Adrenal cysts are rare, and mostly asymptomatic. The incidence in autopsy series varies from 0.064% to 0.18%.1 With computed tomography (CT) and ultrasonography, more cysts are being detected incidentally. In one study, adrenal cysts were discovered incidentally in 0.02% of 12 000 CT scans.2 We describe a case of a giant adrenal pseudocyst mimicking a malignant lesion.
Case report
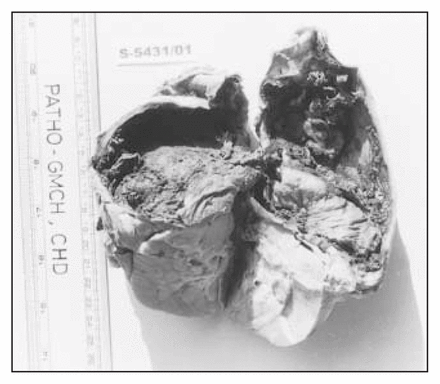
A 16-year-old girl presented with 1- month history of right-side flank pain and an abdominal mass, palpable in the right lumbar region. CT revealed a cystic adrenal mass adherent to upper pole of the right kidney. Fine-needle aspiration yielded a hemorrhagic aspirate. Cytologic examination revealed a few scattered benign cells. The possibility of a malignant tumour was considered because of the large size of the lesion and the hemorrhagic aspirate. At lap-arotomy, the cyst was found to be densely adherent to the posterior abdominal wall, the liver and the right kidney (Fig. 1). It was resected en bloc, with ipsilateral nephrectomy. The cyst was unilocular and measured 11 × 11 × 10 cm. It contained reddish brown fluid. Cyst-wall thickness ranged from 0.3 to 0.5 cm. Microscopically, the innermost part of the cyst was lined by hemosiderin-laden macrophages, and the wall was composed of fibrocollagenous tissue. Normal adrenal cortical tissue was compressed to the periphery.
Excised adrenal cyst. The cyst is densely adherent to the underlying kidney.
Comment
Adrenal cysts are rare: over 300 cases have been reported in the literature.3 Four types are recognized: parasitic, epithelial, endothelial and pseudocyst. Adrenal pseudocysts are defined as cystic lesions arising within the cortex or the medulla, enclosed by a fibrous wall that is devoid of a recognizable lining. They are the commonest of all the non-neoplastic cysts of adrenal origin, accounting for 40% of reported adrenal cysts, but are sufficiently uncommon to cause concern, both clinically and diagnostically. Cysts occur from birth to 80 years, with a peak in the third to sixth decade. The female:male ratio is 2:1. The majority of the adrenal cysts are asymptomatic. Large cysts can give rise to lumbar pain, vomiting, gastrointestinal discomfort and abdominal mass. An acute abdomen and a tender mass have been reported occasionally, likely to be due to intracystic hemorrhage, rupture or infection.1
The pathogenesis of adrenal pseudocysts is unclear. Theories include vascular neoplastic growth, malformation and hemorrhage into the adrenal parenchyma.4 Pseudocysts tend to become adherent to adjacent structures and mimic malignant tumours, as in our case. The distinction between benign and malignant adrenal cyst can be difficult. Underlying carcinoma should be suspected in patients with a high erythrocyte sedimentation rate, mixed echoes on ultrasonography, stippled calcification on plain films and neovascularization on arteriography. Some have recommended aspiration of adrenal cysts larger than 3.5 cm: a clear aspirate largely excludes malignancy, but a hemorrhagic aspirate may indicate malignancy or bleeding in a benign cyst.5
Surgery is indicated when the aspirate is hemorrhagic, the cyst is functional, the cyst wall is irregular on cystography, or if a pheochromocytoma is suspected. If the criteria for a simple nonfunctioning cyst are satisfied, the patient may be treated conservatively with aspiration alone. If the cyst enlarges with recurrence of symptoms, it may be reaspirated or excised. Nephrectomy has been rarely reported in the literature, owing to adhesions.6 In our case, the adrenal cyst simulated a malignant lesion, and a nephrectomy had to be performed because of the dense adhesions.
Footnotes
In this section we publish brief case notes that we believe contain information of interest to Canadian surgeons.
Competing interests: None declared.