Presentation
A 49-year-old woman presented for evaluation of perineal discharge. Her medical history was significant for Crohn’s disease (CD) associated with severe colitis and perianal involvement, diagnosed at age 30 years. At age 42, she underwent a loop ileostomy for a rectovaginal fistula, with a total proctocolectomy and end-ileostomy 1 year later. The patient had been well for 6 years, until the development 1 month earlier of an abscess in her perineum, which ruptured spontaneously with moderate purulent drainage. Her physician prescribed an oral cephalosporin and referred her to a surgeon.
On examination, the abscess had resolved and the patient was asymptomatic except for a scant amount of yellow discharge from a 1–2-mm pinhole located in mid-perineum (midline). She had no symptoms or signs of CD. She was instructed to return in 1 month, or sooner if anything changed.
At follow-up, she remained completely asymptomatic; the pinhole/ discharge remained unchanged. She was referred for a sinogram (Fig. 1 and Fig. 2), which revealed a sinus tract (thin arrow, Fig. 2) extending from the skin to an unusual finding in the pelvis (thick arrow). What is the unusual radio-opaque end to this patient’s sinus?
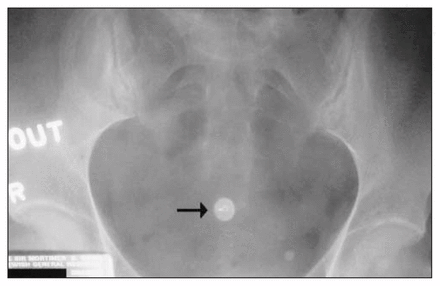
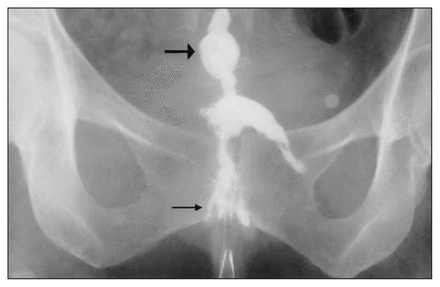
Diagnosis
This unusual end to her sinus is a thumbtack (thick arrow) embedded in the sacrum. This thumbtack was placed to control pre-sacral bleeding at the time of her proctocolectomy 6 years earlier. In 2 years of conservative management of this unusual problem, the patient has not had recurrence of symptoms. The diagnosis is sacral thumbtack sinus following proctocolectomy.
Presacral bleeding is not uncommon as a complication of pelvic dissection. When bleeding occurs from the presacral plexus, it can be massive and lethal.1 Hemostasis in these cases can be very difficult to achieve because of the complex system of intertwined veins both beneath and on the surface of the sacral periosteum.2 When the vessels of the plexus are severed, they tend to retract into the sacral bone, making bleeding very difficult to control. Bleeding is often brisk, and pooling of blood in the pelvis makes visualization and control difficult.
Various manoeuvres, techniques and devices have been developed, tested and used to attempt to control presacral hemorrhage. One of these devices, the “sacral thumbtack,” has been used with some success.3–6 Qunyao and coauthors2 first described achieving hemostasis with sterilized stainless-steel thumbtacks in 1985. The technique was developed in rural hospitals in China to control severe pelvic hemorrhage after low anterior resection. The thumbtack is placed into the sacrum over the area of bleeding, to tamponade the bleeding veins. The thumbtack remains in place permanently.
To our knowledge, this is the first report of a sinus tract complicating the use of a sacral thumbtack. It is undoubtedly related to the patient’s underlying CD.
Footnotes
Submissions to Radiology for the Surgeon, soft-tissue section, should be sent to the section editor: Dr. Lawrence A. Stein, Department of Radiology, Royal Victoria Hospital, 687 Pine Ave. W, Montréal QC H3A 1A1; lawrence.stein{at}muhc.mcgill.ca
Competing interests: None declared.






