Abstract
Objective: To evaluate early discharge from hospital with community-based care as an alternative to hospital-based care for patients who have undergone transurethral resection of the prostate (TURP).
Design: Prospective comparative study.
Setting: A major urban hospital and the urban community.
Patients: Of 198 patients who underwent TURP between Jan. 10, 1994 and Sept. 30, 1994, 81, discharged on postoperative day 1, received the caremap method of health care delivery at home. They were compared with 85 patients who were discharged on postoperative day 2 or 3 and received standard hospital-based care.
Main Outcome Measures: Readmission to hospital, reuse of health care services, complications and patient satisfaction.
Results: Comparison of the 2 groups revealed no significant differences in readmissions to hospital, reutilization of health care services or complications. Following these initial results, the early discharge program was expanded to include all acute care hospitals and the surrounding community.
Conclusions: Postoperative care for TURP can be delivered in the home. A critical success factor was the ability to provide quality care in the community without adverse effects.
The rising costs of hospital-based services require new, collaborative approaches to postoperative care. Planned early surgical discharge programs may offer acute care at lower cost while assuring continuity of care by shifting inpatient hospitalization to community-based home care.1–8
The Royal Alexandra Hospital, a major urban teaching hospital, and Capital Health Authority Home Care (HC) implemented and evaluated a planned early discharge program as an alternative to traditional postoperative hospital care for patients who had undergone transurethral resection of the prostate (TURP). Collaboration with Home Care, a public organization that provides community-based home care by trained nurses, permitted a major change in postoperative care for TURP and a basis for comparing patient care outcomes, satisfaction and overall costs. The planned early surgical discharge program in this study is defined as an alternative service delivery model, replacing hospital treatment with acute care administered by a community-based home care nurse (HCN).
Community-based home care was compared to traditional hospital care in patients who underwent TURP to determine if there was a difference in readmission rate, postoperative complications or patient satisfaction.
Patients and method
A review of all patients who underwent TURP at the Royal Alexandra Hospital, a 932-bed urban teaching hospital in Edmonton, in 1992 and 1993 showed that this group comprised a high volume of surgical patients and a high proportion of long-stay outliers with above-average length of hospital stay and demonstrated low severity of illness. A high proportion of outliers and above-average length of stay suggested variations in care that might lend themselves to more standardized approaches to management. A steering committee of clinical leaders from medicine, nursing, professional support services, education and quality improvement participated in developing a care map.9 The care map developed and implemented in early 1993 by this multidisciplinary team outlined clinical practice guidelines for patients who underwent TURP, taking into account recommended length of stay, medications, treatments, diagnostic tests and discharge planning. Continuing education was provided for all multidisciplinary health care providers.
Consecutive patients in the study were either kept in hospital for standard postoperative care or entered into the planned early discharge program, leaving hospital on postoperative day 1 under the care of a community-based HCN. Selection criteria for early discharge included the following: patient consent, residence in Edmonton, access to medical services in case of an emergency, adequate support by informal caregivers and no other procedures done. Criteria for early discharge included the following: patient or family ability to switch from leg bag to overnight bag, vital signs stable and no excessive bleeding with clots. Patients stayed in hospital if they required care not provided in the community, lived in a long-term care facility, had complications after TURP, had a comorbid condition requiring medical intervention or if their urologist requested in-hospital care. Patients were returned from communitybased home care to hospital if they could not be cared for at home.
Urologists were provided with written information to give to patients, describing the impetus toward communitybased home care and informing them about the study. Patients eligible for the study were identified in the preadmission clinic, where the study was explained to them and a consent to participate in the study was obtained.
Patients received standard hospital care as determined by the care map. For patients who were to receive home care, the preadmission process included an in-depth discussion about postoperative care appropriate to their surgery. Patients in this group received usual surgical care and were discharged with a Foley catheter in place. A follow-up telephone call was made by the HCN that evening, followed by a visit the next day. Suitable arrangements for patient transportation home, postoperative medications and analgesics as appropriate were determined individually.
Each patient had phone access to a specific HCN on a 24-hour basis for continuing care and close liaison in the early postoperative period. The HCN responsible maintained close communication with the patient, visited at least once after discharge from the hospital and maintained appropriate records.
On postoperative day 2, the HCN identified any postoperative problems, removed the Foley catheter when indicated, secured home assistance as necessary with referral to other agencies if appropriate and communicated specific concerns to hospital nurses and urology staff. Education of the patient and family was reinforced.
The HCN contacted hospital nurses and other medical staff as necessary for problem-solving. If a patient had to be reassessed or readmitted to hospital in the planned postdischarge interval, the participating urologist or resident was notified to meet the patient. It was anticipated that home care as outlined would last no longer than 24 to 48 hours after TURP, after which patients would be discharged from the program.
A structured phone interview with patients 2 weeks after discharge provided data on readmission, utilization of health services, complications and patient satisfaction. Readmission was defined as admission to hospital within 2 weeks of TURP for a complication related to the procedure. Utilization data included patient visits to physicians (other than regularly scheduled appointments), clinics or hospitals and contacts with a nurse or pharmacist. Patients were questioned with respect to assistance from relatives or friends, whether they required access to community services, level of satisfaction with care received, whether they had enough information to look after themselves at home and if they understood the information provided.
A steering committee of clinical leaders from urology, medicine, nursing, professional support services, education and community home care participated in revising the original hospital day 3 care map to a day 1 care map followed by home care for days 2 and 3.
Ethics approval was granted by the Investigational Review Committee at the Royal Alexandra Hospital. Data were edited, and a sample of randomly selected cases was used to provide verification. In analysis of the data, a probability value of less than 0.01 was considered significant. Comparisons between groups were made using the χ2 and t-tests.
Results
Of 198 patients who underwent TURP in the interval Jan. 10, 1994 to Sept. 30, 1994, inclusion and discharge criteria were met by 81 patients (41%) for discharge on postoperative day 1 with home care. Of the remaining 117 patients who received standard hospital postoperative care, 32 (16%) remained in hospital for 4 days or longer owing to complications of TURP, comorbid conditions or additional unrelated surgery requiring longer convalence, leaving 85 (43%) patients who were discharged from hospital on day 2 or 3 available for comparison (Fig. 1). Of these 85 patients, 57 did not live in metropolitan Edmonton, 9 did not consent to participate in planned early discharge, 8 did not have a phone, 4 did not speak English, and 7 did not have a physician order for discharge. Both groups were comparable with respect to age, severity of their illness and availability of support within the home.
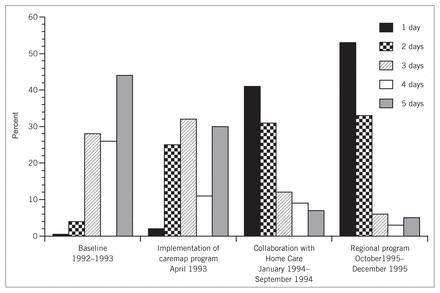
Length of hospital stay for patients who underwent transurethral resection of the prostate during implementation of the caremap program.
At the 2-week post-discharge phone survey, 64 (75%) hospital (H) patients and 63 (78%) early discharge home-care (HC) patients provided follow-up data. In some patients records were incomplete because of an inability to make contact after 3 attempts (H = 4, HC = 6), failure to communicate because of a language barrier (H = 4, HC = 4), no phone (H = 8), an unwillingness to participate in the telephone survey (H = 5, HC = 5) because the patients resided in extended care facilities (H = 0, HC = 3). Nonrespondents did not differ significantly from respondents in regard to demographic and clinical characteristics.
There was no significant difference between groups in reuse of health services (Table I). Readmission in the hospital group was due to pneumonia in 1 patient, hematuria in 2 patients, urinary tract infection in 1 patient and urinary retention in 3 patients. In the early discharge group, readmission was due to pneumonia and urinary retention in 1 patient each. Patients returning to hospital because of urinary retention were catheterized and sent home.
Reuse of Health Care Services for Patients After Transurethral Resection of the Prostate (TURP) Who Received Either Standard Hospital Care or Early Discharge Home Care
Patient survey disclosed that early discharge patients required more assistance with meals and housework (Table II). Both patient groups were satisfied with overall care and the information they were given (Table III). Pain relief was satisfactory and comparable in both groups. In the early discharge group, 81% of patients preferred recuperating at home and 97% were satisfied with overall care and stated that the assistance and reassurance from the HCN was critical.
Assistance Needs by Group of Patients Who Underwent TURP
Survey by Group of Patients Who Underwent TURP
Discussion
Early discharge for selected patient groups appears both safe and cost-effective, 1–8 but comprehensive evaluation of quality, efficiency and cost-effectiveness of care is lacking.
Attention to length of stay has become imperative because it is a major indicator of a hospital’s financial performance. One contemporary trend in acute care is shortening the average inpatient length of stay. This has raised concern that patients may be discharged from hospital before their needs have been addressed adequately. As hospitals attempt to determine the benchmark for length of stay within specific diagnostic groups, it is critical to evaluate quality indicators such as readmission, reuse of health care services, post-discharge complications and patient satisfaction, in order to claim that quality has been maintained or improved. A decrease in length of stay does not demonstrate that quality care has been provided. This aspect can only be assessed through measurement of patient outcome after discharge.10
The limitation of this study is the lack of randomization of groups. Economic pressure to reduce length of stay for acute-care patients and a reduction of surgical beds precluded the feasibility of randomizing patients in that it would prolong post-discharge data collection. Reducing hospital costs might have economic benefits but would have little value if complications were increased. Failure to show significant differences between groups might be explained by the sample chosen in that patients underwent elective surgery for illness of low severity. If this program were to be introduced for more complex surgical interventions, the results might be quite different.
In this collaborative study of care after TURP, in which the major portion of the postoperative period occurred when the patient was at home, clinical outcomes were generally satisfactory. There were no differences in complications compared with standard hospital care, and complications that did arise were readily treatable with physician response and readmission as necessary.
Despite earlier discharge, patients were satisfied with the care received both in hospital and under the auspices of an HCN. They felt adequately informed and did not have unmet analgesic or other needs compared with hospital patients. All 7 urologists continue in the early discharge program, and it has been expanded to include all acute care hospitals in Edmonton. Since the completion of the study protocol, regionalization and restructuring of services have occurred, and patients undergoing TURP are admitted to 1 institution. A follow-up of 203 patients between Oct. 1 and Dec. 31, 1995, demonstrated the sustainability of length of stay (Fig. 1). Demonstrating quality care in the community without adverse occurrences was a critical factor in expanding the program regionally. In our geographic region it is estimated that 50% of patients who undergo TURP can be discharged on postoperative day 1 to community-based care. Of the 166 patients available for the study, 57 (34%) resided outside metropolitan Edmonton, where community-based home care for TURP patients was not available. If these services were available, 84% percent of this population could feasibly be discharged on postoperative day 1.
Close links between community and hospital caregivers are essential. A critical tool was the care map, which gives a standardized approach to care for patients in hospital and out in the community, thus providing a seamless continuum of care. As part of the care map continuum, a home-care protocol was developed to guide assessments and evaluations completed by the HCN on days 2 and 3.
Initial concern was voiced by some urologists who thought care maps might interfere with professional autonomy in patient care. A respected urologist worked with his colleagues to gain acceptance of the standards of care outlined in the care map. Although difficult to quantify, the nurse manager played an instrumental role in working with urologists on a daily basis to encourage early discharge if selection criteria were met and provided daily feedback with respect to patient progress at home. Without this leadership, our results might have been different. Further study is needed to examine the role health care providers have in influencing program goals.
Conclusions
Our study suggests that a discharge program for patients who undergo TURP, combining education with home visits, can provide care comparable to that in hospital. Early discharge is not only safe but is highly acceptable to patients. As outcome studies provide evidence of research, maintaining or improving quality, the concept of “hospitals without walls” will continue to evolve, and services formerly reserved for acute care will shift to the community sector.
Footnotes
Supported in part by the Capital Health Authority Home Care and Royal Alexandra Hospital Foundation
- Accepted October 30, 1996.