Abstract
Objective: To determine if saphenous vein required for coronary bypass could be quickly, easily and safely removed with a minimally invasive technique.
Design: A consecutive series.
Setting: A university centre.
Material and Methods: In cadavers, a standard mediastinoscope was used to remove segments of the greater saphenous vein. Thigh segments, superior leg segments and ankle segments were removed. Fifteen minutes were allowed for removal of a segment.
Results: Segments of vein 15 to 17 cm long could be removed. One segment could not be removed within 15 minutes. Thigh segments were easy to remove, calf segments were the most difficult. There were no avulsed side branches. All incisions were less than 5 cm long.
Conclusions: Saphenous vein can be harvested quickly and safely by a minimally invasive method. Lower extremity complications may be reduced and long-term patency improved with this in-situ technique of vein removal.
Leg complications after coronary bypass surgery are relatively common. Edema is almost uniform and can take months to resolve. In some patients, edema never resolves. Infection at the site of saphenous vein harvest occurs in 2% to 6% of patients,1,2 requiring reopening of the incision and débridement or antibiotic treatment, or both. Anything that can lower complications from saphenous vein harvesting will help decrease morbidity in many patients. Using the minimally invasive techniques developed in other fields of surgery, we have been able to remove portions of the greater saphenous vein in a short time and with minimal trauma to the skin. We believe that the technique can be adapted to most patients and will greatly diminish morbidity after coronary artery bypass.
Methods
We could find no animal equivalent of the greater saphenous vein in the lower extremity of a human, so we used noninfectious cadavers of patients who had given their consent before death for unrestricted autopsy.
Harvesting attempts were made on eight thigh segments and four ankle segments through short (2 to 5 cm) incisions placed over the saphenous veins at the knee and ankle. All instrumentation was through a standard mediastinoscope. We used a pair of endoscopic scissors to dissect the vein and a 10-mm diameter clip applier to clip the side branches and the superior aspect of the vein before removal. Dissection was done as in mediastinoscopy (i.e., at the leading edge of the scope). Dissection time was measured starting from the time of skin incision. Dissection was stopped after 15 minutes because this was considered to represent a reasonable time in which to remove the vein before converting to an “open” technique. Visual inspection of all vein segments was performed to determine the quality of harvested vein.
Results
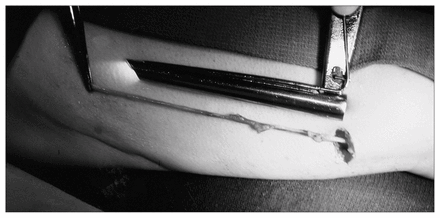
We were successful in removing 11 segments of vein within 15 minutes of skin incision (Fig. 1). We could not remove one segment from the ankle area because of skin and ankle inflexibility. By 15 minutes, two segments, both from the calf area but starting at the knee, were less than 10 cm long. The rest of the segments ranged from 15 to 17 cm long (i.e., the full length of the mediastinoscope). Visual inspection revealed good-quality segments in all vein portions, no injuries to the vein and no side-branch avulsions. The saphenous nerve was easily identified and protected in the ankle segments. Side branches were very easy to see; however, the 10-cm diameter endoscopic clip applicator reduced visibility when placed through the scope. Despite this, no veins were grossly damaged by the clip applier. Removal of calf segments was most tedious, followed by ankle segments. Thigh segments were easy to remove.
Saphenous vein segment harvested with mediastinoscope through small incision.
Comment
Endoscopic surgery has revolutionized many fields of surgery, allowing operations to be performed with less morbidity in most patients, often shortening hospital stay. However, current methods have not allowed most cardiac surgical patients to benefit from smaller incisions and less traumatic methods of surgery. In cardiac surgery, video-assisted techniques have been used mainly in the interruption of patent ductus arteriosus3 and in the management of pericardial effusion.4,5 Others have used minimally invasive methods to view inaccessible intracardiac lesions,6 to divide vascular rings6,7 and to resect portions of myocardium in patients with hypertrophic obstructive cardiomyopathy.8 Whereas endoscopically performed coronary anastomosis remains a formidable task, endoscopic dissection of the internal thoracic artery (ITA) is conceivable, as is the retrosternal dissection of the heart in “redo” operations. However, a simple application, and one that is well within our reach, is the safe removal of saphenous veins. The fact that 15- to 17-cm lengths can be removed within 15 minutes means that the procedure would not add greatly to the overall duration of the surgical procedure. Vein would be available when needed, and full wound closure would entail closure of a 2- to 5-cm incision, instead of one that may range in length from 10 to 100 cm.
The technique we describe was limited by the length of the mediastinoscope, which was approximately 17 cm. With this limitation, the vein could be retrieved from the ankle to approximately half way to the knee, then in an inferior direction from the knee to join the first dissection and finally into the thigh for 15 to 17 cm. In this manner, enough vein for three saphenous bypass grafts could be harvested with minimal skin trauma. If postoperative edema is related to lymphatic damage and skin trauma, then fewer postoperative problems would be expected when less skin and fat are cut. However, this needs to be proven by further study. The use of longer instruments would allow more vein to be taken with only one incision at the knee. We are presently working on the development of a longer “scope” instrument with video capability in order to accomplish this.
When we initially started removing veins, a preliminary tunnel overlying the saphenous vein was made. However, we found that this hindered rather than helped the process. We had to “find” the saphenous vein in the middle of the tunnel. The “dissection as you go” technique seems to work best because the direction of the tunnel is guided by the vein, which can be left in the middle of the field. It is imperative that the vein not be divided before full dissection because the small amount of counter-traction provided by the in-situ vein helps in the dissection. Allowing the vein to be “held” by the body in its natural state may diminish trauma that is caused by pulling and stretching the vein when the open technique is used. Again, this needs to be studied further.
Removal of the thigh segments of veins is easier than segments inferior to the knee. We found that the calf segment inferior to the knee was most difficult to remove, but we were pleasantly surprised at how easily we were able to remove some ankle segments. However, even if a partial open technique is used, this method offers advantages, especially in patients with large thighs. Once in the perivascular space, the distance to the skin becomes irrelevant. Thus, an incision inferior to the knee can be made followed by endoscopic techniques superior to the knee. This method would still decrease the overall trauma to the extremity and thus would be expected to decrease morbidity.
To be considered practical, a technique should be safe, rapid and reliable. If the vein is not dissected in a reasonable time, conversion to an open technique should be considered. We chose 15 minutes as a reasonable time and therefore limited our dissection time. When conversion to an open method is used, it can be a total conversion or a partial one, as described above. Thus, in our series by our standards, we would have converted to an open technique for 3 of 12 veins. Only one segment could not be removed at all. Considering our relative inexperience owing to the newness of the technique and that we were using instruments not intended for this purpose, our results were satisfactory. Conversion rates for laparoscopic cholecystectomy are now less than 10%.9 For video-assisted thoracic surgery, conversion rates of 24% are quoted.10 Since this technique is in its infancy, true conversion rates are unknown. However, persistence without a specific time frame is likely not in the surgeon’s or patient’s best interest.
In summary, we have described the preliminary results of a new technique whereby segments of greater saphenous vein are removed using a standard mediastinoscope and endoscopic instruments in use today. Seventy-five percent of vein segments could be removed in reasonable time. The quality of veins was uniformly good, with no avulsed branches. The development of newer instruments will allow longer segments of vein to be removed. Although this was a cadaver study, the potential benefits to the living are a decrease in morbidity and possibly prolonged patency related to less vein handling during extraction. This last benefit needs to be proven by prospective randomized trials in the living.
Footnotes
↵† Deceased
Presented at the 48th annual meeeting of the Canadian Cardiovascular Society, Toronto, Ont., Oct. 26, 1995
- Accepted March 6, 1996.