Abstract
Primary lymphoma of the breast is an uncommon malignant breast tumour, which is seldom distinguished preoperatively from other more common forms of breast cancer. The management differs from the more typical adenocarcinoma of breast in that the emphasis is on systemic chemotherapy. A young white woman presented during the 3rd trimester with bilateral breast enlargement, which failed to involute post partum. Subsequent biopsy revealed primary breast lymphoma of the large cell immunoblastic type. She received systemic chemotherapy and was alive and well with no evidence of recurrence 28 months later.
Primary nonHodgkin’s lymphoma (NHL) is a rare form of malignant breast disease. It constitutes between 0.04% and 0.5% of primary malignant breast tumours in cumulative series.1–8 A recent review1 reported that approximately 350 cases of primary NHL had been described in the literature. The disease tends to follow a bimodal age distribution, with a unilateral, localized type resembling typical breast carcinoma in older women and a bilateral, more diffuse type affecting younger often puerperal women.2,9 In this paper we report on a young woman with bilateral primary breast lymphoma.
Case report
A previously healthy 27-year-old white woman, with no family history of breast disease, presented at 7 months’ gestation with profound engorgement, tenderness and lumpiness of the right breast but no constitutional symptoms. She had a normal vaginal delivery but was unable to breast feed because of breast discomfort. There was no improvement after treatment with bromocriptine.
Examination of the breast revealed a large, firm central mass, 15 cm in diameter, in the right breast, with no fixation or skin changes. There was a 5 cm diameter mass in the left breast at the six o’clock position. Fine-needle aspiration biopsy showed cellular atypia but was not diagnostic. Mammography of the breast demonstrated ill-defined abnormalities, with calcifications suggestive of malignancy.
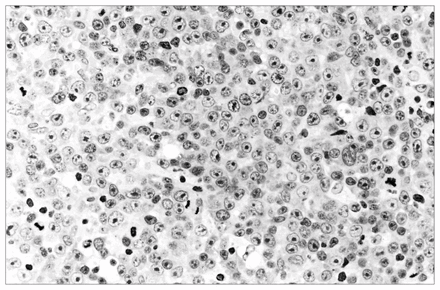
An incisional biopsy of the right breast revealed diffuse infiltration by a large cell malignant neoplasm with a high mitotic rate. Necrosis was common and in some areas there was a “starry sky” pattern. The cells were non-cohesive and had rounded nuclei with prominent, usually single, nucleoli that were centrally located (Fig. 1). The cytoplasm was moderately abundant and basophilic. Immunoperoxidase analysis in formalin-fixed sections showed strong positive staining of the malignant cells for common leukocyte antigen and the B-cell marker L26 (CD20). Staining was negative for keratin, S100 protein and histiocytic markers. The tumour was diagnosed as a large cell immunoblastic lymphoma of B-cell type. Findings on bone marrow and lumbar puncture were normal.
Numerous cells having rounded nuclei with large, single, central nucleoli and moderately abundant, strongly basophilic cytoplasm. These features are most in keeping with B immunoblasts (hematoxylin–eosin, original magnification × 450).
Seven courses of a chemotherapy regimen, consisting of cyclophosphamide, doxorubicin, vincristine and prednisone were given. This resulted in almost complete clinical resolution of disease in both breasts. Biopsy of a residual lump in the scar of the right breast that remained after five courses of chemotherapy revealed coagulative necrosis with a foreign-body reaction. The appearance was consistent with tumour necrosis secondary to a chemotherapy effect. The chemotherapy was followed with bilateral breast radiotherapy (35 Gy in 20 fractions). At follow-up 28 months later the patient was well, with no evidence of recurrent disease.
Discussion
Many reported cases of breast lymphoma may not have been truly primary, because secondary involvement of the breast is often difficult to rule out. Criteria for a diagnosis of primary NHL of the breast require the following: adequate tissue for pathological examination, close association of breast tissue and the lymphoma infiltrate, no evidence of concurrent widespread disease at presentation and no preceding extramammary lymphoma.2,3,10,11
The B-cell type is the commonly seen breast lymphoma, with the T-cell type being very rare.1,7,12 An increased incidence of right-breast versus left-breast involvement has been reported in numerous series.1,5–7,11,13–15
Bilateral primary NHL of the breast has been reported sporadically in the literature.16 The Italian literature in the early part of the century reported cases of primary bilateral breast lymphoma with an aggressive course in young women.16–18 This has been reported more recently, emphasizing two distinct clinicopathological types.2,9 Case reviews revealed a bimodal age distribution with a unilateral type, which resembles the typical adenocarcinoma of the breast in age distribution, and a bilateral, diffuse type that affects younger, often puerperal woman.2,9,19,20
These tumours tend to disseminate widely, and histologically they most often correlate with a small noncleaved cell, or Burkitt-type, lymphoma.
Two series from Africa,21,22 have reported on Burkitt’s lymphoma of the breast associated with pregnancy and lactation. The majority of the cases were characterized by widespread aggressive disease. However, they were not staged according to presently accepted criteria and could not be classified as primary lymphoma of the breast.
The small noncleaved cell that constitutes Burkitt’s and Burkitt’s-type lymphoma is distinct from the cells that constitute diffuse large cell lymphoma, which is the most commonly reported primary lymphoma of breast,1,4,10–13,23,24 and the large cell immunoblastic lymphoma that this patient had. It has been suggested that Burkitt’s lymphoma25 and some other primary NHLs of the breast may be derived from mucosa-associated lymphoid tissue (MALT) and have a different behaviour from nodally derived lymphomas. There appears to be a markedly increased potential for prolonged disease-free survival after even local therapy in distinction to the non-MALT lymphomas. This theory, however, is not universally accepted.20
Lymphocytic mastopathy, or lymphocytic lobulitis, is described as a possible autoimmune breast disease that is characterized by lymphocytic infiltrates and sclerosis.10,20,26 It has been suggested that this condition may be an antecedent of mammary lymphoma. This might explain how MALT lymphomas develop in breast, which normally does not have an appreciable lymphoid component.
Preoperatively NHL of the breast is usually not distinguished from the more common adenocarcinoma of breast.9 Clinical features that might raise suspicion of lymphoma include: a rapidly enlarging mass, absence of nipple discharge and retraction, multiple or bilateral lesions, violaceous skin colour and a softer consistency than expected in axillary nodes when present.11
Frozen or quick sections may not be reliable in distinguishing lymphoma from adenocarcinoma histologically. 1,23 Fine-needle aspiration cytology has been suggested as the best method of preoperative assessment for primary breast lymphoma.9,11,23 Immunohistochemical study of frozen or paraffin-embedded tissue sections, with a panel of antibody reagents may be required to establish a definite diagnosis.
In 1987 Brustein and associates14 reported on 57 cases of primary breast lymphoma and found clinical stage and histologic grade to be the most important prognostic factors for outcome, a finding corroborated by others. 12,23 Although treatment results vary greatly among reported series, avoidance of radical surgery in favour of systemic chemotherapy has generally been recommended.5,7,11,13,22
Conclusions
Because of the rarity and variability of primary lymphoma of the breast, the question of the most appropriate treatment is controversial. Cooperative multicentre studies will be required to accrue appropriate numbers of comparable patients to study and thus to derive appropriate therapeutic principles. Practising surgeons with an interest in diseases of the breast must be aware of the possibility of lymphoma in the differential diagnosis of breast masses so as to avoid unnecessary surgery. A hematologist-oncologist should be consulted to help in determining management that will give the best results.
Acknowledgments
We thank Dr. U. Ambus, Department of Surgery, The Toronto Hospital, General Division, for reviewing the manuscript.
- Accepted March 24, 1995.