Abstract
Objective: To examine the combined and individual predictive values of fine-needle aspiration (FNA), physical examination (PE) of the breast and mammography (the “triple test”) in diagnosing breast cancer in relation to the results of open surgical biopsy.
Design: A study of the records of patients who received both FNA and open surgical biopsy for the same palpable breast lump. The results of diagnostic assessment and open surgical biopsy were categorized as positive or negative. Concordance (percentage of tests found to be correct at biopsy), sensitivity, specificity (percentage of patients without breast cancer for whom the diagnostic test was negative) and positive predictive value (percentage of patients with a positive test found to have breast cancer) were determined for the triple test for each diagnostic modality. In addition, prognostic variables (tumour size, node positivity, estrogen and progesterone receptor status) and outcomes were assessed in patients with a diagnosis of breast cancer.
Setting: A university-affiliated general hospital with a special focus on women’s health.
Patients: Of 290 patients who had both FNA and open surgical biopsy, 191 underwent all three diagnostic procedures.
Main Outcome Measures: The diagnostic accuracy of FNA, PE and mammography to permit preoperative definitive therapy or to allow observation without mandating open surgical biopsy.
Results: In 81 patients all three diagnostic modalities were in agreement for a diagnosis of either benign or malignant disease; the concordance for the triple test was 98.8%, specificity was 100% and sensitivity was 95.5%. Nodal status, tumour size and outcome were similar whether or not the triple test was positive, but, interestingly, when the triple-test results were positive, estrogen (p < 0.05) and progesterone (p < 0.03) receptor values were more likely to be negative.
Conclusions: When all three diagnostic modalities were in agreement for a diagnosis of malignant disease, the combination of FNA, PE and mammography had excellent concordance with the results of open surgical biopsy, and in this situation definitive treatment may be carried out. If all three modalities are in agreement for a diagnosis of benign disease, a period of close observation with repetition of FNA may be safely entertained. Lack of concordance of the three diagnostic modalities mandates biopsy. Triple-test positivity does not predict a worse outcome.
Diagnosis of a mass by fine-needle aspiration (FNA) was introduced by Martin and Ellis at the Memorial Hospital for Cancer in New York more than 60 years ago.1 The method has been widely utilized in parts of Europe but acceptance has been slower in North America, partly because of concern about implanting cancer along the needle tract. Engzell and associates,2 in a rabbit model with popliteal lymph-node metastases, failed to show that FNA had clinical implications for tumour spread. In addition, Berg and Robbins3 found no difference in survival among 370 women with breast cancer initially diagnosed by FNA, compared with an equal number of patients not having FNA.
The diagnostic capability of FNA varies. Review of the literature showed that the accuracy of needle-aspiration cytology ranged from 70% to 90%.4–26 Several factors may affect the results from a given institution, for example, the experience of the pathologist and the surgeon.
The combination of FNA, physical examination (PE) and mammography, which has been termed the triple test,27 has shown a high degree of accuracy in several centres.27–32 The accuracy of diagnosis has assumed greater importance with the growing interest in preoperative treatment modalities such as chemotherapy or radiotherapy. Benefits of preoperative chemotherapy in locally advanced breast cancer have been reported.26,33 Currently, two trials have evaluated preoperative chemotherapy in earlier stage breast cancer.34,35 The National Surgical Adjuvant Breast and Bowel Project B-18 trial, in addressing the question of preoperative chemotherapy, required a definitive diagnosis without open surgical biopsy. In this context, we wished to assess whether the diagnostic efficacy of combined FNA, PE and mammography is sufficiently accurate to permit preoperative therapy. Also, if a diagnosis of breast cancer can be confirmed before definitive surgery, counselling and optimal use of hospital resources can be facilitated. It is true, also, that if a high degree of accuracy can be obtained, a decrease in the number of biopsies for benign disease may be possible.
The Henrietta Banting Breast Centre (HBBC) of Women’s College Hospital in Toronto is an established referral centre for women with breast disease. We studied a group of women referred to the HBBC who had undergone surgical biopsy for palpable breast lumps. We wished to compare outcome for patients having a diagnosis of breast cancer in whom all three diagnostic modalities were concordant with the outcome for patients in whom one or more tests failed to confirm malignancy. Follow-up for the cohort with a diagnosis of breast cancer was complete for 96% of the cases.
Methods
Patients
To obtain the results of FNA, PE and mammography, and the surgical pathological findings, we examined the charts of 290 patients seen between 1985 and 1988 who underwent FNA followed by open surgical biopsy for 300 benign or malignant lesions, all of which presented as a palpable lump. Almost all of the FNAs (293 of 300) and biopsies were performed by three surgeons who have been part of the HBBC since its inception.
Variables assessed
FNA was carried out according to a standardized protocol. A 21-gauge needle attached to a disposable 10-mL syringe was inserted into the palpable lump and three passes were made. The material drawn up into the hub of the needle was expelled into 50% alcohol. A cytospin preparation was made and stained with Papanicolaou stain (modified hematoxylin and eosin). The clinical impression of the examining surgeon as to the nature of the mass (benign or malignant) was recorded as the PE at the time of the FNA. Mammography was done on 201 of these patients not more than 6 months before surgical biopsy; mammographic results were not included if mammography preceded surgery by more than 6 months.
Pathological, clinical and radiologic results were routinely categorized by the criteria utilized at our institution. Aspiration cytologic findings were classified as malignant, equivocal, benign or unsatisfactory. PE was categorized as malignant, probably malignant, probably benign, benign or uncertain. Mammography results were classified as malignant, probably malignant, probably benign or benign. Criteria used to diagnose malignant disease mammographically included demonstration of a spiculated density or typically malignant-appearing microcalcifications (linear, branching, irregular), particularly if these findings were associated with a density or an area of architectural disturbance. If mammography was not carried out at Women’s College Hospital, films from outside institutions were used if available. However, in many of the patients, the only mammograms available were obtained more than 6 months before surgery, and these were not included in the analysis. Histologic appearance of the surgical biopsy specimen was classified as malignant or benign. Aspiration cytology results were reviewed without knowledge of the surgical biopsy results.
To assess the diagnostic potential of the combination of modalities (FNA, PE and mammography), we considered the following findings:
Criteria for a positive diagnosis: FNA — malignant; PE — malignant or probably malignant; mammography — malignant or probably malignant;
Criteria for a negative diagnosis: FNA — benign, unsatisfactory, equivocal; PE — benign, probably benign or uncertain; mammography — benign or probably benign.
A positive result of open biopsy included all patients with a diagnosis of infiltrating adenocarcinoma of breast (ductal or lobular). There were no pure in-situ carcinomas in this series.
One hundred and ninety-one patients underwent all three investigations. Several patients had more than one palpable lump, thus there were more FNAs than PEs. In 81 cases the combination of all three modalities could be categorized as either positive or negative.
The data were cross-tabulated to compare FNA, PE, mammography or the combination of all three with the results of open surgical biopsy. The concordance (percentage of tests found to be correct at biopsy), sensitivity (percentage of patients with breast cancer for whom the diagnostic test was positive), specificity (percentage of patients without breast cancer for whom the diagnostic test was negative) and positive predictive value (percentage of patients with a positive test found to have breast cancer) were determined for each diagnostic modality and for the triple test.
For patients who had biopsyproven primary breast cancer, we used the χ2 test to examine whether there were significant differences for the following prognostic factors: tumour size (< 2, 2–5, > 5), nodal status (positive, negative), estrogen receptor status (< 10, > 10 fmol/mg protein) and progesterone receptor status (< 10, > 10 fmol/mg protein) in the number of patients in whom the triple test was positive versus those for whom one or more diagnostic tests were negative. As well, we examined these two groups of patients for differences in outcome in terms of distant disease-free survival with the Wilcoxon (Peto–Prentice) test statistic.
Findings
FNA alone compared with open surgical biopsy
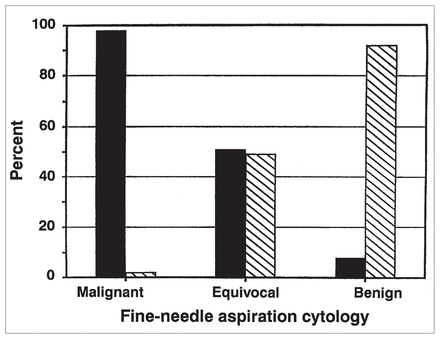
The data for FNA compared with those for surgical biopsy are shown in Table I. For all 300 assessments, the concordance was 83.0%, sensitivity 49.0% and specificity 99.5% for a malignant diagnosis. Fig. 1 shows a positive predictive value of 98% when FNA cytology was compared with the surgical pathological findings, grouping FNA cytology into positive (malignant) and negative (benign, unsatisfactory and equivocal).
Positive predictive value of fine-needle aspiration cytology alone versus surgical pathological findings. Black bars = malignant, hatched bars = benign.
Fine-Needle Aspiration (FNA) Versus Surgical Biopsy
PE alone compared with open surgical biopsy
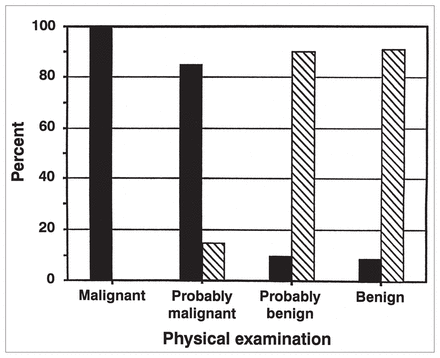
These data are presented in Table II. For all 290 assessments, concordance was 86.2%, sensitivity 67.4% and specificity 95.4%. Fig. 2 shows a positive predictive value of 87.7% when physical examination was compared with the surgical pathological findings, grouping physical examination into positive (malignant or probably malignant) and negative (benign, probably benign and uncertain).
Positive predictive value of physical examination alone versus surgical pathological findings. Black bars = malignant, hatched bars = benign.
Physical Examination (PE) Versus Surgical Biopsy
Mammography alone compared with open surgical biopsy
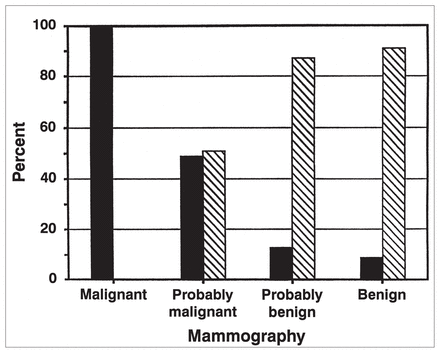
Table III sets forth the results of mammography compared with biopsy. For all 201 assessments, the concordance was 76.1%, sensitivity 85.3% and specificity 70.6%. Fig. 3 shows a positive predictive value of 63.4% when mammography was compared with the surgical pathological findings, grouping mammography into positive (malignant or probably malignant) and negative (benign or probably benign).
Positive predictive value of mammography alone versus surgical pathological findings. Black bars = malignant, hatched bars = benign.
Mammography Versus Surgical Biopsy
Triple test compared with open surgical biopsy
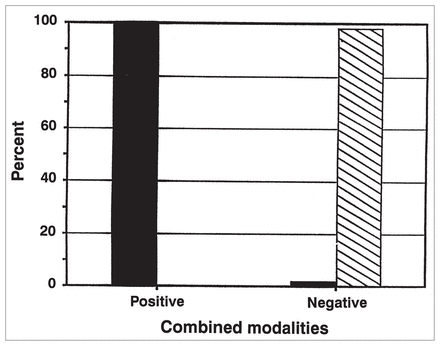
Finally, Table IV contains the data for the combination of modalities FNA, PE and mammography compared with surgical biopsy. Although 191 patients underwent all three diagnostic modalities, only the data for the 81 cases in which all three modalities were in agreement were considered. For these cases concordance was 98.8%, sensitivity 95.5% and specificity 100%. The combination of all three diagnostic modalities gave a positive predictive value of 100% (Fig. 4) when compared with open surgical biopsy. The negative predictive value of the triple test was 98.3%.
Positive predictive value of “triple test” versus surgical pathological findings. Black bars = malignant, hatched bars = benign.
“Triple Test” Versus Surgical Biopsy
Prognostic variables and outcome
For the 92 patients with primary breast cancer, we assessed both prognostic variables and distant disease-free survival, comparing those who were triple-test positive with those having one or more negative diagnostic test results. We found no significant difference in distant disease-free survival, with a median follow-up of 4.8 years. With respect to prognostic variables, the patients with a positive triple test were more likely to be both estrogen receptor (p < 0.05) and progesterone receptor (p < 0.03) negative. However, there was no difference in tumour size or nodal status between those patients with a positive triple-test result and those having one or more negative diagnostic test results.
Discussion
Combination of diagnostic procedures
Our results confirmed that the combination of diagnostic modalities (FNA, PE and mammography) is more accurate than any one modality. When all three modalities were in agreement for a diagnosis of either benign or malignant disease, biopsy confirmed the diagnosis with a specificity and positive predictive value of 100% and a sensitivity of 95.5%. The single case for which the triple test was in agreement for a benign diagnosis but the biopsy positive for malignancy was that of a 44-year-old woman in whom two previous biopsies on the same breast had revealed “fibrocystic changes.” On physical examination, the breast had marked nodularity with a more discrete lump. The mammogram was read as “dense mammary dysplasia with a grossly benign density, probably representing a cyst.” Benign ductal cells were found on FNA. A biopsy performed 2 months later because of persistence of the nodule revealed a T1N0 carcinoma, which was receptor positive. At last follow-up, the patient was well, without evidence of recurrence. This does confirm the need for follow-up of any discrete palpable lump.
The data resulting from the study at the Women’s College Hospital are similar to those of other large series in the literature that compared the triple test of FNA, PE and mammography with surgical biopsy and showed improved diagnostic efficacy using the combination of modalities over a single modality. Kreuzer and Boquoi,28 Hermansen and associates,27 Thomas and colleagues,29 Johnsen,30 Azzarelli and associates31 and Layfield, Glasgow and Cramer,32 all showed that in women with palpable breast lesions, the combination of modalities greatly enhanced the diagnostic accuracy over any single modality. In all these series, there was only the occasional false-positive or false-negative result. Crone and associates11 did not find that combining the three diagnostic modalities improved the diagnostic accuracy over that seen with any individual test; however, they designated any combination test as positive if only one diagnostic modality was considered positive. This would perhaps improve sensitivity but lower specificity.
In these studies, no comparison was made in terms of prognostic variables or outcome between patients in whom the triple test was positive and those in whom one or more diagnostic tests were negative. We found no significant difference in distant disease-free survival in those who were triple-test positive compared to those with one or more negative diagnostic tests, but we realize that the numbers are small and further investigation is needed to confirm this result.
In our series, the high specificity and positive predictive value for the triple test of infiltrating carcinomas as diagnosed at open surgical biopsy, indicated that a false-positive result was very unlikely and that proceeding with preoperative treatment on the basis of the triple-test findings was a safe option.
FNA alone
The value of using FNA alone in the assessment of breast lumps has been reported extensively in the literature. 4–26 Our results show a rather low sensitivity of 49.0% for FNA alone compared with surgical biopsy for all 290 patients. However, the malignant FNA category included only those with a firm diagnosis of malignant disease and excluded those designated as equivocal. We chose to consider as malignant only those cases clearly diagnosed malignant by FNA, because this is most relevant clinically for making decisions regarding preoperative chemotherapy. Also, distinguishing infiltrating from in-situ carcinoma is not always possible on FNA alone, and yet this information is needed when contemplating preoperative chemotherapy. However, pure in-situ carcinomas rarely present as palpable lumps consistent with the findings of our present study. In several other series, 9,10,15,17,18,20,23 a positive FNA result included both malignant and equivocal categories. The inclusion of equivocal with malignant in our FNA results would have improved our sensitivity to 83.7% but would have greatly reduced our specificity. In the present study 67 cases were interpreted as equivocal and 33 as negative for malignancy, whereas 34 were found to be positive, making the category of equivocal ineffective for breast cancer diagnosis if one is contemplating treatment before surgical extirpation. This has been the experience of others.7,10,12,16,17,21,24,28,29,31,33 Also, our results were based on a single FNA study; a second study whenever the cytologic findings were equivocal might have improved our sensitivity. In one other study involving several clinicians,10 sensitivity was also lower than usually reported in the literature. However, there was little variation of FNA results among the surgeons doing the procedure in the present study.
It is usually considered that frozen-section diagnosis has a specificity of approximately 98%, which is comparable to our results with FNA. There was one false-positive result when FNA alone was compared with surgical biopsy. This was the case of a lactating woman, and the pathologist interpreting the slide did not have this information. The findings of PE were thought to represent benign disease.
PE alone
The interpretation of the PE was relatively accurate as confirmed by surgical biopsy (Fig. 2), reflecting the experience and expertise of the three examining surgeons. It has been reported 36 that PE has limitations particularly in younger women and women with small lesions, and the importance of expert assessment was stressed. Our results would support this.
Mammography alone
Overall, mammography had the lowest concordance and positive predictive value of the modalities considered. This may be partially explained by the fact that the mammograms were done at a variety of centres, rather than at only one with recognized expertise. Several of the FNAs preceded the mammography by less than 2 weeks. It has been suggested that mammography should be done before FNA because the resulting edema or hematoma may obscure the diagnosis,37–39 although this suggestion is not universally accepted. When patients less than 50 years of age were considered separately from those older than 50 years, the positive predictive value was considerably greater in the older group of patients (84.8% v. 63.7%), suggesting that the greater density of breast tissue in the younger patients could obscure some malignant lesions.
Conclusions
Our data suggest that single diagnostic modalities were inadequate in a majority of patients. In only 81 (42.4%) of these patients was the combination of the three modalities in agreement for a diagnosis of either benign or malignant disease. In only 21 of the 98 malignancies was the triple-test result positive. However, when all three diagnostic modalities were indicative of malignant disease all lesions proved to be malignant at open surgical biopsy.
Intuitively, one might expect that a patient with all three diagnostic modalities indicating malignancy would have worse tumour characteristics and a poorer prognosis. However, we found that although a positive triple test was associated with greater evidence of estrogen- and progesterone-receptor negativity, it did not appear to confer a worse outcome. However, longer follow-up would be required to reach a definite conclusion concerning this.
We believe that at centres such as ours, where there are surgeons, pathologists and radiologists experienced with breast disease who regularly carry out FNA, definitive preoperative treatment may be undertaken if all three modalities are in agreement for a diagnosis of malignant disease. A lack of concordance certainly mandates biopsy. Similar conclusions were reported by Hindle, Payne and Pan.40 Therefore, surgical biopsy will still frequently be required. If preoperative treatment is not contemplated, a definite diagnosis before surgery is still useful for preoperative planning and counselling.
Donegan41 in a recent review article has recommended surgical biopsy for virtually all palpable masses. However, we believe that if all three modalities are in agreement for a benign diagnosis, a short period of close observation with repetition of FNA may be safely undertaken. This should result in a reduction of the number of breast biopsies carried out for benign lesions, which would have definite health resource implications.
Acknowledgments
This work was supported by the Women’s College Hospital Research Fund, and Dr. Steinberg was supported by a Henrietta Banting Research Fellowship.
- Accepted March 6, 1996.