After a fall from standing height, a 54-year-old woman was examined at the emergency department and discharged. Her evaluation included radiographs observed to be normal except for an isolated pubic ramus fracture. Over the ensuing 2 weeks she became bedridden with pain and increasing numbness in her feet, and was readmitted to hospital. Her strength was preserved, but she had numbness in the posterior legs and her soles, saddle anesthesia and an absence of rectal tone, and had become incontinent (both stool and urine). Clinical examination of this cachectic woman found ecchymosis and tenderness over the sacral spine.
Upon admission, the right pubic ramus fracture was observable on an anteroposterior x-ray of her pelvis, along with significant osteopenia (Fig. 1). The lateral lumbosacral x-ray taken just after her initial fall showed acute kyphosis and anterolisthesis of S1 over S2 (Fig. 2), which had been missed by the initial trauma team. Other conclusions from the plain films were difficult because of patterns left by overlying bowel gas; a CT scan, however, exhibited a U-shaped fracture pattern around the body of S1 (Fig. 3). MRI further characterized the injury, demonstrating an epidural collection consistent with hematoma located posterior to the S1 body as well as anterolisthesis of S1 over S2 and acute kyphosis at this level (Fig. 4).
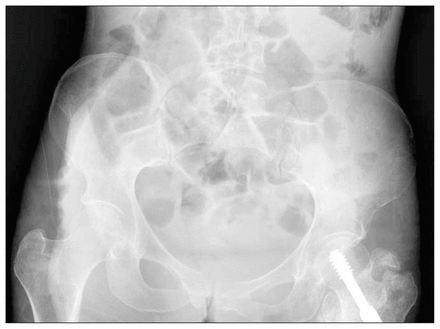
Anteroposterior pelvic radiograph showing right pubic ramus fracture and osteopenia. Details of sacral anatomy are obscured by the abdominal gas pattern.
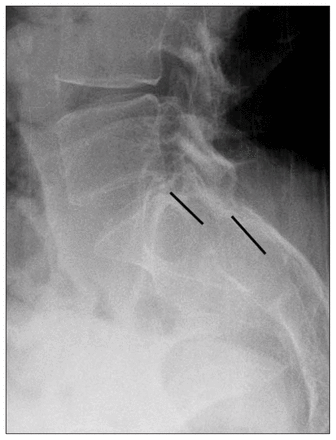
Lateral lumbosacral radiograph revealing acute kyphosis and anterolisthesis of S1 over S2. Lines represent the posterior margins of S1 and S2. In a patient with this type of severe osteoporosis the alignment is difficult but not impossible to determine.
Coronal CT reconstruction of the lumbosacral spine. The U-shaped fracture pattern around the body of S1 is characteristic of sacral insufficiency fractures. Arrowheads point to the fracture lines.
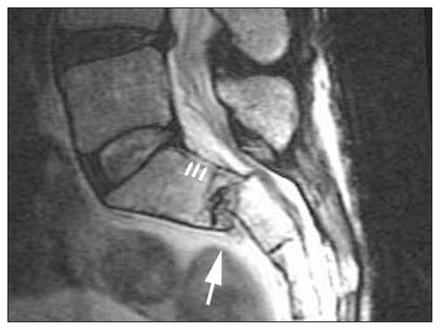
T2-weighted sagittal MRI of the lumbosacral spine demonstrating epidural collection posterior to the body of S1 (small arrows), acute kyphosis and anterolisthesis of S1 over S2 (large arrow).
The patient underwent urgent posterior decompression with sacral laminectomies from S1 to S3. Both S2 nerve roots were found to be entrapped in the fracture line and were freed. In addition, open reduction and internal fixation with bilateral sacroiliac screws at S1 and S2 were performed. The patient became progressively steadier on her feet and within 2 months regained partial sensation in her legs and full voluntary bladder and rectal control.
Review of the patient’s history revealed intestinal malabsorption as a cause for her severe malnourishment and consequent osteoporosis. The H-shaped pattern (U-shaped, in this case) of the fracture as seen on CT or bone scintigraphy is characteristic of sacral insufficiency fractures.
Sacral insufficiency fractures can be expressed as low-back pain in the elderly. Plain radiographs often do not clearly reveal the abnormality, particularly in the absence of a lateral x-ray of the lumbosacral spine. These injuries require a high index of suspicion for the diagnosis to be made. The spine may become unstable in flexion; open reduction may be warranted for stabilization and early mobilization. Patients with these fractures may present with cauda equina syndrome that is often delayed in its manifestation.
Footnotes
Submissions to Surgical Images, musculoskeletal section, should be sent to the section editor: Dr. Edward J. Harvey, McGill University Health Centre, Montreal General Hospital, 1650 Cedar Ave., Montréal QC H3G 1A4; edward.harvey{at}muhc.mcgill.ca
Competing interests: None declared.