Constipation is a common patient complaint and is frequently secondary to poor bowel or dietary habits. Organic causes include endocrine or electrolyte abnormalities, colonic neoplasm or other obstructing mass lesions, and neurologic dysfunction such as Hirschsprung’s disease. Constipation that is refractory to treatment or results in complications such as fecal impaction warrants consideration of occult causes. One rare cause of chronic constipation is sacral agenesis. Sacral agenesis in a triad of anorectal malformation, sacral bony abnormality and a presacral mass (which may be a meningocele, a teratoma or an enteric cyst) is known as Currarino syndrome. 1 In most cases, the syndrome (also known as Currarino’s triad) is diagnosed in childhood, with most descriptions being found in the pediatric literature. It is extremely uncommon for the syndrome to present in adulthood. We describe a man who presented with a fecalith and lifelong absence of spontaneous bowel movements as his only indication of Currarino syndrome.
Case report
A 59-year-old man was referred with a right lower quadrant mass and a history of lifelong constipation. He had chronic painful abdominal cramps and distension but except for mild hypertension he was healthy. He claimed to have never had a spontaneous bowel movement. His normal bowel habit consisted of one bowel movement per week following oral use of Agarol, replaced more recently by milk of magnesia. He denied a change in his bowel habit, unusual weight loss or rectal bleeding, and he had no history of bladder or sexual dysfunction. He reported that 2 maternal aunts and a maternal uncle had similar bowel symptoms.
Examination revealed a distended abdomen with a spherical, freely mobile mass 15 cm in diameter in the right lower quadrant that was presumed to be a fecalith. A barium contrast study planned before referral could not be performed because of severe anal stenosis. The patient’s anus was so stenotic that no more than 2 phalanges of the index finger could be inserted.
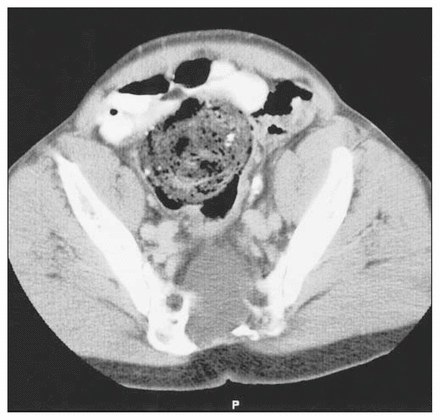
Computed tomography of the patient’s pelvis and abdomen (Fig. 1) confirmed fecal impaction at the rectosigmoid junction with dilatation of proximal large bowel in the right lower quadrant. It also revealed partial sacral agenesis, a probable anterior sacral meningocele and an associated solid soft-tissue mass, measuring 2 cm in diameter, inferiorly. A horseshoe kidney with bilateral duplex collecting systems was also observed. Subsequent neurologic testing of motor and sensory function performed to S1–2 yielded results within normal limits.
On computed tomography, the axial view of the pelvis shows fecal impaction at the rectosigmoid junction and partial sacral agenesis with an anterior sacral meningocele.
The presumptive diagnosis was large-bowel obstruction, made on the basis of an impacted fecalith and atonia secondary to sacral agenesis. The patient was scheduled for resection of the mass. At laparotomy, dilated loops of small and large bowel as well as a thin-walled megacolon were found. A large impacted fecalith was located at the rectosigmoid junction. The involved segment was resected and primarily anastomosed after dilatation of the stenotic anus. Due to a distended, thin bowel wall and poor bowel preparation, a defunctioning transverse loop colostomy was performed. Postoperatively, the patient experienced a prolonged ileus, which was believed to be related to his underlying megacolon. This gradually resolved and, 11 days after surgery, he was discharged home having regular bowel movements. Pathology reports of the resected bowel showed no evidence of atypia or malignancy. Over the next 4 months the patient recovered well, noting an improvement in his appetite and no further abdominal distension or discomfort.
Five months postoperatively, after demonstration of anastomotic patency on single-contrast barium enema, the patient underwent reversal of his colostomy. He again suffered a prolonged colonic ileus postoperatively. However, 10 days later he was discharged home tolerating a regular diet and having regular bowel movements. The patient continued to thrive and gain weight. Although he stated that he was having normal bowel movements without aid of a laxative, he was advised to use a laxative on a regular basis.
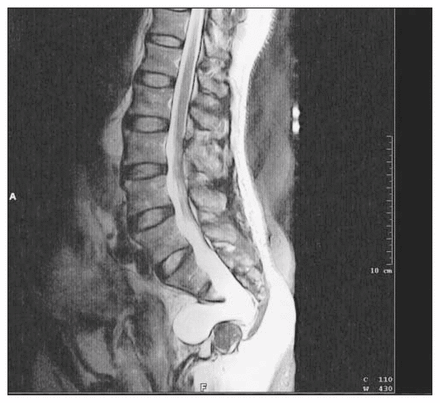
To confirm the diagnosis of Currarino syndrome, magnetic resonance imaging of the lumbosacral spine was performed 10 months after reversal of the colostomy (Fig. 2). The results confirmed the findings of the previous CT. Partial sacral agenesis was observed with non-formation of the segment inferior to S2. An anterior meningocele, measuring 4.5 × 4.8 × 2.7 cm, was observed at the site of the sacral agenesis, and inferior to the meningocele in the presacral region was a mass of indeterminate nature measuring 2.8 × 2.7 × 2.5 cm. This mass abutted the meningocele without definite invasion and was thought to be separate from the meningocele, although this fact could not be definitely established. A possible posterior septation or lobulated component was demonstrated. The mass did not appear to arise from any adjacent structure. It was suggested that it was dermoid due to the indication of lipid content.
On magnetic resonance imaging, sagittal view, the lumbosacral spine shows partial sacral agenesis with an anterior meningocele and an associated mass inferiorly. [F indicates the direction of the patient’s feet.]
Discussion
The triad of anorectal malformation, sacral bony abnormality and a presacral mass was first described by Bryant in 1838.2 Kennedy in 19263 and Ashcraft and Holder in 19744 further characterized the condition, with Currarino and associates1 in 1981 recognizing the triad as occurring by a common embryogenic mechanism. Since literature concerning the syndrome is rarely seen in surgical journals, it remains largely unknown in the surgical community beyond, perhaps, a small number of pediatric surgeons. Therefore, we sought to describe this unusual cause of a common problem.
In over 80% of cases, presentation of Currarino syndrome occurs in infancy or childhood.5 Symptoms such as intractable constipation, bowel obstruction in infancy, urinary retention, incontinence and infection are frequently associated with this condition.5–8 Although rare, there have been reports of the syndrome presenting in adulthood.2,5–16 In these cases, in addition to the symptoms already mentioned, dysmenorrhea, obstructed labour, perianal sepsis or low back pain may also constitute the initial complaint.7–9,17,18
Patients with Currarino syndrome frequently present with other anomalies including hydronephrosis, vesicoureteric reflux, duplex ureters, congenital single kidney, urinary incontinence, voiding dysfunction, tethered cord, bicornuate uterus, subseptate vagina, and rectovaginal fistulas.1,6–9,19 Thus, it is important to note that, although his urologic function was normal, our patient had an associated horseshoe kidney and a bilateral duplex collecting system.
In their review of the literature, Lynch and associates8 found that 16% of patients with Currarino syndrome presented with bowel obstruction in infancy. However, in our own review, we did not discover any adults presenting with a massive fecalith similar to our patient’s. Therefore, we believe that this type of presentation in adults is quite rare. In those who do present with Currarino syndrome in adulthood the diagnosis is usually made in 1 of 3 situations.
The syndrome, recently linked to the HLXB9 homeobox gene, is familial in approximately half of all cases and often demonstrates in an incomplete form.1,5,6,8,20 Family screening has been suggested as a routine part of management to allow identification of asymptomatic family members at risk.6,8,9,14,16–19
Previously mild symptoms of Currarino syndrome can be exacerbated during pregnancy, labour and delivery, or discovered during routine prenatal ultrasonography.2,5,11,12
Meningitis: due to an infection arising from spontaneous rupture, iatrogenic puncture of the presacral mass, or a fistula between the rectum and the presacral mass.1,11,15,21
When present, bowel obstructions associated with Currarino syndrome have been variably attributed to spinal cord tethering, obstruction from the presacral mass or obstruction due to rectal malformation. 8 However, none of these explanations adequately accounts for the presence of our patient’s fecalith. Our patient did not suffer from a tethered cord. During surgery, it did not appear that the presacral mass was causing a blockage of the colon. There was no pressure exerted by the presacral mass on the colon nor was there a fistula between the presacral mass and the colon. Our patient did suffer from severe anal stenosis; however, it is unlikely that anal stenosis alone would result in the development of this massive fecalith since the point of fecal impaction was located at the rectosigmoid junction. This gives rise to the intriguing possibility that our patient’s ailment was the result of a focal neurologic deficit affecting a segment of his colon even though his bladder and sexual functions were spared. However, this hypothesis would be difficult to verify.
Regardless of the direct cause of constipation associated with Currarino syndrome, it is generally agreed that the majority of patients with this syndrome require surgical management to resolve the bowel symptoms. Most authors recommend resection and excision of the presacral mass in order to (1) avoid the possibility of malignant degeneration of a teratoma, although this is a very uncommon occurrence;5,6,8,18 (2) avoid infection and meningitis arising from an existing rectal–presacral mass fistula, an accidental presacral mass rupture or an accidental presacral mass puncture; 1,11,15,20 and (3) relieve external pressure on the rectum.1,8,22 However, surgical excision poses several risks including postoperative infection, meningitis and nerve damage resulting in possible bladder and sexual dysfunction.1,5,7,19
Proper treatment of Currarino syndrome varies according to the severity of the case. It has been suggested that disease of milder severity can be successfully managed by conservative treatment.8 Given our patient’s age at presentation, the absence of a fistula between the rectum and the presacral mass, and the apparent absence of external pressure from the mass, we considered he was suffering from a less severe form of the condition. Also, the statistics provided by others illustrate that our patient had little risk of malignant degeneration.5,6,8,18 Therefore, we believe that conservative treatment, including resection of the deficient segment of the rectosigmoid colon in combination with dilatation of the stenotic anus, was warranted. As demonstrated by the outcome of his management, this can result in improved bowel function while avoiding the dangers engendered in resection of the presacral mass. Thus, it would seem reasonable in the adult with mild Currarino syndrome to avoid excision of the presacral mass since rectosigmoid resection and anal dilatation can provide a relatively safe and effective resolution of the patient’s symptoms.
We report this case to increase awareness of occult existence of Currarino syndrome and to emphasize the importance of considering the syndrome when approaching cases of long-standing refractory constipation, fecal impaction or a family history of similar problems. Identification of the syndrome allows for both therapeutic and prophylactic management of anomalies. Imaging in the form of CT or MRI should follow detection of sacral bony abnormalities on plain film to aid identification of associated presacral masses. In a case such as this, laparotomy and bowel resection with diverting colostomy, as well as consultation with relevant disciplines regarding management of the presacral mass is recommended. Continued follow-up is needed to better characterize long-term outcome of surgery.
Acknowledgements
We acknowledge Dr. Shim Felsen, Don Valley Medical Associates, for his initial examination and referral of this patient and Dr. Hassan Deif, North York General Hospital, for his assistance with the radiologic findings
Footnotes
Competing interests: None declared.
- Accepted February 11, 2003.