Abstract
Objectives: To assess the surgical technique and the frequency of different types of antireflux surgery used in Canada after the introduction of laparoscopic antireflux surgery.
Design: Gastroesophageal reflux (GER) surgery and population data in fiscal years 1992 through 1996. were accessed through the Canadian Institute of Health Information, provincial health ministries, MED ECHO and Statistics Canada databases. Data were also analysed by province and nationally for type of surgery (e.g., open abdominal, thoracic, thoracoscopic and laparoscopic).
Results: National data showed a slight increase in GER surgery in the last 5 years. Laparoscopic surgery increased 2.8 fold in 1993 and 1.6 fold in 1995 over the previous years. Open abdominal cases decreased 1.1 fold from 1992 to 1996. Thoracic cases remained essentially unchanged. Provincial and regional disparities in procedures per 100 000 population exist (Ontario 7.1 versus Nova Scotia 20.7). Areas in which little or no laparoscopic surgery was done had an average increase of 3%, whereas areas in which laparoscopic surgery was done had an average increase of 16% in GER surgery during the course of the study. In provinces west of Quebec (with the exception of Manitoba) more than 50% of GER surgery is laparoscopic; in areas east of Ontario less than 25% of GER surgery is performed laparoscopically. Five provinces (Manitoba, Quebec, Nova Scotia, Prince Edward Island and Newfoundland) performed significantly fewer laparoscopic procedures than the national average.
Conclusions: The frequency of GER surgery is increasing modestly in Canada and is performed most often by the open abdominal route. Regional disparities in open and laparoscopic techniques are apparent. Laparoscopic surgery for GER is increasing rapidly and accounts for the decrease in open GER surgery.
Gastroesophageal reflux disease (GERD) is endemic in Canada. Up to 40% of adults have symptoms. The key to treatment is effective maintenance therapy with proton pump inhibitors. The other alternative is antireflux surgery. Studies have shown that surgery for GERD is effective, and cost-effectiveness studies have confirmed its benefit in younger patients.1,2
Since the introduction of laparoscopic cholecystectomy, surgeons’ and patients’ attitudes toward biliary tract surgery have changed dramatically. In fact, the change in the overall provision of health care related to the diagnosis of cholelithiasis and its related diseases is based solely on the laparoscopic approach.3 Studies have demonstrated the benefit of laparoscopic biliary tract surgery with respect to pain, length of hospital stay and time to full recovery.4–6 Randomized controlled trials of laparoscopic cholecystectomy compared with open cholecystectomy have shown the superiority of the laparoscopic technique. 7 However, after widespread adoption of this procedure, complications unique to the laparoscopic technique began to appear.8–11 Also, known complications of open cholecystectomy (e.g., bile-duct injuries) were reported with increased frequency after use of the laparoscopic technique.8,9 These findings have spawned a new series of papers in the literature on prevention and management of these complications.9,10 With the public’s increased awareness of health care issues and technologic advances it was not surprising that patient demand, in part, led to the explosion of laparoscopic cholecystectomy before adequate controlled clinical trials were performed. The laparoscopic era for gastrointestinal surgery also led to changes in health care delivery, placing greater emphasis on ambulatory or short-stay surgery.
Some authors have questioned the value of the laparoscopic antireflux surgical technique.12 If laparoscopic antireflux surgery is seen as an effective alternative to lifelong medication, it must be be based on sound rationale and be performed on the “right” patients as determined by clinical criteria and objective diagnostic tests. The first report of a laparoscopic Nissen fundoplication was in 1991.13 Since then, reports of laparoscopic Nissen fundoplication and laparoscopic Hill repair have appeared. 14,15 Outcome studies looking at physiologic assessment, symptoms and quality of life measures have shown good results in 93% to 96% of patients having typical symptoms of GERD.16–18 To answer the question: Is antireflux surgery increasing or decreasing in Canada and to what extent has this been influenced by the advent of laparoscopic surgery? we searched the Canadian health databases.
Methods
The Canadian Institute for Health Information (CIHI), provincial health ministries and MED ECHO databases were accessed for antireflux surgery data during fiscal years 1992/93, 1993/94, 1994/95 and 1995/96. The data were provided by geographic area, provincially and nationally, and included the numbers of antireflux procedures listed by operative approach (e.g., laparoscopic, open abdominal, thoracoscopic, and thoracic) but not the specific technique used (i.e., Nissen, Hill or Belsey procedure). When CIHI information was incomplete, the health ministry of that province was contacted to obtain the missing data. The data for Quebec were completely supplied by the Quebec Ministry of Health through the MED ECHO database. Statistics Canada provided national, provincial and municipal population data. A municipal database was created but does not take into account the population of the referral area for individual cities, making the rate per 100 000 population of questionable significance. The data were analysed using Lotus 123 97 and Approach 97.
Results
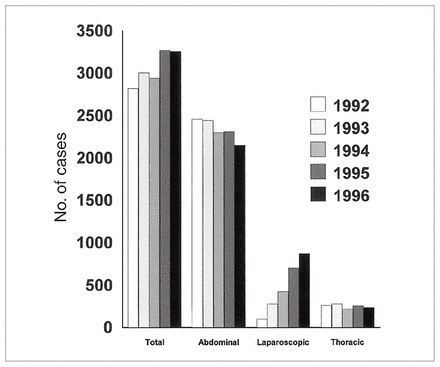
The number of antireflux procedures performed in each province is shown in Table I. Thoracoscopic antireflux surgery is not performed commonly in Canada. The data are presented graphically for the fiscal year 1996 in Table II. It is evident that provincial disparities exist in the use of antireflux surgery. The rate of antireflux surgery in 1996 per 100 000 population for all of Canada was 11.4. Prince Edward Island had the lowest rate at 3.0, and Nova Scotia had the highest rate at 19.6. Disparities also exist in the use of laparoscopic antireflux surgery (LS). The rate of LS is highest in Alberta and the western provinces with the exception of Manitoba and, with the exception of New Brunswick, is performed minimally east of Ontario and in the 2 territories. There has been a marked increase in the utilization of laparoscopic GER surgery (Fig. 1). Between 1992 and 1996, those regions using LS at or above the national average had an overall 16% increase in GER surgery. This compares with a 3% increase in the use of antireflux surgery in those provinces where LS is not prominent and with a 3.5% decrease in the overall national use of antireflux surgery. In those regions where essentially no laparoscopic surgery was performed in 1996, there was a net decrease of 6.5% in their overall antireflux surgery rates between 1992 and 1996. Five regions that performed 2 or fewer laparoscopic repairs per year in fiscal year 1993 (Manitoba, Quebec, Nova Scotia, Prince Edward Island and Newfoundland) stopped performing laparoscopic surgery thereafter. Thirteen regions started performing laparoscopic antireflux surgery after fiscal year 1993.
National antireflux surgery rates by year.
National Date of Antireflux Procedures Performed Between Fiscal Years 1992 and 1996
National and Provincial Antireflux Surgery Rates for the Fiscal Year 1996*
Discussion
Concerns exist among many esophageal surgeons that the rigid indications for GER surgery may be relaxed and that inappropriate antireflux surgery will be performed simply because it can be done laparoscopically.19 Because of the increasing interest in laparoscopic surgery, a concern for patient welfare, and the availability of laparoscopic fundoplication, the number of patients referred for laparoscopic GER surgery is likely to increase, so the concerns may be valid. Such findings have been reported for laparoscopic cholecystectomy.20 Laparoscopic antireflux surgery is one of a number of advanced laparoscopic techniques now becoming more readily available. Although the learning curve for mastery of the GER technique is much longer than for cholecystectomy, surgeons may believe that it is simply a natural extension to their skills acquired in biliary tract surgery. This belief combined with the perceived benign nature of laparoscopic procedures could lead to a proliferation of this operation by surgeons not skilled in analysing patients with suspected GERD. However, as shown in our study, laparoscopic surgery has not yet resulted in a marked proliferation of the number of antireflux procedures.
We found that the use of antireflux surgery to control the symptoms of GERD varies widely from one geographic area to another. This finding could be explained in part by the referral patterns of the gastroenterologists and family doctors. The data also support a national trend toward increasing use of laparoscopic antireflux surgery with a consequent reduction in open abdominal techniques.
It is of concern that in some regions using laparoscopic surgery only a few such procedures are performed each year. This study could not identify if these procedures were performed by a single surgeon or by several surgeons. Any future outcome studies for GER surgery must evaluate what objective investigations are utilized preoperatively in regions where antireflux surgery is done. Laparoscopic techniques are still evolving, so outcome studies will need to evaluate these changes for established laparoscopic esophageal surgeons also.
Conclusions
The future of laparoscopic antireflux surgery and its place in the management of GERD is still unclear, but it appears that Canadian surgeons are adopting the laparoscopic approach in place of the open approach. We conclude that, unlike the situation after the introduction of laparoscopic cholecystectomy, the introduction of laparoscopic antireflux procedures has not yet resulted in an increase in GER surgery, which is still performed most often by the open abdominal route. Marked regional disparities in open and laparoscopic surgery are apparent. Although this study did not look at the reasons behind such differences, we conclude that since this type of surgery is performed on patients who have usually been evaluated by gastroenterologists, practice referral patterns could account for the disparities. Laparoscopic surgery is infrequent but is increasing rapidly, and the increase in laparoscopic GER surgery has been coincident with a decrease in open GER surgery. The number of centres offering laparoscopic GER surgery is also increasing.
Footnotes
Presented in part at the annual meeting of the Royal College of Physicians and Surgeons of Canada, Montreal,Que., September 1996 and at the Canadian Association of General Surgeons Resident Research Retreat, Mississauga, Ont., June 1996.
- Accepted June 14, 1999.