1. AUDIT OF PATHOLOGY REPORTING FOR RECTAL CANCER IN BC
We reviewed the pathology of 933 rectal cancer specimens in BC for the years 1996 and 2000. Pathology reports were assessed for inclusion of data elements now used as standard reporting for rectal cancer in view of the surgical technique total mesorectal excision including radial margins and lymph-node examination in at least 12 nodes.
We found that pathology reports routinely assessed tumour size (95%), distal margin (80%), layer of bowel wall invasion (99%), differentiation (97%), and lymphatic and vascular invasion (90%). However, radial margin was assessed in only 48% of reports and the average number of lymph nodes assessed was 7. Assessment of intactness of the mesorectal fascia was given in 9% of reports. High-volume hospitals (> 10 rectal cancer cases per year) compared to low-volume hospitals assessed a higher percentage of radial margins (49% v. 26%, p = 0.002) and lymph nodes (7.0 ± 5 v. 5.1 ± 4, p = 0.02).
Therefore, BC pathologists need to improve their reporting of rectal cancer specimens in order for us to better understand the quality of our surgical technique of mesorectal excision and to improve staging for recommendation of adjuvant treatment and prognosis.
2. VITAMINS AND MINERALS FOR THE PREVENTION OF COLORECTAL ADENOMAS AND CANCER
We have conducted a systematic review of the effect of vitamins and minerals for the prevention of colorectal adenomas (CRAs) and cancer (CRC).
We identified randomized controlled trials (RCTs) up to April 2003. All subjects had no previous history of CRC. Interventions included all vitamins and minerals. The primary outcomes were the number of subjects with at least 1 CRA, the change in polyp burden, or CRC. The secondary outcome was adverse events. Two reviewers independently extracted data and assessed trial quality. The outcomes were reported as relative risks (RRs) and the number needed to treat or harm (NNT or NNH) with 95% confidence intervals (CIs). The data were combined with the fixed effects model if it was clinically and statistically reasonable. The primary outcomes for secondary prevention trials for subjects with familial adenomatous polyposis (FAP) were analyzed descriptively only.
Twelve trials with 109 FAP and 55 766 population subjects met the inclusion criteria. The interventions included beta carotene, vitamin C, E, A, selenium, folic acid and calcium. For the primary prevention trials, there was no statistically significant difference between the intervention and control groups for the number of subjects who developed at least 1 CRA (RR 1.47 [95% CI 0.97, 2.23]) or CRC (RR 0.91 [95% CI 0.76, 1.09]) in the general population. For the secondary prevention trials, there was a statistically significant reduction for the number of subjects who developed at least 1 sporadic adenoma with calcium (RR 0.82 [95% CI 0.69, 0.98]; NNT 17 [95% CI 9, 100]). There was a statistically significant increase in minor adverse events in the intervention groups (RR 1.22 [95% CI 1.15, 1.29]; NNH 33 [95% CI 25, 50]).
There is evidence from RCTs to suggest that calcium, but not other vitamins or minerals, reduces the recurrence of adenomatous polyps in the general population.
3. IMPROVED LOCAL REGIONAL CONTROL OF RECTAL CANCER WITH TME AND ADJUVANT CHEMORADIATION
Local regional recurrence is a devastating outcome following radical curative resection of rectal cancer. The combination of mesorectal excision and adjuvant radiation therapy has reduced the incidence of pelvic recurrence dramatically. The aim of this study was to examine the local regional recurrence rates in a large urban centre as they relate to the introduction of the technique of mesorectal excision with selective use of adjuvant chemoradiation.
From January 1994 to December 2001, 238 patients underwent surgery for rectal cancer, 177 of these for cure. 109 were male with a mean age of 68 (range 36–97). Median follow-up was 36 months. Procedures included 128 anterior resections (mean anastomotic height 7.4 cm), 45 abdominoperineal resections (mean tumour height 3.5 cm) and 4 Hartmann’s.
Local recurrence occurred in 7 patients (4.0%); 5 of 91 (5.5%) without adjuvant radiation and 2 of 86 (2.3%) with adjuvant radiation. Of 44 patients receiving preoperative radiation, none developed a local regional recurrence, while only 2 of 42 patients receiving postoperative radiation developed a local regional recurrence. All but 1 of the recurrences were in T3 or T4 tumours. The addition of adjuvant therapy to these high-risk tumours decreased the local recurrence rate from 9.8% (4 of 41) to 2.7% (2 of 75).
Mesorectal excision alone achieves local regional recurrence rates that are superior to historical controls. The addition of adjuvant chemoradiation improves overall local regional recurrence and has its greatest effect in high risk T3 and T4 tumours.
4. NONSTEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDS) AND ASPIRIN FOR THE PREVENTION OF COLORECTAL ADENOMAS AND CANCER
We have conducted a systematic review of the effect of NSAIDS on the outcome of colorectal adenomas (CRAs) and cancer (CRC).
We identified randomized controlled trials (RCTs) up to April 2003. All subjects had no previous history of CRC. NSAIDS and Aspirin were the interventions. The primary outcomes were the number of subjects with at least 1 CRA, the change in polyp burden, and CRC. The secondary outcome was adverse events. Two reviewers independently extracted data and assessed trial quality. The outcomes were reported as relative risks (RR) and the number needed to treat or harm (NNT or NNH) with 95% confidence intervals (CIs). The data were combined with the fixed effects model if it was clinically and statistically reasonable. The primary outcomes for secondary prevention trials for subjects with familial adenomatous polyposis (FAP) were analyzed descriptively only.
Seven trials with 150 FAP and 23 236 population subjects met the inclusion criteria. The interventions included sulindac, celecoxib, or Aspirin. For the primary prevention trials, there was no statistically significant difference between the intervention and control groups for the number of subjects who developed at least 1 CRA in the general (RR 0.87 [95% CI 0.68, 1.10]) population groups. For the secondary prevention trials, there was no difference between groups in the number of subjects who developed at least 1 recurrence of sporadic CRAs (RR 0.88 [95% CI 0.77, 1.02]) or whose CRAs regressed (RR 1.67 [95% CI 0.45, 6.14]). FAP subjects who received NSAIDs had a greater proportional reduction (range: 11.9%–44%) in the number of CRAs compared to those in the control group (range: 4.5%–10%). There was no difference in the outcomes of CRC or adverse events.
Overall, there is no evidence from RCTs to support the effectiveness of NSAIDS or Aspirin for reducing the incidence or recurrence of sporadic adenomatous polyps. There is short-term evidence to support regression, but not elimination or prevention of CRAs in FAP.
5. THE ROLE OF HOME TPN IN THE MANAGEMENT OF ENTEROCUTANEOUS FISTULAE: A PARADIGM SHIFT
The standard management of enterocutaneous fisulae is currently a 6-week trial of bowel rest with conservative medical intervention, including octreotide and total parenteral nutrition (TPN), and subsequent surgery if spontaneous closure has not occurred. This may not be a sufficient interval to allow for spontaneous closure of fistulae or preoperative patient nutrition optimization, despite a prolonged hospital stay. The experience of the Home Parenteral Nutrition [HPN] Program at a single academic centre is retrospectively reviewed. In the first 6 years, the program has processed 197 new patient consults, resulting in 115 patients receiving TPN at home. Twenty of these patients had enterocutaneous fistula as the primary indication for initiating HPN, 18 of whom have finished their course of TPN to date. Nine of 18 patients had initial successful closure of fistula, 4 nonoperatively. Three of 18 patients whose fistulae closed eventually recurred and required further intervention. The average time on HPN for all 18 patients was approximately 7 months. This study provides a descriptive analysis of one institution’s experience. The availability of HPN provides an opportunity to allow adequate time for nonoperative closure of enterocutaneous fistulae whilst also providing sufficient nutritional optimization for patients who may eventually require surgery. Further prospective investigation on the role of HPN in patients with refractory enterocutaneous fistulae is required before this can be recommended for routine use.
6. THE ARTIFICIAL BOWEL SPHINCTER — A PROCEDURE WITH A STEEP LEARNING CURVE, AND SATISFACTORY PATIENT OUTCOMES
The artificial bowel sphincter is currently being implanted by designated surgeons for the management of neurogenic fecal incontinence refractory to conservative management and other surgical techniques. Since 1998, we have implanted 11 devices in 10 female patients (1 complete revision). The longest follow-up is 4fi years. Two patients had had a colostomy preoperatively as the initial management of their incontinence. At present, all devices are in place and there are no infections. One of the 10 patients required removal of the device because of cuff erosion through the skin, and the device has since been reimplanted successfully. One patient is awaiting colostomy closure and 1 is awaiting activation of the device. The devices are fully functional in 8 patients. All 8 patients report a satisfactory degree of sphincter control and have a good quality of life. The most common significant problem postoperatively has been impaction and constipation secondary to obstructed defecation, requiring revision of the cuff to a larger diameter cuff in 3 patients. In contrast to the international literature describing a 30% infection rate requiring explantation of the device, the only infection in our series was secondary to cuff erosion. In this pilot project, we conclude that the artificial bowel sphincter implantation procedure requires familiarity with the device, careful follow-up, and willingness to revise the device to achieve continence. With appropriate revisions and modifications of surgical technique, we believe from this pilot project that the ABS device will be very useful in the management of fecal incontinence in the future.
7. THE IMPACT OF MEDICAL THERAPY AND PELVIC POUCH SURGERY ON REPRODUCTIVE ABILITY IN WOMEN WITH ULCERATIVE COLITIS
While ulcerative colitis (UC) commonly affects young women, the impact of UC and its treatment on female reproductive ability have not been well studied. The purpose of this research was to measure the infertility rate in women with UC treated with medical therapy alone or ileal pouch anal anastomosis (IPAA), and to compare the ability of women to become pregnant before and after diagnosis with UC and before and after IPAA.
Based on age at surgery and marital status, 77 women who had medical treatment and 158 women who had IPAA for UC were identified for retrospective review. Data were collected by mail questionnaire and phone interview. Married or cohabiting women aged 18–44 who failed to become pregnant after 12 months of unprotected intercourse were defined as infertile.
Complete data were available for 67 (87%) of the medically treated patients and 147 (93%) of the IPAA patients. In the medically treated group 9/67 (13.4%) women reported an episode of infertility compared to 56/147 (38.1%) women after IPAA (p < 0.001). In the IPAA group 44 (78.6%) of the episodes of infertility occurred after surgery. In the medically treated patients, 39/39 (100%) women who tried to become pregnant prior to diagnosis with UC were successful, compared with 40/41 (97.5%) women after diagnosis (p = 0.51). Prior to IPAA, 90/94 (95.7%) women trying to become pregnant were successful compared with 34/62 (54.8%) after IPAA (p < 0.001). There was a significant difference in the use of fertility treatments before and after IPAA (4/94 [4.3%] v. 18/62 [29%] respectively, p < 0.001).
Prior to IPAA for UC, women experience high rates of pregnancy, suggesting that UC and medical treatment do not impact on reproductive ability. After IPAA, difficulty becoming pregnant is a common problem and should be discussed routinely with patients considering this procedure.
8. ACCURACY OF LOCOREGIONAL STAGING OF RECTAL ADENOCARCINOMA AT LONDON HEALTH SCIENCES CENTRE
Preoperative staging of rectal cancer using the current gold standard of transrectal ultrasound (TRUS) is essential for planning optimal therapy, including the addition of neoadjuvant therapy and type of surgical resection.
This retrospective study evaluated the accuracy of TRUS in the preoperative staging of 24 patients with rectal cancer who underwent surgery at our institution from 1998–2002. Two patients had TRUS performed on 2 different occasions and each ultrasound result was evaluated for accuracy for a cumulative total of 26 TRUS and histopathologic results. Based on TRUS results, 9 cases required neoadjuvant therapy and 17 cases did not receive neoadjuvant therapy. Subsequent surgical resection involved 5 different procedures including 6 transanal excisions and 20 radical proctectomies. Following surgical resection, in groups with and without neoadjuvant therapy, histopathologic stage was compared with ultrasound staging.
Overall accuracy in assessing tumour (T) stage was 39%, the majority of which were understaged (94%). As a result of understaging, 62.5% (10/16) of patients were not considered for potentially beneficial neoadjuvant therapy. Overall accuracy in assessing nodal involvement (N) was 59%, 87.5% of patients inaccurately staged were understaged. Neoadjuvant therapy was not received by 50% (4/8) of patients as a result of nodal understaging.
In conclusion, the accuracy of TRUS in locoregional staging of adenocarcinoma is clearly lower at London Health Sciences Centre than that reported in the literature. As TRUS is an essential staging modality in rectal cancer, a review of local TRUS equipment and protocols is required to ensure patients receive appropriate neoadjuvant therapy and subsequent surgical procedures. An awareness of the limitations of TRUS at our institution should improve staging accuracy and contribute to optimum clinical decision-making.
9. A POPULATION-BASED SURVEY OF PATTERNS OF CARE FOR COLORECTAL CANCER — PRELIMINARY FINDINGS
To evaluate utilization of health resources for colorectal cancer, we performed a retrospective chart review of all incident cases registered in 1999 in a defined Quebec region.
Of 696 cases, 186 (27%) were available for this analysis. Mean age (68) and sex distribution (50\50) were comparable to that of the entire population. There were 155 colon and 31 rectal neoplasms.
Preoperative visits were done in the emergency room in 35% of cases. Surgery was performed on 89% of 165 evaluable patients. The median length of stay (LOS) was 11 days overall and 8.5 days postoperatively. The 54th and 74th percentile for intraoperative blood loss were 200 mL and 400 mL, respectively. Approximately 15% of patients received at least 1 transfusion. The median number of transfusions prior to, on the day of surgery and postoperatively were respectively 3, 2 and 2 units. An ICU stay was noted in 31% of cases.
Chemotherapy was administered to 38% of patients, and a dose reduction recorded in one third. Radiation therapy was delivered to 11/31 rectal cancer patients. The number of fractions received varied (18–30), while the total dose was more constant (50–54 Gy).
This preliminary study indicates that health resources are not utilized efficiently in comparison to single-institution series. We also noticed frequent dose reductions with adjuvant chemotherapy and dose variation in the administration of radiation therapy that are warranted of future inquiries. Transfusions are not commonly used, but we were not able to estimate the prevalence of anemia at this stage.
10. PREFERENCES AND ATTITUDES OF COLORECTAL SURGEONS TOWARDS OFFICIAL RECOMMENDATIONS OF THE AMERICAN CANCER SOCIETY FOR COLORECTAL CANCER SCREENING
The purpose of this study is to assess the preferences and attitudes of colorectal surgeons with respect to the American Cancer Society’s guidelines for colorectal cancer screening and determine what they do in their clinical practices as well as in their personal lives.
A questionnaire was sent to 300 ABCRS certified colon and rectal surgeons in the United States and Canada. Results were analyzed with respect to agreement with the American Cancer Society guidelines and what screening methods surgeons use in their clinical practice and in their personal lives.
Of surgeons who agree with American Cancer Society guidelines, 95% follow them in high-risk individuals and 74% follow them with average-risk patients. Surgeons recommend colonoscopy exclusively to their average-risk patients 22% of the time. Surgeons who are average-risk chose colonoscopy 71% of the time when getting screened themselves and recommend it 75% of the time to their average-risk relatives. Of surgeons who recommend only colonoscopy to family members, 71% did not recommend only colonoscopy to average-risk patients (p = < 0.0001). Of surgeons who have not yet been screened, 96% plan a colonoscopy as their screening test. 67% of surgeons prefer colonoscopy as the primary screening test for average-risk individuals. No colorectal surgeons choose fecal occult blood testing as the primary screening modality for their patients or themselves.
There is less agreement among surgeons with respect to screening average-risk individuals than when screening high-risk individuals. Colon and rectal surgeons choose colonoscopy more commonly for screening themselves and their families than when screening their patients. The majority of colon and rectal surgeons prefer colonoscopy as the primary screening modality for average-risk individuals.
11. FUNCTIONAL ANALYSIS OF HUMAN MLH1 MISSENSE MUTATIONS USING SACCHAROMYCES CEREVISAE
Newly described functional assays are utilized to characterize 2 hMLH1 mutations: T117M and R182G. The reproducibility and validity of the results indicate that these assays may be used in a clinical setting for HNPCC genetic testing.
Saccharomyces cerevisiae were transformed with hMLH1 cDNA expression vectors containing either mutation. The presence of functional hMLH1 produces an accumulation of mutations in mismatch repair (MMR)-proficient yeast due to MLH1 protein homology and interference with normal MMR (dominant mutator effect). The transformants were tested for increased mutation rates using 3 assays: mutation of the gene for canavanine resistance (CAN1), reversion of the hom 3–10 allele, and insertion-deletions at a dinucleotide repeat regulating expression of beta-galactosidase.
Wild-type (WT) hMLH1 have an increased CAN1 mutation rate as well as an increased hom 3–10 reversion rate when compared to yeast transformed with vector alone. When expressed in conjunction with the lacZ reporter vector, pCIZ1, the transformed yeast colonies stain blue in the presence of X-gal, indicating that the lacZ reading frame is in-frame. The T117M mutation reduces or completely eliminates the dominant mutator effect when tested in the CAN1 mutation rate and hom 3–10 reversion rate assays. When expressed in conjunction with pCIZ1 the transformed yeast colonies do not stain blue in the presence of X-gal. The R182G mutation maintains a dominant mutator effect in all of the assays.
Based on the results of these assays T117M is likely a functional mutation while R182G may be a polymorphism. We conclude that this assay may be applicable as an adjunct in genetic testing for HNPCC.
12. POUCH–VAGINAL FISTULA AFTER ILEAL POUCH–ANAL ANASTOMOSIS
Pouch–vaginal fistula (PVF) is an uncommon but serious complication after ileal pouch–anal anastomosis (IPAA). The purpose of this study was to examine the risk factors associated with early and late PVF and to compare the management and outcomes for each group.
Patients who developed PVF after primary IPAA at Mt. Sinai Hospital were eligible for inclusion and were identified from the Inflammatory Bowel Disease database. Early fistulae were defined as those developing within 3 months of surgery, and late developing after 3 months.
Since November 1982, 25/619 (4%) women undergoing primary IPAA at Mt. Sinai Hospital have developed a PVF. An early fistula was diagnosed in 14 patients after a mean of 1.1 months (range 0–3), while late fistulae were diagnosed in 11 patients after 21.7 months (range 4–106). All patients with early fistulae had a J pouch with a stapled anastomosis and a diagnosis of ulcerative colitis. In comparison, 4/11 (36%) patients with late fistulae had Crohn’s disease or indeterminate colitis, 3/11 (27%) had S-pouch construction and 3/11 (27%) handsewn anastomosis. A diverting ileostomy was created at IPAA in 7/14 (50%) patients with early fistulae compared to 8/11 (72.7%) patients with late fistulae. Early fistulae were treated with ileostomy in 6 (43%) patients, fistula repair in 3 (21%) and pouch reconstruction in 7 (50%). Late fistulae were treated with a diverting ileostomy in 4 (36%) patients, fistula repair in 6 (55%) and reconstruction in 4 (36%). Pouch excision was performed in 3 (21%) patients with early fistulae and 3 (27%) with late fistulae, for an overall failure rate of 24%.
Late pouch–vaginal fistula appears to be associated with a diagnosis of Crohn’s disease or indeterminate colitis. Treatment for pouch–vaginal fistula is variable, most patients require multiple interventions and pouch salvage is possible for the majority of patients.
13. PREFERENCES AND PRACTICE FOR COLORECTAL CANCER SCREENING
The purpose of this study was to determine the screening preferences and practice patterns for colorectal cancer (CRC) and the barriers that affected such patterns. We surveyed 196 family physicians in London, Ont., and had a response rate of 79%.
Barriers to colorectal cancers were felt to be lack of resources (49%), patient resistance (32%) and lack of time to discuss with patients screening issues (16%). Only 68% of respondents screened average-risk patients. While 57% reported a screening preference for colonoscopy, only 4% used colonoscopy in practice. This was in contradistinction to the fecal occult blood test (FOBT), which was the preferred screening method by only 28% but was used by 91% of respondents.
High-risk individuals were screened by 97% of physicians surveyed. If resources were not a limitation, colonoscopy was the preferred screening test for high-risk individuals as reported by 79% of the respondents. However, in practice only 47% chose colonoscopy and 46% used an FOBT based screening method even in high-risk individuals. Most of the FOBT-based screening tests were performed in conjunction with digital rectal examination rather than testing spontaneously passed stool as recommended in screening guidelines.
CRC is a major health concern for general surgeons. Limited access to endoscopic procedures is resulting in practice patterns that are not in agreement with screening guidelines for high-risk patients nor in agreement with the preferred practice of referring physicians. A significant percentage of physicians do not screen average-risk individuals for CRC and when such patients are screened it is with methodologies not endorsed in guidelines.
14. OBESITY AND SEVERE OBESITY IS NOT A BARRIER FOR COLORECTAL SCREENING OR DIAGNOSTIC PROCEDURES
The objectives were to determine if obesity is a barrier to completion of colorectal (CRC) screening tests or diagnostic gastrointestinal procedures.
Subjects included 1749 survey respondents, 50 to 75 years of age that were randomly selected from Ontario and Seattle by the NIH Cooperative Family Registries for Colorectal Cancer Studies. The proportion of nonobese (body mass index [BMI] < 30 kg/m2), obese (BMI ≥ 30 and < 40 kg/m2) or severely obese (BMI ≥ 40 kg/m2) individuals who had fecal occult blood testing (FOBT) or endoscopy for screening or diagnostic purposes was determined. Univariable analyses and multivariable logistic regression were performed.
The 3 BMI groups were similar with respect to baseline demographics and family history of CRC. There was no statistically significant difference between rates of FOBT or endoscopy for screening or diagnostic purposes between obese and nonobese subjects. There was a nonstatistically significant trend, where severely obese individuals compared to nonobese individuals were more likely to obtain FOBT for screening (OR 1.4 [95% CI 0.7, 2.7]) and diagnostic (OR 2.2 [95% CI 0.0, 5.0]) purposes or endoscopy for screening (OR 1.4 [95% CI 0.7, 2.8]) and diagnostic (OR 1.4 [95% CI 0.7,2.9]) purposes. In a descriptive multivariable model, living in Seattle compared to Ontario (OR 6.6 [95% CI 5.0, 8.7]) and family history of CRC (OR 2.2 [95% CI 1.4, 3.5]) were significant predictors of CRC screening.
Obesity or severe obesity does not appear to be a barrier to obtaining CRC screening or diagnostic gastrointestinal procedures. The factors influencing CRC screening are the same in the obese and nonobese individuals.
15. PATIENT’S PREFERENCES FOR ADJUVANT POSTOPERATIVE CHEMORADIATION THERAPY IN RECTAL CANCER
Patients treated for colorectal cancer were asked to choose between 2 scenarios of adjuvant treatment after surgery for rectal cancer. Their willingness to trade off side-effects for treatment efficacy was evaluated.
A cohort of 47 volunteers previously treated for a lower gastrointestinal malignancy was prospectively interviewed. We constructed a probability trade-off tool that compared a treatment strategy including or excluding postoperative chemoradiation therapy. Health states between treatment arms were based on a detailed analysis reported in the literature. Using visual aids and a standard interview protocol, the test was initiated with a 10% local recurrence rate for both arms. The age and sex distribution was comparable with the overall colon cancer population. Rectal cancer had been diagnosed in 20 respondents. Chemotherapy was administered to 76% of the cohort and radiation therapy to 51%. We observed 4 modes to the distribution of switch points, graded from each extreme. The median and mean switch points selected were respectively 5% and 4%, a value reflecting the critical local recurrence rate acceptable. The important items that influenced decisions were the effects on bowel function, the possibility of pain and fatigue. Eighty-one percent of respondents were willing to participate in a clinical trial to examine the role of radiation therapy in rectal cancer.
This small sample size suggest that patient’s preferences for adjuvant radiation therapy varies between individuals. A 5% local recurrence rate was the median value chosen as a reasonable trade-off with the long-term side-effects on bowel function. The majority of patients saw this issue as a relevant one to further investigate in clinical trials.
16. INCREASED COLORECTAL CANCER RISK IN PATIENTS WITH CHRONIC LYMPHOCYTIC LEUKEMIA
To determine if patients with chronic lymphocytic leukemia (CLL) develop colorectal cancer (CRC) at a rate greater than the general population.
We reviewed the Saskatchewan Cancer Registry for patients diagnosed with CRC or CLL between 1971 and 2000. Patients were grouped according to age. To determine the risk of developing CRC in patients with CLL, we calculated the hazard using a life-table analysis approach. To determine the risk of developing CRC in the general population, we used population incidence rates derived from the Registry and Saskatchewan population data. Standard errors were calculated using the Delta method for both sets of data.
Between 1971 and 2000, 16 793 patients developed CRC and/or CLL. Of the 1666 patients who were 45 or over and first diagnosed with CLL, 30 patients developed CRC. There were 4 cases in the 45–64 age group (out of 476 patients with CLL), and 26 cases in the 65+ age group (out of 1190 patients with CLL). Using life-table analysis, the population risk (per 100 000) of developing CRC was 106.9 in the 45–64 age group and 424.8 in the 65+ age group. The relative risk (RR + [95% CI]) was 1.6 (0.6, 4.3) and 1.6 (1.1, 2.4) for the 45–64 and 65+ age groups respectively.
Patients greater than 65 years of age with a prior diagnosis of CLL appear to be at a higher risk of developing CRC than the general population; thus, careful screening for colorectal cancer may be indicated in these patients.
17. RECTAL CANCER SURGERY IN BC — OUTCOME IMPROVEMENT STRATEGIES
Outcomes of rectal cancer patients in BC in 1996 were suboptimal relative to current published standards using preoperative radiation and total mesorectal excision (TME). The objective of our interdisciplinary group is to improve outcomes for rectal cancer patients in BC by seeking acknowledgment of the problem of high recurrence and encouraging collaboration from surgeons to use these techniques.
We asked surgeon representatives from hospitals performing 10 or more rectal cancer operations to provide the number of surgeons performing rectal cancer surgery and numbers who have taken a technical TME course, were willing to take our technical TME course, and numbers using preoperative radiation.
Fourteen hospitals were identified as performing 10 or more rectal cancer operations per year. Of 80 general surgeons in these hospitals, 9 were dedicated to other subspecialties and were not performing rectal cancer surgery. Thirty-nine surgeons attended our technical TME course last year; the remainder except 1 will take a future course. All surgeons but 1 will arrange for preoperative staging imaging and refer patients for consideration of preoperative radiation.
Surgeons in high-volume hospitals are collaborating by taking a technical TME course and by referring patients for consideration of preoperative radiation. This collaboration will capture about 80% of rectal cancer cases in BC. We hope that about 55 surgeons in low-volume hospitals will adopt our rectal cancer strategies through our communications. We anticipate that rectal cancer outcomes will improve in BC as a result of surgeons participating in our educational and outcomes feedback programs.
18. BREAST RECONSTRUCTION AFTER MASTECTOMY: A SURVEY OF CANADIAN GENERAL SURGEONS
To ascertain the factors influencing a surgeon’s decision to refer for post-mastectomy breast reconstruction and concerns general surgeons may have about breast reconstruction. To outline what percentage of mastectomy patients get breast reconstruction (immediate or delayed) in Canada.
A postal survey of all general surgeons registered by the Royal College of Physicians and Surgeons of Canada was conducted. A questionnaire involving hypothetical criticism of breast reconstruction received a 54% response.
Age, anticipated psychosocial morbidity, the need for adjuvant therapy and comorbid conditions influenced referral for breast reconstruction. Respondents mentioned patient preference as the most important factor in referring a patient for breast reconstruction. Less than half of all general surgeons always discuss breast reconstruction with their patients. Only 10% of general surgeons always refer their patients to a plastic surgeon. Ten percent of general surgeons never refer their patients. Almost 31% of respondents were concerned that reconstruction could mask a local recurrence. Almost 60% of general surgeons mentioned that less than 10% of their patients get some kind of breast reconstruction done. More than half of general surgeons stated that none of their patients had immediate breast reconstruction.
Almost all respondents were in favour of breast reconstruction in principle. One-third were concerned that reconstruction might delay detection of local recurrence. This is comparable to studies performed in the United Kingdom and in Singapore. Patient disinterest and the perception that patients would not want reconstruction may be important reasons for the low emphasis placed on breast reconstruction in post-mastectomy patients. Post-mastectomy reconstruction does not have a high priority, as demonstrated by the small number of surgeons who routinely discuss and refer their patients for breast reconstruction.
19. CURRENT OPINION ON INCIDENTAL CHOLECYSTECTOMY: FINDINGS FROM A PROVINCIAL SURVEY
The management of incidentally discovered gallstones while operating for unrelated indications remains controversial. Although the current surgical literature favours incidental cholecystectomy based on its safety and the reduction of potential complications of cholelithiasis, we questioned whether the practical management of incidentally discovered gallstones followed suit.
A survey of all FRCSC-trained general surgeons in the province of Saskatchewan was conducted to assess the current opinion on incidental cholecystectomy.
Thirty-three of the 49 (67%) general surgeons polled responded. Sixteen of the 33 (48%) surgeons reviewed the literature concerning incidental cholecystectomy. Only 7 of the 33 (21%) surgeons felt that cholecystectomy should routinely be performed for incidentally discovered gallstones. The remaining 26 surgeons indicated they would consider incidental cholecystectomy under certain circumstances; however, the influencing factors were highly variable. The 3 most consistently listed factors making cholecystectomy more likely were: diabetic patient (44%), signs of previous inflammation (44%), and adequate surgical exposure (36%).
The majority of general surgeons in Saskatchewan favour a noninterventional approach to incidentally discovered gallstones while operating for an unrelated indication. This opinion challenges the current recommendations expressed in the literature. We propose that the current opinion reflects either a reluctance to expose patients to the potential morbidities of a concomitant procedure or a lack of confidence in the current literature.
20. PREDICTORS OF REFERRAL FOR ADJUVANT CHEMOTHERAPY FOR COLORECTAL CANCER
Our objective was to determine the proportions of patients referred for and provided adjuvant therapy for colorectal cancer (CRC) among patients eligible according to published clinical practice guidelines. All patients who had resection for CRC at the Ottawa Hospital during 1999 and 2000 were identified and hospital and regional cancer centre records reviewed.
Among 565 patients who had surgical resections, 158 had stage III colon (n = 104) or stage II or III rectal cancer (n = 54) and survived to discharge. Medical and/or radiation oncology consultation were obtained in 135 patients (85%): by multivariate analysis, such patients were younger and had less comorbidity (Charlson Index) (both p < 0.05). Ninety-four percent of eligible patients aged < 70 years had a consultation, compared with 75% of older patients (p < 0.001). One hundred and thirteen of 158 patients (72%) received adjuvant therapy: treated patients were younger and had less comorbidity than those not treated (both p < 0.01). Eighty-seven percent of eligible patients aged < 70 years received adjuvant therapy (93% of those referred) compared with 53% of older patients (71% of those referred) (p < 0.001).
Referral and treatment rates of 85% and 72% for adjuvant therapy of CRC are greater than generally published, although optimal rates are undefined. Older patients were less likely to be referred for and receive adjuvant therapy. Survival benefit and toxicity are reported similar to those in younger patients, but our knowledge of how other outcomes, such as health-related quality of life, may be influenced by age is limited, and our knowledge of the factors important in decision-making about adjuvant therapy is incomplete.
21. OLDER PATIENTS TOLERATE ADJUVANT THERAPY FOR COLORECTAL CANCER WELL
Our objective was to compare the impact of adjuvant therapy for colorectal cancer (CRC) on physical function and other functional domains in young (< 65 yr) and older patients. Patients completed the EORTC QLQ-C30 core questionnaire and CR38 module, handgrip strength, and other measures before, during and after treatment.
Baseline physical (PF), role (RF), social (SF), and cognitive function (CF) were similar in young (n = 85, age range 35–64 yr) and older patients (n = 65, 65–79 yr). Emotional function was better in older patients at baseline and throughout (p < 0.05). PF did not change during therapy or follow-up in older patients but improved slightly during therapy in young patients (p < 0.05). RF declined moderately during therapy in older patients (p < 0.05) but was similar to baseline at completion of therapy and greater than baseline at 6-month follow-up (p < 0.01). In young patients, by contrast, RF was much improved at completion of therapy and follow-up (p < 0.01). CF declined to a minor extent during therapy in both groups (p < 0.05) but had returned to baseline by completion of therapy. SF increased in both groups during therapy and follow-up (p < 0.01).
Adjuvant therapy for CRC was well tolerated by older patients who experienced minor or no impairments in most functional domains. The impairment in RF (work, leisure and other daily activities) was moderate and recovered well. Age-related differences were modest and may reflect slower recovery of older patients following major surgery. Older patients should not be excluded from adjuvant therapy solely on the basis of age and the assumption of greater adverse effects.
22. PANCREATICODUODENECTOMY: A PROSPECTIVE AUDIT
Results of surgery for periampullary cancers have improved over the last decade. We performed a prospective audit of 53 consecutive patients undergoing a pancreaticoduodenectomy at our hospital over a 4-year period. Patient demographics were: mean age 63, ASA status 1 — 15, 2 — 24, 3 — 14, diagnosis pancreas cancer — 21, ampullary cancer — 13, ampullary adenoma — 6, cholangiocarcinoma — 4, duodenal cancer — 4, neuroendocrine tumour — 3, other — 2. Twenty-nine patients had a pylorus-preserving procedure and 24 had a standard Whipple procedure. Ten patients had extended resections: 5 — portal vein, 1 — hepatic artery, 4 — right colon. Mean operative time was 6 hours 44 minutes, estimated mean blood loss was 571 mL, 4 patients required postoperative ICU, 24% required perioperative blood transfusions and median length of hospital stay was 13 days. Minor complications occurred in 38% (wound infection — 23%) and major complications occurred in 19% of patients (pancreatic fistulas — 13%). Three patients required reoperation and 3 required early readmission. Only 53% of patients did not have a complication. There was no in-hospital or 30-day mortality. Nine percent of patients had new onset diabetes and 26% had pancreatic insufficiency after surgery. Three-year actuarial survival was 40% for patients with pancreas cancer and 100% for patients with ampullary cancer. There was a trend towards earlier return of gastric function without pylorus preservation and a trend towards fewer pancreatic fistulas without the use of intraperitoneal drains. Pancreaticoduodenectomy can be done with low mortality; however, morbidity remains significant.
23. ALTERED FURIN PROFILE IN SPECIFIC SUBTYPES OF NEUROENDOCRINE TUMOURS OF THE PANCREAS (NETs)
This project’s objectives were first to identify the proprotein convertases (PC) and specifically the furin profile of primary and metastatic NETs. Second, to determine if this profile differs between NETs subtypes or from unaffected pancreas (upancreas) or liver (uliver).
At resection for NET, a tissue biopsy of the tumour and the uliver/upancreas counterparts was frozen. mRNA and protein extracts were analyzed via semiquantitative RT-PCR and Western blotting.
Semiquantitative RT-PCR: PC1 and PC2 mRNA: present in all biopsies. PC1 mRNA: higher in glucagonoma biopsies. 7B2 mRNA: detected in all biopsies except uliver, levels higher in secreting NETs compared with nonfunctioning tumours (NF) or upancreas. Furin mRNA: present in all biopsies, levels higher in all tumours compared with upancreas. Western blots: PC1: protein levels high in all tumour biopsies compared with uliver/upancreas; levels highest in glucagonomas. Active PC2 (68 kDa): found in all tumour biopsies, weakly in upancreas and not in uliver (where only ProPC2 [75 kDa] was found), protein levels higher in secreting tumours compared with NF or upancreas. 7B2: protein detected in all secreting tumours, not in uliver and weakly in upancreas and NF, levels higher in all secreting NETs. Furin: levels high in NF compared with other tumours or upancreas.
PCs profile is altered in NETs. The elevated PC2 and 7B2 protein levels in secreting tumours correlates well with their excessive hormone production and permits speculations concerning their role in the pathophysiology of the disease. The elevation of furin in NF reveals a different proteolytic activity. The role of PCs as diagnostic or prognostic tools currently remains unclear, but their implication in islet cells growth and malignant transformation is highly possible.
24. UNILATERAL EXPLORATION FOR PRIMARY HYPERPARATHYROIDISM IN THE ERA OF SESTAMIBI SCANS
Thirty-four consecutive patients with primary hyperparathyroidism (phpt) were assessed preoperatively with a Sestamibi scan. Sixteen patients with a positive scan had planned unilateral exploration. Bilateral exploration was planned for the remaining 18 patients with a negative scan.
Unilateral surgery was successful in 15 of 16 patients with a positive scan. Two patients with a negative scan and a history of previous neck surgery also had unilateral exploration. In both patients, the abnormal parathyroid was found on the unoperated side, and the procedure was terminated. Solitary adenomas were identified in all 17 patients. One patient with a positive scan underwent bilateral exploration for an ectopically located solitary adenoma. Bilateral exploration was also performed in 16 scan-negative patients with identification of 14 adenomas, 1 double adenoma and 1 case of hyperplasia. All patients were normocalcemic within 48 hours of surgery. The operative time was shorter for patients undergoing unilateral exploration compared to bilateral surgery (54 v. 79 minutes; p = 0.0005). There was a trend toward longer operative times in 10 of the 17 unilateral explorations performed with intraoperative use of the gamma probe.
Unilateral exploration for phpt, primarily determined by positive preoperative imaging, can be performed with equal success and shorter operative times than standard bilateral exploration.
25. LAPAROSCOPIC APPENDECTOMY FOR COMPLICATED APPENDICITIS: A PROSPECTIVE EVALUATION OF POST-OPERATIVE FACTORS
Significant disagreement still exists regarding the utility of laparoscopic appendectomy for patients with complicated appendicitis. The objective of this study was to compare postoperative recovery, analgesic use and complication rates between patients who had laparoscopic procedures for uncomplicated versus complicated appendicitis.
Three hundred and four consecutive patients who underwent laparoscopic appendectomy between January 1995 and March 2003 were included in this study. Precise postoperative analgesia requirements, length of hospital stay, return to all regular activity intervals and complication rates in uncomplicated and complicated appendicitis subgroups were analyzed. All conversion to open procedures were included in the corresponding laparoscopic groups on an intention to treat basis. Factors were compared using χ2 and Fisher’s exact tests.
Complete follow-up data was available for 243 (80%) of the patients enrolled. 132 (55%) and 101 (45%) successful laparoscopic appendectomies were completed for uncomplicated and complicated appendicitis respectively. There were no statistical differences between patient groups regarding age, sex, height, weight or previous surgeries (p > 0.05). Furthermore, operating times, length of hospital stay and return to normal activity intervals were also similar (p > 0.05). Complication rates, as well as postoperative in-hospital, and post-discharge analgesia requirements were also statistically equivalent between groups (p > 0.05). There was a significant increase in conversion to open procedures in the complicated appendicitis group (p < 0.05).
This is the first large prospective study to investigate detailed postoperative analgesia requirements, recovery and complication rates after laparoscopic appendectomy for complicated appendicitis. We conclude, much like for uncomplicated appendicitis, that the minimally invasive laparoscopic technique is safe and efficacious, and should be the procedure of choice for nearly all cases of complicated appendicitis.
26. REASSESSING THE INDICATIONS FOR APPENDECTOMY IN THE LAPAROSCOPIC ERA
Laparoscopic appendectomy has gained tremendous popularity over the last decade. Advocates of laparoscopic surgery, recommend its application both as a diagnostic and therapeutic intervention. This study aims to determine whether the indications to operate for suspected appendicitis have changed in the era of laparoscopic surgery.
203 consecutive patients age > 13 years undergoing an appendectomy between January 2001 to December 2002 were reviewed. Patients undergoing appendectomy incidental to another procedure were excluded. Ten (10%) laparoscopic appendectomies were converted to open. These were analyzed within the laparoscopic group, consistent with the original operative intention. Data collected included: preoperative temperature and leukocyte count, results of x-rays, ultrasound (US) or computed tomography (CT) if performed, the negative appendectomy rate and the perforation rate. These factors were compared between patients undergoing laparoscopic versus open appendectomy.
During the study period, laparoscopic appendectomy was performed in 104 patients and open appendectomy in 99 patients. In the laparoscopic group the average temperature and leukocyte count was 37.1°C and 12.4 respectively, compared with 37.2°C and 13.7 in the open group (p = 0.50, p = 0.05). While US and CT were performed almost 2–3 times more frequently in the laparoscopic group, the rate of misdiagnosis was comparable (US: p = 1.00, CT: p = 0.28). The overall negative appendectomy rate was 23.2%. The negative appendectomy rate was similar in the laparoscopic and open groups at 25% and 21.2%, respectively (p = 0.62). Moreover, the incidence of perforation in the laparoscopic group was 17% and 13% in the open group, not reaching statistical significance (p > 0.05).
The indications to operate for suspected appendicitis have not changed significantly with the more widespread application of laparoscopic appendectomy.
27. THORACOSCOPIC SPLANCHNICECTOMY FOR PAIN CONTROL IN CHRONIC PANCREATITIS
Attaining adequate pain control in patients with chronic pancreatitis remains a therapeutic challenge. Thoracoscopic splanchnicectomy (TS) is a minimally invasive surgical approach to pancreatic denervation and has been shown to provide significant pain relief in this patient population. The aim of this study was to evaluate the short- and long-term effectiveness of this surgical approach in controlling pancreatic pain.
We retrospectively reviewed the charts of the patients who underwent TS between 1997 and 2001. Using the documented pre- and postoperative pain scores and the amount of daily medications used, as well as the patients’ characteristics and the descriptions of the operative procedures, the TS effectiveness was examined.
Twelve procedures were performed on 7 patients during this period. Three patients had bilateral TS, 2 had delayed sequential TS and 2 had unilateral TS. The mean preoperative pain score was 8.85. TS was technically successful in all patients with low morbidity and no mortality. The mean length of postoperative follow-up was 23 months. The mean postoperative pain score was 4.92 at 6 months (p = 0.013) and 3.75 at 24 months (p = 0.057). Six patients (85.71%) had decreased postoperative pain score at 6 months and so as the 3 out of 4 patients (75%) who were followed for more than 2 years. Of 3 patients who underwent unilateral TS with improved short-term pain control, 2 developed recurrent debilitating pain requiring contralateral TS.
Bilateral TS is a safe minimally invasive procedure that should be considered in the management of severe pancreatic pain secondary to chronic pancreatitis.
28. CHANGING SCENARIO IN THE MANAGEMENT OF THE EARLY GASTRIC CANCER: LAPAROSCOPIC SURGERY
Early gastric cancer is defined as a gastric cancer confined to the mucosa or submucosa regardless of presence of lymph-node metastasis. In Japan, where the incidence of gastric cancer is very high, this early form represents more than 40% of cancer that are diagnosed by means of mass survey. The approach to its management continues to undergo technical modifications. Laparoscopic surgery for gastric cancer is currently a matter of much debate. We describe here our experience of laparoscopic surgical resection of early gastric cancer for 120 cases done during June 1996 to December 2001. The age range was 42–88 years. Male to female ratio was 81:39. Mean operative time was 3.5 hours. The procedure done includes intragastric mucosal resection in 8 cases, lesion lifting method in 49 cases, laparoscopic assisted distal gastrectomy in 57 cases and intragastric mucosal resection through laparotomy in 6 cases. LADG was added in January 1998. Its indication includes mucosal cancer with unclear margins and submucosal cancer without massive submucosal invasion (sm 1–2) as D1/D2 lymph-node dissection can be done in LADG. All resected specimens underwent detailed histopathological examination. Subsequent diagnosis includes stomach cancer 112, submucosal tumour 6, duodenal cancer 1, stomach adenoma 1 case. Complications to date include wound infection 2, anastomatic leakage 2, stenosis 3, port-site recurrence 1, pancreatic fistula 1, pulmonary embolism 1, vomiting 1. Five-year follow up is available for the first year group. We have had no mortality to date but our follow-up is obviously too short to draw any conclusions. When compared to conventional open gastrectomy, laparoscopic resection has several advantages including less pain, less surgical trauma, less impaired nutrition, rapid return of gastrointestinal function, shorter hospital stay, better postsurgical appearance and with no decrease in operative curability. When performed by a skilled surgeon, laparoscopic resection is a safe and useful technique in early gastric cancer.
29. APPENDICITIS IN THE ELDERLY PATIENT: A LENGTHY ORDEAL
It is known that elderly patients have an increased morbidity and mortality for many surgical procedures. In a retrospective study, those who underwent an appendectomy aged 60 or greater were compared to adult and pediatric cohorts to determine if there was any significant differences in length of operating time or length of stay in hospital.
For the years 2000–2002, the pathological reports and charts of all appendectomies performed in Saskatoon were reviewed. Of a total of 254 cases, 15 (5.9%) were aged 60 or greater, 165 (65.0%) aged 17–59 and 74 (29.1%) aged 3–16. Of these cohorts, they were further broken into laparoscopic and open groups for statistical analysis. In the elderly age group, 9 had the procedures done open (O) at an average operating room (OR) time of 49.25 minutes versus 6 laparoscopically (L) at an average OR time of 60.00 minutes. The average length of stay in hospital was 8.38 days in the open group versus 5.83 done laparoscopically. In the pediatric group, the average O.R. time was 44.69 minutes (O) and 48.22 minutes (L) while the length of stay was 3.31 days (O) versus 3.35 days (L). The third, adult, group had an average OR time of 48.06 minutes (O) versus 55.40 minutes (L) and a length of stay of 3.26 days (O) versus 2.46 days (L).
In summary, we found that appendicitis in those over 60 tends to result in an increased length of hospital stay regardless of the surgical method. As well, we did not find a difference in OR time in the pediatric or adult age groups when comparing open to laparoscopic appendectomies.
30. THE EFFECT OF EVIDENCE ON ABDOMINAL FASCIAL CLOSURE PRACTICE
An examination of surgeons’ attitudes toward published evidence and an evaluation of the change in abdominal fascial closure techniques in relation to the best available evidence.
A retrospective chart review examining suture choice and fascial closure technique was conducted before, immediately following and 10-months after publication of a meta-analysis presenting recommendations on fascial closures. A multi-question survey was then distributed to all general and urologic surgeons and residents in Edmonton, Alberta.
The chart review demonstrates that a significant increase in fascial closure practice using a continuous, nonabsorbable (or polydioxanone) suture was evident 10 months following publication of this meta-analysis (p < 0.001). However, a majority of surgeons (56%) chose to close abdominal fascia with techniques other than that recommended by this level I evidence. The survey demonstrated that a majority of surgeons and surgical residents report to prefer use of a continuous, nonabsorbable suture for fascial closures across a variety of clinical scenarios. 88% of respondents identified randomized control trials as their preferred study design.
While a significant change in fascial closure practice was observed, general and urology surgical disciplines appear slow to adopt new clinical recommendations — even when they are of the highest quality. It seems surgeons temper new recommendations with their own clinical judgement and evidence assessment before adopting new practice guidelines. Of all study designs, randomized control trials are the most widely accepted by surgeons and surgical residents. Perhaps part of the considerable effort expended in producing practice guidelines needs to be directed towards convincing surgeons that level I evidence is truly the best available, and superior to other forms of evidence.
31. TRANSFER OF LAPAROSCOPIC SKILLS FROM A VIRTUAL REALITY (VR) SIMULATOR TO THE PHYSICAL ENVIRONMENT
To determine whether laparoscopic skills acquired in a VR simulator were transferable to complex laparoscopic tasks in the physical environment.
20 residents in surgical specialties (PGY1–3) participated. Residents were scored at baseline in a physical simulator (MISTELS) peg transfer task (“pegs”), VR simulator (LapSim) diathermy task (“diathermy”) and MISTELS intracorporeal suturing (“stitch”). VR performance was evaluated using “time-error” and “motion” scores. Residents were then randomized to training in either a physical or VR simulator, with 10 repetitions of a basic laparoscopic task, either MISTELS “pegs” or VR “diathermy.” Following this, they were retested in the MISTELS peg transfer, LapSim diathermy and MISTELS suturing (“final scores”). Baseline and final scores were compared using paired t-test.
The table shows the mean differences (SD) between baseline and final scores for each task, for each practice group.
Practice using the MISTELS “pegs” task results in enhanced performance of a complex laparoscopic task. Practice using the LapSim “diathermy” task also results in improved performance of a complex laparoscopic task in a physical environment. Physical and VR simulators are effective tools in enhancing laparoscopic skills in novice laparoscopists.
32. PREDICTORS OF WOUND INFECTION FOLLOWING APPENDECTOMY
A retrospective cohort of 236 patients with acute appendicitis who underwent open appendectomy at a university hospital was studied to determine the predictors for postoperative wound infection. Pearson’s χ2 and Fisher’s exact tests for categorical variables, and Mann–Whitney U-test for continuous variables were used to determine statistically significant predictors at the bivariate analysis level. These statistically significant predictors were included in a multivariable stepwise logistic regression model to determine a final model predicting wound infection.
Predictors of wound infection at the bivariate level were: ASA score, midline versus right lower quadrant incision, peritoneal cavity irrigation, intraoperative or pathologic findings of perforation, use of wound wicks, and pathology findings other than inflammation. The final logistic regression model retained only pathology other than inflammation (odds ratio [OR] = 4.1; 95% confidence interval [CI] = 1.8, 9.3; p = 0.0003) and peritoneal cavity irrigation (OR = 2.12, 95% CI = 0.9, 5.1; p = 0.0766). Stratifying the results by pathology did not change the results for the inflamed only category. However, for the necrotic, gangrenous and perforated appendices, wound irrigation was associated with an increased risk of postoperative wound infection even after controlling for potentially confounding variables.
In this study, only pathology findings other than inflammation of the appendix (after controlling for peritoneal irrigation) appear to be predictive of postoperative wound infection following open appendectomy. This effect appears to be modified by pathology findings, as it applies to cases of inflammation only. However, for cases of necrotic, gangrenous or perforated appendicitis, wound irrigation was found to increase the risk of wound infection and not peritoneal irrigation. Wound irrigation in cases of advanced appendicitis may promote bacterial dissemination into the wound and promote development of infection. Further studies would be required to verify these findings.
33. PREDICTING THE BENEFIT OF SUPPLEMENTAL CHEMOTHERAPY USING THE CLINICAL RISK SCORE
We attempt to validate the role of the clinical risk score (CRS) in a novel series of patients who have undergone partial hepatectomies for colorectal metastases and to determine whether the CRS can be used to identify those patients who most benefit from receiving supplemental chemotherapy.
Demographic, disease-specific, surgery-specific, and follow-up data on 103 patients who had undergone 119 resections for colorectal liver metastases were examined. The CRS was calculated for each patient and both survival and disease-free survival were determined after stratification by CRS. The differential effects of the addition of systemic supplemental chemotherapy were then determined.
Median survival of the low-CRS group (n = 63) was 4.51 years (95% CI: 4.02–5.00) compared with 2.66 years (95% CI: 1.38–3.93) (p = 0.02) in the high-CRS group (n = 40). Disease-free survival in the low-CRS group was 1.91 years (95% CI: 0.70–3.11) significantly greater than that of the high-CRS group: 0.82 years (95% CI: 0.59–1.38) (p = 0.03). When the benefits of supplemental systemic chemotherapy were examined in the low-CRS group, a significant improvement in survival was noted at 4-years (hazard ratio = 0.26 [95% CI: 0.07–0.9]) as well as a significant improvement in 1-year disease-free survival (HR = 0.37 [95% CI: 0.14–0.94]) with a strong trend persisting beyond 3 years. There was no apparent benefit in survival or disease-free survival attributable to the addition of supplemental chemotherapy in the high-CRS group.
Patients with low CRS demonstrated increased survival and disease-free survival compared with those with high scores. In addition, CRS may be used to select patients who are most likely to benefit from the addition of supplemental chemotherapy. Low-CRS patients who have undergone partial hepatectomies show significantly increased 4-year survival and a strong trend toward improved disease-free-survival with the addition of supplemental systemic chemotherapy. Chemotherapy did not contribute to survival or disease-free survival in high-CRS patients.
34. ROUX-EN-Y GASTRIC BYPASS IN THE TREATMENT OF SEVERE OBESITY: A CANADIAN EXPERIENCE
A retrospective study of 66 patients between January 1999 and February 2003 who underwent Roux-en-Y gastric bypass (RYGB) for the treatment of severe obesity to determine long-term weight loss.
A single surgeon performed 66 consecutive RYGB surgeries for severe obesity, creating a 25-mL gastric pouch and a 100-cm Roux limb. The retrospective data collected for analysis included patient demographics, comorbidities, previous obesity surgery, complications, weight change, and average weekly aerobic exercise.
The mean waiting time for surgery was 13 ± 7 months. Mean hospital stay was 6 ± 3 days. Seventeen (29%) of the 58 female patients and 1 (13%) of the 8 male patients had had previous surgery for severe obesity. At 1, 2 and 3 years postoperatively, female patients had lost 64 ± 19%, 71 ± 20% and 65% ± 36% of their excess body weight (EBW), and their mean body mass index (BMI) had decreased from a preoperative mean of 52 ± 10 kg/m2 to 32 ± 6 kg/m2, 30 ± 6 kg/m2, and 29 ± 3 kg/m2 respectively. At 3 years, 83% of female patients had maintained greater than 50% EBW loss. At 1 and 2 years postoperatively, male patients had lost 25 ± 15% and 20 ± 4% EBW, and their mean BMI had decreased from 52 ± 8 kg/m2 to 48 ± 3 kg/m2 and 50 ± 2 kg/m2 respectively. At 2 years, none of the male patients had achieved greater than 50% EBW loss. There were 34 complications (52%), the most common being incisional hernias (26%), gallstones (8%) and wound infections (3%). There were 2 deaths (3%); 1 from sleep apnea in the immediate postoperative period and 1 from hepatic failure 1 year postoperatively.
RYGB is an effective long-term treatment for morbid obesity, resulting in an excellent rate and degree of weight loss, especially in female patients, with a minimal length of hospital stay and an acceptable complication rate.
35. PENETRATING THORACOABDOMINAL INJURIES IN QUEBEC: IMPLICATIONS FOR SURGICAL TRAINING AND MAINTENANCE OF COMPETENCE
The incidence of penetrating trauma is low in Canada. Current recommendations for the care of these patients originate from high-volume centres. The purpose of this study was to determine the incidence and treatment of penetrating thoracoabdominal injuries in the Quebec tertiary trauma centres.
All patients with penetrating thoracic and/or abdominal injuries from 1998-04-01 to 2001-03-31 included in the Quebec trauma registry from any of the 4 trauma centres were extracted. Patients with no vital signs upon arrival in the emergency room were excluded. Only patients with Abbreviated Injury Scale greater or equal to 2 for the thoracic or abdominal regions were included.
There were 245 cases. Ninety-one percent were males. Mean age was 33.8 ± 13.2 (range: 15–90). Median Injury Severity Score was 10 (range: 4–75). Overall in-hospital mortality was 6.9%. There were 153 patients (62.4%) with thoracic injuries, 142 patients (57.9%) with abdominal injuries. Fifty patients (20.4%) had injuries to both regions. The chest was opened in 48 patients (31.4%) and the abdomen was explored in 133 patients (93.7%). The incidence of these injuries varied from 3–49 cases per centre per year.
The incidence of penetrating thoracoabdominal injuries is extremely low in Quebec tertiary trauma centres. The number of thoracoabdominal procedures is even lower. Such a weak exposure may jeopardize education and clinical competence. We believe that we need to rethink our educational strategies both for residents and for continuous medical education. New approaches for training and maintenance of competence must be developed.
36. CHARACTERIZATION OF RESIDENT OPERATIVE EXPERIENCE: ACADEMIC VERSUS COMMUNITY CENTRES
Resident rotations at community or nonteaching hospital centres have been an integral part of many surgical training programs. The advent and implementation of community-based medical schools (as seen in Ontario) will further this interaction between academic and community-based medicine. Thus far, it has been difficult to objectively assess the breadth and depth of training residents have received at community centres. Our goal in this study is to characterize the practices of residents at community and academic centres via personal digital assistant (PDA) facilitated Web-based procedure logging.
PDAs were distributed to senior general surgery residents at the University of Western Ontario (London, Canada). Log summaries were evaluated over a 3-month period. The community rotation log summaries were also assessed for the 3 residents who completed community general surgery rotations. The average number of procedures per resident was calculated for each of the 2 rotation settings (academic v. community centres). The 20 most common procedures were also delineated for each group.
While there was no difference in the average number of procedures done by residents in each setting, the type of surgical experience for these 2 groups varied significantly. The residents in community rotations were exposed to a greater variety of surgical procedures from other surgical specialties (e.g., plastic and orthopedic surgery). Academic-centre-based residents performed more tertiary-type general surgical procedures, including pancreatic and hepatobiliary surgeries. There was some overlap between the 2 practice patterns.
Use of PDAs and Web-based procedure logging has facilitated evaluation of resident procedure practices in academic centres and community hospitals. The operative volume is comparable in both settings, however, the types of procedures performed are different. Training programs may use these findings to develop optimal surgical rotations for residents.
37. CHOOSING A CAREER IN SURGERY: TIMING AND RELATIONSHIP TO THE CaRMS MATCH
The declining interest in general surgery is of increasing concern to programs in the US and Canada. The timing of medical students’ career decisions is an important issue that cannot be overlooked. Efforts at student recruitment should be focused on that pivotal time.
The aim of this study was to determine the timing of surgical career choices and their relationship to surgical clerkship rotations. The hypothesis is that students interested in surgery decide this prior to starting clerkship, and accordingly, choose to complete their rotation in the middle of the academic year. Rotations scheduled in this time provide advantages with respect to selection of final-year electives and the Canadian Resident Matching Service (CaRMS) process.
A retrospective analysis of 5 clerkship years (1997–2002) at the University of Western Ontario (London, Canada) was completed. The majority of students who eventually matched to general surgery (69%) or surgical subspecialties (77%) completed their surgical rotations in the middle 2 clerkship blocks. Very few students with surgical rotations at the beginning or end of the clerkship year eventually matched to general surgery (24% and 7%, respectively). Thus, most students have decided on their career paths prior to any clinical experience.
The conclusion is that recruitment efforts in general surgery should be directed at the preclinical years. This may take the form of mentoring programs and exposure to different types of surgical practices.
38. UNDERSTANDING NEUTROPHIL ACTIVITY IN PLASMA FOLLOWING TRAUMA AND ITS ASSOCIATION WITH PLASMA FREE RADICAL PRODUCTION
A prospective study evaluating neutrophil activity among patients at a regional trauma centre. The objective was to identify peak neutrophil activity following trauma and correlate this with changes in plasma free radical production in the same patients. Neutrophil activity was measured over a 7-day period in 120 plasma samples using the myeloperoxidase assay (MPO). The results were compared with the Injury Severity Score (ISS) and free radical activity using the oxistress assay. We observed 2 activity peaks irrespective of the injury score (the first between 7 h and 10 h and the second smaller peak between 13 h and 16 h). This correlated with the changes seen in plasma free radical levels, which peaked between 12 hours and 18 hours. We conclude that activated polymorphonuclear cells have the capacity to generate and release substantial amounts of reactive oxygen species after trauma, which is responsible for the increased free radical production. Based on these findings we suggest that commencing antioxidant intervention within the first 8 hours of trauma may reduce the toxic effects of these free radicals on the host tissue.
39. IMMEDIATE AND LONG-TERM OUTCOMES FOR SEMI-PERMANENT CENTRAL VENOUS CATHETERS (PORTS AND TUNNELLED LINES)
To determine immediate and long-term outcomes for the insertion of central venous catheters and to identify factors predictive of complications for these devices for the purposes of quality improvement.
At a single university hospital, between June 2001 and June 2002, 188 central lines were inserted in 170 patients by 2 surgeons in the radiology department under fluoroscopy. Patient demographics and difficulties at insertion were recorded prospectively. Long-term complications were collected retrospectively on the 148 oncology patients from the electronic chart.
A line could not be inserted in 2 patients, 1.1% (0.1%–2.1%, 95% CI). There was 1 pneumothorax for an immediate complication rate of 0.5% (0.0%–1.5%, 95% CI). Follow-up ranged from 0–381 days with a median of 128 days. Long-term complications requiring premature removal occurred in 17.6% (11.3%–23.9%, 95% CI) of patients. No line was removed for venous thrombosis. In the univariate and multivariate analyses only patient diagnosis was a significant predictor of long-term complications. Premature line removal occurred in 28.2% (17.6%–38.8%, 95% CI) of patients with hematological malignancies or disorder and 7.8% (1.6%–14.0%, 95% CI) of patients with solid malignancies. Overall there were 1.2 complications per 1000 access days. Kaplan–Meier catheter survival at 6 months was 77.4% (68.4%–86.4%, 95% CI).
Line insertion complications and long-term complication rates for semipermanent central lines in this study, except for venous thrombosis, are comparable to those in the literature. Patients with hematological malignancies or disorders are at highest risk for line complications. Strategies to improve line outcomes should target this group. The low complication rate of these lines, particularly in patients with solid malignancies, should be noted when considering central venous access.
40. MANAGEMENT OF HEPATIC COLORECTAL METASTASIS: A SURVEY OF ONTARIO PRACTITIONERS
Despite a large body of evidence supporting hepatic resection in selected patients with hepatic colorectal metastases (HCM), eligible patients may not be referred for consideration for surgery. To examine the management of these patients, we surveyed 4 types of Ontario physicians (total n = 1152): all general surgeons, medical oncologists, gasteroenterologists and a randomly selected group of general practitioners. The survey consisted of 4 actual cases, briefly outlining actual initial available clinical test reports and patient history (e.g., ultrasound, CT scans, chest x-ray, bloodwork). Physicians were asked to indicate their initial management, 5-year survival rate with surgery, operative mortality rates and approach to adjuvant therapy. Three cases included patients with multiple hepatic metastases (MHM) and the fourth case had a solitary hepatic metastasis (SHM). Of the 1152 surveys mailed, (74 wrong addresses), 362 practitioners responded, of whom 228 completed the survey and 134 did not. Results indicate that for cases with MHM, the minority of respondents indicated that they would further investigate or refer the patients for surgical management (case 1 = 32%, case 2 = 57% and case 4 = 36%). 90% of practitioners referred the patient with a solitary hepatic metastasis for surgery or did further investigations. The outcomes of the actual patients on whom these cases were based are; cases 1 and 4 underwent hepatic resection for their MHM (4 and 2 mets respectively) and currently have reached 4- and 5-year disease-free survival. Case 2 (multiple mets in all liver segments) was sent for palliative chemotherapy and survived 14 months. Case 3 (solitary met) underwent hepatic resection and is currently disease free 3 years postoperative. Only 34% of physicians selected the correct operative mortality range (1%–5%) and 36% selected operative mortality ranges greater than 11% or were unsure. The majority of physicians offer palliative treatment only for patients with MHM who may be candidates for surgical management.
41. MELANOMA PROGNOSIS: SHOULD THE INDICATION FOR SENTINEL NODE BIOPSY BE DIFFERENT IN WOMEN?
Gender has long been considered a prognostic indicator in melanoma with an improved outcome for women. This study prospectively compares the incidence of N stage disease in male and female melanoma patients using > 1.00 mm depth of invasion as the indication for sentinel nodal assessment.
Prospective series of sequential patients referred for surgical assessment through a multidisciplinary melanoma clinic. Data collected included age at presentation, gender, primary site, Breslow depth, operative interventions, clinical and pathological staging. Parametric data was analyzed with the Student’s t-test, and categorical data with the χ2 test.
One hundred fifteen patients were collected over an 18- month period ending March 2003. Women had thinner lesions (1.9 mm v. 2.24 mm, p < 0.01) and more frequently an extremity primary (61% v. 16%, p < 0.001). Women who had a lesion with at least 1.0 mm or more depth of invasion were as likely as men to have positive N stage disease (45% v. 53%, p = 0.37).
Although women present in general with thinner lesions, the women who do have melanomas > 1.0 mm in depth are as likely as men to have nodal metastasis. The indications for nodal assessment based on depth of invasion should be the same in men and women.
42. OMISSION OF MECHANICAL BOWEL PREPARATION (MBP) IN PATIENTS UNDERGOING ILEOPOUCH–ANAL ANASTOMOSIS (IPAA) AND CLOSURE OF LOOP ILEOSTOMY (CLI)
An audit of outcome following changes in MBP routine was performed to assess compliance and outcome.
Beginning July 2002, all patients undergoing IPAA and CLI were not to receive MBP. Compliance with the new policy was assessed. The rate of anastomotic leak (AL), intra-abdominal sepsis (IAS) and wound infection (WI) in this group (group I) between July and Mar. 1/03 was compared to patients undergoing the same procedures from July 2001 to June 2002 (group II) when MBP was given routinely. Antibiotic prophylaxis was unchanged.
Between July 2002 and March 2003, 58 patients underwent IPAA (64% having had previous subtotal colectomy (STC)), compared with 83 in group II (40% having had previous STC). Of these 58 patients, 32 (55%) received no MBP, 7 (12%) seen before July 2002 received MBP as per protocol and 19 (33%) received MBP in breach of the new protocol. There was 1 (1.7%) AL, 3 (5.2%) IAS and 1 WI (1.7%) following IPAA (group I) compared with 3 AL (3.6%), 3 IAS (3.6%) and no WI (0%) in group II. Between July 2002 and March 2003, 34 patients underwent CLI, 24 (71%) received no MBP and 10 (29%) received MBP. There was 1 WI (2.9%) and no other complications in group I compared with 3 IAS (5.1%) in group II.
Our audit confirmed it is safe to perform IPAA and CLI without MBP. However, strategies to educate residents and nursing staff are necessary to achieve 100% compliance.
43. A GENDER BIAS EXISTS IN THE CHOICE OF OPERATIVE APPROACH IN PATIENTS UNDERGOING APPENDECTOMY
Four years of retrospective data was analyzed to determine if an age and gender bias exists with regards to undergoing a laparoscopic appendectomy (LA) at the Ottawa Hospital. Secondary objectives included comparisons of patient age, length-of-stay, total operative time and final pathology findings between the groups undergoing LA and open appendectomy (OA).
A total of 1319 cases of laparoscopic and open appendectomies were extracted from the health records database for the period from January 1999–June 2002. Of these cases, pathologic diagnoses were determined for 459 cases by accessing the hospital-wide computerized laboratory information system.
A greater proportion of females underwent LA versus OA (57 v. 44%). More patients treated laparoscopically were in the third and fourth decades of life. Operative time was 18 minutes longer, on average, in LA versus OA. Normal appendices were found in 13% of LA cases (v. 9% in OA). Length of stay, while increased in patients with perforated appendices, was not different between LA and OA.
Younger, female patients were more likely to undergo laparoscopic appendectomy. The operative time was increased and the rate of pathologically normal appendix was greater in those undergoing LA. This likely represents an increased use of laparoscopy as a means of diagnosis. Length-of-stay increased with worsening appendiceal pathology but was not appreciably different LA and OA.
44. OUTCOMES FOLLOWING LAPAROSCOPIC APPENDECTOMY
To study an institution’s experience with laparoscopic appendectomy (LA) and compare these data to published outcomes.
A retrospective chart review was completed for all patients undergoing LA for a clinical presentation of acute appendicitis for the period 1995–2002. Exclusion criteria and key outcomes were established following a detailed literature review. A datasheet was developed and data abstracted from hospital charts.
Using established exclusion criteria, 175 patients were identified. The mean age was 37.6 ± 14.5 years (range 16–83) including 95 males, 80 females. Mean operating time for all cases was 61.9 ± 22.5 minutes (range 23–139). Excluding cases converted to open surgery (14/175, 8%), operating time was 59.9 ± 20.5 minutes. On clinical assessment, 141 patients had acute nonperforated appendicitis, 18 perforated and 16 gangrenous. Histopathologic assessment demonstrated 13 cases of normal appendix (13/175, 7.4%). Length of stay was 2.7 ± 2.5 days (range 1–16) for all cases, converted cases had a mean length of stay of 4.3 days. Intraoperative complications include 2 cases converted for hemorrhage, stapler malfunction and suspected cecal injury. Three patients had significant postoperative infectious complications including 1 wound infection, 1 pelvic abscess and 1 patient with 2 intra-abdominal abscesses. All abscesses were managed successfully with percutaneous drainage. Overall, 3 patients did not receive perioperative antibiotics, 84 patients had irrigation of the operative site and 15 patients had appendix removal without an extraction device. Each postoperative abscess occurred in patients where intraoperative irrigation was used.
An institutional review demonstrates outcomes comparable to the Cochrane systematic review of published literature. Challenges facing LA include longer OR time and a possible increased rate of postoperative intra-abdominal abscess. Technical issues that may impact on intra-abdominal abscesses include aggressive manipulation of the infected appendix and increased use of irrigation fluids, possibly producing greater contamination of the peritoneal cavity.
45. A COST-UTILITY ANALYSIS OF LIVER RESECTION FOR MALIGNANT TUMOURS: A PILOT PROJECT
This study is a pilot cost-utility analysis comparing hepatic resection, radiofrequency ablation (RFA), systemic chemotherapy and symptom control only for the treatment of liver malignancies. This is a prospective, nonrandomized, observational study, which did not influence the type of treatment received. All patients with newly diagnosed liver malignancies of any type who were referred to a hepatobiliary surgeon or to CancerCare Manitoba at the St. Boniface General Hospital were eligible. Quality of life, in terms of quality-adjusted life years (QALYs), was serially measured with the Health Utilities Index Mark II and III. Costs were captured from the viewpoint of society in general, and included hospital costs, outpatient medical costs, and costs borne by patients themselves. A cost-utility analysis was then performed with the aid of decision analysis techniques.
Thirty-nine patients were enrolled in the study. Ten patients have undergone hepatic resection, 4 patients have undergone RFA (sometimes in combination with resection), 19 patients received systemic chemotherapy and 6 patients received symptom control alone. The study is still ongoing. However, the preliminary data suggest that liver resection can offer an average of 2.67 QALYs compared with 1.67 and 1.24 QALYs for RFA and chemotherapy, respectively. The cost-utilities of liver resection and RFA appear similar at $3480 and $4419 per QALY, respectively, although patients receiving RFA generally did have more advanced disease. The cost-utility of chemotherapy appears higher, at $6221 per QALY. There is insufficient data at present to report the cost-utility of symptom control alone. RFA is still an experimental treatment. However, if long-term survival is as promising as published short-term data, perhaps a randomized, controlled trial would be warranted in the future.
46. TEN-YEAR EXPERIENCE WITH COLON ISCHEMIA COMPLICATING CARDIAC SURGERY
Colonic complications, including acute mesenteric ischemia and viscus perforation, following cardiopulmonary bypass are rare but sometimes fatal events. A cluster of cases of acute gut ischemia following cardiac surgery precipitated a retrospective review of our experience with the management of this problem. All cases of colonic ischemia following cardiac surgical procedures in our centre requiring general surgery intervention were identified over a 10-year period. A total of 10 cases were identified over this interval; 4567 cardiac surgical procedures were carried out over this 10-year interval, giving an incidence of colon ischemia of 0.2%. The mortality rate for patients requiring surgical management of colon ischemia was 60% giving an overall mortality of 0.13% due to colon ischemia in the cardiac surgical population.
Urgent cardiac surgery had been performed in all 10 patients, all of whom were dependent on inotropes in the immediate postoperative phase. All patients were over 65 years and most had received blood products either for anemia or ongoing bleeding. In 90% of the cases nonocclusive mesenteric ischemia was the final histopathology of the surgical specimens.
A number of clinical factors identified preoperatively, intra-operatively, and in the postoperative period were analyzed to predict mortality from colon ischemia. Although trends were identified, statistical significance was not reached.
Gut ischemia following cardiac surgery is a challenging problem which occurs infrequently but is associated with a high mortality. A high index of suspicion may lead to a decrease in delay of diagnosis. The nature of the abdominal procedure may be influenced by the poor prognosis of this group of patients.
47. THE EFFECT OF INTRAPERITONEAL ARGININE ON END ORGAN INFLAMMATION IN ENDOTOXIN-INDUCED SEPSIS IN MICE
Arginine has potential immunomodulatory effects via lymphocytes and nitric oxide pathways. Our hypothesis is that supplemental arginine decreases the inflammatory response in end organs in a septic mouse model and that the immunomodulatory effect is altered by feeding.
Mice were either fasted for 16 hours or fed standard rodent chow ad libitum prior to the experiments. Mice were then given LPS (4 mg/kg) or an equal volume of saline intraperitoneally. Twenty minutes later, the mice were given a second injection of either arginine (300 mg/kg) or an equal volume of saline. Fasting or feeding was continued. Mice were sacrificed at 6 hours and liver and lungs were harvested. Levels of inflammation were determined by measuring IL6 using a sandwich ELISA protocol.
In fasted mice, arginine significantly reduced IL6 levels by approximately 50% in lung (p = 0.04) and liver (p = 0.017) compared with saline controls. In fed mice, supplemental arginine minimally decreased IL6 levels in lung and liver (p = NS) compared to saline controls.
We conclude that in the fasted state, arginine modulates inflammation in end organs during endotoxemia. This effect may be clinically significant as the administration of parenteral arginine during the initial treatment period of critically ill patients may modulate the inflammatory response. In contrast, arginine did not seem to significantly alter end-organ inflammation in septic mice taking standard rodent chow.
48. SINGLE VERSUS SEQUENTIAL FINE-NEEDLE ASPIRATION BIOPSY IN THE MANAGEMENT OF THYROID NODULAR DISEASE
This study was undertaken to evaluate usefulness and cost-effectiveness of sequential fine-needle aspiration biopsy (FNAB) compared to single FNAB in the management of thyroid nodular disease.
Charts of all patients who underwent thyroidectomy from 1998–2000 were retrospectively reviewed. FNABs with “suspicious for malignancy,” “follicular lesion,” “cellular atypia” were classified as positive. Data were analyzed using χ2 test and z-test.
There were 268 patients (225 females, 43 males; age from 18–89 yr with mean of 47) underwent a total of 449 FNABs (from 1–6 aspirations with mean of 1.7 FNAB per patient) within a 12-month period before thyroidectomy. Benign disease was as frequent as thyroid cancer (47.8% v. 52.2%; p = 0.351). The accuracy, sensitivity and specificity of single FNAB were 63.8%, 73.8% and 69%, respectively. Sequential FNAB increased the method accuracy in 22.6%, sensitivity in 13.8% and specificity in 6.2% with reduction of false results in 14.2% and “non-diagnostic” results in 100%. There were significant differences between single and sequential FNABs with regard to accuracy (p = 0.009), sensitivity (p = 0.046) and rate of “non-diagnostic” specimens (p < 0.001), but no significance was detected for specificity (p = 0.48) and rate of false results (p = 0.543). However, the costs of sequential cytology per patient were 70% higher than single FNAB. The cost of a sequential FNAB was similar to the cost of a scintigraphy with I-123, but it was 1.5 times more expensive than scintigraphy with Tc99m or I-131 and almost twice the cost of a thyroid ultrasound.
Multiple FNABs are unpleasant for patients, but useful in the selection for treatment of patients with thyroid nodular diseases. Although sequential FNAB increased the method cost, the improvement of FNAB precision may imply a reduction in overall healthcare costs.
49. THE DECLINING POPULARITY OF GENERAL SURGERY IN CANADA: 1993–2003
General surgery is a challenging and rewarding specialty. However, in North America, there has been a widespread perception that general surgery has become increasingly undesirable to medical school graduates. Work by Bland and Isaacs has verified this trend over 23 years in the United States. Our previous work has also verified this trend in the short run, 1996–2001, within the Canadian context. This work sought to extend and further verify previous conclusions by extending the Canadian data through to the beginning of the Canadian Residency Match to the present date. The Canadian Residency Matching Service publishes a report each year outlining the match results. The results from 1993 through 2003 were reviewed to determine the percentage of students choosing general surgery in the first iteration of the match. First choice applicants and vacant spots after the first iteration were chosen as primary outcome measures. A statistically significant negative trend (p < 0.01) can be identified in the number of first choice applicants over the chosen time period. There is also an established trend towards vacant general surgery spots every year. Since 1996, there have been more positions offered, thAn first choice applicants. Currently, general surgery stands at a significant annual risk of having unfilled positions after the culmination of the first iteration of the match. This is a source of significant concern as there may be an impending shortage of general surgeons in the Canadian health care system.
50. ANALYSIS OF ESTROGEN RECEPTOR-α mRNA IN ARCHIVAL PRIMARY HUMAN BREAST CANCERS
Estrogens play an important role in the carcinogenesis and progression of breast carcinoma. Estrogen action is mediated through the estrogen receptor (ER). Approximately one third of breast cancers do not express ER. Indeed, these cancers have an overall increased aggressiveness and resistance to hormonal and standard chemotherapies, as compared with ER-positive cancers. It is not clear why some breast cancers are ER-negative. Genetic changes do not occur with a high enough frequency to explain the ER-negative phenotype.
We studied a cohort of 50 ER-protein positive and 200 ER-protein negative archival primary human breast cancers. Messenger RNA (mRNA) was extracted from these tumours and subjected to standard and real-time reverse transcriptase (RT-PCR) to assess the level of expression of the ER-α gene in ER-positive and ER-negative tumours. Levels of ER-α expression in plasmids and the MCF-7 breast cancer cell line served as our quantitative standards.
Using standard RT-PCR, we demonstrated that 100% of the ER-negative tumours expressed ER-α mRNA. Quantitative analysis of real-time RT-PCR results showed that ER-α mRNA levels in the ER-positive and ER-negative breast cancers overlapped considerably and that the mean levels were not significantly different (p > 0.50).
Breast cancers are labelled as ER-positive or negative based on identification of the protein in cytosolic assays. However, this study shows no significant difference in the ER gene expression in the 2 groups, strongly suggesting that selective post-transcriptional degradation of the ER protein in ER-negative tumours. Our study also verifies the ability to quantify the expression of any gene in archival tumour specimens using real-time RT-PCR.
51. SENTINEL LYMPH-NODE BIOPSY IN BREAST CANCER: ANTIMONY VERSUS TECHNETIUM-99 FILTERED SULFUR COLLOID
We review our experience with antimony and technetium-99 filtered sulfur colloid to test the commonly held notion that antimony, due to its smaller particle size, is better at displaying sentinel nodes than filtered sulfur colloid in breast cancer patients undergoing sentinel lymph-node biopsy.
A chart review of all patients undergoing sentinel lymph-node biopsy at the Vancouver Hospital and Health Sciences Centre was undertaken. Patients were divided into 2 cohorts, those who received antimony and those who received technetium-99 filtered sulfur colloid for their lymphocintoscans prior to sentinel lymph-node biopsy.
In total 172 patients were reviewed, 109 of whom received technetium-99 filtered sulfur colloid and 63 of whom received antimony. There was no evidence of a difference between the 2 in regards to intramammary, supraclavicular or internal mammary nodes. Patients who received technetium-99 filtered sulfur colloid had sentinel nodes identified on preoperative lymphocintoscans in their ipsilateral axillae significantly more often than patients who received antimony, 57% versus 40% respectively (p = 0.03). This is important as there was also evidence of an association between lymphocintoscan positivity and the ability of the surgeon to find a sentinel node at the time of surgery (p = 0.002).
In our cohort of patients technetium-99 filtered sulfur colloid was superior to antimony in identifying sentinel nodes in the axillae and was similar to antimony in identifying nodes in other locations including intramammary, supraclavicular and internal mammary sites.
52. THE INVOLVEMENT OF PHOSPHATIDYLINOSITOL 3-KINASE (PI3-K)/AKT PATHWAY IN OXIDATIVE-INDUCED REPROGRAMMING OF LPS SIGNALLING
Shock/resuscitation following trauma predisposes to the subsequent development of lung injury. Our previous work has demonstrated that ischemia/reperfusion (I/R) primes alveolar macrophage for increased responsiveness to LPS through a mechanism involving increased oxidant stress. Using a cellular model, we have also shown that oxidants reprogram LPS-signalling such that it involves an Src-dependent mechanism. The purpose of this study is to examine the role of the PI3-K/Akt pathway in the reprogrammed LPS-signalling.
The murine macrophage cell line, RAW 264.7, was first incubated with H2O2 μM for 1 hour and then with LPS 0.01 μg/mL for 5–60 minutes. In a separate experiment, the cells were pretreated with PP2 or wortmannin, a specific inhibitor of the Src family and PI3-K respectively. PI3-K/Akt activation were assessed in whole cell lysates using western blotting. NFκB translocation was detected by immunofluorescence (IF) analysis using anti-p65 antibody.
H2O2/LPS caused a marked increase in Akt activation at all time points compared with either LPS or H2O2 alone (Figure, left, T = 30 min). The Src inhibitor, PP2 and the PI3-K inhibitor, wortmannin, prevented Akt activation in H2O2/LPS, indicating their upstream signalling location (Figure, left and right). However, neither affected LPS or H2O2 activation of Akt, consistent with altered signalling by the combination H2O2/LPS. IF showed complete translocation of p65 by 1 hour for both LPS and H2O2/LPS-treated cells (98.3%, 87.5% respectively). Further, the PI3-K inhibitor had no effect on LPS-stimulated p65 translocation but caused a 46% reduction of p65 translocation in H2O2/LPS-treated cells.

Oxidant stress generated during global I/R activates the PI3-K/Akt pathway in an Src dependent manner, a pathway distinct from LPS alone. The ability of the PI3-K inhibitor to inhibit NFκB translocation in H2O2/LPS-treated macrophages supports the concept of reprogrammed LPS-signalling involving the PI3-K/Akt pathway. This study provides a novel potential mechanism whereby oxidants might prime alveolar macrophages and suggest different cellular targets for immunomodulation after I/R.
53. THE EFFECT OF ACIDOSIS ON THE MYOGENIC RESPONSE IN RAT CORONARY ARTERIES
The myogenic response is the process by which blood vessels autoregulate vascular smooth-muscle tone in response to changes in transmural pressure, such that regional blood flow remains constant. It is characterized by vessel contraction or dilation with increased or decreased pressure, respectively. The goal of our study was to identify whether acidosis, a disturbance commonly encountered in surgical patients, impacts the myogenic response in rat coronary arteries.
Ventricular septal arteries (inner diameter 200–300 μm) were isolated from male Sprague–Dawley rats and mounted on a pressure myograph. Tone spontaneously developed when the vessels were equilibrated at 37°C for 1 hour with an intraluminal pressure of 80 mm Hg. The myogenic response was assessed under various experimental conditions by measuring the arterial diameter at pressures ranging from 10 to 120 mm Hg. The ratiometric fluorescence indicators BCECF and Fura-2 were utilized to measure intracellular pH (pHi) and calcium (Ca2+i), respectively.
A decrease in the extracellular pH (pHo) from 7.4 to 6.9 produced a fall in pHi and an increase in the myogenic response. At a constant pHo, blockade of the sodium-hydrogen exchanger (an intracellular acid extruder) with HOE694 also resulted in a fall in pHi and similar enhancement of myogenic activity. Dose response curves were constructed to measure the potency of HOE694: the EC50 was 34 μM for pHi change, and 19 μM for vessel constriction. Ca2+i remained unchanged during HOE694-induced intracellular acidosis. Furthermore, HOE694 did not affect pHi in the presence of HCO3, and vascular tone was consequently unaltered.
Acidosis causes augmentation of the myogenic response, and constriction of rat coronary arteries. This result is at least in part due to the fall in pHi caused by the reduction in pHo, and an increased myofilament Ca2+i sensitivity within vascular smooth muscle.
54. THE ADVANCED BREAST BIOPSY INSTRUMENTATION (ABBI) AT McGILL: MORE THAN JUST A DIAGNOSTIC TOOL?
Stereotactic breast biopsy techniques have emerged to minimize the surgical trauma associated with conventional wire-guided open breast biopsy. Advanced breast biopsy instrumentation (ABBI ) allows for a core of breast tissue to be excised under stereotactic guidance in an outpatient setting. We report our initial experience with ABBI in the diagnosis and treatment of nonpalpable breast lesions.
Hospital charts from 89 ABBI procedures between 10/1996 and 07/2002 were retrospectively reviewed for patient and ABBI characteristics, radiographic appearance, tissue pathology, complications and clinical follow-up. Data are presented as percentage/median (range).
Median age was 59 (39–80), mammographic lesions were classified as calcifications 49% (44/89), soft tissue 39% (35/89) or mixed 11% (10/89). Median radiographic size was 7 mm (1–60). Final pathology revealed DCIS in 7% (6/89) and invasive cancer in 22% (20/89). Microscopically clear margins were obtained in 55% (11/20) of patients with invasive cancer. Of these, 82% (9/11) did not undergo further local surgical therapy. Eight patients remain disease free at 45 months’ (31–66) follow-up, while 1 patient had recurrent disease at 24 months necessitating salvage partial mastectomy. The overall complication rate was 3% (3/89), comprising 1 infection and 2 hematomas. A definitive diagnosis was obtained with ABBI in 100% of malignant and 87% of benign cases. Median waiting time for the ABBI procedure was 19 days (0–90).
Our initial experience demonstrates that ABBI is an effective diagnostic tool for nonpalpable breast lesions, is associated with minimal complications and provides negative margins in over half of malignant cases. In selected patients with invasive cancer and negative margins, this procedure may obviate the need for further local surgical treatment, and merits additional investigation as a therapeutic modality for early breast cancer.
55. PRELIMINARY RESULTS USING A DYNAMIC METHOD FOR DELAYED PRIMARY SKIN CLOSURE OF ABDOMINAL WOUNDS
In the present study we describe our experience with a new dynamic wound closure method that improves on currently available techniques. This case series reviews 8 patients who were referred for delayed primary closure of large abdominal wall defects. In each case local infection control was achieved and significant granulation tissue was present at the time of referral. A dynamic wound closure system was applied under local anesthesia at the bedside and tightened incrementally every second day. The method employs retention cleats, attached to an adhesive base, spaced approximately 1 inch inset and 1 inch along the wound edge. Between opposing cleats a 12 Fr silicone elastomer is passed from superficial to deep (just above the level of the granulation tissue). This technique ensures eversion and prevents devascularization of the skin edge. The dynamic nature of the elastomer allows wound stretch with increased abdominal pressure, such as with coughing or movement. The rate of wound closure and occurrence of complications were measured. All 8 abdominal wounds were closed within 14 days. The patients tolerated the tightening with minimal discomfort and there were no complications of wound infection or skin edge necrosis.
In conclusion, the dynamic wound closure method effectively closed difficult granulating abdominal wounds within 2 weeks. The method improves upon previously described approaches because it takes advantage of biological creep, a physiological property of skin that allows it to proliferate in response to tensile factors, thus expanding the utility of this dynamic wound closure method to include wounds that cannot be closed despite maximization of biomechanical skin stretch. Although the present case series concerns abdominal skin closure, this method was designed for use in full-thickness abdominal closure, both in the setting of postoperative evisceration and as primary prevention in patients who are prone to develop wound complications. A prospective study is currently underway to investigate its use in this setting.
56. EVALUATING META-ANALYSES IN THE GENERAL SURGICAL LITERATURE: A CRITICAL APPRAISAL
Objective:
To assess the methodologic and overall scientific quality of meta-analyses published in peer-reviewed journals pertaining to general surgical topics.
Methods:
A systematic literature review was performed involving: MEDLINE, bibliographic citation review and solicitation of general surgery specialists with knowledge of other meta-analysis publications. We identified all meta-analyses pertaining to general surgery between Jan. 1, 1997, and Oct. 1, 2002. All potential meta-analyses were reviewed independently by 2 reviewers for inclusion. In total 456 articles were identified, exclusion of articles dealing with surgical subspecialties other than general surgery resulted in 70 eligible articles. Exclusion of papers which did not include a statistical analysis of the results from independent studies, aiming to produce a single estimate of treatment effect left 51 articles for final inclusion. The Overview Quality Assessment Questionnaire (OQAQ), a 10-item index was used by 2 reviewers to independently assess the quality of the publications. Disagreements between reviewers were resolved by consensus. In cases where agreement was not reached, a third reviewer was used to settle disagreement. Overall agreement was good with a kappa coefficient of 0.62 (0.55–0.69, 95% CI) prior to consensus resolution. Two cases required a third reviewer.
Results:
Of the 51 articles included in the review, 38 were published in surgical journals. Overall, the mean scientific quality of the articles was 3.33 (median 3, scale of 1–7, poor quality to high quality). This is a low score, indicating the studies had major methodologic flaws. Areas of particularly high methodologic failure include bias in the selection of studies, reporting of criteria for validation assessment of included studies, and appropriate use of validation criteria. Factors associated with a low overall scientific quality include: no other meta-analysis publication by authors, and publications produced by surgical departments alone. In contrast, meta-analyses tended to be of high quality when the authors had published prior meta-analyses or were produced by departments of public health/epidemiology alone or in combination with surgical departments.
Conclusion:
The quality of meta-analyses publications in the general surgery literature is low as a result of methodologic flaws in design. This may limit the validity of reported results. In the future, the use of strict methodology criteria such as the OQAQ may improve the quality of meta-analysis publications and avoid systematic errors.
57. NEEDS ASSESSMENT: CONCORDANCE OF PERCEIVED AND OBJECTIVELY ASSESSED LEARNING NEEDS
Needs assessments in continuing medical education enable the design of targetted educational interventions. Although the CME literature advocates triangulation of needs assessment strategies in order to identify both perceived and objective learning needs, such efforts are time-consuming and costly. Surveys remain the most common method to identify learning needs. The objective of this study was to determine the extent to which self-reported needs are reliable by contrasting the perceived learning needs and objective learning needs of general surgeons.
A survey and multiple-choice examination were mailed to all members of the Canadian Association of General Surgeons. The survey was developed to explore perceived learning needs according to 3 parameters: (1) perceived level of knowledge, (2) interest to pursue continuing education and (3) relevance to clinical practice. The 90-question examination was designed to test knowledge-based competencies and addressed 7 broad topic areas in general surgical practice, corresponding to topics also covered by the survey. Rankings of learning needs generated by analysis of the survey results and the written examination scores were compared.
One hundred and nine general surgeons completed both the written multiple-choice examination and the survey. The 2 needs assessment methods generated dissimilar stratifications of learning needs for the group. There was little congruence between rankings of learning needs based on objective knowledge and rankings based on perceived knowledge. There was a nearly inverse relationship between rankings of learning needs based on the parameters perceived level of knowledge and interest.
The results of this study suggest that failure to consider “real” learning needs may lead to neglect of important learning priorities. Greater interest to pursue continuing education was associated with increased perceptions of knowledge on a particular topic. Therefore, these findings support the comprehensive approach to needs assessment, including strategies to elicit objective learning needs, perceived learning needs, and motivational factors.
58. GROIN SOFT-TISSUE TUMOURS — A CHALLENGE FOR LOCAL CONTROL AND RECONSTRUCTION: A PROSPECTIVE COHORT ANALYSIS
Groin soft-tissue tumours are associated with a high local recurrence rate of 20%–25% and wound complications in 20%–60% of cases. A prospective, phase II study was undertaken at the Tom Baker Cancer Centre using neoadjuvant therapy and specialized reconstructive techniques. The objective was to assess for local control and outcomes in patients with greater than 3 years of follow-up.
Twelve patients presenting with groin soft-tissue tumours were treated with neoadjuvant chemoradiation (3000 cGy/90 mg doxorubicin) followed by surgery (9), radiation (5000 cGy with tissue spacer) followed by surgery (2) for tumours with a retroperitoneal component, or surgery alone (1) for a small, low-grade tumour. Surgery included wide local excision of tumours plus reconstruction techniques involving reconstruction of the abdominal wall, myocutaneous flap reconstruction for large defects and potential vascular reconstruction. All patients were followed prospectively for complications and local recurrence.
Mean age was 53 (range 22–72) at time of diagnosis and 17% presented with recurrent tumours. All tumours presented locally with a mass: stage I (36%), II (36%) or III (27%) disease. Interestingly, 4 patients were initially operated on for possible incarcerated hernia prior to referral. Pathology included 11 sarcomas and 1 desmoid tumour. Sarcoma tumour grade was low (36%), moderate (36%) or high (27%).
There have been no local recurrences (minimum follow-up of 3 yr) and limb salvage rate was 100%. Two patients developed metastatic disease approximately 6 months and 4 years following surgery. One died secondary to metastatic disease, and the other is currently being treated with chemotherapy. Minor wound complications occurred in 2 patients, lymphedema occurred in 2 and there were no postoperative hernias.
Preoperative therapy provides excellent local control of soft-tissue tumours of the groin without the need for hemipelvectomy. Current resection and reconstructive techniques allow for extensive resection with limb salvage, dependable primary wound healing and reliable, long-term integrity of the abdominal wall where it attaches to the pelvis.
59. HAS THE INTRODUCTION OF LAPAROSCOPIC HELLER MYOTOMY ALTERED THE TREATMENT PARADIGM OF ACHALASIA?
Laparoscopic Heller myotomy (LHM) is well established as an effective first-line treatment for achalasia with minimal morbidity. We sought to determine the effect of LHM availability on the treatment paradigm of achalasia in Quebec.
All patients undergoing Heller myotomy (open and laparoscopic) between 1997–2002 were identified from the RAMQ database and divided into 2 groups (pre-lap, post-lap) defined by the approximate date when LHM became generally available in Quebec (1/1/2000). The number and date of endoscopic treatments (pneumatic dilatation or botox) prior to myotomy were noted. A questionnaire examining treatment preferences for achalasia was sent to all Quebec gastroenterologists (GE). Data presented as median (range), χ2 or Mann–Whitney U-test determined significance (*p < 0.05).
| Timing | Age | M/f | Preopendo | Interval, mo | Fundoplication |
|---|---|---|---|---|---|
| Pre-lap | 46 (11–83) | 45/41 | 14/86 | 7 (0.25–57) | 9/86 |
| Post-lap | 51 (13–83) | 47/52 | 23/99 | 3 (0.25–18) | 51/99 |
| p value | 0.04 | 0.51 | 0.24 | 0.04 | 0.01 |
The number of myotomies performed remained stable (pre-lap = 28.6/yr; post-lap = 33/yr) but were done on an older population. The rate of preoperative endoscopic treatment (Endo) did not differ from pre-lap (16.3%) to post-lap (23.3%). Time interval between the last Endo and myotomy diminished significantly. The rate of concurrent fundoplication in myotomy cases increased. Overall myotomy failure rate (requiring postoperative Endo or reoperation) was 8/185 (4.3%). Questionnaire response rate was 41% (60/147). Although myotomy was recognized by GEs as the most effective treatment 54/60 (90%), only 22/60 (37%) would actually refer a healthy patient for myotomy as initial treatment. The remaining GEs chose dilatation 33/60 (55%), botox 2/60 (3%), or Ca-channel blockade 3/60 (5%).
Despite a decrease in time interval between endoscopic treatment and surgery, no decrease in the rate of prior endoscopic therapy occurred after LHM became widely available. The benefits and minimal risk of laparoscopic myotomy need to be more effectively communicated to GEs; they represent the front line in the treatment of achalasia.
60. LAPAROSCOPIC RESECTIONS FOR COLORECTAL CANCER: CONVERSION ADVERSELY IMPACTS OUTCOMES
Objective:
This paper examines the impact of conversion to open surgery on the outcome of patients undergoing laparoscopic resections for colorectal cancer.
Methods:
A prospective database of 377 consecutive laparoscopic resections for colorectal cancer performed between November 1991 and June 2002 was reviewed. The impact of conversion to open surgery was measured on the perioperative outcomes of operative time, complications, mortality and length of stay. In addition, survival curves were determined for the converted and non-converted groups at 2 and 5 years.
Results:
Conversion to open procedure occurred in 46 cases (12.8%). Converted and laparoscopic groups were similar in age, sex, comorbidities, location and size of tumour. The converted group had significantly higher weight (75 kg v. 69 kg, p = 0.013) and conversion score (2.18 v. 1.87, p = 0.005). There was no difference in the conversion rate between stage I (14%), II (8%) or III (13%) colorectal cancers. Patients with stage IV disease were more likely to be converted than stage I–III (23.0% v. 11.2%, p = 0.04). Operative time (210 min v. 175 min, p = 0.002), intraoperative complications (26% v. 6%, p < 0.001), postoperative complications (41% v. 26%, p = 0.023) and perioperative mortality (13% v. 4%, p = 0.021) were significantly increased in the converted group. Converted patients also had a significantly longer median length of hospital stay (8 d v. 5 d, p < 0.001). Median follow-up was 30.5 months for stage I–III and 10.8 months for stage IV patients. There were 190 patients followed at least 2 years and 73 patients followed at least 5 years. Survival curves demonstrate significantly lower 2-year survival after converted procedures as compared with laparoscopic (75.7% v. 87.2%, p = 0.02), with a trend toward lower 5-year survival (61.9% v. 69.7%, p = 0.077).
Conclusions:
Conversion to open surgery was associated with significantly increased operating time, intraoperative complications and length of hospital stay. Conversion also resulted in higher postoperative complications and perioperative mortality. Survival rates at 2 and 5 years are lower for patients in the converted group compared with patients with laparoscopic resection.
61. LONG-TERM SURVIVAL AFTER LAPAROSCOPIC RESECTION FOR CURABLE COLORECTAL CANCER
Objectives:
To examine long-term outcomes in patients undergoing laparoscopic resections for potentially curable colorectal cancer.
Methods:
A prospective computerized database of 377 consecutive laparoscopic resections for colorectal cancer performed between November 1991 and June 2002 was reviewed. Kaplan–Meier survival curves were developed on the basis of intent-to-treat.
Results:
Long-term follow-up was available in 359 of 377 cases (95%). There were 192 male, 167 female patients with a median age of 65 (range: 30–96). The distribution of cases was: cecum/ascending colon 117 (33%), transverse 15 (4%), descending 23 (6%), sigmoid 97 (27%) and rectum 103 (29%). Median operative time was 180 minutes (range: 60–590) and intraoperative complication rate was 9% (hemorrhage most common — 32%). Conversion to open procedure was required in 46 patients (12.8%). Postoperative complication rate was 27% (2% DVT, 2% pulmonary, 6% cardiac) and median length of stay was 5 days. Median follow up for 311 patients with potentially curable disease (stageS I–III) was 30.5 months. Cancer related survival for stages I–III at 2 years were 100%, 94.3% (95% CI: 89.4–99.2), 89.6% (95% CI: 83.1–96.1) and at 5 years were 97.6% (95% CI: 93.0–100), 87.6% (95% CI: 79.8–95.5) and 73.6% (95% CI: 61.8–85.4). Overall survival rates for stage I–III cancers at 2 years were 88.9% (95% CI: 81.6–96.2), 85.0% (95% CI: 78.3–91.7), 84.8% (95% CI: 77.4–92.2) and at 5 years were 79.8% (95% CI: 68.9–90.7), 68.0% (95% CI: 56.8–79.2), 61.7% (95% CI: 49.4–74.1). These results compare favourably with historical controls. Patients with stage III disease may be outperforming historical controls.
Conclusions:
For potentially curable colorectal cancer, long-term survival is not adversely affected by laparoscopic resection. There may be a survival advantage for patients with stage III disease when compared to historical controls. Further confirmation is needed.
62. RESULTS OF COMBINED RADIATION AND RESECTION FOR RETROPERITONEAL SARCOMA
Retroperitoneal sarcoma (RPS) presents late and is difficult to cure with surgery alone. Reported 5-year survival rates after curative resection range from 25%–50%. Our purpose was to develop a management protocol for RPS that combines radiation and resection and to determine the oncologic outcomes of this protocol.
From June 1996 to December 2002, 134 patients were referred to PMH with a diagnosis of RPS. 77 patients were eligible for treatment with curative intent and were started on an institutional protocol of combined management with external beam radiation (XRT, 45–50 Gy preop), resection ± postoperative brachytherapy (BT). Following treatment, patients were followed with regular serial physical examination and imaging. Follow-up is complete. Survival curves were constructed by the Kaplan–Meier method and compared by log rank analysis.
60 patients have completed combined management with radiation and total gross resection, and of these 23 received BT. Postoperative mortality was 1.7%. Median follow-up time is 29 months. Overall survival (OS) at 5 years is 79% (95% CI, 63%– 95%). OS was dependent on disease status at presentation to PMH (95% for primary and 53% for locally recurrent disease, n = 41 and 19 respectively, p = 0.009). 6 patients died of disease and 4 died of other causes, all treatment related. 18 of 60 patients developed relapse following combined management, and 4 of the 18 have undergone subsequent complete re-excision. Relapse-free survival (RFS) at 5 years is 48% (95% CI, 28%–69%). Presentation to PMH with recurrent disease predicted significantly reduced RFS (p = 0.007). BT delayed the time to relapse (p = 0.002) but was associated with a high rate of delayed treatment related mortality (3/23) and an adverse effect on OS (p = 0.038).
We conclude that combined preoperative XRT and complete gross resection for RPS results in favourable oncologic outcomes.
63. The ICOS-B7H PATHWAY AND ITS TOLEROGENIC POTENTIAL IN EXPERIMENTAL ISLET TRANSPLANTATION
The blockade of costimulation is a powerful approach to prevent allograft rejection and facilitate transplantation tolerance. Blockade of CD28:B7 and CD40:CD40 ligand (CD40L) costimulatory pathways with CTLA4-Ig or anti-CD40L, respectively has had considerable success in preventing allograft rejection. Recently, a series of novel costimulatory molecules have been identified, including an inducible costimulatory molecule (ICOS).
In a fully MHC-mismatched mouse model of islet transplantation, we demonstrated that while monotherapy with CTLA4-Ig, anti-CD40L or rapamycin improved islet allograft survival, rejection of the graft was inevitable. Immunohistochemical analysis of rejected grafts revealed increased ICOS expression, suggesting that this costimulatory molecule may provide an alternate escape pathway for T-cell activation leading to graft rejection. The combination of a blocking monoclonal antibody to ICOS (anti-ICOS) with the above therapies resulted in significantly improved islet allograft survival, confirming the importance of ICOS signalling in islet allograft rejection. Percentages of grafts that survived beyond 100 days increased from 18%–60% with combined anti-ICOS and CTLA4-Ig (n = 15), 75%–100% with anti-ICOS and anti-CD40L (n = 10), and 15%–50% with anti-ICOS and rapamycin (n = 21). Study of the mechanisms in mice treated with combined anti-ICOS and rapamycin demonstrated a lack of donor-specific hyporesponsiveness and an absence of regulatory T-cell activity. Re-challenge with donor-strain islets in mice treated with anti-ICOS and rapamycin resulted in delayed rejection of the second graft indicating that operational rather than full immunological tolerance was induced. Mechanistic studies during induction therapy revealed that anti-ICOS and rapamycin therapy significantly reduced in vivo donor-specific proliferation of both CD4+ and CD8+ T cells (61% and 91% reduction), and frequency of IFN-γ producing CD4+ and CD8+ T cells (89% and 90% reduction).
These data demonstrate that blockade of the ICOS-B7h pathway has potential therapeutic benefit given its role in enhancing islet allograft survival and in the regulation of acute allo-responses in vivo.
64. HYPERPARATHYROIDISM: A RISK FACTOR FOR THYROID CANCER
Hyperparathyroidism (HPT) is frequently and mistakenly conceived as a discrete problem on its own. This study was undertaken to evaluate clinical features and therapeutic implications of the association of HPT with thyroid disease.
A retrospective survey of 194 parathyroidectomies from January 1995 to December 2000 was carried out.
One hundred and eighty-two were primary procedures, 12 secondary. Patients ranged in age from 9–85 years with a median of 60; 24% male, 76% female; 12 with family history; 16 had radiation exposure. HPT effects included fatigue 54%, body pain 46%, osteoporosis 34%, hypertension 30%, genital-urinary abnormalities 28%, fractures 20%, previous orthopedic procedures 32% and gallstones 11%. Preoperative ionized calcium was 1.4 nmol/L (mean) and preoperative parathormone 17 pmol/L (mean). Bilateral neck exploration revealed solitary adenoma 165, hyperplasia 27, multiple adenoma 2 with postoperative cure in 97% and postoperative mean calcium 1.2 nmol/L and mean parathormone 4.9 pmol/L. Preoperative ultrasound was positive in 50%, and Sestamibi 85%. Thyroid disease occurred in 41% of HPT consisting of hyperplasia 56%, thyroiditis 20%, cancer 10% and adenoma 4%. There was no mortality or morbidity. Seven recurrent HPTs showed reoperative cure 2, familial hypocalciuric hypercalcemia 1, thyroid cancer 1, Paget’s disease 1 and awaiting operating room 2. There was no correlation in the level of calcium, PTH and nature of symptomatology. Thyroid nodular disease occurred in 50% of HPT. Thyroid cancer occurred in 5% compared to a general population incidence of 0.0004%.
Surgical planning should recognize the interrelationship of HPT and thyroid nodular disease to avoid undue morbidity and even mortality of overlooked thyroid problem.
65. ASSESSMENT OF PERSISTENT ADENOPATHY: PREDICTORS OF A MALIGNANT DIAGNOSIS
Objective:
To determine the significance of persistent adenopathy (6 wk or more) in current general surgical practice, and to delineate features predictive of a malignant diagnosis.
Methods:
Prospective database of consecutive patients referred to an adult surgical practice for the assessment of adenopathy. Inclusion criteria included persistence of adenopathy for at least 6 weeks, no malignant diagnosis in the past 2 years and no obvious primary tumour on initial examination. The database includes age, sex, single or multiple nodes, basin/s involved, size of largest affected node, history of prior malignancy, and the presence or absence of “B” symptoms. Categorical data was assessed with χ2 analysis and parametric data with the Student’s t-test.
Results:
One hundred and seven patients were enrolled over an 18-month period, and all were followed to diagnosis. Tissue was obtained from 99, 1 died of presumed NHL without tissue confirmation and 7 spontaneously resolved during the assessment phase, accounting for all 107 patients. Sixty-nine percent were determined to have a hematological (47%) or solid tumour malignancy (22%). Groin and axilla sites were less likely to be malignant, while multiple basins, retroperitoneal involvement, and supraclavicular locations predicted a malignant diagnosis (p < 0.02). Node size > than 2 cm and age > 55 at presentation also predicted a malignant outcome (p < 0.001). A previous cancer more than 2 years prior to this presentation was not predictive.
Conclusion:
Persistent adenopathy for more than 6 weeks was associated with a malignant diagnosis in 69% of cases. Large node size, basins involved and age were all predictive of a malignant diagnosis, but the high overall rate of significant disease mandates the careful assessment of any persistent node.
66. RATE OF ELECTIVE CHOLECYSTECTOMY AND THE INCIDENCE OF SEVERE GALLSTONE DISEASES
The rate of elective cholecystectomy increased substantially following the widespread adoption of laparoscopic cholecystectomy by surgeons in 1991. We sought to determine how the increase in the rate of elective cholecystectomy affected the incidence of severe gallstone diseases such as acute cholecystitis, acute biliary pancreatitis and acute cholangitis.
We used a quasi-experimental longitudinal design to compare trends in the incidence of gallstone diseases in Ontario from 1988–2000, during time periods with different rates of elective cholecystectomy. We accounted for the effects of age, gender and for secular trends in the use of hospitalization for similar acute abdominal diseases (acute diverticulitis) using overdispersed time series binary regression models.
The average rate of elective cholecystectomy increased 37.2% after 1990, from 197.1–270.3 procedures per 100 000 population per year. During the study period, there were 100 451 hospital admissions for acute cholecystitis, 18 293 admissions for acute biliary pancreatitis and 7476 admissions for acute cholangitis. Overall, the annual incidence of any gallstone disease (cholecystitis, pancreatitis or cholangitis) declined after 1991 (adjusted incidence rate ratio (IRR) for 1992–2000 as compared with 1988–1991, 0.92, 95% confidence interval (CI) 0.89, 0.95). This decline was entirely the result of a reduction in the incidence of acute cholecystitis (IRR 0.86, 95% CI 0.83, 0.89). As compared with the period 1988–1991, there was an increase in the incidence of acute biliary pancreatitis (IRR 1.34, 95% CI 1.17, 1.54) and acute cholangitis (IRR 1.12, 95% CI 0.96, 1.30) after 1991.
The incidence of severe gallstone diseases fell after 1991 when the rate of elective cholecystectomy increased. This reduction was attributable to a reduction in the incidence of diseases caused primarily by gallbladder stones such as acute cholecystitis and not diseases caused by bile duct stones such as biliary pancreatitis or cholangitis.
67. INCIDENCE OF PERIOPERATIVE STROKE FOLLOWING NECK DISSECTION FOR HEAD AND NECK CANCER: A REGIONAL OUTCOME ANALYSIS
The incidence of perioperative stroke in patients undergoing neck dissection is currently estimated to be between 3% and 5%, based on the findings of 2 studies of low methodological quality. Given the potentially high frequency of this complication, it has been suggested that preoperative screening and/or intervention for carotid artery pathology may be indicated. The purpose of this project was to study the incidence of perioperative stroke in patients undergoing a neck dissection in a large urban health region.
This historical cohort study was conducted using discharge data for all neck dissections performed in a geographically defined health region in Alberta, Canada from 1994–2002. Subjects were included in the study if they had an assigned ICD-9CM procedure code for a neck dissection at one of the region’s 3 adult-care hospitals. Our main outcome measure was perioperative stroke.
499 patients were identified as having had a neck dissection (mean age 56.5 ± 15.3 SD, 65.3 % male). Seven patients had ICD-9CM codes for postoperative central nervous system complications (incidence of 1.4%). However, on detailed chart review, only 1 of these was found to have experienced a perioperative stroke. This therefore suggests a stroke incidence of only 0.2% (95% CI = 0.01, 1.12). No missed strokes were found in a confirmatory random review of 10% (n = 50) of charts.
The incidence of perioperative stroke in this study is significantly lower than that previously reported in the literature. This suggests that preoperative screening and/or intervention for carotid artery disease may not be necessary in this patient population.
68. MEDICAL STUDENT CONTACT WITH PATIENTS DURING A SURGERY CLERKSHIP — CONTRAST BETWEEN A CANADIAN AND AN AMERICAN MEDICAL SCHOOL
The Canadian and American health care systems differ in many ways. Two of the most important differences are with regard to the socialized approach to health care in Canada (leading to limited resources and staffing), as well as a paucity of malpractice litigation compared to the United States. We hypothesized, that due to these discrepancies, medical clerks in Canada get more hands-on training than clerks in the United States.
In order to evaluate the differences in medical student exposure to patients between Canadian and American medical schools, a survey was administered to clerkship students at McGill University in Montréal, Canada as well as at the Southern Illinois University School of Medicine, Illinois, United States. Results of questions posed to students were tested for between-group differences using the χ2 test.
Forty-four percent of Canadian students compared with 22.5% of American students (p = 0.001) were the first to elicit the chief complaint and obtain a history on surgical patients. When asked how often students were the first to perform the surgical physical examination on the patient, 64.0% of Canadian and 36.3% of American students (p < 0.001) responded positively. 46.0% of Canadian students were asked to generate the initial hypothesis regarding a patient’s diagnosis, compared with 14.8% in the American group (p < 0.001). 44.0% of Canadian-trained students were permitted to suggest the initial investigations to be ordered in the work-up of the patient, compared with 11.6% of American-trained students (p < 0.001). 85.2% of American students knew the patient’s diagnosis prior to seeing the patient, compared with 54.0% of Canadian students (p < 0.001). 88.4% of students were among the first 3 people to examine a new patient in the Canadian group, compared with only 65.6% in the American group (p = 0.003).
Canadian hospitals are forced to function with limited resources secondary to budgetary limitations on health care. This leads to limited staffing on surgical services. These limitations, however, may be beneficial to medical students. Canadian medical students get more hands-on training and experience than their American counterparts.
69. COMORBIDITY AND AGE ARE BOTH INDEPENDENT PREDICTORS OF LENGTH OF HOSPITAL STAY AMONG TRAUMA PATIENTS
The goal was to determine the separate and combined impact of age and comorbidity on length of stay for trauma patients in a tertiary trauma centre.
A cohort of trauma patients surviving to hospital discharge in a tertiary trauma centre between April 2000 and March 2001 was identified. Patient characteristics, severity of injuries and length of stay were obtained from the trauma registry. Each medical record was reviewed for completeness of information and assessment of comorbid conditions. A multivariate linear regression model was developed to predict log length of stay from age and presence of comorbidity while adjusting for Injury Severity Score.
Among the 994 trauma patients surviving to hospital discharge, mean age was 49.7 years and mean Injury Severity Score 10.3. At least 1 comorbid condition was present in 32% of patients. Mean length of stay was 15.3 days. Presence of comorbidity increased from 8.7% before age of 55 to 92% at 85 or more (p < 0.0001). According to the multivariate model, the presence of comorbidity, age and Injury Severity Score were all independent predictors of hospital stay (p < 0.0001). When applied to patients with the mean Injury Severity Score value of 10.3, the model showed a steady increase in the length of stay for patients with comorbidity over those without any.
Comorbidity and age are both independent significant predictors of length of stay over and beyond that which is expected, based on the severity of the injuries. With aging of the population, this phenomenon will impact on future resource utilization in trauma centres.
70. SENTINEL LYMPH-NODE BIOPSY FOR CUTANEOUS MELANOMA OF THE HEAD AND NECK
A retrospective study of 35 patients over 6 years shows the sentinel lymph-node (SN) biopsy for cutaneous head and neck melanoma to be technically demanding but accurate. Using a standardized protocol of preoperative lymphoscintigrams, intraoperative blue dye injections and hand-held gamma probes, sentinel nodes were identified in 33/35 (94.3%) patients. Histologically, 7 patients had at least 1 SN positive for metastatic melanoma; no false-negative case was identified during follow-up (mean 13.89 mo [median 15; range < 1–56 mo]). The sensitivity (7/7 + 0) and negative predictive value (26/26 + 0) were 100%. There was disagreement in the location of the SN on the preoperative lymphoscintigram report and that found at the time of the surgical procedure in 31.4% of cases. The sites of drainage of the primary lesion were found to be varied and discordant with clinically predicted sites. Early results show that the SN biopsy in the head and neck region is a technically difficult and cumbersome procedure with an often unpredictable drainage pattern. We conclude that combined preoperative, intraoperative and histological techniques produce a sensitive procedure with a high negative predictive value and that the lack of false-negative results precludes the need for prophylactic neck dissections.
71. THE MISTELS PHYSICAL LAPAROSCOPIC SIMULATOR IS AN EFFECTIVE EDUCATIONAL TOOL
The advent of minimally invasive surgery (MIS) has required surgeons to learn new skills including ambidexterity, depth perception from a monocular image, and tissue handling in a reduced tactile environment. Simulation has been used extensively for teaching, but few programs have objectively evaluated their systems for reliability and validity, nor assessed the outcomes of their simulator curricula. MISTELS is a physical simulator incorporating 5 tasks of graded complexity. Performance on each task can be assessed on the basis of speed and accuracy. Inter-rater reliability for the MISTELS program has been shown to be 0.99 and test–retest reliability 0.95 (by intra-class correlation). Validity has been demonstrated by showing significant difference in performance in MISTELS between junior and senior residents (p < 0.01), and between residents with superior versus average technical skills based on their in-training evaluation (p < 0.05). There is good correlation between performance in MISTELS and performance in live animal surgery (r = 0.7, p = 0.0001).
Pedagogical components of MISTELS as an educational tool include an opportunity for graduated practice of skills with objective performance indicators, evidence that practice improves performance of these simulated skills, and that practice enhances performance in live animals. Further, practice of a simple MISTELS task (peg transfers) results in improved performance of a complex task (intracorporeal suturing; p < 0.01) for novice laparoscopists. Finally, we have established a pass/fail cutoff score that can distinguish between “competent” and “non-competent” laparoscopic surgeons with sensitivity, specificity, positive and negative predictive values > 0.80.
A high-quality educational tool has been developed for MIS that has been shown to be effective for learning and for evaluating basic MIS skills.
72. THE EFFECT OF LONG OPERATING TIMES ON LAPAROSCOPIC COLON RESECTION FOR CANCER
The purpose of this study was to determine if prolonged operating time has a deleterious effect on survival following laparoscopic colon resection for colon cancer.
A prospective computerized database of 359 consecutive laparoscopic resections for colorectal cancer was reviewed. Forty-eight converted cases were excluded. Median operating time for the remaining 311 procedures all completed laparoscopically was 180 minutes. Cases were then divided into 2 groups based on operative time: group A (≤ 180 min) and group B (> 180 min). Kaplan–Meier curves for survival and disease-free survival were generated for each group and analyzed stage by stage using the log rank test.
The 2 groups were comparable for demographics, comorbidities, tumour location, size and stage. Overall survival was not statistically different between the groups when comparing all curable stages (I–III) together and stage by stage. However, the disease-free survival was significantly better for group A versus group B when analyzing stage III disease only: 2-year survival of 84.3% versus 67.6% (p = 0.046) and 5-year survival of 64.8% versus 42.3% (p = 0.041). Disease-free survival did not differ significantly for stage I or II.
In this series of successfully completed laparoscopic colon resections, operating times of greater than 3 hours lead to decreased disease-free survival for stage III colorectal cancers.
73. OBJECTIVE ANALYSIS OF GASTROESOPHAGEAL REFLUX AFTER LAPAROSCOPIC HELLER MYOTOMY: AN ANTIREFLUX PROCEDURE IS REQUIRED
The purpose of this study is to objectively analyze gastroesophageal reflux following laparoscopic Heller myotomy where an antireflux procedure was not performed.
A prospectively collected database was used to compile and analyze 54 cases of laparoscopic Heller myotomy without concurrent antireflux procedure performed between November 1996 and June 2002. Minimal hiatal dissection was performed and intraoperative endoscopy was used to accurately identify the gastroesophageal junction thereby avoiding injury to the gastric sling fibres. Follow-up included symptomatic assessment in 50 (93%) patients. Heartburn was assessed on a 4-point scale with clinical significance defined as > 2/wk. Objective testing including endoscopy, esophagogram, manometry and 24-hour pH monitoring was offered to all patients. Objective evidence of reflux was defined as the composite end point of positive 24- hour pH monitoring or esophagitis on endoscopy.
Significant heartburn was reported in 15 of 50 (30%) patients. Positive 24-hour pH recordings were seen in 11 of 21 patients while esophagitis was seen in 13 of 20 patients resulting in objective evidence of reflux in 18 of 28 (65%) patients tested. Of these 18 patients, 7 (39%) did not complain of significant heartburn. Patients without objective reflux did not complain of significant heartburn. Therefore, out of the 28 patients with objective testing, 7 (25%) had silent reflux.
Objective analysis reveals an unacceptable rate of gastroesophageal reflux in laparoscopic Heller myotomy without an antireflux procedure. This includes a concerning 25% incidence of silent reflux.
74. OXIDANTS IN HEMORRHAGIC SHOCK INDUCE LIPID RAFT RECRUITMENT OF TOLL LIKE RECEPTOR-4 (TLR-4)
Oxidant stress (OX) during shock/resuscitation (SR) contributes to organ failure by priming alveolar macrophages (AM) for increased responsiveness to subsequent inflammatory stimuli such as LPS. Recent studies showed that lipid rafts, detergent-insoluble cell membrane areas implicated in cell signalling, cluster the LPS receptor complex: TLR4 and CD14 upon LPS stimulation. Since our initial studies showed that OX/SR induces peripheralization of the TLR4 on AM’s, (Surg Forum 2001), we hypothesize that priming of AM’s during OX/SR involved lipid raft recruitment of TLR4.
Rats were bled to an MAP of 40 mm Hg, 1 hour later resuscitated with their shed blood plus an equal volume of Ringer’s lactate (RL) plus or minus antioxidant, N-acetylcysteine (0.5 g/kg). After 1 hour, AMs were recovered by bronchoalveolar lavage (BAL) and analyzed, or AMs from untreated rats were incubated with hydrogen peroxide (H2O2, 100 μM for 1 h) ex vivo. Cells were fixed, permeabilized and stained with fluorescent anti-TLR4 antibody and rhodamine-cholera toxin B specific for a lipid raft marker GM-1 ganglioside.
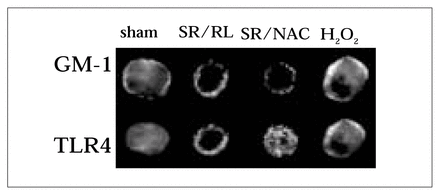
Lipid rafts were primarily distributed in the plasma membrane (upper panel of figure). SR/RL caused peripheralization of the TLR4 receptor and colocalization with GM-1 in the lipid rafts, while NAC resuscitation reversed the effects of SR on the TLR4 peripheralization and rafting (lower panel of figure). Consistent with a role of oxidants in this effect, ex vivo oxidant stress mimicked the effects of SR, by causing migration of the TLR4 into the lipid rafts. Thus: OX in vivo or ex vivo induces TLR4 migration into the lipid rafts of AM. These findings suggest a novel mechanism for oxidant-mediated AM priming. Modulating raft recruitment of TLR4 may represent a potential therapeutic target.
75. ANASTOMOTIC LEAK: CAN WE PREDICT IT?
Anastomotic leak is a major cause of morbidity and mortality in GI surgery. Identification of high-risk patients would help the surgeon evaluate an individual’s risk of leakage following intestinal anastomosis. The aim of this study was to develop a preoperative scoring system to predict the risk of anastomotic leak.
Medical records of all patients who underwent an intestinal resection with primary anastomosis between Apr. 1, 2000, and Mar. 31, 2002, were retrospectively reviewed. Data was collected on previously identified variables felt to contribute to anastomotic leak including: age, gender, diagnosis, weight loss (> 10 lb), bowel obstruction, steroid use, ASA class, comorbidities, adjuvant chemoradiotherapy, surgical procedure and anastomotic site, emergent procedure, blood transfusion, soilage, metastasis, stoma construction, complications, ICU admission, hospital stay and intestinal leak or abscess. Following univariate and multivariate analysis 2 scoring systems were created and applied retrospectively to the database.
488 patients (248 male and 240 female) underwent 507 resections with primary anastomosis (multiple anastomosis, 19 patients). Anastomotic leak occurred in 20 (3.9%). The most significant variables included weight loss (RR = 3.1), bowel obstruction (RR = 4.2), COPD (RR = 6.3). When all 3 variables were present the leak rate was 40%, with 2 variables 22%, with a single variable 5.7% and in absence of all 3 variables 0.3%. The addition of gender (RR = 2.2), steroid use (RR = 2.2), ASA class > 2 (RR = 3.0) or multiple transfusion (RR = 3.9) improved the distribution but not the accuracy.
The risk of anastomotic leak can be predicted preoperatively. Weight loss, bowel obstruction and COPD are independent predictors and are additive in their effect.
These factors may be useful to guide operative decision-making; however, they require prospective evaluation to assess their validity.
76. THE NEED FOR SEQUENTIAL FINE-NEEDLE ASPIRATION BIOPSIES IN THE DETECTION OF CANCER IN THYROID NODULAR DISEASE SURVEILLANCE
Background:
Fine-needle aspiration biopsy (FNAB) directs treatment of thyroid nodular disease (TND). Patients with benign cytology are treated by thyroid suppression and follow-up. It has been stated that 2 consecutive “benign” FNAB reports suffice to exclude cancer.
Objective:
This study was undertaken to appreciate the importance of repeated needle biopsies in management of thyroid nodular disease to avoid failure of diagnosis of cancer.
Method:
Patients with “benign” FNAB who revealed thyroid cancer were studied as to incidence in thyroid cancer, demography, tumour size, and application for management.
Results:
Sixty-two patients with thyroid cancer were seen in 2002; 55 with well-differentiated thyroid carcinoma (WDTC) underwent surgery including 15 (27%) who had been consigned to conservative management in which sequential FNAB had revealed WDTC. They varied in age from 33 to 70 years with a mean of 50 with 12 females and 3 males. The number of FNABs varied from 2 to 5 with a average of 3. Duration of nodule varied from 3 months to 10 years, < 1 year in 6, > 1 year in 9. Tumour size varied from 0.35–4 cm (mean of 2.05 cm). Ultrasound FNAB used in 7 of 15 cases (47%) made the diagnosis in 3 (20%). Diagnoses included scanty benign aspirates (insufficient) 16, “benign” 5, cyst 2, Hurthle 1, follicular 2, atypia 4, colloid 2 and degenerative 1. Clinical features included suppressed TSH 3, node positivity 4, previous surgery 1 and radiation exposure 3.
Conclusion:
Thyroid cancer is showing a remarkable increase in incidence throughout the world. TND is frequent and cannot be ever completely managed by surgery. Appropriate FNAB fortifies selection of patients for conservative management which should include sequential FNAB to minimize failure in detection of thyroid cancer.
77. A SURVEY OF COLORECTAL CANCER SCREENING PRACTICES IN A LARGE CANADIAN URBAN CENTRE
Introduction:
Colorectal carcinoma (CRC) is the second leading cause of cancer in Canada and is an ideal tumour to implement screening policies. Screening guidelines for CRC are based on differing levels of evidence and opinion. The aim of this study was to determine current screening practices in Alberta for asymptomatic patients with and without a family history of colorectal carcinoma.
Methods:
A questionnaire was mailed to a representative sample of physicians in a large urban centre in Alberta. Nine hundred twenty-two surveys were mailed and results including response rate, type of practice/specialty, presence or absence of a screening policy and type of policy — age at initiation of screening, screening tests employed and frequency of screening — were tabulated.
Results:
A 61% response rate was achieved overall. 58% (CI 53.6%–62.6%) of physicians employed a screening policy in patients without a family history of CRC compared with 96% (CI 94.7%–98%) of physicians who screened patients with a family history of CRC (p < 0.0001). In the subgroup without a family history of CRC, the majority of physicians chose the age of 50 to initiate screening (63%), hemoccult blood testing was used most frequently (79%), and frequency of screening varied mainly by modality used. In patients with a family history of CRC, most physicians initiated screening prior to the index case (45%) or by age 40 (31%), colonoscopy was most frequently employed (84%), and frequency of screening varied mainly by modality.
Conclusion:
Despite evidence supporting CRC screening in all average risk patients, only 58% of physicians currently employ screening strategies in patients with a negative family history of CRC. The majority of physicians with a screening policy use hemoccult blood testing in this patient subgroup. However, most physicians screen patients with a positive family history of CRC with colonoscopy suggesting they believe it is a superior screening modality. Additional studies exploring the true cost:benefit ratio of screening colonoscopy at a patient and society level need to be constructed.
78. BARRIERS TO OPTIMIZING LYMPH-NODE RETRIEVAL AND ASSESSMENT IN COLORECTAL CANCER
Introduction:
Lymph-node (LN) retrieval and assessment is critically important for accurate staging and treatment planning in colorectal cancer (CRC). A recent NIH consensus panel has suggested that a minimum of 12 LN should be examined to insure node negativity. The purpose of this study was to identify barriers to achieving this standard.
Methods:
We conducted an audit of stage II CRC resection specimens in patients aged 19 to 75 in Ontario between 1997 and 2000. Practising pathologists were identified using databases of the College of Physicians and Surgeons and the Royal College of Physicians and Surgeons (RCPSC). Final-year pathology (n = 7) and surgery residents (n = 25) in Ontario were identified. Participants were surveyed by phone to identify perceived and “blind” barriers to optimal LN retrieval and assessment.
Results:
1789 stage II specimens from 100 hospitals across Ontario were assessed. A median of 8 LN was reported in node-negative specimens. Seventy-three percent of specimens had fewer than 12 LN assessed. 224 out of 263 (85.2%) eligible pathologists were surveyed. Obstacles identified in this group included technical difficulty identifying LN, lack of time and inadequate specimens. 57% percent of pathologists indicated an awareness of guidelines for LN retrieval in CRC, but only 25% of the provincial total identified that a minimum of 12 LN are necessary for accurate designation of node negativity. Five of 7 (71%) pathology residents and 15 of 24 (63%) surgical residents specified that 12 or more LN should be assessed.
Conclusion:
The complexity and commensurate time requirement to complete pathology reports in oncology has increased in the last decade. A number of centres have started to use pathology assistants to ease the workload. To optimize CRC staging, at least 3 factors need to be addressed: pathologist workload, awareness of current guidelines and appropriateness of the surgical mesenteric specimen. We have initiated a multi-modal province-wide education change initiative directed at both surgeons and pathologists to address these issues.
79. EVALUATING LEARNING IN A TOTAL MESORECTAL EXCISION (TME) COURSE FOR SURGEONS
Purpose:
To determine whether a combined didactic and hands-on course in the optimum surgical management of rectal cancer by total mesorectal excision could improve surgeons’ knowledge of fundamentals of this approach.
Methods:
A multiple-choice examination was developed covering aspects of the anatomy, pathology, functional outcomes and relevance of TME. Standardization of the tool was based on the performance of the course instructors. The validity of the testing tool was determined by testing surgical residents (R1–R6) who had not taken the course. Course participants completed the examination at the start and at the end of the course. Data was analyzed using standard statistical techniques.
Results:
The mean instructor score (n = 8) on the test was 25.8 of 33 possible marks, with no difference in pre- and post-course testing (p = 0.6, CI –2.4, 1.5). Resident testing demonstrated a positive progression of marks with a significant difference (p = 0.001) in the performance of senior residents as compared to junior residents. Senior resident scores compared favourably with instructor scores. Course participants improved their performance with a mean of 19.2 on the pretest (n = 55) and 25.4 on the post-test (n = 57) (p = 0.001, CI 5.0,7.5). Participant post-test scores were no different from instructor scores (p = 0.9). The degree of improvement varied among the different aspects of knowledge being tested.
Conclusions:
Surgeons attending a combined didactic and hands-on course in total mesorectal excision for the optimum surgical management of rectal cancer are able to improve their knowledge of the principles of this approach.
80. BREAST CONSERVATION FOLLOWING A BREAST CANCER DIAGNOSIS IN THE MANITOBA POPULATION
Background:
National guidelines for the management of breast cancer were published in Canada in February 1998. Breast conservation for stage 1 and 2 disease was generally recommended.
Objective:
The primary objective was to determine breast conservation rates in the Manitoba population. Secondary objectives were to determine factors that influenced that rate and to compare Manitoba outcomes to benchmarks.
Methods:
Manitoban women with a breast cancer diagnosis from 1995–1999 were retrospectively reviewed using the Manitoba Cancer Registry and administrative data.
Results:
Of 3956 women with breast cancer, 3728 (94.0%) had definitive surgery to the primary breast cancer. 1720 (43.5%) had breast conservation. Breast conservation increased over the duration of the study, was higher in Winnipeg versus other regions and decreased with increasing stage. Breast conservation was not affected by age at diagnosis. The breast conservation rate was 51.2% in 1999 for breast cancer patients with stage 1 and 2 disease residing in Winnipeg.
Conclusions:
In this population-based study, breast conservation rates appear to be low when compared to similar population based studies. The most favourable data shows a rate 10% below the ideal. These results provide key baseline information for subsequent quality improvement initiatives.
81. MESORECTAL EXCISION: A PARADIGM SHIFT IN THE TREATMENT OF RECTAL CANCER
Purpose:
Local recurrence (LR) and ultimately survival following curative resection of rectal cancer depends primarily on surgical technique and experience. Conventional techniques result in LR rates of 15%–40%. Total mesorectal excision (TME) emphasizes the circumferential margin and is associated with LR rates of 5%–10%. The aim of this study was to determine the rate of local recurrence following the introduction of TME in a large Canadian city and compare it to historical controls.
Methods:
A retrospective chart review of all patients with stage I, II and III rectal cancer who underwent TME from 3 TME-trained surgeons in a large urban health region from 1994–2002.
Results:
223 patients (145 male, mean age 67.7 yr) underwent primary resection for rectal cancer during this time period with 179 patients resected for cure (80.3%). The mean height of curative lesions was 8.6 cm (range 2–15) from the anal verge. Surgical procedures included anterior resection in 126 patients (mean anastomotic height 7.1 cm), APR in 48 and Hartmann’s in 5. Operative mortality was 2% with an overall leak rate of 8.8% (4 radiologic leaks and 7 pelvic abscesses). Local recurrence occurred in 6 patients (3.4%) operated on with curative intent, with distant recurrence in 16, 8% at a median follow-up of 24 months, 45% of patients with leaks had undergone preoperative radiation. In the group of patients who received preop radiation, the overall leak rate was 17.9%, compared with only 6.3% in those without pre-operative radiation. Actuarial 4-year overall survival (OS), cancer specific survival (CS) and local recurrence (LR) rate was 84%, 88% and 6% respectively. The latter compares very favourably with historical rates of 20% or greater.
Conclusions:
TME has been associated with a dramatic decrease in the rate of local recurrence of rectal cancer in our region. Patients who received preoperative radiation had an overall leak rate almost triple that of patients not receiving preoperative radiation. The OS, CS and LR in this series compares favourably with that reported in recent series, and is far better than in historic controls.
82. PHENOMENOLOGICAL ASSESSMENT OF PATIENT EXPERIENCES IN EXTENDED PELVIC RESECTIONS FOR RECTAL CANCER
Background:
Locally advanced or recurrent rectal cancer (LARC, LRRC) presents a difficult management problem for the surgeon and a daunting process for the patient. Aggressive surgery offers the only chance for cure, but the physical, psychological, social and emotional experiences of cancer patients undergoing this treatment have not been fully researched.
Methods:
Qualitative methods were used to examine the experiences, decision-making, quality-of-life and supportive care needs of 10 patients undergoing a total pelvic exenteration ± partial sacrectomy (TPE) for LARC (n = 7) or LRRC (n = 3). Patients were selected from a population of 33 patients undergoing TPE (n = 24) or APR/sacrectomy (n = 9) for LARC/LRRC during the period 1999–2002. Phenomenological methods using Colaissi’s analytic method were used. Qualitative interview data was used to identify “thematic classification” of critical elements common to the experience within and between participants. Non-MD professionals performed the interviews that ranged in duration from 1.5–2 hours.
Results:
Major, common themes uncovered included: 1) variance between patient and MD perception of the amount and nature of information given preoperatively; 2) lack of options in decision-making; 3) difficulty in seeking and receiving help for problems associated with TPE (e.g., coping with urostomy difficulties); 4) forgiveness of medical practitioners for significant side effects (e.g., postop sexual dysfunction and 5) mistaken perceptions of likelihood of cure (i.e, most patients overestimate the likelihood of cure).
| Patient characteristics | |
|---|---|
| Median age (range) | 70 (48–78) |
| M/F | 9:1 |
| Chemo ± radiation (pre- or postop) | 10 patients |
| Median follow-up from operation (range) | 11 mo (2–19) |
| Disease status | 9 NED, 1 AWD |
Conclusion:
Surgical oncologists may overestimate the degree of understanding achieved by patients consenting for surgical management of LRRC and LARC. This analysis suggests elements to amplify in preop discussions with LARC/LRRC patients consenting for exenterative procedures.
83. SPONTANEOUS HEPATOMAS AND DEFECTIVE POST-HEPATECTOMY CELL CYCLE REGULATION IN SAK+/− MICE
Sak is a member of the polo family of cell-cycle regulated protein kinases. We previously demonstrated significantly reduced levels of Sak mRNA in a subset of colorectal cancer cell lines displaying chromosomal instability, and in a fraction of patients with colorectal cancer. We hypothesize that Sak haplo-insufficiency causes defects in mitosis, leading to chromosomal instability and carcinogenesis. To test this, we generated Sak knockout mice by replacing exons 1 and 2 with a neomycin cassette. While Sak−/− mice died in utero at ≈ day 7 (Hudson et al, Current Biology, 2001), Sak +/− mice were viable and fertile. For the present studies, Sak +/+ and +/− mice were aged to 24 months, sacrificed and scored for tumours. We identified a significantly higher incidence of spontaneously-arising hepatomas in Sak +/− versus +/+ mice (42.2% v. 4.7%, respectively, p < 0.02). To determine whether cell cycle regulation is defective in Sak +/− animals, we used the partial hepatectomy (PH) model to induce synchronized proliferation of hepatocytes in the remnant liver. Gene expression was analyzed by real-time RT-PCR at 0, 24, 36, 40 and 72 hours post-PH. PH induced marked upregulation of Sak expression, which was maximal at 40 hours post-PH and was significantly reduced in Sak +/− compared with +/+ mice (≈ 10× less). Remnant livers of Sak +/− mice displayed delayed entry into S phase (Brdu labelling) and reduced entry into mitosis (decreased cyclin B1 levels, confirmed by Western blot), compared with Sak +/+ animals. We conclude that normal levels of Sak are required for proper cell-cycle progression in this in vivo model. Further, Sak deficiency predisposes to the development of spontaneous hepatomas in elderly mice, possibly through mitotic instability. To determine whether the observed defects in cell-cycle regulation contribute to carcinogenesis, we are currently evaluating the development of hepatomas post-PH in Sak +/− mice.
84. BLOOD TRANSFUSION IN CRC PATIENTS IS ASSOCIATED WITH INCREASED DISEASE-SPECIFIC MORTALITY
Introduction:
Debate continues regarding the impact of blood transfusions in the management of patients with colorectal cancer (CRC). Although immunosuppressive qualities of blood transfusion have been demonstrated, previous studies of patients with CRC have conflicted regarding the influence of transfusion on survival. The objective of this study was to determine the independent effect of transfusion on survival in CRC patients using Cox proportional hazards regression models.
Methods:
A cohort of consecutive, surgically treated CRC patients managed between 1994–1999 was identified. Prospective follow-up was collected until June 2002. Univariate analyses were performed to determine risk factors for transfusion. Logistic regression was used to develop a multivariable model describing the individual risk of transfusion. Factors affecting survival were analyzed in a univariate fashion by the Kaplan–Meier technique. A Cox proportional hazards model was then used to evaluate the independent effect of possible confounders along with transfusion.
Results:
398 patients with a median age of 71 years and a median follow-up of 31.5 months post-operation were analyzed. There were 135 (35%) deaths in follow-up. Transfusions were given to 137 (36%) patients. Univariate factors that were risks for transfusion included: age > 70 years, presenting hemoglobin level < 100 g/dL, estimated blood loss > 500 cc, additional surgery, and type of colorectal resection. The final logistic regression model identified that estimated blood loss > 500 cc, presenting hemoglobin < 100 g/dL and right hemicolectomy were independent, significant risks (p < 0.003) for transfusion in patients with CRC. The final Cox regression model showed that transfusion (HR = 1.7, 95% CI 1.1–2.5) and advanced stage (HR = 7.9, 95% CI 5.3–11.6) were the only significant factors affecting survival.
Conclusion:
Transfusion imparted a significantly negative impact on survival in the final multivariable Cox model. This further underscores the importance of efforts aimed at reducing transfusion rates in surgically treated CRC patients.
85. ADDITIONAL IMPACT OF ULTRASTAGING LYMPH NODES IN STAGE II COLORECTAL CANCER
Background:
Accurate identification of lymph-node (LN) metastases is critical for staging colorectal cancer (CRC) patients because decisions regarding prognosis and adjuvant chemotherapy are based upon this variable. We have previously shown that the number of LN assessed to render a diagnosis of “node-negative” CRC has a major predictive impact on 5-year survival (85% in high retrieval group v. 54% in low retrieval group, p < 0.001). The objective of this study was to assess the added ability to identify LN metastases through retrospectively ultrastaging retrieved LN.
Method:
398 consecutive patients operated on for CRC from 1994–99 were studied. One hundred thirteen patients were designated as stage II (node negative) using standard pathology processing of LN. In this investigation, all LN retrieved from this group of patients were step sectioned and examined after H & E and immunostaining using anticytokeratin (Cam 5.2) monoclonal antibody. Outcome data for overall and disease-specific survival as well as recurrence was assessed.
Results:
967 lymph nodes from 113 patients were evaluated. Ultrastaging required 50 hours of pathologist and technologist labour. 6 micrometastases were identified using this approach.
| Characteristic | Micro metastases − | Micro metastases + | p |
|---|---|---|---|
| Total patients, n | 107 | 6 | — |
| Median follow-up, mo | 39.0 | 60.5 | 0.17 |
| Tumour size, mean (cm) | 5.5 | 5.5 | 0.98 |
| T4 invasion, n (%) | 19 (17.7) | 3 (50) | 0.09 |
| Total lymph nodes retrieved, mean | 8.4 | 11.3 | 0.20 |
| Specimen length, mean (cm) | 29.8 | 23.4 | 0.12 |
| Lymphovascular invasion, % | 13.1 | 66.7 | 0.006 |
| Number receiving chemotherapy, n (%) | 18 (16.8) | 3 (50) | 0.08 |
| 5-year overall survival, % | 72.9 | 100 | 0.17 |
Conclusions:
Ultrastaging of LN is labour intensive and did not identify a large number of additional LN metastases. In addition, this approach did not identify a group with clearly worse prognosis. The group with micrometastases (which coincidentally had more T4 and LVI) received proportionally more chemotherapy, which may have affected survival. Our experience suggests that human resources are better expended in trying to maximize the number of LN retrieved and assessed in the standard fashion (in the OR and the pathology suite) rather than investing in costly ultrastaging manoeuvres.
86. DUCTAL CARCINOMA IN SITU IN CORE BIOPSIES CONTAINING INVASIVE BREAST CANCER: CORRELATION WITH EXTENSIVE INTRADUCTAL COMPONENT AND LUMPECTOMY MARGINS
Background:
The diagnosis of invasive breast cancer is most commonly made on image-guided core biopsy (CB). The presence of extensive intraductal component (EIC), as identified on subsequent lumpectomy, is associated with an increased risk of positive margins and need for further surgery. CBs demonstrating invasive breast cancer may also contain ductal carcinoma in situ (DCIS), although the significance of this finding is unclear. The objective of this study was to examine the implications of DCIS found in the original CB, specifically related to the risk of EIC and/or positive lumpectomy margins.
Methods:
All patients at a single academic institution who underwent initial breast conserving surgery for invasive breast cancer diagnosed on image-guided CB between 05/00–04/02 were included in the study. A systematic, blinded review of all CB and lumpectomy specimens was performed using standardized definitions of DCIS on CB, EIC and margins.
Results:
A total of 95 patients were included in the study, with a mean of 5 CB/patient. Of these, 43 (45%) patients had DCIS identified in their CB; in 34 (79%) of these patients the DCIS was mixed with the invasive cancer. No differences in age, tumour size or lumpectomy volume were identified between patients with or without DCIS on CB. Overall, EIC was identified in 13 (14%) patients; the risk of EIC was significantly higher in patients with DCIS than in those with invasive carcinoma alone (30% v. 0%, respectively; p < 0.0001). Expectedly, the incidence of positive margins on lumpectomy was higher in patients with EIC (38% v. 16%; p = 0.05). A trend, although not statistically significant, towards more positive margins was also noted in patients with DCIS on CB compared to those with invasive carcinoma alone (24% v. 15%, p = 0.3).
Conclusions:
The identification of DCIS in conjunction with invasive cancer on CB appeared important; the absence of DCIS ruled out the possibility of eventually finding EIC. Knowledge of DCIS on CB may be helpful for surgeons in planning gross resection margins at lumpectomy.
87. DEVELOPMENT OF A GENE THERAPY MODEL USING MYCOBACTERIAL Ag85A PLASMID DNA TO TREAT MALIGNANT MELANOMA
The disappointing lack of success in treating cutaneous malignant melanoma (CMM) with chemotherapies makes immunotherapy an attractive alternative approach. Bacillus Calmette–Guerin (BCG) immunotherapy has been successfully used in the treatment of in situ transitional cell bladder cancer. The mechanism is thought to involve a Type 1 immune response elicited by BCG in the bladder epithelium. Mycobacterial antigen 85A (Ag85A), a major secreted protein of Mycobacterium species, is associated with a Type 1 or DTH-like response in both humans and mice. This study evaluated the ability of Ag85A to limit tumour growth when transfected into B16-F10 melanoma cells.
Plasmid DNA that contained either no insert or the gene encoding Ag85A was transiently transfected into the B16-F10 mouse melanoma cell line by liposome-mediated transfection. Western blotting confirmed protein expression and secretion by transfected B16-F10 cells. C57BL/6 mice (5 per group) were injected subcutaneously with 105 untransfected B16-F10 cells or B16-F10 cells transiently transfected with either control plasmid DNA, or the vector that contained the gene for or Ag85A. C57BL/6 mice were also sensitized to Ag85 complex prior to injection of Ag85A transfected B16-F10 cells.
B16-F10 cells transiently transfected with the Ag85A plasmid, but not mock plasmid, exhibited approximately 50% reduced tumorigenicity when grown subcutaneously in syngeneic mice (p < 0.05, Welch’s alternative t-test). The decreased tumour weight was not due to a reduced ability of Ag85A transfected B16-F10 cells to proliferate. H & E staining revealed an inflammatory infiltrate associated with the Ag85A group of mice that received B16-F10 cells transfected with the Ag85A plasmid. Nevertheless, the reduction in tumour progression of Ag85A transfected B16-F10 cells suggests that immunotherapy based on inducing transient Ag85A expression by melanoma cells may be an attractive alternative approach for treating CMM.
88. PREDICTING THYMOMA INVASIVENESS: THE ROLE OF CT SCAN
Computer tomography (CT) remains the leading imaging modality to investigate mediastinal tumours including thymoma. However, the ability of CT to determine invasiveness of thymoma remains questionable.
Forty patients with a diagnosis of thymoma were identified using the Saskatchewan Cancer Centre database. Thirty-two patients had complete data available for analysis including CT, operative reports and pathology reports. The CT reports were compared to operative and pathology reports with pathology reports being considered the “gold standard” to determine invasiveness. CT correctly identified invasion in 9 out of 19 cases found to be invasive at operation. An additional 4 cases, totalling 23, revealed microinvasion into surrounding fat on pathologic examination. In 3 of the 9 cases demonstrating invasion, CT showed very advanced disease not amenable to surgical treatment. One of these 3 patients died soon after admission.
The sensitivity of CT in predicting invasiveness was 47.3% as compared to intraoperative diagnosis and 39.1% as compared to pathology evaluation. The accuracy of CT to predict invasion of thymoma into surrounding structures is relatively poor.
89. IMMUNOHISTOCHEMICAL ANALYSIS OF N2 MEDIASTINAL LYMPH NODES
The purpose of this study was to evaluate N2 mediastinal lymph nodes of non-small-cell lung cancer patients for presence of micrometastatic disease using immunohistochemistry.
Tissue blocks of N2 mediastinal lymph nodes obtained from patients with non-small-cell lung cancer were restained using ck-7, multi-ck and TTF-1 immunochemical stains. Presence or absence of micrometastases was correlated with survival data obtained from the Saskatoon Cancer Centre.
Thirty-eight patients with stage I and II non-small-cell lung carcinoma were identified and treated between January 1997 and December 2001. All patients had node-negative disease on routine histopathologic analysis and underwent resection of their primary tumour. Twenty-two of the 38 patients were identified as having micrometastases on multi-ck staining. Patients with micrometastases demonstrated a trend toward a poorer survival outcome (p = 0.13). Staining with ck-7 and TTF-1 showed no correlation with survival data.
Routine use of immunohistochemistry may help identify patients with poorer prognosis.
90. IMPORTANCE OF NODAL STATUS AND IMPACT OF MEDIASTINOSCOPY IN PREOPERATIVE STAGING OF PATIENTS WITH MALIGNANT PLEURAL MESOTHELIOMA
Introduction:
The presence of metastatic lymph nodes (LN) is a factor of poor prognosis in patients with malignant pleural mesothelioma. However, the value of mediastinoscopy in the preoperative staging of malignant pleural mesothelioma has not been analyzed systematically. We have, therefore, evaluated the importance of metastatic LN and the impact of mediastinoscopy in the treatment of malignant pleural mesothelioma.
Methods:
Retrospective review of 33 consecutive patients (25 men and 8 women, median age 58 yr) with malignant pleural mesothelioma undergoing extrapleural pneumonectomy (EPP) between 1993 and 2002 in our institution.
Results:
Tumours were right- (n = 14), or left-sided (n = 19). Perioperative mortality was 6% (2 deaths) and morbidity 33%. Although all patients had small (< 1.5 cm in greatest diameter) and non-suspect mediastinal LN on preoperative computed tomography (CT), 15 patients presented with extrapleural metastatic LN (45%) and 3 with intrapleural metastatic LN (9%) on final pathologic examination after EPP. Recurrence rate was significantly higher in patients with metastatic LN than in patients with N0 LN status (2-yr disease-free survival of 14% versus 54%, respectively; p = 0.009). Mediastinoscopy was performed preoperatively in 18 patients and was positive for metastatic mediastinal LN in only 1 patient. Of the 17 patients with negative mediastinoscopy, 9 were found to have extrapleural metastatic LN on final pathology. Metastatic LN were located in the aortopulmonary window, along the phrenic nerve, and in the lower mediastinum in 4 of these patients and, thus, were not accessible by cervical mediastinoscopy. The remaining 5 patients had metastatic LN along the trachea or in the subcarinal space that were not detected by mediastinoscopy.
Conclusions:
Metastatic LN is an important predictor of outcome that may help to select patients for EPP. However, in our experience, the negative predictive value of mediastinoscopy to detect extrapleural nodes is low (47%) and not significantly different from CT (44%). The low yield of mediastinoscopy in detecting metastatic LN may be due to the distribution of metastasis outside of the regions easily accessible by cervical mediastinoscopy and to the difficulty to detect small clusters of mesothelial cells on samples obtained by mediastinoscopy.
91. 15 YEARS’ SINGLE-CENTRE EXPERIENCE WITH SURGICAL RESECTION OF THE SUPERIOR VENA CAVA FOR NON-SMALL-CELL LUNG CANCER
Objectives:
The role of surgical resection for locally advanced non-small-cell lung cancer (NSCLC) invading the superior vena cava (SVC) is controversial. We examined our results in this group of patients.
Methods:
Retrospective analysis of patients who underwent surgical resection for NSCLC with direct SVC involvement, between 1988 and 2003. Postoperative morbidity and long-term outcome were reviewed. Risk factors for overall and disease-free survival were examined using Kaplan–Meier methods and log-rank test.
Results:
Of 21 patients who underwent SVC resection for thoracic malignancies, 13 were operated upon for NSCLC (7 males, 6 females). Median age was 60 years (28–78). None had SVC syndrome preoperatively. All patients had direct SVC invasion by tumour. All underwent mediastinoscopy as part of their staging. Six patients with N2 disease (discovered during mediastinoscopy in 5, and based on CT scan in 1) received induction therapy. Nine underwent lobectomy, and 4 had pneumonectomy (2 carinal). The SVC was replaced by interposition graft in 8 patients, whereas 5 had partial resection and repair. There were 2 (15%) postoperative deaths secondary to respiratory failure, and 3 (23%) major morbidities (1 postop SVC syndrome, 1 recurrent laryngeal nerve palsy and 1 cardiac herniation). No SVC-related late morbidities were observed. Mean follow-up time was 22 months (1–132, median 9). Overall 1- and 3-year survivals were 74% and 40%, respectively. Disease-free survival was 67.5% and 30%, respectively. All late deaths were due to recurrence. Survival of those with N2 disease was not significantly worse than those with localized (N0/N1) disease. There was a trend towards delay in recurrence in patients who had induction therapy (median disease-free interval of 34 mo v. 10 mo in the untreated group) although there was no significant effect on overall survival. The extent of lung resection and type of SVC resection (repair v. replacement) were not found to influence long-term survival.
Conclusions:
Carefully selected patients with NSCLC and SVC involvement can be operated upon with acceptable postoperative morbidity and mortality. In this small group of patients, no significant prognostic factors could be identified. SVC resection with curative intent should be considered for patients with NSCLC involving the SVC.
92. MINI-INVASIVE TRANSAXILLARY UPPER LOBECTOMY FOR LUNG CANCER PATIENTS
The purpose of this study is to report the experience of the Thoracic Surgery Service at the Vancouver General Hospital with lung cancer patients who underwent upper lobectomy by video-assisted procedure.
Retrospective chart review was carried out of patients with lung cancer who underwent upper lobectomy at Vancouver General Hospital between 1995 and 2001. They were divided into video-assisted, transaxillary lobectomy (VATSL) performed by surgeon 1 (group 1, n = 32), posterolateral thoracotomy (PLTL) by surgeon 1 (group 2, n = 24) and PLTL by surgeon 2 (group 3, n = 22). Demographic data, medical history, preoperative risk factors, surgical data and hospital stay information were recorded. Unpaired t-tests and χ2 were performed using significance levels of p < 0.05.
Group 1 showed a shorter total operating time than group 2 (186.9 v. 203.7 min, p = 0.043). Group 1 reported lower pain levels throughout hospital stay (p < 0.05 at 1st, 5th, 6th and 7th days) and used epidural catheter less times (p < 00.1) and received less epidural drugs (38.5 v. 119.7 mL, p = 0.000).
Comparison of group 1 with group 3 showed that VATSL reported lower pain levels throughout hospital stay (p < 0.05 at 1st, 3rd, 6th and 7th days) and needed less Leritine and epidural analgesic drugs (176.6 v. 570.8 mg, p = 0.019; 38.6 v. 132.4 mL, p < 0.000).
Group 1 compared to groups 2 + 3 confirmed the following: group 1 reported lower pain levels at 1st, 3rd and 5th days (p < 0.05). Epidural catheter was indicated less times for group 1 (p < 0.000). Total mg of morphine IV were higher in VATSL (p = 0.03) but paracetamol and Leritine were lower (p = 0.053 and p = 0.02, respectively).
This study suggests that lung cancer patients who underwent upper lobectomy by VATS presented lower pain levels with less-invasive analgesic management. The results indicate the need to conduct a randomized controlled trial with sufficient power and sample size to answer these questions.
93. A QUANTITATIVE APPROACH TO MAXIMIZING UTILIZATION OF SURGICAL RESOURCES FOR ELECTIVE OPERATIONS
The objective of this project was to devise a linear program based on quantitative approach of management science, which can then be used as a tool by the hospital managers and surgeons to maximize utilization of surgical services and resources for elective operations.
This maximization approach to resource management was focused on 4 commonly performed elective pulmonary operations in a thoracic surgery section of a tertiary-care hospital. Using linear programming formulation, a maximization model was constructed. The model looks at 8 constraints: minimum number of operations of each type, maximum number of operating room hours, number of available hospital beds, number of operating room nurses, number of anesthetists, recovery room beds, intensive care unit beds, and number of nurses on the ward. All the constraints were then quantified into the number of hours per month. The program was formulated based on 2 core alternative pathways. First, the demand for the surgical services made by a surgeon exceeds the available resources, and second, the resources offered to the surgeon exceeds or is equal to the surgeon’s demand.
The linear programming model was able to provide 2 sets of information. In situations where demand exceeded the available resources, the program was able to identify and quantify what constraints are the limiting elements. In other situations where resources matched or exceeded the demand, the program could identify and quantify the underused resources, and suggest which operations and in what quantities — from the pool of operations already designed into the program — can be added to the schedule.
Using our linear program as a blueprint, a more extensive model can be formulated that encompasses the activities of all the surgical services. This model will then allow for optimal utilization of the available resources to accommodate elective surgeries in a hospital.
94. CASPASE INHIBITION DECREASES APOPTOSIS AND LEADS TO IMPROVED LUNG FUNCTION IN A RAT MODEL OF LUNG TRANSPLANTATION
Previously, we have described significant apoptotic cell death in the lung following transplantation in humans and animals. Multiple pathways lead to programmed cell death; it is not known which are relevant in lung transplantation. Furthermore, the clinical significance of this cell death has not been studied.
In randomized blinded studies, syngeneic left single-lung transplantation (Lewis rats) was performed after 6 hours (n = 15) and 18 hours (n = 8) of cold ischemic storage (CIT). Animals and storage solutions were treated with caspase inhibitors or control. After transplantation and reperfusion, the Po2 level of the transplanted lung at FiO2 1.0 was used to assess lung function. Caspase 3, 8 and 9 activities in lung tissue lysates were measured through fluorometric assays. Lung samples were subjected to electron microscopy; TUNEL was used to evaluate apoptosis in paraffin-embedded lung sections.
After 6 hours CIT, transplantation and 2 hours reperfusion, the Pao2 levels, at FiO2 1.0, were not significantly different. However, after 18 hours CIT, transplantation and 2 hours reperfusion, the Pao2 levels at FiO2 1.0 were significantly higher in the caspase inhibitor group as compared to control. Caspase 3, 8 and 9 activities rose dramatically from baseline to 6 hours CIT and then dropped back down by 18 hours CIT in control animals. Animals treated with caspase inhibitor did not exhibit any significant changes in caspase activities. Electron microscopy demonstrated apoptotic cell death in endothelial cells and lymphocytes in control animals. TUNEL studies show that apoptosis was significantly reduced in animals treated with caspase inhibitor.
Activation of caspases during cold ischemia contributes significantly to ischemia-reperfusion induced apoptosis of endothelial cells and lymphocytes in lung transplantation. A systemically administered pan-caspase inhibitor successfully inhibited caspase activity in the lung, led to decreased TUNEL positivity, and improved lung function after 18 hours CIT, transplantation and 2 hours reperfusion.
95. LEVELS OF EVIDENCE AND GRADES OF RECOMMENDATIONS IN GENERAL THORACIC SURGERY
To determine the grades of recommendations and levels of evidence available if the formal practice of evidence-based medicine (EBM) is applied to general thoracic surgery.
Three general thoracic surgeons, by consensus developed a sample of 10 clinically important questions. The first 3 steps of evidence-based medicine (creation of answerable clinical questions, search for best external evidence, and. critical appraisal of literature) were performed. The best evidence found was categorized according to the Oxford Centre for Evidence-Based Medicine, grades of recommendations (A–D) and level of evidence (1–5).
Abstracts and appropriate articles were identified through MEDLINE January 1999–December 2001. A hierarchial series of search strategies was employed to identify the best level of evidence in order of systematic reviews then randomized controlled trials or other types of evidence.
The best evidence found for the 10 sample questions was categorized as grade A recommendations in 7 and grade B recommendations in 3. The levels of evidence found were 1a in 2 studies, 1b in 5, 2a in 1 and 2b in 2.
A formal evidence-based-medicine approach to general thoracic surgery found the grades of recommendation and levels of evidence for a sample of clinically important questions was high.
96. A PHASE II TRIAL OF INDUCTION CHEMOTHERAPY FOLLOWED BY EXTRAPLEURAL PNEUMONECTOMY AND HIGH-DOSE HEMITHORACIC RADIATION FOR MALIGNANT PLEURAL MESOTHELIOMA
Introduction:
We performed a single institution phase II trial with induction chemotherapy followed by extrapleural pneumonectomy (EPP) and high-dose hemithoracic radiation therapy for malignant pleural mesothelioma.
Methods:
Patients were eligible if they had a diagnosis of malignant pleural mesothelioma, a resectable tumour on computed tomography (CT) and adequate cardiopulmonary reserve to undergo EPP. Patients received 2–3 cycles of cisplatin/navelbine before EPP, and hemithoracic radiation (54 Gy) after EPP.
Results:
Between 06/01 and 12/02, 18 patients (13 men and 5 women, median age 59 yr) were eligible for the study. Nine patients (50%) completed the protocol. Two patients declined preoperative chemotherapy, 2 were found to have extensive disease at surgery and did not undergo EPP and 5 did not receive postoperative radiation therapy. Chemotherapy was performed in 16 patients and was well tolerated in all but 1 patient (fever and tachycardia). Chest CT was performed before and after chemotherapy to assess the response. Nine patients had no change in the bulk of disease, whereas 3 had minimal improvement and 1 had a partial response. Three patients had an increase in the size of the tumour during chemotherapy, and 2 of these were unresectable at surgery. Out of 16 patients undergoing EPP, 1 died postoperatively of arrhythmia and 7 developed complications (atrial fibrillation n = 2, recurrent nerve palsy n = 2, mild temporary kidney dysfunction n = 1, wound infection n = 1, and esophageal perforation n = 1). Eleven patients received postoperative hemithoracic radiation therapy to a total dose of 54 Gy. Fatigue (n = 8), skin erythema (n = 6), nauseas (n = 4) and esophagitis (n = 3) were often seen, but no major complications were observed. The 1-year disease-free survival for the 9 patients who completed the protocol was 74%, and tended to be better than for the remaining patients who underwent EPP but did not complete the protocol (1-year disease-free survival of 33%, p = 0.2).
Conclusions:
Induction chemotherapy followed by EPP and high-dose hemithoracic radiation is an aggressive but tolerable regimen for selected patients with malignant pleural mesothelioma. This approach may delay recurrence and improve survival. New chemotherapy regimens are needed to increase the response rate before surgery.
97. A TWELVE-YEAR EXPERIENCE WITH ESOPHAGEAL RESECTION FOR MALIGNANT DISEASE OF THE ESOPHAGUS IN THE REGINA HEALTH DISTRICT
The outcome of all surgical resections of the esophagus or gastroesophageal junction (GEJ) for malignant disease undertaken in all 3 hospitals of Regina from Jan. 1, 1989–Dec. 31, 2001 was retrospectively reviewed. A total of 129 patients were taken to the operating room; 119 underwent esophageal resection. Ten procedures were abandoned due to unresectable disease.
There were 16 postoperative deaths (13.4%). Perioperative morbidity was high, with 26 patients experiencing anastomotic leaks (21.8%); anastomotic strictures occurred in 32 patients (26.9%). Respiratory complications were frequent with 22 patients (18.5%) developing respiratory failure postoperatively requiring reintubation and ventilation (for a mean of 202.8 h). Atelectasis occurred in 102 patients (85.7%), pulmonary edema in 30 patients (25.2%), pneumonia in 21 patients (17.6%) and aspiration documented in 9 patients (7.6%).
Resource utilization was extensive with a mean hospital length of stay of 23.9 days (range 0–196 d). The mean ICU stay was 5.4 days (range 0.2–32 d).
Procedures were carried out by 14 members of the Divisions of General Surgery or Cardiovascular and Thoracic Surgery in the 3 Regina hospitals. Individual surgeon experience ranged from 1–46 cases over the 12-year interval. Perioperative mortality rates by individual surgeon ranged from 0%–50%.
The Regina-Qu’Appelle Health Region’s Department of Surgery lacks a defined management pathway for malignant diseases of the esophagus or GEJ. Individual surgeon volumes are generally low and may contribute to high perioperative mortality and morbidity rates observed in the Regina Hospitals. Development of a specialized unit to maximize clinical experience of health care providers would appear to be a reasonable approach to improve patient outcome.
98. CONTEMPORARY MANAGEMENT OF RUPTURE OF THE DESCENDING THORACIC AORTA
Objectives:
To evaluate to the current role(s) of CT angiogram (CTA), nonoperative and endovascular approaches in managing traumatic thoracic aortic rupture (TAR).
Methods:
A retrospective review of patients admitted between 02/1998–3/2003 with injuries in the descending thoracic aorta. Patients were categorized as unstable if systolic pressure < 90 within 1 hour of admission. Repair was emergent if performed < 24 hours after admission, delayed if > 24 hours.
Results:
46 (38 male, age 37.8 ± 18.4 yr, Injury Severity Score 43.5 ± 15.6) patients were admitted with overall mortality 12 (26%) due to: free rupture prior to control (3), closed head injury (2), cardiac causes (4), pulmonary embolism (1), late bleed (1), ARDS (1). Mortality by category was as follows: emergent (including 3 with free rupture) 10/32 (31%) versus delayed 2/8 (25%) versus nonoperative 0/6; stable 5/36 (14%) versus unstable 7/10 (70%); operative repair 9/30 (30%) versus endovascular stent graft 3/10 (30%). Multi-regression analysis identified that stable patients were 5.7 times more likely to survive than unstable (CI 2.0–15.6). The diagnosis was made by angiogram in 29 (63%) cases, including 6 at the time of embolization and by CTA in 17 (37%). Time to operating room in the urgent group was 2.9 ± 1.4 hours after CTA versus 4.4 ± 1.5 hours after angiogram (p = 0.02). The most common indication for not performing emergent intervention was acute lung injury (7), and no patient in the delayed and nonoperative groups (11/13 treated with beta blockade) suffered free rupture.
Conclusions:
Selective use of endovascular stent grafts and nonoperative therapy is appropriate. Mortality is primarily linked to patient stability. Angiograms should be used to make the diagnosis if embolization is required, but CTA [may] be quicker in other cases.
99. VATS SYMPATHECTOMY AND SYMPATHICOTOMY IN PATIENTS WITH PRIMARY PALMAR HYPERHIDROSIS
VATS sympathectomy is the most frequently used technique for surgical hyperhidrosis of the upper limbs. It has proven to be particularly effective.
Objective:
To evaluate the role of VATS in management of palmar hyperhidrosis.
Patients and methods:
40 cases undergoing VATS for palmar hyperhidrosis, in 2 groups. Group I 20 patients (sympathectomy), group II 20 patients (sympathicotomy).
Results:
Mean operation time 23.47 ± 2.85 minutes in resection, and 18.87 ± 2.07 minutes in division. The mean duration of the operation was significantly longer in group I when compared with group II. Main outcome measures included incidence of dry hands, compensatory hyperhidrosis and recurrence. After both procedures 100% reported significant improvement of palmar hyperhidrosis. Post-surgery compensatory hyperhidrosis was experienced in 3.3% of cases, and 6.66% showed partial recurrence. VATS is a very useful, speedy and safer way than conventional thoracotomy in managing cases of palmar hyperhidrosis, with excellent cosmetic results while minimizing complications.

