Abstract
Background: Total knee replacement is now the most common joint replacement procedure performed in Ontario, and many patients require bilateral replacement. However, whether bilateral total knee arthroplasty (TKA) should be staged or simultaneous is hotly debated. To determine the current common operative practices of orthopedic surgeons in Ontario, we carried out a province-wide survey.
Methods: Orthopedic surgeons from Ontario listed in the 1999 Canadian Medical Directory or the membership list of the Canadian Orthopaedic Association were sent questionnaires, asking about their practice in the timing of bilateral TKA, tourniquet use, type of guide and use of techniques to minimize fat embolization.
Results: Of the 416 surveys mailed, 219 (53%) surgeons responded. The majority responded that they perform staged bilateral TKA (28% 3-mo interval and 37% 6-mo interval). Simultaneous TKA with 2 teams was the least performed procedure (2%). When performing bilateral TKA, 95% of surgeons use an intramedullary femoral alignment guide, 78% utilize an over-reamed entry hole and 53% suction the canal before inserting the guide rod. With respect to the tibia, 32% use an intramedullary guide, 60% over-ream the entry hole and 60% suction the entry hole; 22% of surgeons stated that they had never considered over-reaming or suctioning the canal to minimize fat embolization.
Conclusions: There is no consensus regarding the timing of bilateral TKA in Ontario. Furthermore, many surgeons are not overdrilling or suctioning the femoral canal despite evidence in the literature that overdrilling may be beneficial in decreasing fat embolization. Further research is required to compare the risk of complications of bilateral TKA after staged versus simultaneous TKA.
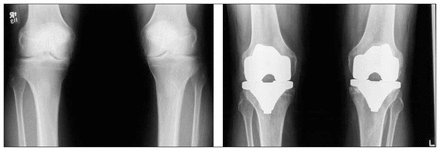
Over the last 10 years, the rate of total knee replacement has tripled such that it is now the most common joint replacement procedure in Ontario, with a rate approximating 90 per 100 000 people.1 Many of these patients suffer from arthritis in both knees (Fig. 1), necessitating bilateral total knee arthroplasty (TKA). Almost 19% of all knee replacements in the United States from 1985 to 1990 were bilateral procedures (either staged or simultaneous).2
Standing anteroposterior view of the knees of a 70-year-old man suffering from severe bilateral knee osteoarthritis (left). Follow-up view 1 year after bilateral total knee arthroplasty (right).
At present, there is a heated debate regarding the timing of bilateral joint replacement surgery. When both knees have failed conservative management and require joint replacement, the question remains: should bilateral TKAs be performed simultaneously, sequentially (under the same anesthetic) or staged (under a separate anesthetic)? It follows that when both knees are affected by end-stage osteoarthritis, replacement of 1 of the 2 joints does not fully restore a patient’s function, and the patient remains significantly debilitated. Thus, some advocate simultaneous bilateral knee replacement (involving 1 anesthetic),3 whereas others routinely stage the operations from 1 week4 to 1 year2 apart.
There are advantages and disadvantages to each approach. Staged bilateral TKA requires 2 hospitalization and 2 rehabilitation experiences. This places a higher financial burden on the health care system, although each procedure, individually, may place less of a burden on caregivers, physiotherapists and nurses. In contrast, patients receiving simultaneous bilateral TKA return to full function earlier, experience less total anesthetic exposure, and the procedure is more cost-effective.2,3 Simultaneous bilateral TKAs may be associated with a higher rate of blood transfusion requirements,5 cardiopulmonary complications and death due to fat embolism when compared with a single knee replacement.6,7 These potentially higher risks associated with simultaneous bilateral TKA are thought to be the main reason surgeons are reluctant to perform bilateral TKA simultaneously.
Our purpose in this study was to determine the current operative practices of Ontario’s orthopedic surgeons performing bilateral TKA. We wanted to determine whether safe and effective practices are in place and whether these practices contribute to the concerns of orthopedic surgeons with respect to simultaneous TKA.
Methods
Sample
A total of 416 orthopedic surgeons were identified from the 1999 Canadian Medical Directory and the Canadian Orthopaedic Association membership list and were sent questionnaires. As a tracking mechanism, each survey was numbered. Surgeons who did not respond received only 1 follow-up telephone call.
Survey
To examine the practice patterns among orthopedic surgeons in performing bilateral TKA, the survey comprised questions related to the timing of these procedures. Surgeons were asked to identify the timing they predominantly use for bilateral TKA from the following options: staged with 2 hospital visits 3, 6 or 12 months apart; staged with 1 hospital visit; sequential with 1 anesthetic; simultaneous with 1 team; simultaneous with 2 teams and 1 or 2 set-ups. Data on tourniquet use, extramedullary versus intramedullary alignment guide use, and whether entry holes are over-reamed or suctioned at the time of guide insertion were also gathered. A pilot questionnaire was first sent to a sample of 10 orthopedic surgeons and then modified according to their suggestions.
Analysis
Statistical analysis was performed using SPSS version 10.0. Frequency distributions were calculated for the responses to each question. To examine the influence on responses of the number of years in practice, surgeons were divided into 2 groups: those who graduated from medical school in 1979 or earlier (earlier graduates) and those who graduated from medical school in 1980 or later (more recent graduates). The cut-off at 1979 was based on the median year of graduation from medical school of the respondents and that the more recent graduates would represent surgeons in practice for fewer than 20 years. Comparisons of proportions (e.g., 1 v. 2 anesthetics) between the groups were made using χ2 tests. Probability values less than 0.05 were considered significant.
Results
Overall, 219 (53%) of the 416 orthopedic surgeons responded to the questionnaire. Of these, 153 (70%) reported that they currently perform TKA (Table 1). The majority of surgeons perform staged bilateral TKA, with 28%, 37% and 3% of surgeons performing bilateral TKA 3, 6 and 12 months apart, respectively. Only 3% perform staged bilateral TKA during 1 hospital visit. Simultaneous TKA with 2 teams and 2 set-ups was the least performed (2%). Twelve percent of surgeons reported that they perform simultaneous bilateral TKA with 1 team, and 15% perform sequential bilateral TKA under 1 anesthetic. There were no differences between earlier and more recent graduates with respect to performing staged, sequential or simultaneous bilateral TKA, nor was there any difference in the use of 1 versus 2 anesthetics.
Operative bilateral total knee arthroplasty (TKA) practices of Ontario’s orthopedic surgeons
With respect to tourniquet use, all but 10% of procedures were performed with sequential tourniquet use. Only simultaneous bilateral TKA procedures were performed using simultaneous tourniquets. The release of the tourniquet before or after closure was equally distributed among all types of TKA procedures (Table 1).
When performing bilateral TKA, 95% of respondents use an intramedullary femoral alignment guide, 78% use an over-reamed entry hole, and only 53% suction the entry hole. With respect to the tibia, 32% use an intramedullary guide, 60% over-ream the entry hole and 60% suction the entry hole; 22% of surgeons stated that they had never considered over-reaming or suctioning the canal, when performing bilateral TKA.
Discussion
Simultaneous bilateral TKA does not appear to be common practice among orthopedic surgeons in Ontario (14%). However, by combining sequential and simultaneous bilateral TKA, 29% of bilateral TKAs are being performed under 1 anesthetic in Ontario. Several factors may be responsible for these lower percentages, including the availability of extra support staff (i.e., additional nurses or surgeons) required to perform simultaneous operations, a lack of additional equipment, hesitation because of concern over a perceived higher potential for complications and lack of experience. Further studies are needed to determine the underlying reasons why most orthopedic surgeons in Ontario elect to perform staged bilateral TKA.
Reviewing the current practices of orthopedic surgeons is important to determine whether the safest possible practices are being used. Overreaming the entry hole before insertion of an intramedullary femoral guide has been shown to decrease the risk of complications due to fat emboli.8 Canal suctioning may further decrease intramedullary pressure; however, scientific evidence for this assumption is lacking. Among Ontario’s orthopedic surgeons, 95% use an intramedullary femoral alignment guide; however, only 78% of these surgeons over-ream the entry hole, and only 53% suction the entry hole; 22% of surgeons had not previously considered over-reaming or suctioning the canal. Thus, many patients may be exposed to a higher risk of fat emboli during their TKA, especially those who are receiving bilateral procedures under 1 anesthetic. We found, however, that a greater number of surgeons performing bilateral TKA under 1 anesthetic are taking the precautionary step to over-ream the femoral canal compared with those performing staged bilateral TKA (p < 0.05).
There are limitations to our study. First, members of the Canadian Orthopaedic Association constitute only about 70% of practising orthopedic surgeons in Canada and the 1999 Canadian Medical Directory may not capture all Ontario surgeons. Furthermore, we have no way of removing those surgeons who are retired, and would be considered non-clinical, from the sample surveyed. It is also likely that many of the non-respondents do not perform bilateral TKA. Thus, our response rate of only 53% likely represents an underestimate. Second, the survey did not determine the reason for the differing practices of bilateral TKA. Third, differentiation between practices in academic and community settings was not determined. There may be systematic reasons for certain practices in each of these settings given the availability of skilled assistants (residents and fellows v. general practitioner assistants) and other resources. Finally, the reason why some orthopedic surgeons do not over-ream or suction the canal was not determined.
The lack of consensus regarding the timing of bilateral knee replacement surgery for patients with severe bilateral knee arthritis in the literature was reflected in our survey responses. The rate of fat embolism after simultaneous bilateral TKA is higher than for a single knee arthroplasty; 6,7 however, most of the cohort studies that have reported an increased risk of complications with simultaneous bilateral total knee replacement compared bilateral knee replacements to unilateral knee replacements. This represents an unfair comparison since any complications associated with the second knee in the unilateral group (operated on at a later date, but not captured in the study) have not been considered.
Conclusions
Prospective research is required to determine whether the combined risk of complications after staged replacement is less than that for simultaneous replacement. At present, however, since there is some evidence that over-reaming minimizes fat embolization, surgeons should consider implementing this simple technique. In addition, manufacturers should be encouraged to routinely provide reaming equipment that over-reams the canal.
Footnotes
Competing interests: None declared.
- Accepted December 15, 2003.