Spontaneous rupture of the spleen (SRS) is a rare but serious complication of infectious mononucleosis (IM). Although its exact incidence remains unknown, SRS is the most frequent cause of death in IM. The nature of therapy remains controversial: most authors recommend splenectomy in all cases to avoid the possibility of sudden death in the early stages and the risks associated with blood transfusion,1–4 whereas others support conservative treatment considering the immunological importance of this organ.5–7 We report the first case of rupture treated with embolization of the splenic artery. Deciding the better alternative may be difficult, as illustrated by this report.
Case report
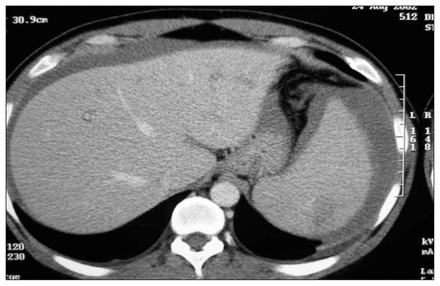
A 34-year-old man was admitted to the medical emergency unit after 5 days of left-upper abdominal pain radiating to the shoulder, fever, dyspnea and diarrhea. He had been complaining of flu-like symptoms for 2 weeks and been treated with an oral cephalosporin. His temperature was 38.7°C, his pulse rate 107 beats/min, and his blood pressure normal. Clinical examination revealed tenderness in the left-upper quadrant, splenomegaly and enlarged cervical lymph nodes. Laboratory tests found his hematocrit to be low (28%) and leukocyte count high (13 400/mm3, with a normal differential). Ultrasonography showed a homogeneous splenomegaly with a subcapsular hematoma and perisplenic fluid. Serology results were positive for an active Epstein–Barr virus infection. A few days later, computed tomography revealed a large subcapsular splenic hematoma with hemoperitoneum (Fig. 1).
Computed tomographic image showing a splenic hematoma with hemoperitoneum.
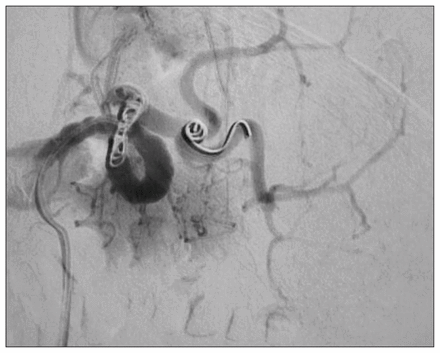
The patient was referred to the surgical unit for closer monitoring. The following day, his hematocrit level fell to 22%, and follow-up ultrasound demonstrated an expansion of the hematoma. He was transfused with 2 units (1 L) of blood. Selective angiography with embolization of his splenic artery was deemed necessary (Fig. 2). An antipneumococcal vaccine was administered; his recovery was uneventful.
Transcatheter coil embolization.
Discussion
IM is an acute, common, self-limiting disease in teenagers and young adults that is caused by the Epstein–Barr virus. Mortality from IM is about 0.1%. Its most serious and life-threatening complication is SRS.
The causal mechanism of SRS in IM is unclear. Two etiological factors have been implicated: an acute increase in portal venous pressure from a Valsalva-like manœuvre and compression of the spleen from contraction of the diaphragm or abdominal wall during vigorous coughing, vomiting or defecation.
Histologically, extensive infiltration of the splenic parenchyma with lymphocytes results from fragmentation of the splenic capsule, predisposing to rupture.
The spleen is most vulnerable to rupture in the second and third weeks after infection. This report illustrates that SRS may develop several days or even weeks after the onset of IM. Close follow-up, including imaging studies, is therefore recommended; the attending physician may have to alter surveillance and treatment plans accordingly.
Our patient was initially treated conservatively: in hemodynamically stable cases, this approach, as advocated for traumatic splenic injuries, is probably safe.5–7 Transfusion, prolonged hospital stay and physical activity restriction are generally required, however.1–8 In addition, delayed hemorrhage is possible, as SRS secondary to IM appears to be more likely to occur than splenic rupture after trauma.3,4
The risk of sepsis after splenectomy is higher in infants than in adolescents and adults.3,9–11 Administration of pneumococcal vaccine has minimized the occurrence of this complication.
In our patient, expansion of the hematoma and the need for transfusion were eventually regarded as indications for embolization. Transcatheter embolization of the splenic artery, which permits preservation of the spleen, has become an alternative to surgery for obtaining splenic hemostasis in the hemodynamically stable patient.
In conclusion, initial observation of hemodynamically stable patients with spontaneous splenic hematoma secondary to IM is adequate, but the threshold for operation should be low. Although splenectomy has been advocated in the past as the definitive therapy, we recommend transcatheter embolization of the splenic artery. Deterioration of our patient’s vital signs, requirement for blood transfusion and expansion of the hematoma seen on ultrasonography or CT imaging call for splenectomy.
Footnotes
Competing interests: None declared.
- Accepted February 16, 2004.