A 59-year-old woman presented with a history of injury to her left second toe. Some months earlier she had “stubbed” it against a chair leg and had experienced immediate pain and swelling of the toe. The pain and swelling had gradually resolved but she was left with a permanent deformity of the toe and now had a dorsal corn over the proximal interphalangeal joint of that toe.
Clinical examination confirmed a claw-toe deformity of the left second toe; physical examination also revealed some shortening of the first toe and a dorsal medial scar. The patient stated that some 20 years before she had undergone a surgical procedure on her left great toe for arthritis. That toe, while stiff, was not painful, but she had been aware of increasing swelling in the vicinity of her great toe and stated that her toe was now “fat” as compared to 1 or 2 years previously.
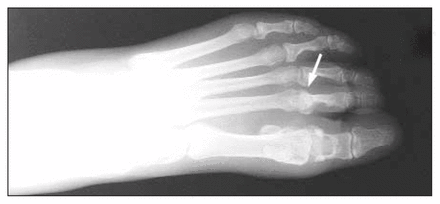
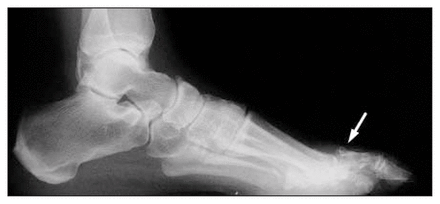
She underwent radiography of her foot. On the anteroposterior film a dislocation of the metatarsophalangeal (MTP) joint of the second toe was demonstrated (Fig. 1, arrow), the problem that brought the patient to the clinic. The left great toe revealed a cystic lesion in the base of the proximal phalanx with some bone destruction; in addition there was considerable soft-tissue thickening around the MTP joint. The lateral film demonstrated the dorsal dislocation of the base of the proximal phalanx of the second toe (Fig. 2, arrow).
The patient’s history revealed that she had undergone silicone replacement arthroplasty at the base of the proximal phalanx of the great toe for treatment of hallux rigidus. This operation, once common, has been abandoned because of problems associated with wear of the silicone implant.
Silicone synovitis is a recognized complication of the use of solid silicone devices that articulate with bone or articular cartilage. These unipolar silicone implants have been used extensively in the foot (MTP joint of the great toe), the elbow (radial head) and the carpus (lunate). Unfortunately, in a significant number of patients clinical symptoms — primarily pain and swelling — appeared years after implantation and were usually accompanied by radiographic changes in the bone against which the silicone was articulating, as well as in the surrounding soft tissues. Typical radiographic findings included cystic change in the bone, often remote from the area with which the silicone was in contact, and soft-tissue swelling. Clinical symptoms of pain and swelling appear to be secondary to synovial inflammation.
Histologic examination of tissue retrieved from around removed implants demonstrate a giant cell response to the particulate silicone debris; this giant cell response causes the characteristic bone loss that accompanies this condition. This patient’s radiographs demonstrate cavitation of the proximal phalanx with periarticular bone destruction as well as cystic change in the metatarsal head.
Although hinged silicone prostheses are still used to good effect (particularly in the metacarpophalangeal joints of the hand), unipolar silicone devices are no longer recommended for orthopedic use.