Abstract
Background: In March 2020, Ontario instituted a lockdown to reduce spread of the SARS-CoV-2 virus. Schools, recreational facilities, and nonessential businesses were closed. Restrictions were eased through 3 distinct stages over a 6-month period (March to September 2020). We aimed to determine the impact of each stage of the COVID-19 public health lockdown on the epidemiology of operative pediatric orthopedic trauma.
Methods: A retrospective cohort study was performed comparing emergency department (ED) visits for orthopedic injuries and operatively treated orthopedic injuries at a level 1 pediatric trauma centre during each lockdown stage of the pandemic with caseloads during the same date ranges in 2019 (prepandemic). Further analyses were based on patients’ demographic characteristics, injury severity, mechanism of injury, and anatomic location of injury.
Results: Compared with the prepandemic period, ED visits decreased by 20% (1356 v. 1698, p < 0.001) and operative cases by 29% (262 v. 371, p < 0.001). There was a significant decrease in the number of operative cases per day in stage 1 of the lockdown (1.3 v. 2.0, p < 0.001) and in stage 2 (1.7 v. 3.0; p < 0.001), but there was no significant difference in stage 3 (2.4 v. 2.2, p = 0.35). A significant reduction in the number of playground injuries was seen in stage 1 (1 v. 62, p < 0.001) and stage 2 (6 v. 35, p < 0.001), and there was an increase in the number of self-propelled transit injuries (31 v. 10, p = 0.002) during stage 1. In stage 3, all patient demographic characteristics and all characteristics of operatively treated injuries resumed their prepandemic distributions.
Conclusion: Provincial lockdown measures designed to limit the spread of SARS-CoV-2 significantly altered the volume and demographic characteristics of pediatric orthopedic injuries that required operative management. The findings from this study will serve to inform health system planning for future emergency lockdowns.
The COVID-19 pandemic has had an unprecedented impact on health care systems. At its height, governments worldwide implemented various public health measures to limit exposure to the virus and to avoid overwhelming hospitals and other health care facilities.
On Mar. 17, 2020, the premier of Ontario declared a state of emergency and instituted a provincial lockdown under the Emergency Management and Civil Protection Act because of the outbreak of COVID-19. Initial restrictions included the closure of schools, child-care centres, indoor recreational facilities, provincial parks, and nonessential businesses. On Mar. 30, 2020, the emergency declaration was extended to include all outdoor recreational amenities, including playgrounds and sports fields. There followed a sequential easing of restrictions through 3 distinct stages over a 6-month period from March to September 2020. For example, playground use was restricted in stages 1 and 2 (Mar. 30 to July 30, 2020) but these amenities reopened in stage 3, starting on July 31, 2020 (Table 1).
Summary of activity-related restrictions during the first 6 months of the COVID-19 pandemic in the Greater Toronto Area
Although the primary objective of these restrictions was to limit virus spread, one could also expect that a lack of access to playgrounds and organized sports would also result in altered patterns of trauma in the pediatric population.1,2 Several reports from the first few weeks of the pandemic noted a decrease (24%–79%) in pediatric presentations to the emergency department (ED) for traumatic injuries.3–9 The reported rates of pediatric orthopedic injuries requiring operative intervention were conflicting, with some studies showing a reduction6–9 and others reporting no change in the rates of operative trauma.3–5,7 Earlier studies were limited by a short time frame, small cohorts, and a lack of association of injury characteristics with specific public health measures. To our knowledge, no longer-term studies have reported the effect of different stages of lockdown measures on the burden of pediatric orthopedic injuries requiring surgical intervention.
Before the COVID-19 pandemic, our centre managed approximately 85% of pediatric orthopedic trauma cases in our region and, more specifically, 40% of all operative pediatric supracondylar humerus fractures in the province.10 During the early phases of the pandemic, all regional acute pediatric surgical care was transferred to our centre. Understanding the effect of different stages of public health lockdown strategies on the demographic characteristics of injured children and the anatomic location and mechanisms of childhood injury is critical for local planning efforts. Furthermore, this information can offer insights for planning health system resources in future pandemics and more broadly for identifying areas of focus to reduce the burden of severe pediatric musculoskeletal injury. Therefore, the purpose of our study was to determine the impact of emergency public health measures implemented to limit the spread of SARS-CoV-2 on the epidemiology of operative pediatric orthopedic trauma and to determine the differential effects of each stage of the lockdown.
Given that the most common causes of orthopedic extremity trauma in children were restricted during the lockdown, we hypothesized that there would be an overall decrease in the burden of cases requiring operative intervention and a change in the demographic characteristics of children with injuries requiring operative management. In addition, we hypotheiszed that the mechanism of injuries requiring surgery would vary by lockdown stage.
Methods
Setting
We performed a retrospective observational cohort study at The Hospital for Sick Children, a level 1 pediatric trauma centre in Toronto, Ontario, in which we compared the epidemiology of pediatric orthopedic trauma cases requiring operative intervention during the 3 stages of the pandemic lockdown, between March and September 2020 (the pandemic group), with that of cases in the same time period 1 year earlier, between March and September 2019 (the prepandemic group). Lockdown stages were defined as per the government of Ontario's emergency declarations (Table 1). The SickKids Research Ethics Board approved the study.
Population
All children with orthopedic injuries who presented to the ED during the study periods were identified using International Statistical Classification of Diseases and Related Health Problems, 10th Revision (ICD-10) codes from electronic medical records. Study cases were selected for further review as follows: we included all patients aged 0–18 years with orthopedic injuries referred from the ED requiring operative management; we excluded cases that did not require operative intervention, slipped capital femoral epiphysis, carpal injuries, and hand injuries (treated by plastic surgeons at our institution).
Design
Chart review was performed to identify patient demographic characteristics, date of injury, geolocation of injury, mechanism of injury, anatomic location of injury, type of injury, severity of injury (single or multiple fractures, open or closed injury, neurovascular injury), and operative intervention. We also recorded whether each case was a primary presentation to our ED or a transfer from another institution.
Cases in the pandemic group were analyzed in terms of ED visits per day and operative cases per day, stratified by lockdown stage, and then compared with cases in the prepandemic group. Age was coded into 3 categories: 5 years and under (preschool age), 6–11 years (elementary school age), and 12 years and over (adolescence). Mechanism of injury was coded into 7 categories: fall within plane (standing height), fall from height, playground, trampoline, self-propelled transit (bike, scooter, skateboard), sports injury, or motor vehicle collision (MVC). Injury locations were categorized as upper extremity or lower extremity. Geo-mapping was used to assess the geolocation of injury in proximity to home and hospital.
Statistical analysis
Data analysis was conducted using IBM SPSS Statistics version 29. Data were first assessed using descriptive statistics and graphic representation. Differences between groups were assessed using independent samples t tests for continuous variables and Poisson analysis for count variables. Percentage change was also assessed between years. Significance for all tests was set at a p value less than 0.05.
Results
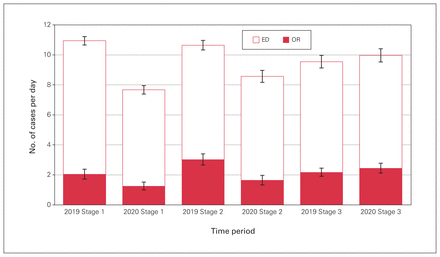
Table 2 provides the breakdown of pediatric orthopedic trauma injuries at our centre by ED visits and operative (OR) cases in both the prepandemic and pandemic periods. A total of 3054 patients were included in the study. There was a 20% absolute reduction in the number of ED presentations for pediatric orthopedic trauma during the 6-month pandemic study period compared with the equivalent prepandemic period (1356 v. 1698 visits, p < 0.001). A total of 633 patients received an operative intervention. There was a 29% absolute reduction in the number of cases requiring an operative intervention in the pandemic period compared with the prepandemic period (262 v. 371 cases, p < 0.001). The overall percentage of ED cases requiring operative intervention was lower in the pandemic period than in the prepandemic period (22% v. 19%, p < 0.001), but this difference did not reach significance when the data were stratified by stage of lockdown. A comparison of pediatric orthopedic ED visits and OR cases by stage both in the prepandemic period and during the first 6 months of the COVID-19 pandemic is presented in Figure 1.
Pediatric orthopedic ED and OR cases before the pandemic (2019) and during the pandemic (2020). Error bars are 95% confidence intervals. ED = emergency department; OR = operating room. Stage 1 = Mar. 30–June 23; stage 2 = June 24–July 30; stage 3 = July 31–Sept. 6.
Emergency department presentation and operative intervention for pediatric orthopedic trauma injuries in the prepandemic and pandemic periods by lockdown stage*
Stage 1 of the pandemic restrictions
There was a significant reduction in ED visits per day during stage 1 of the pandemic versus the equivalent prepandemic period (7.7, 95% confidence interval [CI] 7.4–8.0, v. 10.9, 95% CI 10.7–11.2; p < 0.001) with a corresponding significant reduction in the number of OR cases per day (1.3, 95% CI 1.0–1.5 v. 2.0, 95% CI 1.7–2.4; p < 0.001) (Table 2).
The significant changes in the demographic characteristics of patients with injuries that required operative intervention during stage 1 of the pandemic compared with the prepandemic period included a reduction in the number injuries to girls (42 v. 82, p < 0.001), a reduction in the number of injuries to children aged 6–11 years (40 v. 75, p = 0.001) and aged 12 years and older (11 v. 26, p = 0.017), a reduction in the number of closed injuries (105 v. 171, p < 0.001) and upper limb injuries (81 v. 136, p < 0.001), and a reduction in the number of playground injuries (1 v. 62, p < 0.001) and sports injuries (3 v. 13, p = 0.022). The only significant increase in injuries across all categories was seen for those in which the mechanism was self-propelled transit (31 v. 10, p = 0.002) (Table 3).
Characteristics of patients with operative orthopedic injuries during stage 1 of the pandemic (2020) and the corresponding prepandemic period (2019)
Stage 2 of the pandemic restrictions
There was a significant reduction in ED visits per day during stage 2 of the pandemic versus the equivalent prepandemic period (8.6, 95% CI 8.2–9.0 v. 10.6, 95% CI 10.3–11.0; p = 0.004) with a corresponding significant reduction in the number of OR cases per day (1.7, 95% CI 1.3–2.0 v. 3.0, 95% CI 2.7–3.4; p < 0.001) (Table 2). The significant changes in the demographic characteristics of patients with injuries that required operative intervention during stage 2 of the pandemic compared with the prepandemic period included a reduction in the number of injuries to girls (17 v. 52, p < 0.001), a reduction in the number of injuries in children of preschool and elementary school age (≤ 5 yr: 18 v. 40, p = 0.005; 6–11 yr: 29 v. 59, p = 0.002), a reduction in the number of closed injuries (60 v. 105, p < 0.001) and upper limb injuries (41 v. 88, p < 0.001), a reduction in the number of playground injuries (6 v. 35, p < 0.001), and a reduction in the number of injuries associated with a fall from a height (13 v. 29, p = 0.016). The only significant increase across all categories was an increase in the mean age of children sustaining an injury (from 6.77 [standard deviation (SD) 3.30] yr to 8.26 [SD 4.14] yr, p = 0.014) (Table 4).
Characteristics of patients with operative orthopedic injuries during stage 2 of the pandemic (2020) and the corresponding prepandemic period (2019)
Stage 3 of the pandemic restrictions
When all outdoor recreational areas including playgrounds and indoor recreational facilities were reopened and team sports resumed, the mean number of ED visits per day and the mean number of cases that required operative intervention per day returned to baseline, with no significant difference compared with the prepandemic period (p = 0.62 and p = 0.35, respectively) (Table 2). Furthermore, all patient demographic characteristics and all characteristics of operatively treated injuries returned to prepandemic volumes and patterns, with no significant differences found between the prepandemic and pandemic years (Appendix 1, available at canjsurg.ca/lookup/doi/10.1503/cjs.002723/tab-related-content).
Mechanism of injury by age category
Table 5 depicts only the significant differences found in mechanism of injury stratified by age category between the prepandemic and pandemic periods. Significant reductions in playground injuries and significant increases in self-propelled transit injuries during the pandemic period occurred in the groups of children aged 5 years and under and children aged 6–11 years but not in children aged 12 years and over.
Significant changes in mechanism of injury by age category between the prepandemic (2019) and pandemic (2020) periods
Geolocation
During the pandemic, only 1 patient sustained an injury outside of their residential postal code. During the prepandemic period, 5 patients sustained injuries away from their home, at an average distance of 310 km. There was no difference in the number of patients transferred from outside hospitals in the pandemic period compared with the prepandemic period (p = 0.55).
Discussion
The primary objective of provincially mandated activity restrictions during the COVID-19 pandemic was to limit social mobility and virus spread; however, we found that these lockdown measures were also associated with a significant decrease in the volume of pediatric orthopedic operative trauma cases at our level 1 pediatric trauma centre. Furthermore, the reduction in operative load occurred in proportion to a decreased number of ED presentations for orthopedic trauma overall during the study period. We identified a change in the epidemiology of childhood injuries requiring operative management during the pandemic that appeared to be both predictable and closely related to the changes in the closures of schools, playgrounds, parks, camps, and organized sports activities in each of the 3 stages of lockdown.
Previous studies have shown that schoolyards, playgrounds, and parks are the most common sources of pediatric orthopedic injury in school-aged children.6,11 A systematic review of all playground-related injuries reported that playgrounds are generally safe, and the injuries that occur there are of low frequency and severity.12 However, Canadian injury data in the pediatric population indicate that falls on playgrounds result in the highest number of hospital admissions.13 With playground closures during stages 1 and 2 of the pandemic restrictions, we saw a dramatic decrease in the number of injuries severe enough to require operative intervention (98% and 83%, respectively) in children aged 0–5 years and 6–11 years. The concomitant decrease in closed upper limb injuries fits this narrative, as most distal humerus supracondylar fractures and lateral condylar fractures typically occur at playgrounds.14 Our data support the evidence that playgrounds are a key contributor to the burden of substantial childhood injury given that they typically contribute 30% of our emergency operative load. Although other mechanisms of injury replaced playgrounds as common drivers of operative trauma during the pandemic, the overall operative burden was still reduced by 29%. While studies indicate that playgrounds are safe, assessment has shown that many do not reach specified safety standards and modifications have been shown to reduce injury.12,15
A significant increase in the number and proportion of bicycle, skateboard, and scooter injuries was seen during stage 1 of the pandemic lockdown, particularly in children aged 0–5 and 6–11 years. Given the importance of exercise for healthy development,16 it is likely that children were directed to these sources of play because access to playgrounds and parks was restricted. We posit that the increase in bicycle and scooter injuries is likely to be a function of increased participation, rather than an increase in absolute risk. Given the biggest increase in bicycle injuries was seen in younger children, it is possible that this was related to the learning curve associated with participating in these activities for the first time. Others have also reported an increase in bicycle injuries in children presenting to the ED during the COVID-19 pandemic. In addition to supporting these findings, our study demonstrates that bicycles and scooters are a significant source of more severe injuries requiring operative intervention, particularly in children under 12 years of age.17
The first resurgence of injuries requiring surgery occurred in adolescents when outdoor spaces partially reopened in stage 2, to the extent it raised the mean age of injury significantly above baseline. Interestingly, injuries to girls remained significantly reduced through both stages 1 and 2 before resuming a normal balance of male to female injuries in stage 3. We speculate that the rapid return of the numbers of adolescent injuries to prepandemic levels may be due to inherent characteristics and preferences for higher risk activities of boys versus girls, combined with lower rates of participation of girls in sports.18,19
We found no significant change in the number of trampoline injuries requiring operative intervention at any stage of the pandemic. There are conflicting reports as to the effect of the pandemic on rates of trampoline injuries. Our findings are in keeping with those from other metropolitan centres.8,20 However, an early report from a rural hospital in the United Kingdom showed a large increase in trampoline injuries (both those treated nonoperatively and those treated operatively).7 In addition to study setting, differences in the rates of trampoline injuries may be accounted for by differences in access to and usage of trampolines and differences in lockdown strategies leading to differences in potential mechanisms of injury. One might have expected the number of trampoline injuries to increase during the pandemic, considering that children had reduced social mobility and played more around their homes; however, trampoline injuries are often associated with simultaneous use by multiple users.21,22 It is possible that during lockdown children may have been more likely to use trampolines alone rather than with groups of friends, thus negating the increased risk of injury due to increased participation.
The information gained from our study also serves a broader purpose to inform health system planning for future pandemics. For example, targeted lockdowns may indeed reduce community spread of a virus as intended, but we have shown that there can also be unexpected effects such as changes in the epidemiology of severe orthopedic injuries in children and the associated hospital admission rates.
Limitations
A limitation of our study is that we included data from only a single tertiary level 1 pediatric trauma centre, which may not reflect pediatric trauma patterns across the province. However, our centre is the largest tertiary pediatric hospital in Ontario, and it typically handles approximately 85% of pediatric orthopedic trauma cases in the Greater Toronto Area and, more specifically, 40% of all operative pediatric supracondylar humerus fractures in the province.10 Furthermore, there was no change in referral patterns to our ED between the prepandemic and pandemic periods, and community hospitals were overwhelmed with adult patients in the pandemic period and mandated to redirect pediatric patients to specialist pediatric hospitals. The specific stages of lockdown provided a convenient experimental framework with which to compare the effects of public health measures on the epidemiology of children’s injuries. However, each stage did not exist in isolation, and so children’s activity profiles and volumes of related injuries may have been affected by the characteristics of the preceding stage, further reflecting the complexity of measuring the epidemiologic impact of any single intervention. In addition, weather patterns can affect the patterns of pediatric orthopedic trauma.23 We feel that given the long 6-month time period over which the study was conducted, along with the identical date ranges of the prepandemic and pandemic periods, different weather patterns would be unlikely to add substantial bias. Finally, we did not further subanalyze nonoperatively treated injury patterns, as our focus was on the epidemiology of operative trauma and, as such, surgical indications could have changed during the pandemic, leading to case selection bias. However, any change in surgical indications may have naturally occurred and reflected real-world work patterns at that time and would presumably be similar in future pandemics.
Conclusion
COVID-19 lockdown measures intended to reduce viral spread in the community also had an unexpected effect in that they substantially reduced the burden of pediatric orthopedic extremity injuries that required operative management. Differences in volume, mechanism of injury, and injury type by age group varied by lockdown stage, offering evidence of the burden of operative trauma related to specific childhood activities. The most striking changes were in the reduction of playground injuries and increase in bicycle and scooter injuries in children under the age of 12 years. These findings can be used to inform health systems planning for future pandemics.
Footnotes
Competing interests: None declared.
Contributors: C. Matava and S. Kelley conceived the study. M. Tarchala and S. Grant acquired the data, which C. Bradley, Y. Verma, and M. Camp analyzed. M. Tarchala, C. Bradley, C. Matava, and S. Kelley wrote the article, which S. Grant, Y. Verma, and M. Camp critically revised. All authors agreed to be accountable for all aspects of the work.
- Accepted September 12, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/