Identification and dissection of the sentinel node is now standard in the treatment of melanoma. We describe a a patient with melanoma of the cheek demonstrating contralateral lymphatic drainage.
Case report
An 85-year-old woman was referred to our surgical oncology office after wide local excision of an intermediate-thickness melanoma of the right cheek. Her medical history was significant for hypertension. She had had no previous problems with her skin and there was no family history. The pathology report revealed a 1.2-mm thick melanoma, extending to one of the inked margins. She was scheduled for wide re-excision and sentinel lymph-node dissection.
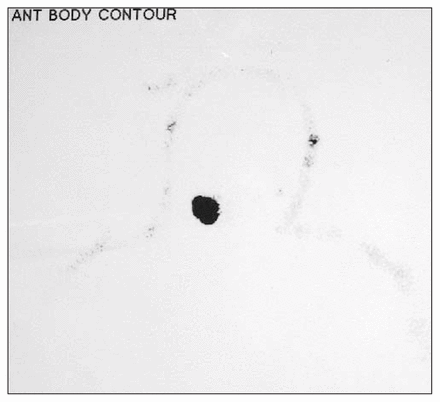
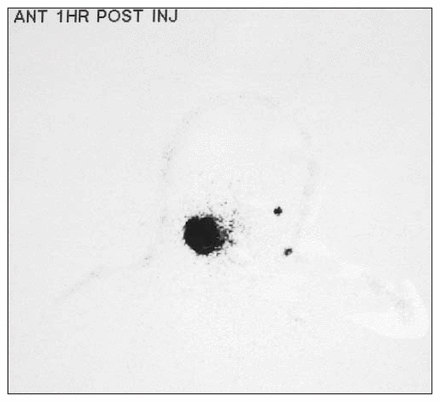
Approximately 4 hours before the operation, technetium 99m was injected at the previous excision site in the right cheek (Fig. 1). Nuclear scanning after the injection revealed increased radioactivity on the left side at 2 sites (Fig. 2). In the operating room, 3 mL of isosulfan blue dye was injected at the previous excision site. The blue dye was seen to move medially toward the base of the nose as well as to the buccal area and the angle of the mandible. Scanning intraoperatively with the hand-held gamma counter revealed that the lowest site on the left side of the nuclear scan (Fig. 2) was the point of highest uptake and correlated with the left submandibular region, contralateral to the primary lesion on the right cheek.
Scan after injection of technetium 99m at the site of the melanoma, 4 hours before operation (anterior view).
Scan 1 hour after injection of technetium 99m demonstrates radioactivity at 2 sites on the left side, contralateral to the primary melanoma on the right cheek.
Discussion
Before the advent of sentinel-node dissection, patients with intermediate-thickness melanoma were managed primarily by wide local excision and regional lymphadenectomy. In the head and neck region, this often entailed either radical neck dissection or modified radical neck dissection. With lesions of the scalp, management of the lymph nodes was particularly difficult because of the known ambiguity of the lymphatic drainage pathways. Lesions on the forehead, however, and especially those of the anterior part of the face, have well-defined lymphatic drainage to the ipsilateral nodes. The drainage is initially to the parotid or buccal nodes, then the superficial cervical or submandibular nodes, continuing down the ipsilateral cervical chain.
Local recurrence rates for lesions on the head and neck vary from 2% to as high as 13% after prophylactic (modified) radical neck dissection.1 The unpredictable nature of melanoma likely contributes to these figures. Our patient demonstrates that primary contralateral drainage is probably a factor in the failure rate of ipsilateral lymphadenectomy. One series had a 2.9% rate of contralateral recurrence after wide excision of facial lesions and ipsilateral neck dissection.2 Sentinel lymph-node identification has become the standard of care in melanoma. Figures vary slightly, but the combination of lymphoscintigraphy with technetium and isosulfan blue identify the sentinel node in well over 90% of cases. Its applicability in carcinoma of the breast has led to its investigation in several other cancers including colon cancer, thyroid cancer and gynecologic malignant disease. With sentinel lymph-node identification being one of the most captivating topics of recent times, this finding as a possible explanation for some of our past failures is just one more reason for our fascination.
Footnotes
Competing interests: None declared.
- Accepted March 9, 2004.