Abstract
Caustic injury to the esophagus, with resultant esophageal stricture, is a challenge for the surgeon. These strictures require multiple esophageal dilatations, which are usually performed under general anesthesia and frequently under fluoroscopic control. Because of the risks of multiple general anesthetics and frequent radiation, a technique is described for retrograde esophageal balloon dilatation in an outpatient clinic setting without a general anesthetic or fluoroscopic control.
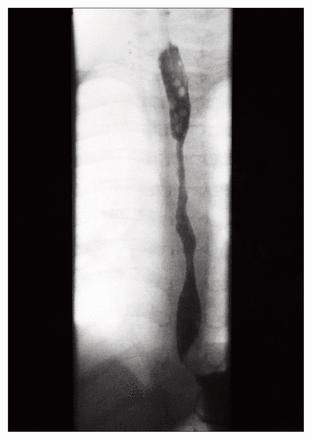
Caustic injury to the esophagus is a common cause of esophageal strictures in children, 1,2 and the treatment of such strictures can be challenging. Repeated esophageal dilatations are employed with varying degrees of success. 2–4 A 20-month-old boy presented to our hospital after ingesting lye. Endoscopy revealed a circumferential burn. A gastrostomy was performed and a transesophageal silk string was placed. After a prolonged hospital course, a diffuse esophageal stricture developed (Fig. 1). He had multiple antegrade esophageal dilatations under general anesthesia with fluoroscopic control using guide-wire directed dilators (the American Dilatation System; Bard Interventional Products, Billerica, Mass.). As a result of the initial response to the antegrade dilatations, the transesophageal silk was removed, but the gastrostomy tube was left in place, and subsequent dilatations were performed by the same method. The dilatations were carried out over 8 months, and averaged 1 per month. However, because of worsening dysphagia, the interval between dilatations decreased. There was increasing difficulty in obtaining venous access, so a subcutaneous infusion port was placed. Because we were concerned about repeated radiation exposure and the need for repeated multiple dilatations, a transesophageal silk was reinserted and retrograde balloon dilatations were performed.
Esophagogram shows a diffuse esophageal stricture.
Technique
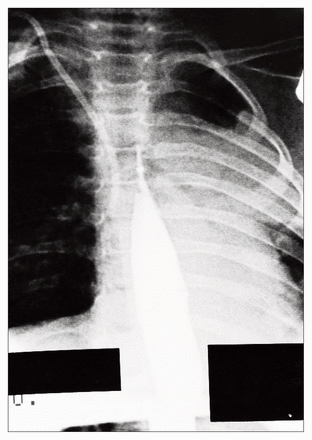
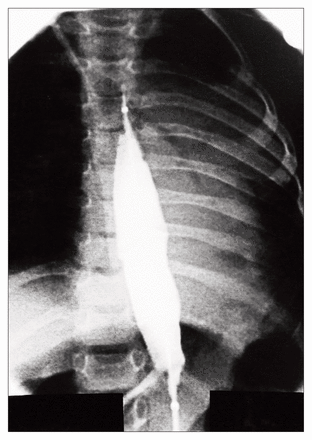
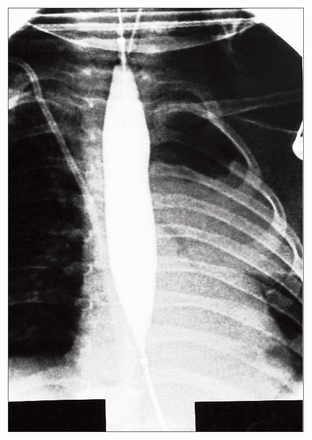
The first retrograde balloon dilatation is performed under general anesthesia with fluoroscopic control. Either preoperative or operative water-soluble contrast esophagography is performed to determine the exact location of the stricture. The size of the balloon is determined according to the esophagographic and fluoroscopic findings. The volume of inflation is determined under fluoroscopic guidance by inflating the balloon with contrast material and observing adequate dilatation of the stricture. Appropriate balloon location is determined (Figs. 2 to 4) by marking the points of the proximal and distal ends of the stricture on the catheter. In cases of multiple or long strictures, such as in this case, after the most distal dilatation is performed, the balloon is deflated and repositioned more proximally according to previous measurements. Subsequent dilatations are performed in the outpatient clinic without anesthesia or fluoroscopic control.
The balloon is positioned in the distal esophagus.
The balloon is positioned in the distal to middle esophagus.
The balloon is positioned in the middle to upper esophagus.
The technique for subsequent dilatations is simple. It requires a heavy silk that serves as a stent, coming out of the nares and the gastrostomy site. The ends are tied, forming a loop. The parents are instructed to stop feeds 6 hours before the clinic visit. The gastrostomy tube is removed, a suction catheter is introduced through the gastrostomy, and gastric contents are aspirated. A soft guide wire (Teflon coated straight catheter exchange; Cook Inc., Bloomington, Ind.) is looped around the heavy silk (Fig. 5), both ends of the guide wire are introduced into the centre lumen of the balloon dilator (Angiocath; Mansfield Scientific, Inc., Mansfield, Mass.) (Fig. 6), and the wire is advanced and retrieved at the other end of the catheter. Traction is applied on the wire until it is snug around the silk (Fig. 7). The catheter with the balloon deflated is advanced into the stomach. Traction is applied to the silk to pull (rather than push) the balloon into position according to the initial measured distance. Dilatation is then performed. At the end of the procedure the catheter is removed and the gastrostomy tube replaced. The catheter is then cleaned in Metricide (Metrex Research Corp., Morrisburg, Ont.) and reused. An outdated (no longer suitable for vascular use) vascular balloon dilator is used to minimize the cost of this repeated procedure. In this case, since the patient lived within 5 minutes of our hospital, observation was limited to 20 to 30 minutes. The parents are instructed to return immediately if there is any problem.
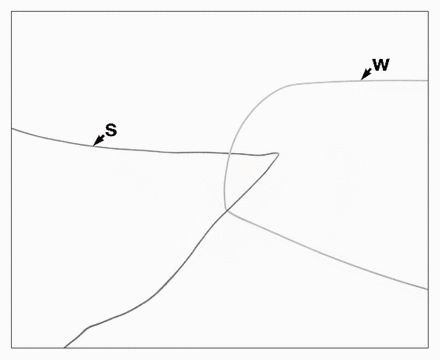
The guide wire (W) is looped around the heavy silk (S).
Both ends of the guide wire (W) are introduced into the central lumen of the catheter and retrieved at the other end.
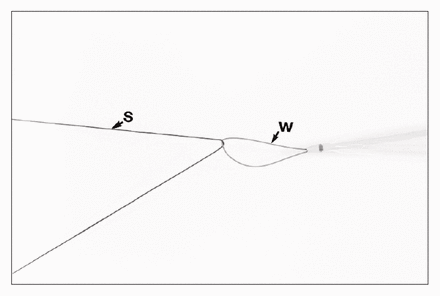
Traction is applied on the wire (heavy arrow) until the silk (S) is snug at the tip of the catheter. Traction on the silk (arrow) advances the catheter into the desired position.
Comment
Balloon dilatation of the esophagus has been described in a variety of conditions. 5,6 It can be performed in an antegrade or retrograde fashion.7,8 Our technique of retrograde dilatation is safe and effective, it reduces health care costs, does not dilate the gastrostomy site, and repeated general anesthetics and excessive radiation are avoided.
- Accepted June 3, 1998.