Tripod fracture
Fig. 1 (see question on page 279) is a cross-table lateral view of the facial bones taken with the patient in a supine position. It demonstrates a fluid level in the maxillary antrum (arrows). The Water’s view (Fig. 2, page 279) also shows soft-tissue (hemorrhage) within the antrum, but in addition a fracture of the right inferior orbital rim (arrow) is seen just lateral to the infraorbital foramen. The zygomatic arch is not well seen on the right, in part because the view is slightly oblique but also because there is a depressed fracture of the zygomatic arch, best seen on the submentovertical view (Fig. 3, page 279 [arrow]).
Caldwell’s view (Fig. 4, page 279) illustrates the other component of the tripod fracture: separation of the zygomaticofrontal suture (arrow).
The tripod fracture, also known as the zygomaticomaxillary or the zygomatic complex fracture, is the most common facial fracture, accounting for 40% of midface fractures. It is usually the result of a punch to the malar eminence.1 The blow is centred on the body of the zygoma, but the lines of fracture usually involve the articulations of the bone: the orbital process to the frontal bone, the zygomatic arch and the maxillary process surrounding the superior and lateral margins of the maxillary antrum.2 The fractures often pass through and separate sutural lines: zygomaticofrontal, zygomaticotemporal and zygomaticomaxillary.
Clinical assessment may be difficult in the presence of severe swelling. In addition, the patient may have associated injuries (e.g., to the skull or cervical spine) that take precedence over potential facial fractures. Signs of facial trauma may be present on views of the skull, and careful attention should be paid to direct and indirect signs of injury. Dedicated facial radiography may be performed when the patient is clinically stable.2
Indirect radiographic signs include maxillary antral opacification, malar soft-tissue swelling and change in orbit size or shape. Although other conditions (e.g., sinusitis or polyps) may cause antral opacification, in the setting of facial trauma this sign should prompt a careful search for an underlying fracture. Acute hemorrhage, as in this case, will level out according to the position of the patient’s head. A lucent fracture line is the most obvious direct sign, but others include suture separation, an absent infraorbital foramen (due to disruption), duplication of an oblique orbital line or an abnormal linear density.2 The latter occurs when a fragment of bone turns on its edge, projecting a density not visible on the opposite side. Comparison with the normal side serves as a valuable internal reference.
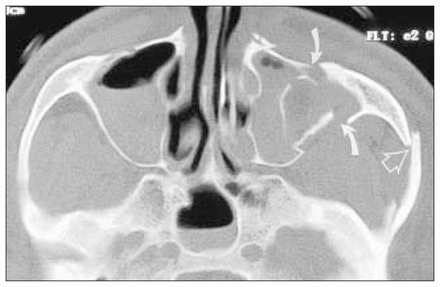
The force of the blow will determine the degree of depression and comminution and the presence of other fractures. Associated soft-tissue injuries include entrapment of orbital contents (blow-out-type injury), trauma to the globe or lens and damage to the infraorbital nerve. The patient should be clinically assessed for these. Additional radiographic views may be required to fully evaluate the injury, including an orthopantomogram to evaluate the mandible and alveolar ridges.2 Computed tomography gives a comprehensive view of the injury (coronal and axial sections), and 3-dimensional reconstruction can be helpful in preoperative planning.3,4 Fig. 5 is an axial (transverse) computed tomography image in another patient with a left-sided tripod fracture. There is clear visualization of a displaced fracture of the zygomatic arch (open arrow). In addition, fractures of the anterior and posterior walls of the maxillary sinus are clearly evident (closed arrows). There is extensive fluid (blood) within both maxillary sinuses.
Treatment consists of reduction and fixation to restore normal anatomical outline and to prevent complications, such as impingement on the coronoid process, diplopia and enophthalmos.