A lack of level 1 evidence, the rarity of the tumour and difficulty in distinguishing primary from secondary lymphomas make the management of rectal lymphoma controversial. To illustrate decision-making we describe a case and discuss treatment options.
Case report
A 52-year-old woman had bled from the rectum for 2 months. Digital examination identified a 2.5-cm tumour on a stalk arising from the anal canal. Sigmoidoscopy led to a presumptive diagnosis of a benign fibroma or epithelial polyp. When excised transanally (in pieces because of friability) the tumour measured 3.0 cm with a 2-cm base 1–2 cm from her anal verge.
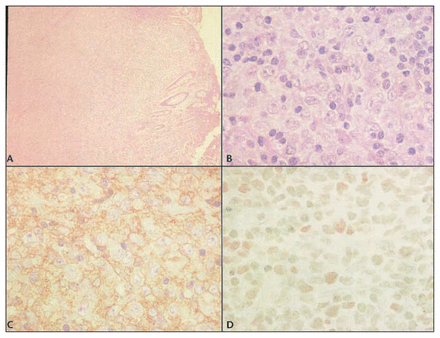
The excised specimen contained portions of fleshy tan-brown tissue, 4.5 cm in aggregate diameter. Thin sections revealed a diffuse proliferation of large neoplastic cells replacing the glands in the lamina propria, with surface ulceration (Fig. 1). The cells had oval to round vesicular nuclei with fine chromatin and 2–4 membrane-bound nucleoli. There were monomorphic and polymorphic cells with scanty amphophilic to basophilic cytoplasm. Immunohistochemical staining showed neoplastic cells that gave positive results for leukocyte common antigen, CD20, Bcl-2 and Bcl-6. The overall appearance of the tumour was compatible with a diffuse large B-cell lymphoma; Bc1-6 positivity suggested an origin in a follicular centre.
The microscopic appearance of a rectal polyp. A. Diffuse large B-cell lymphoma (DLBCL). Note the diffuse infiltrate pushing the glands (hematoxylin–eosin, original magnification ×20). B. DLBCL, centroblastic variant. The tumour cells have a polymorphic and polylobate appearance (hematoxylin–eosin, orig. mag. ×400). C. CD20 immunostain showing strong positivity in the cell membrane (orig. mag. ×400). D. Bcl-6 immunostain shows prominent nuclear staining (orig. mag. ×400).
The lesion was present extensively at the excision margin. In view of the patient’s normal white blood count, spleen, liver and bone marrow; the absence of superficial, mediastinal and abdominal lymphadenopathy; and the lack of other grossly demonstrable involvement at the time of surgical treatment, the final diagnosis was a primary rectal, diffuse, large B-cell lymphoma. After her surgery the patient received adjuvant chemotherapy (cyclophosphamide, doxorubicin, Oncovin and prednisone).
Comment
Rectal lymphomas compose fewer than 1% of malignant rectal tumours.1 Since Dawson’s criteria2 for primary rectal lymphoma have become accepted for diagnosis, and because management depends on whether a tumour is primary or secondary, initial strategies for differential diagnosis ought to include:
a complete physical search for associated adenopathy
chest radiography for mediastinal involvement
laboratory studies including leukocyte and differential blood cell counts
ultrasonography, computed tomography or magnetic resonance imaging to look for involvement of associated tissues such as the liver, spleen and para-aortic lymph nodes
a colonoscopy or barium enema to search for synchronous lesions
Irrespective of treatment, secondary involvement of the rectum usually confers a poor prognosis. Radiotherapy can afford some symptomatic relief. Rectal lesions do not seem to cause life-threatening complications.
There have been no prospective studies evaluating the relative benefits of adjuvant chemotherapy, radiotherapy, surgery or a combination of treatments for primary rectal lymphoma. Nevertheless, most case studies reveal a trend toward improved survival when surgery is used in combination with chemo- or radiotherapy. For example, 3 studies3–5 in which 20 patients with primary rectal lymphoma underwent surgery along with chemo- or radiotherapy or both reported survival rates ranging from 50%5 to 80%,4 whereas patients who received only nonoperative therapy had poor survival: 0%4,5–20%.3
Devine and colleagues4 have advocated that primary rectal involvement should be treated like primary lymphomas elsewhere in the gastrointestinal tract: with surgical excision followed by radiotherapy. If complete excision is not possible, then non-operative therapy becomes the treatment of choice.
To summarize: management strategies for rectal lymphoma are directed at investigating whether the tumour is primary or secondary. Inclusion of surgery for the treatment of primary rectal lymphoma confers a survival advantage over chemotherapy and radiotherapy alone. Secondary involvement of the rectum confers a poor prognosis; such patients should be managed with radiation alone, for relief of symptoms.
Footnotes
Competing interests: None declared.