Abstract
Background
Although laparoscopic cholecystectomy (LC) results in less pain then open cholecystectomy, it is not a pain-free procedure. The aim of this study was to test a new method of preemptive analgesia.
Methods
By simple randomization 60 patients were assigned to two groups (30 in each group). Group A, the placebo group, received 200 ml of 0.9% saline, and group B received 5 mg/kg of a local anesthetic solution (ropivacaine) in 200 ml of 0.9% saline. Local anesthetic or place solution were administer before creation of the pneumoperitoneum.
Results
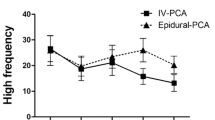
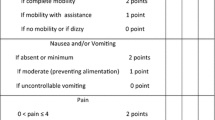
Pain intensity, as rated by visual analog and verbal rating scales, and stress response data were significantly less in the group receiving ropivacaine than in the placebo group. No patients in treatment group received an additional dose of analgesic, whereas two patients in placebo group needed an additional analgesic.
Conclusions
Our results support the clinical validity of preemptive analgesia, but the timing of intraperitoneal administration of local anesthetic is very important. Only application before creation of the pneumoperitoneum may preempt every neuronal central sensitization.
Similar content being viewed by others
References
Aitola P, Airo I, Kaukinen S, Ylitalo P (1998) Comparison of N2O and CO2 pneumoperitoneums during laparoscopic cholecystectomy with special reference to postoperative pain. Surg Laparosc Endosc 8: 140–144
Attwood SEA, Hill ADK, Mealy K, Stephens RB (1992) A prospective comparison of laparoscopic versus open cholecystectomy. Ann R Coll Surg Engl 74: 397–400
Berggren U, Gordh T, Grama D, Haglund U, Rastad J, Arvidsson D (1994) Laparoscopic versus open cholecystectomy: hospitalization, sick leave, analgesia, and trauma responses. Br J Surg 81: 1362–1365
Callery MP, Soper NJ (1993) Physiology of pneumoperitoneum. Ballieres Clin Gastroenterol 7: 757–777
Comyn DJ (1998) Minimizing pain after laparoscopy. In: Abstracts of the 9th World Congress of Anaesthesiologists, p A0004
Fuhrer Y, Charpentier C, Boulanger G, Menu N, Grosdidier G, Laxenaire MC (1996) Analgesia after laparoscopic cholecystectomy by intraperitoneal administration of bupivacaina, Ann Fr Anesth Reanim 15: 128–134
Hunter JG, Staheli J, Oddsdottir M, Trus T (1995) Nitrous oxide pneumoperitoneum revisted: is there a risk of combustion? Surg Endosc 9: 501–504
Jackson SA, Laurence AS, Hill JC (1996) Does postlaparoscopy pain relate to residual carbon dioxide? Anaesthesia 51: 485–487
Joris J, Thiry E, Paris P, Weerts J, Lamy M (1995) Pain after laparoscopic cholecystectomy: characteristics and effect of intraperitoneal bupivacaine. Anesth Analg 81: 379–384
Junghans T, Bohm B, Grundel K, Schwenk W (1997) Effects of pneumoperitoneum with carbon dioxide, argon, or helium on hemodynamic and respiratory function. Arch Surg 132: 272–278
Katz J, Melzack R (1999) Measurement of pain. Surg Clin North Am 79: 231–252
Knudsen K, Beckman Suurkula M, Blomberg S, Sjovall J, Edvardsson N (1997) Central nervous and cardiovascular effects of IV infusions of ropivacaine, bupivacaine, and placebo in volunteers. Br J Anaesth 78: 507–514
Korell M, Schmaus F, Strowitzki T, Schneeweiss SG, Hepp H (1995) Pain intensity following laparoscopy. Surg Laparosc Endosc 6: 375–379
Mjaland O, Reader JC, Aasboe V, Trondsen E, Buanes T (1997) Outpatient laparoscopic cholecystectomy. Br J Surg 84: 958–961
Mouton WG, Bessel JR, Millard SH, Baxter PS, Maddern GJ (1998) A randomized controlled trial assesing the benefit of humidified insufflation gas during laparoscopic surgery. Surg Endosc 13: 106–108
Mouton WG, Bessel JR, Otten KT, Maddern GJ (1999) Pain after laparoscopy. Surg Endosc 13: 445–448
Mraovic B, Jurisic T, Kogler-Majeric V, Sustic A (1997) Intraperitoneal bupivacaine for analgesia after laparoscopic cholecystectomy. Acta Anaesthesiol Scand 41: 193–196
Neuberger TJ, Andrus CH, Wittgen CM, Wade TP, Kaminski DL (1996) Prospective comparison of helium versus carbon dioxide pneumoperitoneum. Gastrointest Endosc 43: 38–41
Neuhaus SJ, Texler M, Hewett PJ, Watson DI (1998) Port-side metastases following laparoscopic surgery. Br J Surg 85: 735–741
Nyerges A (1994) Pain mechanism in laparoscopic surgery. Semin Laparosc Surg 1: 215–218
Pasqualucci A, de Angelis V, Contardo R, Colo F, Terrosu G, Donini A, Pasetto A, Bresadola F (1996) Preemptive analgesia: intraperitoneal local anaesthetic in laparoscopic cholecystectomy: a randomized double-blind, placebo-controlled study. Anesthesiology 85: 11–20
Pier A, Benedic M, Mann B, Buck V (1994) Das postlaparoskopische schmerzsyndrom. Chirurg 65: 200–208
Ure BM, Troidl H, Spangenberger W, Dietrich E, Lefering R, Neugebauer E (1994) Pain after laparoscopy cholecystectomy: intensity and localization of pain and analysis of predictors in preoperative symptoms and intraoperative events. Surg Endosc 8: 90–96
Volz J, Koster S, Weiss M, Schmidt R, Urbaschek R, Melchert F, Albrecht M (1996) Pathophysiologic features of a pneumoperitoneum at laparoscopy: a swine model. Am J Obstet Gynecol 174: 132–140
Wallace DH, Serpell MG, Baxter JN, O’Dwyer PJ (1997) Randomized trial of different insufflation pressures for laparoscopic cholecystectomy. Br J Surg 84: 455–458
Woolf CJ, Mannion RJ (1999) Neuropathic pain aetiology, symptoms, mechanism, and management. Lancet 353: 1959–1964
Zegarra RF II, Saba AK, Peschiera JL (1997) Outpatient laparoscopic cholecystectomy: safe and cost effective? Surg Laparosc Endosc 7: 487–490
Author information
Authors and Affiliations
Additional information
Online publication: 7 May 2002
Rights and permissions
About this article
Cite this article
Maestroni, U., Sortini, D., Devito, C. et al. A new method of preemptive analgesia in laparoscopic cholecystectomy. Surg Endosc 16, 1336–1340 (2002). https://doi.org/10.1007/s00464-001-9181-8
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s00464-001-9181-8