Abstract
Background
An increasing trend in the use of contralateral prophylactic mastectomy (CPM) for the treatment of unilateral breast cancer has been observed nationally. The purpose of this study was to confirm this trend and to identify differences between the groups that chose unilateral mastectomy alone or with CPM.
Methods
A prospectively maintained breast cancer database was retrospectively reviewed. Age, histologic grade, stage, education, family history, tumor receptor status, and use of immediate reconstruction were evaluated. Statistical analysis was performed by Fisher’s exact test, χ2 test, and Student’s t-test.
Results
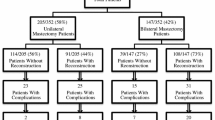
Between 1998 and 2007, a total of 1639 women who selected UM and 201 who had UM and CPM for unilateral breast cancer were identified. An increasing trend in CPM was observed (6.5% in 1999 vs. 16.1% in 2007). The CPM group was significantly younger (mean age 47.8 vs. 55.1 years, P < .001). No difference in histologic grade was noted between the two groups; however, an increasing trend toward CPM was observed with lower-stage disease. Women with a higher educational level were more likely to have CPM (P < .001). Women with a family history of cancer were also more likely to have CPM (57% vs. 41%, P < .001). Use of reconstruction was similar between the groups (6.0% for CPM vs. 6.7% for UM, P = NS).
Conclusions
Our experience parallels the national trend of increasing use of CPM in women diagnosed with unilateral breast cancer. Women who chose to have CPM were younger, more highly educated, and more likely to have a family history of cancer.




Similar content being viewed by others
References
Abrams JS, Phillips PH, Friedman MA. Meeting highlights: a reappraisal of research results for the local treatment of early stage breast cancer. J Natl Cancer Inst. 1995;87:1837–45.
Tuttle TM, Habermann EB, Grund EH, Morris TJ, Virnig BA. Increasing use of contralateral prophylactic mastectomy for breast cancer patients: a trend toward more aggressive surgical treatment. J Clin Oncol. 2007;25:5203–9.
Herrinton LJ, Barlow WE, Yu O, et al. Efficacy of prophylactic mastectomy in women with unilateral breast cancer: a Cancer Research Network project. J Clin Oncol. 2005;23:4275–86.
Robbins GF, Berg JW. Bilateral primary breast cancer, a prospective clinicopathological study. Cancer. 1964;17:1501–27.
Chaundary MA, Mills RR, Hoskins EO, et al. Bilateral primary breast cancer: a prospective study of disease incidence. Br J Surg. 1984;71:711–4.
Rosen PP, Groshen S, Kinne DW, et al. Contralateral breast carcinoma: an assessment of risk and prognosis in stage I (TINOMO) and stage II (T1N1M0) patients with 20-year follow-up. Surgery. 1989;106:904–10.
Vogel VG, Costantino JP, Wickerham DL, et al. Effects of tamoxifen vs raloxifene on the risk of developing invasive breast cancer and other disease outcomes: the NSABP Study of Tamoxifen and Raloxifene (STAR) P-2 trial. JAMA. 2006;295:2727–41.
Lostumbo L, Carbine N, Wallace J, et al. Prophylactic mastectomy for the prevention of breast cancer. Cochrane Database Syst Rev. 2004;4:CD002748.
Peralta EA, Ellenhorn JD, Wagman LD, et al. Contralateral prophylactic mastectomy improves the outcome of selected patients undergoing mastectomy for breast cancer. Am J Surg. 2000;180:439–45.
Wood W. Increasing use of contralateral prophylactic mastectomy: a counterintuitive trend. (The CON Perspective). Oncology. 2008;22:548–51.
Hemminki K, Jianguang J, Forsti A. Risks for familial and contralateral breast cancer interact multiplicatively and cause a high risk. Cancer Res. 2007;67:868–70.
Verhoog LC, Brekelmans CT, Seynaerve C, et al. Survival and tumour characteristics of breast-cancer patients with germline mutations of BRCA 1. Lancet. 1998;351:316–21.
Metcalfe K, Lynch HT, Ghadirian P, et al. Contralateral breast cancer in BRCA1. and BRCA2. mutation carriers. J Clin Oncol. 2004;22:2328–35.
Liebens FP, Carly B, Pastijn A, Rozenberg S. Management of BRCA1/2. associated breast cancer: a systematic qualitative review of the state of knowledge in 2006. Eur J Cancer. 2007;43:238–57.
McDonnell SK, Schaid DJ, Myers JL, et al. Efficacy of contralateral prophylactic mastectomy in women with a personal and family history of breast cancer. J Clin Oncol. 2001;19:3938–43.
van Sprundel TC, Schmidt MK, Rookus MA, et al. Risk reduction of contralateral breast cancer and survival after contralateral prophylactic mastectomy in BRCA1. or BRCA2. mutation carriers. Br J Cancer. 2005;93:287–92.
Tuttle TM. Counseling breast cancer patients on contralateral prophylactic mastectomy: the physician’s role. Oncology. 2008;5:545–8.
Nekhlyudov L, Bower M, Herrinton LJ, et al. Women’s decision-making roles regarding contralateral prophylactic mastectomy. J Natl Cancer Inst. Monogr. 2005;35:55–60.
Frost MH, Slezak JM, Tran NV, et al. Satisfaction after contralateral prophylactic mastectomy: the significance of mastectomy type, reconstructive complications, and body appearance. J Clin Oncol. 2005;23:7849–56.
Montgomery LL, Tran KN, Heelan MC, et al. Issues of regret in women with contralateral prophylactic mastectomies. Ann Surg Oncol. 1999;6:546–52.
Geiger AM, West CN, Nekhlyudov L, et al. Contentment with quality of life among breast cancer survivors with and without contralateral prophylactic mastectomy. J Clin Oncol. 2006;24:1350–6.
Acknowledgment
This study is not supported by any grant support. The authors indicate no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jones, N.B., Wilson, J., Kotur, L. et al. Contralateral Prophylactic Mastectomy for Unilateral Breast Cancer: An Increasing Trend at a Single Institution. Ann Surg Oncol 16, 2691–2696 (2009). https://doi.org/10.1245/s10434-009-0547-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-009-0547-9