Procedures involving the trachea and its adjacent structures can cause tracheal damage such as ulceration of the mucosa, tracheal stenosis, tracheoesophageal fistula, tracheomalacia and neck abscess.1–5 We describe a case of upper tracheal necrosis as a complication of total thyroidectomy in a hyperthyroid patient, highlighting some of the difficulties presented by a thyrotoxic goitre, which, to our knowledge has not been reported before.
Case report
A 30-year-old woman had symptoms of hyperthyroidism dating back 5 years, when she presented for surgical treatment of her thyrotoxicosis. She was treated with propylthiouracil and metoprolol but was not compliant because of side effects of the medication.
When we saw her, she was tachycardic (105 beats/min). Her thyroid gland was diffusely enlarged 4 to 5 times its normal size with audible bruits over the gland and a free thyroxine level of 77.1 pmol/L (normal 9–24 pmol/L). The patient refused treatment with radioactive iodine.
She underwent a total thyroidectomy, preserving the recurrent laryngeal nerves and both inferior parathyroid glands. The thyroid was very vascular, and there was marked, diffuse bleeding, which was difficult to control.
Postoperatively, she was febrile and had a persistent cough. Both conditions were attributed to atelectasis. Her leukocyte count remained normal, and there was no evidence of wound infection or abnormal swelling of the operative site at the time of discharge.
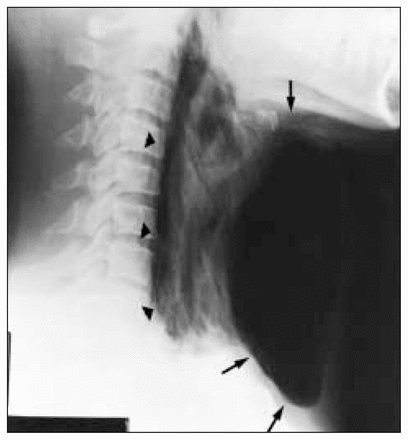
On the eighth postoperative day, she presented with a swollen neck, a productive cough and a temperature of 37.8°C. The neck swelling resolved after needle aspiration of air but recurred when she coughed. A plain roentgenogram confirmed a large collection of air (Fig. 1).
Lateral radiograph of the neck showing a large air collection (arrowheads)and surgical emphysema (arrows).
At surgery, the right side of the trachea involving the second to the fourth tracheal rings was necrotic, exposing the endotracheal tube cuff. The endotracheal tube had intentionally been left long and the cuff was advanced beyond the damaged area. The necrotic trachea was excised, leaving a large eccentric right-sided defect that spanned 3 rings. Complete circumferential tracheal excision with primary repair was not feasible because the tension needed for anastomosis would require superior and inferior tracheal mobilization, involving subhyoid or suprahyoid release, likely causing the infection to spread and preventing healing of the trachea. Instead, the trachea was partially closed around a no. 11 Montgomery T-tube with the adjacent strap muscles closed in layers around the T-tube and the residual defect.
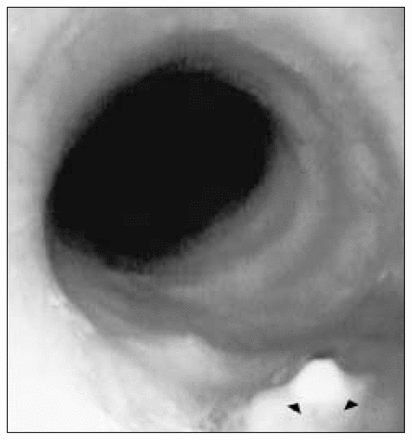
Beta-hemolytic Streptococcus was detected in cultures taken from the damaged area. Her voice was normal postoperatively, and direct fiberoptic laryngoscopy showed normal movement of the vocal cords. She remained in the hospital for only 3 days on intravenously administered antibiotics. There was no evidence of ongoing infection. She was discharged with the Montgomery T-tube in place for 3 months. One month after removal of the T-tube, endoscopic examination showed complete closure of the trachea with no sign of tracheal stenosis (Fig. 2) and no malacia. At 1 year she was well with no tracheal symptoms.
Bronchoscopy 4 months after operation on the trachea shows a small area of granulation (arrowheads) in a normalsized trachea.
Discussion
Several factors, including prolonged intubation,6 elevated cuff pressure,1 disruption of blood supply to the trachea2 and localized and systemic infections,4 have been implicated in tracheal damage after intubation and neck surgery. A number of papers have discussed the consequences of intubation and cuff pressure in ventilated patients.1,2,6 The hypothesis is that elevated cuff pressure exceeds the perfusion pressure of the tracheal mucosa resulting in pressure necrosis. Autopsy studies have shown that the pattern of progressive damage starts with superficial tracheitis followed by mucosal ulceration and finally dissolution of the cartilaginous rings with destruction of the tracheal architecture.1 Microscopic examination of the affected trachea shows infected granulation tissue.2 The typical erosion of the tracheal wall after prolonged intubation consists of a circumferential collar classically located in the area of the cuff extending over a length of 1 to 3.5 cm. Occasionally, a pressure ulcer may occur due to trauma from the tip of the tube.2
Several reports have also suggested that long-term tracheal compression by a large goitre may cause local tracheal wall weakening and subsequent tracheomalecia. 2,3 The resulting thinned tracheal tissue may be more susceptible to vascular damage and necrosis.
Alternatively, tracheal necrosis may be the result of disruption of the tracheal segmental blood supply. Autopsy studies demonstrate that the blood supply to the upper segment of the trachea comes mainly from small branches of the inferior thyroid artery that have lateral points of entry. These fragile vessels are easily disturbed, causing ischemia and subsequent necrosis.2
Systemic and upper respiratory infections have also been associated with an increased risk of tracheal necrosis. The damaged tracheal wall is more susceptible to bacterial infection from contaminated secretions or hematologic seeding.1,5
Our patient had a number of predisposing risk factors. First, the 4-hour thyroidectomy exposed the patient to prolonged intubation. Pressure from the cuff or perhaps trauma from the tip of the endotracheal tube may have caused injury to the trachea, which may already have been compromised by pressure from the long-standing goitre. Second, the thyroid and the trachea share a common blood supply (i.e., the inferior thyroid artery), and ligation of this artery may segmentally decrease tracheal blood flow. Third, there was marked bleeding during the procedure because of increased glandular vascularity, and we suspect that excessive cauterization was employed for hemostasis on the lateral aspect of the trachea and compromised its blood supply. Finally, the damage to the tracheal wall and possible development of a hematoma may create an environment for bacteria to seed, resulting in infection and necrosis.
In retrospect, a number of steps could have been taken to prevent this complication. Lugol’s solution taken for 10 days before surgery decreases the vascularity of the thyroid gland and could theoretically decrease intraoperative bleeding. Care must be taken when using electrocautery on the lateral aspect of the trachea. When dissecting around the trachea, the lateral pedicles should be carefully preserved to maintain the blood supply to the upper segments2 and thyroid branches should be ligated close to the capsule. Furthermore, extended operating time always increases the risk of complications.
- Accepted May 6, 2002.