Tube thoracostomy connected to a chest drainage system is a common procedure in children for the management of pleural effusion. However, it is quite unusual for pneumothorax to occur subsequently in the absence of a pulmonary lesion. We report such a case, which led to numerous superfluous interventions before the true cause was recognized.
Case report
A 4-month-old infant underwent resection of a huge mediastinal lymphangioma through a median sternotomy. When oral alimentation was resumed, a right chylothorax developed, for which a chest tube was inserted 21 days postoperatively. The tube was connected to an underwater chest drainage system (Pleurevac A-6020; Genzyme, Fall River, Mass.). A small pneumothorax was apparent on the subsequent chest film, and the system was connected to suction (−10 cm H2O). The pneumothorax persisted, but on postoperative day 26, the chest tube stopped draining and was removed.
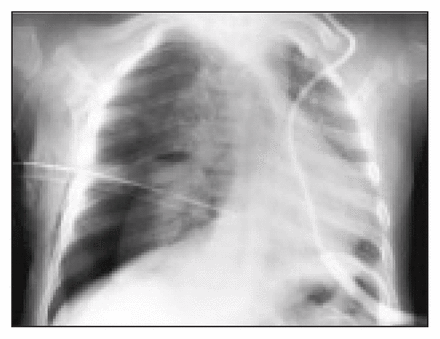
On day 27, the pleural effusion reappeared, without pneumothorax. A central venous catheter and a new chest tube were installed under general anesthesia. From this day on, the pneumothorax was intractable (Fig. 1), necessitating numerous manipulations, changes of tube, increases in suction (up to −30 cm H2O) and placement of a second tube on postoperative day 31, all without success. When the child cried, negative pressure went high in the water seal chamber, even reaching the high negativity float valve. On day 31, the nursing staff noted for the first time that the high negativity relief valve was used to vent excessive negativity. When use of this valve was prohibited, the pneumothorax progressively disappeared and never recurred.
Chest film obtained on postoperative day 29 shows the right pneumothorax.
Discussion
A chest tube functions according to a few basic physical principles related to pressure.1 The lungs have an elastic tendency to recoil away from the chest wall, and a negative intrapleural pressure is required to keep them expanded to normal size.2 Exposure of the pleural space to atmospheric pressure leads to a pneumothorax, which can be prevented if a water seal is used.
Since its introduction in 1991, the Pleur-evac A-6020 has contained a high negativity relief valve, which is intended as a manual vent to reduce residual negative pressure to a desired level within the collection chamber. It allows entry of air into the drainage system between the patient and the water seal chamber. In this case, the valve was used repeatedly by the nursing staff, because high negative pressure developed when the child cried. This led to pneumothoraces and superfluous interventions until the cause was finally recognized. We strongly suspect that similar situations arose previously in our neonatal unit. The negative pressure relief vent adds complexity to the chest drainage system,1 and it is doubtful whether its clinical value outweighs the potential hazard.
- Accepted January 19, 2000.