Abstract
As transplantation waiting lists lengthen because of the shortage of donor organs, the death rates of patients continue to rise. Xenotransplantation offers the potential to solve the problem of organ shortage br providing an unlimited supply of healthy donor organs. However, there are several barriers to xenotransplantation, including graft rejection, potential xenozoonosis, physiologic incompatibilities and ethical concerns. Experimental xenotransplantation studies continue in several areas, ranging from tissue to whole-organ grafting. Clinical studies continue in the area of tissue xenotransplantation. Trials with extracorporeal xenografts in an acute setting to support fulminant organ failure are likely to begin in the near future. The reintroduction of whole-organ xenotransplantation must be based on sound scientific analysis with broad societal input so as to offer the maximal benefit to transplant recipients and their families.
Xenotransplants are organs or tissues that are transplanted between different species. Whole-organ xenotransplants are classified as either concordant (transplants between closely-related species) or discordant (transplants between distantly-related species).1 The problems, progress and potential application of xenotransplantation are discussed in this paper.
Why do we need xenotransplantation?
Transplantation allows patients with organ failure to resume a normal lifestyle. The long-term results of heart, kidney and liver grafting are steadily improving, with 5-year survival rates approaching 70%. Whereas the demand for transplantation has been steadily increasing, organ donation rates have remained relatively constant. Waiting lists continue to increase; currently, almost 3000 Canadians are awaiting an organ transplant. 2 As waiting lists grow, an increasing number of patients will die without ever receiving a transplant.
Many avenues are being pursued to deal with the shortage of donor organs. Although improving health measures to prevent disease may reduce organ failure rates, this approach will never be completely effective. Donation rates can be improved, but there will never be enough human organs to meet the demand. Even in a country such as Spain, which has the highest donor rates in the world (38 donors per million people each year compared with 14 donors per million in Canada), there are still not enough donors to fulfil all transplant needs. Artificial organs will undoubtedly play a greater role in the treatment of organ failure, but the technologies will take many years to perfect.
Xenotransplantation offers the potential for an unlimited supply of healthy donor organs. As waiting lists lengthen, many patients decompensate while waiting for a transplant. Xenotransplantation could be performed electively and timed so that both the donor and recipient are in optimal condition before transplantation. Moreover, the donor animal could be matched or manipulated, or both, to facilitate long-term acceptance of the graft without the need for maintenance immunosuppression. Before xenotransplantation can be offered to patients, a number of hurdles must be overcome, including immunologic barriers, disease transmission, physiological differences and ethical concerns.
Pigs versus primates
Although concordant transplants (primate-to-human) might seem to be ideal, there are significant drawbacks to their use, including ethical concerns, transmission of infectious disease, and the cost of breeding and maintaining primates.3 Currently, pigs are the most promising source of donor organs. Pigs have large litters with a short maturation period, they are easy to breed, and their organ size and physiology are remarkably similar to that of humans. A disadvantage of performing pig-to-human (discordant) transplants is the occurrence of hyperacute rejection, which leads to organ loss within minutes to hours after grafting.
The immunologic reaction
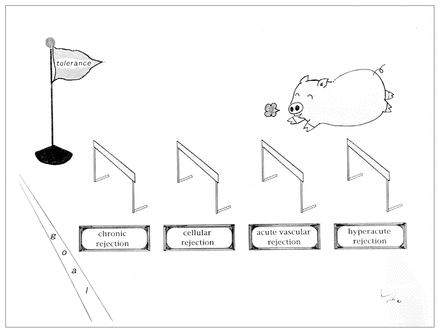
The immunologic reaction of the recipient to a xenograft is mediated initially by xenoreactive antibodies, complement and natural killer cells and later primarily by cellular immune responses. These mechanisms result in hyperacute, acute vascular, cellular and chronic graft rejection (Fig. 1).4–6
The immunologic hurdles of xenotransplantation.
Hyperacute rejection is a major barrier to discordant xenotransplantation. Humans have natural IgM antibodies (xenoreactive antibodies) to 1,3-galactose, a carbohydrate that is expressed on all nucleated pig cells. After binding of these preformed antibodies, serum complement is activated, resulting in massive thrombosis to vascular endothelium with vessel occlusion and graft failure within minutes to hours of the transplantation.7 Xenoreactive antibodies can be removed by adsorption columns, but this is only a temporary solution. A more promising approach is to create transgenic pigs expressing selected human genes that modify the immune response. Recently, pigs have been raised that express human complement regulatory genes, thereby preventing activation of complement and ameliorating hyperacute rejection.7–9
The next major hurdle is to prevent acute vascular rejection which leads to graft destruction over a period of days to weeks. Xenoreactive antibodies, macrophages, natural killer cells and complement appear to play important roles in this process.1 Later (in days to weeks), xenografts may also be damaged by cellular and chronic graft rejection. It is not known whether any of these processes can be reliably prevented by currently available immunosuppressive drugs.10
Our centre has evaluated different combinations of antirejection drugs for xenotransplantation in a baboon-to-monkey model and the results have been promising. The combination of cyclosporine, cyclophosphamide and rapamycin provided long-term survival in concordant kidney xenografts. One monkey with a baboon liver lived for 3 years, despite withdrawal of all immunosuppression 1 year after transplantation. 11
Ultimately, the goal of transplantation is to attain a state of tolerance whereby the recipient’s immune system accepts the graft as “self” without the need for maintenance immunosuppression. 12 The opportunity to genetically manipulate pig donors provides new ways to induce tolerance to xenografts in humans. Donor bone-marrow transplantation, radiation and the production of monoclonal antibodies directed against specific lymphocyte receptors are currently being studied as methods to induce tolerance.12–16
Xenozoonosis
Xenozoonosis, the introduction of xenograft-derived diseases into humans is a potential risk of xenotransplantation. 17–19 Pig herds, free of known bacterial and viral pathogens, can be developed; however, the risks of introducing unknown pathogens with a xenograft are difficult to evaluate. There is a theoretical risk that pig genome retroviruses could become functional through recombination events. Some of these retroviruses are capable of infecting human cells, although the clinical consequence, if any, of this infection is unknown.19,20
It seems likely that the risk of unusual infections will be low since humans and pigs have lived in close proximity for many years. Moreover, many immunocompromised patients have been treated with full-thickness pig skin grafts with no evidence of adverse effects. Nonetheless, xenotransplant recipients, their families and their health care providers will have to be monitored closely for infectious complications.
Physiologic incompatibilities
There may be physiologic incompatibilities with some xenografts. For example, patients with porcine kidney grafts may require supplemental erythropoietin to maintain normal hemoglobin levels. It is unlikely that pig livers will be able to provide all of the functions of the more than 2600 proteins and enzyme systems that are produced in human livers. Finally, the lifespan of pigs is less than 15 years; whether their organs will work for a human lifetime is unknown. There is limited information about the function of xenografts in humans. Previous attempts at clinical xenotransplantation, however, have shown that adequate function may occur early after transplantation.
Clinical xenotransplantation
The current clinical experience with xenotransplantation is limited to 3 main areas: tissue xenotransplantation, extracorporeal perfusion of a xenograft for the treatment of fulminant liver failure and whole-organ xenotransplantation.
Tissue xenografting
Tissue xenotransplantation with pig-to-human skin grafts and pig heart valve implants has been used successfully for many years. Xenotransplantation using pig neural cells has shown promise as a treatment for Parkinson’s disease.21 Pancreatic islet xenotransplantation offers the potential to cure insulin-dependent diabetes. Transplanted islets are not initially vascularized: they become vascularized by recipient vessels over time, thereby bypassing the hyperacute rejection seen in whole-organ xenotransplantation. Pigs are a good source of donor islet tissue because porcine and human insulin are structurally similar, pigs and humans have similar glucose metabolism, and porcine insulin has been used for many years to treat diabetes.
Xenoislet transplantation has been combined with allograft kidney transplantation in patients with diabetes and end-stage diabetic nephropathy.22 Islet cell function was demonstrated by porcine C peptide found in the urine in some patients; however, insulin requirements were not affected by the xenotransplant. This work shows that it is possible to attain viable islet cells after xenotransplantation, but further modifications are required to achieve clinical function that allows tapering or withdrawal of insulin.
Extracorporeal perfusion with xenografts
Extracorporeal xenogeneic liver support has been used in patients with fulminant liver failure as a temporary measure to allow time for the liver to recover function or for an allograft to become available. A perfusion circuit is established that carries blood from the patient through the hepatic artery and portal vein of the ex-vivo organ and then returns the detoxified blood to the patient. Two of 5 patients described in the recent literature were successfully managed by this technique until allotransplantation could be performed.23–26
Whole-organ xenografting
There have been sporadic attempts at clinical whole-organ kidney, heart and liver xenotransplantation. In the early 1960s, Reemtsma and colleagues27 transplanted chimpanzee kidneys into human recipients before dialysis was widely available. Some of these grafts had adequate function early, but eventually all of the recipients succumbed to uncontrollable rejection or infection. In 1985, Bailey and associates28 transplanted a baboon heart into a newborn infant who survived for 3 weeks until the graft was lost to antibody-mediated damage. In 1993, Starzl and colleagues29 reported 2 cases of baboon-to-human liver xenotransplantation in patients with end-stage liver disease secondary to chronic active hepatitis B (1 patient was also HIV positive). Evidence of liver function included normal coagulation profile, correction of hyperammonemia and clearance of serum lactate; however, both patients had low serum albumin requiring repeated transfusions. The first patient lived for 70 days, but the second patient died 26 days postoperatively. Neither graft had evidence of rejection, and both of these patients died from sepsis secondary to profound immunosuppression. The use of a liver xenograft as a bridge to allotransplantation has been investigated.30–32 Recently, a woman with fulminant hepatic failure received a heterotopic, auxiliary, pig liver xenograft as a temporary “bridge” in an attempt to stabilize her condition until an allograft became available.30 The liver showed signs of function but her neurologic status did not improve and she died 34 hours after xenografting.
Ethics of xenotransplantation
Xenotransplantation raises many important issues related to the application and regulation of new biotechnologies. In Canada, a federal working party, comprising regulatory of fi cials, clinical and laboratory scientists, ethicists, veterinarians and lay people, has been established to determine how, when and if xenotransplantation should proceed. The risk of xenozoonosis poses challenges for obtaining informed consent because there are not only possible hazards for the patient but also for the family and other close contacts. Other ethical issues related to xenografting include animal rights, organ allocation, financing, and the potential psychological responses to receiving and living with tissues from a non-human source.18
We believe that prolonged survival should be achieved in a transgenic pig-to-nonhuman primate model before proceeding with clinical whole-organ xenotransplantation. The most likely candidates for the early trials are those patients who are currently excluded from allotransplantation either because they are considered to be at excessive risk or because of a lack of available donors. Potential recipients include the following: highly sensitized patients with renal failure who must wait for years (or indefinitely) until a suitably matched human kidney becomes available; neonates with heart failure who currently face a severe shortage of donors and patients with liver failure secondary to advanced hepatocellular carcinoma; and some patients with viral hepatitis infection. There is some evidence to suggest that xenografts may be preferable to allografts in patients with viral infections that exclusively affect humans.33
There will be several economic issues related to the introduction of xenotransplantation into clinical practice. Human organs are generous gifts from donor families, although there are significant costs associated with the organ procurement process. The expenses of xenotransplantation include developing, breeding and maintaining donor animals as well as the costs associated with lifetime surveillance for infectious diseases. If an unlimited supply of donor organs becomes available, many patients who are currently denied transplantation because of risk factors will become candidates for xenotransplantation. This will lead, in turn, to more questions regarding the use of health care resources, minimal listing requirements and the outcomes needed to justify sacrificing donor animals.
Future directions
Xenotransplantation offers the potential to save lives and alleviate human suffering. This new technology requires thorough scrutiny at every step, with sound scientific analysis and broad societal input, to ensure that its clinical application proceeds in a timely and safe fashion.
Acknowledgments
Some of data reported here were supplied by the Canadian Organ Replacement Register, a registry of the Canadian Institute for Health Information. The analysis and interpretation of these data are the responsibility of the author and do not necessarily reflect official policy or interpretation of the Register.
- Accepted April 9, 1998.