that patients frequently consent to procedures they do not fully understand.2,5,8,9
True informed consent for surgical procedures requires comprehension, assimilation and retention of information. However, many factors, such as preoperative anxiety, level of education, readability of consent forms and language limitations, may impede the full process.8,10,11 Anxiety and psychological distress related to a perceived risk of death or disability are common preoperatively.12,13 This, combined with a large volume of new information and the pressure of time constraints for a decision, often results in patients’ being overwhelmed and distressed14 and might affect the assimilation of information during the informed consent interview.
It must be emphasized that the current study does not suggest that an electronic tool can replace the essential dialogue between the surgeon and the patient but, rather, enhance it, in accordance with the College of Physicians and Surgeons of Ontario’s Consent to Treatment policy15 based on the Ontario Health Care Consent Act. The ethical and legal obligation of the surgeon to explain, educate and obtain consent can be better fulfilled if the patient has an opportunity to become informed in advance in a leisurely manner.
Before the availability of electronic tablets, the use of audiovisual tools was shown to improve patient understanding and indirectly benefit the communication between patients and health care providers.16 More recently, Sahyouni and colleagues17 used the same platform that we did (iPad) to deliver information to outpatients with traumatic brain injury. They found that the use of an interactive iBook-based education tool resulted in better self-reported knowledge scores and an enhanced clinical experience compared to the standard information pamphlets routinely used in the clinic. Similar trends were shown among patients undergoing elective cholecystectomy. 17 Our findings indicate that patients who used the e-book appeared to retain more information than those who did not use the e-book. Interestingly, patients in the control group scored the same before and after the consent discussion, which indicates that little (if any) new information was gained or retained. This suggests that, even when the same content is delivered to 2 groups, the e-consent process with an audiovisual component and self-controlled pace may enhance acquisition and retention of information. Patients can tailor their preferred way of learning (e.g., reading, animation or illustrations) and have enough time to understand the information and to formulate questions. Also, the delivery of information before the encounter with the surgeon provides sufficient background, enabling the patient to formulate context-appropriate questions during the discussion with the surgeon. Interestingly, in addition to higher knowledge scores, patients undergoing cholecystectomy who received multimedia consent during the surgical consultation reported a “better experience” during the consent process.18
Much work has been done to evaluate the perception of risk and benefit, although much more is required. Very different risk expectations are reported by patients compared to those described by their surgeon, even when known statistics are provided.18–20 This holds true for procedures such as carotid endarterectomy,19 for which there are well-established risks associated with conservative and surgical intervention derived from multicentre trials.19,20
Complex surgical procedures and medical legal requirements contribute to the creation of lengthy consent forms that are difficult to read. A retrospective computerized analysis of the readability of over 500 clinical and research consent forms suggested that an estimated 15 years of formal education was required for understanding.11 In addition, increasing cultural diversity introduces language barriers into the informed consent process. According to the 2011 census, more than 200 languages are spoken in Canada, and 20.6% of Canadians reported a mother tongue other than English or French.21 In a survey of 444 Harvard University medical students, only 20% reported feeling well prepared to care for patients with limited English-language proficiency.22 As cultural demographic characteristics evolve, more attention must be paid to making the technical and legal attributes of the consent process more accessible to patients.
The availability of information on the Internet can be detrimental if the information is taken out of context or misinterpreted. Providing supplemental information to patients that is vetted by a surgeon and tailored to a particular patient or high-risk population may reduce the likelihood of misinformation.
It should be noted that, even though the use of the electronic booklet improved patients’ understanding in the current study, scores were still below what one might expect. This is similar to the highest scores reported in a meta-analysis evaluating patients’ understanding of informed consent for surgery and clinical research23 and indicates that ample room for improvement in the consent process remains. Comprehension and learning are affected by age, education, intelligence, cognitive function, locus of control, desire for detail and anxiety.8 The necessity to tailor consent discussions to accommodate all of these variables underlines the need for supplementary material.
Limitations
Important limitations to this work should be noted. First, the sample was small, and statistical matching of patients according to surgical subgroup was not feasible owing to variation in surgical referrals. For consistency in this preliminary evaluation, we used a single surgeon’s clinic; future study will provide an updated version using multiple sites. In addition, matching for educational background was not realistic within the clinic population; however, participants who had previously taken part in surgical consent discussions were not enrolled. Patients’ knowledge was evaluated at 2 time points within 20–30 minutes of one another, and differences in short-term memory would have been reflected in the scores. Finally, we do not consider the questionnaire scores to reflect patient understanding, which is beyond the scope of this research, but, rather, a reflection of new information gained.
Conclusion
Many factors, including time and resource constraints, increasing language diversity, patient education level and patient anxiety, challenge the informed consent dialogue around high-risk surgical procedures. Our findings suggest that the use of an e-book can enhance knowledge retention and the informed consent process. Optimizing the process so that it is both thorough and efficient may alleviate some time constraints in busy surgical clinics while simultaneously minimizing patient anxiety. An adjunct multimedia tool such as the e-book used in the current study may also benefit patient autonomy in the decision to accept inherent risks and proceed with the surgical treatment. The consistency of the material delivered with such a tool would ensure that all patients receive thorough background information, enabling a truly informed decision. Enhancing knowledge and autonomy may, in turn, promote patient engagement. One can expect that appropriate education will strengthen the patient–surgeon relationship, reduce additional follow-up visits and limit potential medicolegal issues.
Footnotes
Funding: This work was supported by grant SHS-13-009 from the Academic Health Sciences Centre Alternative Funding Plan Innovation Fund.
Competing interests: None declared.
Contributors: A. Bethune and L. da Costa designed the study. A. Bethune, M. Davila-Foyo and M. Valli acquired the data, which L. da Costa analyzed. All authors wrote and reviewed the article and approved the final version for publication.
- Accepted January 22, 2018.