1. Botulinum toxin for treatment of chronic anal fissures: one surgeon’s experience
To evaluate the experience at a single centre with the use of botulinum toxin in the management of chronic anal fissures.
The records of all patients treated for chronic anal fissures from 2002 to 2005 were reviewed retrospectively. Data on outcomes and complications were collected.
Twenty-two patient charts were reviewed. Follow-up data were available for 17 patients. Mean follow-up was 10 weeks. Fifteen of 17 patients (88%) had improvement of their symptoms. Only 3 patients experienced symptoms of incontinence after treatment.
Botulinum toxin is an effective therapy in the management of chronic anal fissures and is an appropriate alternative to surgical treatment.
2. Withdrawn
3. Proctocolectomy in patients with colorectal cancer — a retrospective cohort study of indications and outcomes of the ileal pouch anal anastomosis compared to permanent ileostomy
The ileal pouch anal anastomosis (IPAA) is the procedure of choice in patients with ulcerative colitis (UC) and familial adenomatous polyposis (FAP). However, little is known about the role of reconstruction with the IPAA in patients with colorectal cancer (CRC) who require proctocolectomy. The purpose of this study was to assess the indications and outcomes of the IPAA compared with proctocolectomy and permanent ileostomy (PI) in patients with CRC.
Between 1983 and 2005, over 1600 patients with colorectal cancer have been treated at the Mount Sinai Hospital (MSH). Demographic, surgical, pathological and outcomes data for all patients have been maintained in the MSHCRC database. During that period, 51 patients were treated for CRC with proctocolectomy: 30 patients with PI and 21 patients with IPAA. Clinical features, pathologic findings and survival outcomes were compared between these 2 groups.
Patients in the PI and IPAA groups were similar with respect to age, gender, cancer stage, histologic grade and the presence of multiple primary CRCs. However, the diagnosis leading to proctocolectomy was more commonly UC or FAP in patients treated with IPAA (18/21 v. 21/30, p = 0.04). Moreover, patients with rectal cancer were more likely to have a PI than an IPAA (19/30 v. 7/21, p = 0.0002). Analysis using the Cochran–Armitage trend test suggests that utilization of IPAA has increased over time (p = 0.002). Finally, survival is similar after either PI or IPAA
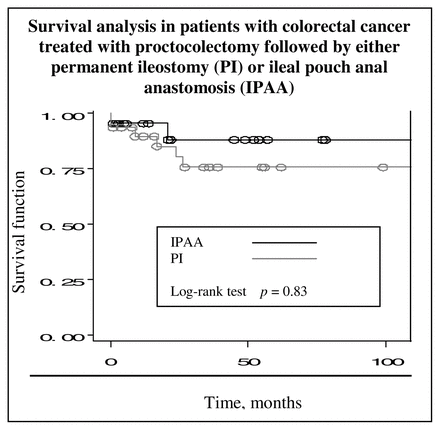
Increased experience and improved outcomes following IPAA has led to its more liberal use in patients who would otherwise require PI. Therefore, with careful patient selection, the IPAA is a viable and safe option for patients who would otherwise require PI.
4. Straight coloanal versus colonic J pouch versus transverse coloplasty for rectal reconstruction after low anterior resection: a systematic review
Total mesorectal resection (TME) has led to improved survival and reduced local recurrence in patients with rectal cancer. Straight coloanal anastomosis after TME can lead to problems with frequent bowel movements, fecal urgency and incontinence. The colonic J pouch and the transverse coloplasty were developed to improve bowel function. The purpose of this study is to determine which rectal reconstructive technique results in the best postoperative bowel function.
A systematic review of the literature (MEDLINE, CANCERLIT, EMBASE and Cochrane databases) was conducted independently by 2 investigators. Of 2014 relevant studies, 14 randomized controlled trials (RCTs) met our inclusion criteria: adults with rectal cancer, low rectal resection, and comparison of bowel function between at least 2 of straight coloanal anastomosis (SCA), colonic J pouch (CJP) or transverse coloplasty (TCP).
Results of 11 RCTs (n = 597) investigating SCA versus CJP suggest fewer bowel movements and fewer patients experiencing fecal urgency up to 8 months postoperatively. However, more than 8 months after surgery, bowel frequency, urgency and fecal incontinence scores are similar between SCA and CJP. Three RCTs (n = 158) compared CJP with TCP. These studies demonstrated similar bowel function, but one study suggests a higher anastomotic leak rate with TCP.
A systematic review of the literature reveals that CJP improves bowel function in the first year postoperatively when compared with SCA. While outcomes appear to be similar after CJP and TCP, further RCTs are needed to clearly elucidate surgical and functional outcomes.
5. Clinical outcomes of laparoscopic and open colorectal resection: a meta-analysis
Our objective was to evaluate whether current evidence about clinical outcomes of laparoscopic and open colorectal resection supports the adoption of laparoscopic resection as standard care. Randomized clinical trials (RCTs) comparing these procedures were identified by searching MEDLINE and other electronic sources, reviewing reference lists and questioning content experts. Clinical outcomes and other data were abstracted independently by 2 reviewers.
We identified 24 reports of RCTs to which 3202 patients had been randomized. Diagnosis was colorectal cancer in 2816, benign in 286 and not specified in 100 patients; 1431 patients (89% of 1610 patients) were ASA physical status class 1 or 2 and none were class 4 or 5; 1174 (44% of 2667 patients) and 802 (30%) patients had sigmoid or right colon resections. Among patients having laparoscopic resection, colorectal cancer was stage 1 in 389 (27%), 2 in 500 (35%), 3 in 432 (30%) and 4 in 108 (8%). The overall conversion rate was 17% (273/1602 patients). In 14 reports, data for patients converted to an open procedure were analyzed with the laparoscopic group, or there were no conversions; in 10 reports, the data were analyzed in another manner or not reported. Operative mortality and pulmonary complications did not differ between laparoscopic and open resection. Wound infection and anastomotic leaks appear less frequent following laparoscopic resection. Lymph node retrieval, cancer recurrence and survival did not appear to differ between laparoscopic and open resection.
Current evidence suggests that differences in clinical outcome between laparoscopic and open colorectal resection are modest. Patients enrolled in published RCTs have tended to be relatively healthy and to have localized cancers; few have had benign disease.
6. Preoperative high dose rate endorectal brachy-therapy (HDREBT) for locally advanced operable rectal cancer
In an attempt to decrease the toxicity associated with preoperative chemotherapy and external beam radiation, HDREBT was used preoperatively in patients with locally advanced resectable rectal cancer with the objective of evaluating the treatment toxicity and the effects on local control. Patients with newly diagnosed resectable adenocarcinoma of the rectum and no evidence of metastasis were eligible. A dose of 26 Gy was prescribed to the tumour bed and intramesorectal deposits seen on MRI and given over 4 consecutive daily treatments, using high dose rate delivery system. Surgery was done 4–8 weeks after brachytherapy completion. Those patients with positive nodes were to receive postoperative adjuvant 5-FU chemotherapy and external beam radiation with 45 Gy in 25 fractions.
One hundred patients were treated on protocol between 1998 and 2002. Based on preoperative endorectal ultrasound and MRI, the study included 93 T3 tumours, 4 T4 and 3 T2 tumours. All patients completed their planned treatment. The median age was 72 (range 42–90) years old. Acute proctitis was observed in all patients 7–10 days after the treatment. In 99 patients, the radiation proctitis was of grade 2, while 1 patient (grade 3) required blood transfusions. There was no hospitalization for treatment-related toxicity.
Two patients refused the planned abdominal resection based on a normal restaging endorectal ultrasound. Two patients died before surgery. One died from a stroke and the other from a myocardial infarct. A leak rate of 8% was observed. Among the surgical specimens, 29% were ypT0N0–1, 34% showed residual tumour and 37% showed microfoci of residual disease. Postoperative adjuvant external beam therapy and chemotherapy was given in 27 of the 31 patients with positive nodes. The median follow-up time was 42 months. At 5 years, the actual local recurrence rate is 3%, the disease-free survival is 65%, the overall survival rate is 74% and the specific survival 84%.
HDREBT is effective as a new downstaging modality and prevented tumour recurrence in this study. The 1% grade 3 acute toxicity compares favourably with the 25%–30% grade 3 toxicity with the chemotherapy and external beam radiation. A phase III study is highly desirable.
7. Treatment of the primary tumour in patients with stage IV colorectal cancer: a systematic review of the literature
To systematically review the literature on the treatment of the primary tumour in the setting of metastatic colorectal cancer (CRC).
A bibliographic search of MEDLINE (1966–October 2004) and EMBASE (1980–October 2004) was conducted to identify studies of patients with metastatic CRC and the surgical treatment of the primary tumour. Articles were included if the population of interest was patients with metastatic colorectal cancer, the interventions included both a resection group (RG) and non-resection group (NRG) and the outcome was median survival.
Five retrospective cohort studies met the criteria. The smallest study included 5 patients in the NRG, and the largest study included 127 in the RG. One of the 5 studies had no information regarding confounders, and another study was too small to draw any conclusions about similarities between the 2 groups (n = 5). In the 3 remaining studies, the RG included more right-sided cancers than the NRG. Two studies reported the functional status of the patients, and in both cases the RG had a better functional status than the NRG. Co-interventions were not reported in 4 of the 5 studies. Four studies showed an improvement in survival in those patients who had their primary tumour removed. The range of median survival in the NRG was between 2 months and 16.6 months. The range of median survival in the RG was between 11 months and 16 months.
Patients with stage IV CRC who are selected to have their primary tumour removed have a prolonged survival compared with those who are not selected to have their primary tumour removed. Because of selection bias, it remains unknown whether or not it is better to resect the primary tumour electively, and, therefore, a randomized controlled trial is required to answer this question.
8. Knowledge retention after a continuing medical education course on total mesorectal excision for surgeons
The purpose of this study was to determine whether knowledge gained (as determined by a formal course test) by surgeons in a continuing education course on total mesorectal excision and rectal cancer management is retained 1 year later.
A formal course test had been previously developed and validated. The test evaluated course content including pelvic anatomy, surgical techniques, imaging, pathology, adjuvant therapies, and cancer and functional outcomes. Validation was determined by absence of change in pre- and post-test scores of the “expert” course instructors (n = 8, p = 0.6) and by a linear correlation in test scores with increasing level of general surgery resident training (n = 16, p = 0.001). Significant learning by the 58 surgeons taking the course had been demonstrated by improvement in test scores from before the course (mean score 19 out of a possible total mark of 33) to after the course (mean score 25.3, p = 0.001). At 1 year after the course, those course participants (n = 44, 76%) who had provided post-course contact information were asked to complete the course test again.
Responses were received from 18 surgeons (41% of those surveyed, 31% of the original course participants). Mean score on the test after 1 year was 23.8. Compared with the immediate post-test scores, there was no significant knowledge loss over the year (p = 0.09).
We conclude that knowledge acquired during a continuing education course for surgeons on total mesorectal excision and rectal cancer management is retained 1 year later.
9. Evaluation of the surgical options for the treatment of diverticular disease — the Cleveland Clinic diverticular disease propensity score
The present study compares early outcomes between the primary resection and anastomosis (PRA) and Hartmann’s procedure (HP) and describes a propensity score for the selection of patients for restorative versus non-restorative procedures.
Data were collected from 731 patients undergoing primary resection and anastomosis and 123 patients undergoing primary HP for diverticular disease. Primary outcomes were 30-day operative mortality, medical, surgical adverse events (the latter referring to complications related to surgical technique) and readmission rates. Multifactorial logistic regression was used to model the risk of death, postoperative complications and the likelihood of performing a restorative PRA versus non-restorative procedure.
The apparent variation in adverse events between the 2 treatment groups was explained (PRA v. HP, adjusted OR 1.026, p = 0.932) by the differences in age (OR 1.04 per 10-yr increase), ASA grade (ASA IV, III, II v. I, OR 11.8, 6.0, 2.8), extent of diverticular disease (right- and left-sided v. left-sided, OR 2.1) and operative urgency (emergency, urgent v. elective surgery, OR 1.9, 1.5). Independent predictors in favour of HP were the number of patient comorbid conditions (OR 1.4 per unit increase), preoperative duration of peritonitis in excess of 24 hours (OR 3.8), presence of bowel perforation (OR 5.1), diffuse peritonitis (OR 5.1) and operative urgency (emergency, urgent v. elective surgery, OR 6.7, 11.5).
Although HP was associated with higher incidence of postoperative adverse events, following adjustment of confounding factors, HP and PRA were equally effective for the treatment of diverticular disease. The choice of operation was dependent on the patient presentation and intra-abdominal contamination, which can be quantified in the preoperative setting with appropriate treatment plans made for individual patients.
10. Effect of ischemia on intestinal anastomotic healing: the role of hypoxia-induced angiogenesis
Impaired healing and subsequent leakage of intestinal anastomosis is a major complication of intestinal surgery. Studies have shown that adequate local tissue oxygen level is a significant determinant of anastomotic integrity. Prior studies by our lab have demonstrated that systemic hypoxia impairs intestinal wound healing, with a reduction in anastomotic burst pressure.
To determine if hypoxic-induced impairment in wound healing is due to a reduction in angiogenic cytokine production and/or subsequent neovascularization.
Seventeen juvenile male Sprague–Dawley rats underwent colonic transection with immediate re-anastomosis and were placed in a normoxic (FiO2 21%) or hypoxic (FiO2 11%) environment for 7 days. Local tissue hypoxia was confirmed by direct measurement. At sacrifice, peri-anastomotic tissue samples were examined for neovascularization with von Willebrand factor (vWF) immunohistochemical staining and vascular endothelial growth factor (VEGF) Western blot analysis.
Hypoxia resulted in a qualitative and quantitative increase in neovascularization in hypoxic versus normoxic conditions (overall mean vWF neo-vessel density 47.12 ± 10.60 v. 23.29 ± 10.17, p = 0.0005). In parallel, mean VEGF protein expression was elevated in hypoxic versus normoxic specimens (247.1 ± 9.5 OD/mm2 v. 142 ± 10.6 OD/mm2, p < 0.002).
We have previously shown that systemic hypoxia translates into local tissue hypoxia in surgical anastomotic specimens with a reduced mean burst pressure. The result of the present study demonstrates that both cytokine-mediated angiogenic stimulation (VEGF) and directly visualized vWF neovascularization is increased in hypoxic tissues. These findings suggest that the deleterious effects of hypoxia on wound healing occur downstream of revascularization, affecting processes such as collagen synthesis or cross-linking.
11. Improved outcome due to increased experience and individualized management of leaks following ileal pouch anal anatomosis (IPAA)
To assess the management and outcome of leaks in patients with ileal pouch anal anastomosis (IPAA).
Between 1981 and 2003, 1424 patients underwent IPAA: 145 leaks (10%) occurred in 141 patients (81 male, 60 female; median age 36). These patients’ charts were reviewed.
Of 141 patients experiencing a leak, 94 had a defunctioning loop ileostomy and 90 were taking steroids at the time of operation. Eleven asymptomatic leaks were evident only on radiologic contrast studies. The remaining 134 leaks were IPAA leaks without (48) or with (30) an associated abscess, cutaneous fistulae (15) or associated vaginal fistulae (18). Twenty-three were leaks from the ileal pouch itself. Median time to leak was 18 days (range 1 d–10 yr). Overall, the leaks healed in 119 (84%) patients, and they have a functioning ileal pouch. Of the remaining 22, 18 (13%) had their ileal pouches excised and 4 (3%) with pouches in situ have permanent ileostomies. There were no significant differences in healing rates among the various leak types. Healing rates by primary treatment were: rectal tube pouch drainage 53/58 (91%), percutaneous drainage 19/22 (86%), perineal drainage 8/10 (80%), transanal repair 22/32 (69%), laparotomy and repair 4/5 (80%) and pouch reconstruction 13/18 (72%). For the period 1993–2003, the salvage rate (90%) was higher than for 1981–1992 (80%).
The salvage rate of pouches following IPAA leak has increased over time so that 90% of patients will have a functioning pouch. Various methods of management may be required depending upon the type of leak and other clinical factors.
12. Hospital readmission rates after ileal pouch anal anastomosis
The objective of this study was to determine the unplanned hospital readmission rate following ileal pouch anal anastomosis (IPAA) prior to loop ileostomy closure.
This retrospective epidemiologic observational study identified all patients who had undergone IPAA at a single teaching hospital in Calgary over a 5-year period. The percentage of patients readmitted prior to elective ileostomy closure was determined. Steroid use, duration of illness, elective versus emergent indication, age, use of regional anesthesia and length of stay (LOS) were evaluated as factors possibly predictive of early readmission. Readmission diagnoses were compiled. LOS and in-hospital costs were compared between patients readmitted and not readmitted.
Thirty-six of 105 patients (34%) undergoing IPAA had at least 1 unplanned readmission following IPAA: 23 had a single readmission, 9 patients had 2 admissions, and 5 patients had more than 2 admissions. Small bowel obstruction was the most common readmitting diagnosis (20/57). There were 14 readmissions for pelvic or intra-abdominal abscess. Additional readmitting diagnoses included abdominal pain, dehydration, portal vein thrombosis, wound dehiscence and enterocutaneous fistula. Fifteen patients (14%) required operative intervention following readmission and 21 (20%) were managed nonoperatively.
Patients operated on in an emergent situation were more likely to be readmitted compared with those who underwent elective surgery (23/48 [48%] v. 13/57 [23%], p = 0.007). Perioperative steroid use (p = 0.027) and age < 35 years (OR 3.19) were other factors that significantly influenced readmission rates. LOS for patients requiring readmission (including the initial admission for IPAA) averaged 22.7 days versus 9.7 days for patients not readmitted. Not including the costs of reoperation/intervention, the average cost of IPAA for patients requiring hospital readmission was $31 069 versus $13 266 for patients not readmitted.
Hospital readmission after IPAA is common and costly. Readmission may be avoided in some high-risk, conservatively managed patients by instituting more intensive postoperative outpatient follow-up and support.
13. Evaluation of operative mortality and morbidity in surgery for diverticular disease — comparative analysis of surgical versus medical adverse events
The purpose of the study was to identify important predictors of operative mortality and morbidity in patients undergoing surgery for diverticular disease and to develop a disease-specific prognostic index for quantifying operative risk in such patients.
Data were collected from 921 consecutive cases undergoing 1071 major colorectal procedures for diverticular disease. Multilevel logistic regression was used to model the risk of death and postoperative complications. A multifactorial model was developed and compared with the Mannheim peritonitis index (MPI) and Hinchey classification (HC).
Operative 30-day mortality was 2.1%, and overall morbidity was 33.2%. Multivariate analysis identified the following independent risk factors of adverse outcomes: right- and left-sided disease versus sigmoid diverticular disease (OR 2.0), patient comorbidity, cardiac (OR 1.5), pulmonary (OR 1.4), renal (OR 1.9), widespread peritonitis (OR 1.4), large bowel stricture (1.7), presence of enterovaginal fistulae (OR 1.7), mode of presentation (emergency, urgent v. scheduled, OR 2.1, 1.6) and additional small bowel resection (OR 1.8). The model offered better discrimination (higher area under ROC curve) than the MPI and HC for all complications (0.67 v. 0.65, 0.63) and operative mortality (0.90 v. 0.85, 0.76). There were no significant differences between observed and model-predicted outcomes over various subgroups of patients.
The predictive model provided an accurate means of estimating the risk of adverse events for patients undergoing surgery for diverticular disease. It has important implications in everyday practice, as it may be used in the postoperative period for close monitoring of high-risk patients and for resource allocation.
14. How evidence-based are CAGS surgeons?
Experience and the teaching acquired from trusted, respected mentors and teachers define surgical practice. These factors may out-weigh best (level I) evidence, e.g., heparin and antibiotic prophylaxis, facial closure suture and technique, drain or nasogastric tube usage. It is likely that an increasingly informed and litigious public will demand that surgery be practised according to the strongest evidence.
This study sought to evaluate how much evidence-based surgery CAGS surgeons practise and whether demographic factors play a part.
Using email addresses obtained through CAGS, a previously piloted (n = 30) survey was administered.
Responses were received from 198 (80% male) CAGS surgeons from all provinces (35% Ontario, 17% Quebec, 15% Alberta, 12% BC). These surgeons had been in practice a median of 19 years with 80% working in communities > 100 000, 7% in 50 000–100 000 and 13% in < 50 000. A quarter had no university affiliation while 30% had clinical and 45% had fulltime faculty appointments. One in 3, 4, 5, 6 and 7 call was done by 11%, 15% 18%, 13% and 12%, respectively. Trauma call was done by 52%.
Bariatrics (5%), abdominal aortic aneurysm (11%) and cesarean section (11%) were the 3 least commonly done procedures, while laparoscopic appendectomy (82%), gastroscopy (69%) and thyroid (66%) were the 3 procedures done by the most surgeons.
Betadine (71%) was the most common wound prep, but only 15% used opsite. Eye protection was worn by 75%, but only 33% double gloved. Continuous polydioxanone suture (60%), continuous vicryl (22%) and continuous prolene (19%) were the most common fascial closure. In an elective uncomplicated colorectal resection, 92% would prep the bowel, 84% would prophylax with heparin, 93% with preoperative antibiotics, 46% with postoperative antibiotics, 40% would prescribe thromboembolic deterrent stockings, 18% would insert a nasogastric tube, only 5% would drain a colon resection, but 26% would drain a rectal resection.
General surgical practice amongst CAGS surgeons is diverse with considerable variability in acceptance of evidence-based practice. Gender, community size or university association or not were significant (p < 0.01) associations.
15. The Surgical Site Infection Working Group: timing of perioperative antibiotic administration remains a significant challenge
The Surgical Site Infection (SSI) Working Group at McMaster University in Hamilton, Ontario, has initiated a 3-phase study to develop new protocols for glucose control, perioperative temperature management and preoperative antibiotic prophylaxis in an effort to reduce the incidence of surgical infections in patients undergoing major abdominal surgery. Phase 1 is an observational study examining current practices for the above variables. We present the findings related to antibiotic administration from phase 1 of our study.
One hundred sequential patients undergoing major abdominal surgery classified as “clean-contaminated” are being followed prospectively in phase 1. The time of antibiotic initiation and surgical incision were abstracted from the patient’s record. Fifty-five patients have been enrolled to date; 37 patients have completed charts for review. Twenty-seven of the 37 patients received 2 preoperative antibiotics; 10 patients received 1 preoperative antibiotic. Six of the 37 patients received their first (or only) antibiotic within 30–90 minutes of the surgical incision (16.2%, range 0:35–5:43). Of 27 patients receiving 2 preoperative antibiotics, 7 received their second drug within 30–90 minutes of their incision (25.9%, range 0:20–5:28). One patient had 2 antibiotics ordered but only 1 documented as having been administered. Twenty-three patients started receiving their antibiotics more than 2 hours before surgery (62.2%). The combination of cefazolin and metronidazole was used most frequently (23 cases, 62.2%).
The majority of patients in this study received their preoperative antibiotics in a time frame that is associated with a dramatic increase in surgical site infection rates (N Engl J Med 1992;326:281–6). More work needs to be done to review and modify the process of perioperative antibiotic administration. This work is ongoing at our institution.
16. Infrastructure availability in British Columbia and implications for breast cancer care
The objective of the study was to assess how well hospitals in British Columbia meet the facility requirements of a leading breast cancer guideline. A provincial infrastructure survey was conducted by mail and compared with recommended requirements. Survey results show that only 10 hospitals meet the requirements of an international breast cancer guideline. Based on our results so far, of the 32 respondent facilities that conduct breast cancer surgery, women in these centres have access to the following equipment and services onsite: ultrasound (32/32), mammography (27/32), MRI (9/32), stereotactic core biopsy (10/32), mammotome (1/32), gamma probe (10/32), onsite nuclear medicine (12/32), onsite pathology (21/32) and pathology with tumour site expertise (13/32). Only 75% of facilities indicate that they have access to the BC Cancer Agency’s online cancer management guidelines. Results indicate that most hospitals in BC lack the infrastructure that has been demonstrated to produce the best outcomes in breast cancer treatment. This is particularly true in northern communities. In these regions, women have limited access to key services, therefore they have to travel hundreds of kilometres for care. Provincial strategies to promote the use of practice guidelines and referral protocols are crucial in overcoming these deficiencies in infrastructure. The BC Surgical Oncology Network has developed 2 guidelines for sentinel lymph biopsy to improve breast care for BC women.
17. Withdrawn
18. Le traitement coelioscopique du kyste hydatique du foie
Le but de ce travail est de rapporter les résultats préliminaires du traitement coelioscopique du kyste hydatique du foie.
Il s’agit d’une étude prospective portant sur 61 malades consécutifs ayant un kyste hydatique du foie et opérés par voie coelioscopique entre le 1er janvier 2002 et le 31 décembre 2004. Résultats : La population de l’étude est formée de 19 hommes et 42 femmes avec un age moyen de 50 ans (extrêmes 14 et 74 ans). L’échographie abdominale a permis le diagnostic dans tous les cas. Les kystes étaient uniques chez 56 malades et doubles chez les 5 autres. Ils siégeaient au niveau du foie droit (47 kystes) et le foie gauche (19 kystes). Une conversion était nécessaire chez 10 malades (16.4 %) dont 8 avait un kyste postérieur. Le traitement coelioscopique a consisté en une ponction vidange du kyste avec résection du dôme saillant (54 kystes), périkystectomie (2 kystes). Chez les malades qui ont eu une conversion, il a été réalisé une résection du dôme saillant (8 kystes) et une périkystectomie (2 kystes). Onze malades ont eu une cholécystectomie. Des complications post-opératoires sont survenues dans 22 % des cas. La mortalité était nulle. Le séjour post-opératoire était inférieur à 10 jours chez 49 malades (80 %). Avec un recul moyen de 7 mois (extrêmes 3 et 28 mois), un seul cas de kyste résiduel, passé inaperçu initialement, a été détecté. Conclusions: Les résultats préliminaires du traitement coelioscopique du kyste hydatique du foie sont satisfaisants.
L’échec de cette voie est du essentiellement aux localisations kystiques postérieures. Les résultats à distance méritent un suivi plus long.
19. Measuring academic productivity in a division of general surgery
Measuring the academic productivity of an academic division is an inexact science. We developed an academic productivity index to measure the academic productivity of our division of general surgery over a 10-year period. All the papers of division members were identified in a “PubMed” search. Each paper was assigned a score based on the “journal impact factor” multiplied by an author score (maximum 100 points) calculated as follows: single author, 100 points; 2 authors, 50 points each; 3 or more authors, first and last author 40 points each and intermediate authors split 20 points. Articles that were marked as “review” were multiplied by 0.5, and papers without abstracts (editorials, letters, etc.) were multiplied by 0.25. The gross academic productivity per year (GAP) was calculated by adding the scores of all the papers in that year and the academic productivity index (API) was determined by dividing the gross academic productivity by the number of division members.
| Year | Staff, no. | Papers, no. | Papers/staff | GAP | API |
|---|---|---|---|---|---|
| 1995 | 11 | 13 | 1.2 | 710.6 | 64.60 |
| 1996 | 11 | 20 | 1.8 | 408.4 | 37.12 |
| 1997 | 11 | 7 | 0.6 | 346.3 | 31.48 |
| 1998 | 12 | 11 | 0.9 | 260.1 | 21.67 |
| 1999 | 12 | 21 | 1.7 | 772.6 | 64.38 |
| 2000 | 12 | 27 | 2.2 | 964.9 | 80.40 |
| 2001 | 13 | 17 | 1.3 | 874.3 | 67.25 |
| 2002 | 15 | 22 | 1.5 | 561.9 | 37.46 |
| 2003 | 14 | 29 | 2.1 | 756.8 | 54.05 |
| 2004 | 15 | 49 | 3.3 | 1802.2 | 120.15 |
API = academic productivity index; GAP = gross academic productivity per year.
With the exception of 2004, academic productivity as measured by the API did not increase over the decade it was measured.
20. Construct and external validation of LapSim summary metrics
To assess construct validity and external validity for LapSim summary metrics.
In a previous study, 3 groups (expert laparoscopists, junior residents, medical students) underwent testing on the LapSim grasping, cutting and clipping tasks. Using the metrics generated by the software, formulae for efficiency (time–error) and economy of motion (motion) were developed to maximize differences between groups. The purpose of this study was to prospectively validate these summary metrics.
Eighty-two subjects were tested at an outside institution and time–error and motion scores were calculated. Construct validity was assessed by comparing expert (n = 15) with novice (n = 67) scores. External validity was evaluated by comparing these scores with 24 subjects previously tested at our institution, stratified by level of training. Data (mean ± SD) were evaluated by t test (*p < 0.05).
| LapSim metrics; task, mean (and SD) score | ||||||
|---|---|---|---|---|---|---|
| Time–error | Motion | |||||
| Group | Grasping | Cutting | Clipping | Grasping | Cutting | Clipping |
| Novice | 91 (31) | 47 (22) | 25 (35) | 594 (342) | 981 (312) | 532 (562) |
| Expert | 108 (29)* | 58 (16)* | 47 (30)* | 723 (321) | 809 (425) | 839 (489)* |
For the time–error score, experts had higher scores in all 3 tasks. For the motion score, experts only had higher scores in the clipping task (see Table). There were no significant differences in scores between the 2 institutions except for motion analysis of the clipping task (data not shown).
These prospective data provide evidence for construct and external validity of the LapSim summary metrics. The summary metrics rewarding speed and precision were better at discriminating between level of surgical experience compared with the motion score.
21. Learning styles in general surgery
A survey of general surgery residents and faculty was conducted to determine whether the learning styles of these 2 groups differ and if there are any such differences between residency levels.
An established and validated Kolb learning style inventory was administered to the general surgery residents and faculty within the general surgery residency training program at the University of Alberta. The surveys were conducted via email, and data were collected and analyzed for each participant’s learning style.
The predominant learning style identified in both groups was convergent, with greater than 60% of resident respondents and greater than 50% of faculty respondents identifying this as their learning style. More than 85% of both groups were identified as either convergent or accommodative learners. There were no significant differences in learning styles between the faculty and residents, nor between residency levels.
We conclude that there are no significant differences between the learning styles of general surgery residents and faculty. The predominant learning styles of general surgery residents and faculty are convergent and accommodative.
22. Resident attitudes towards script concordance testing
Script concordance tests (SCTs) designed to assess the intraoperative decision-making skills of general surgery residents have not been studied previously. We therefore created a 100-question SCT to measure the intraoperative decision-making skills of general surgery residents. To determine the attitude of residents toward this new style of examination, a post-SCT survey was conducted.
Thirty-six residents at a Canadian university wrote the SCT. All were surveyed regarding their opinion of the SCT, and 20 returned a completed questionnaire. Only 1 resident had previous exposure to an SCT. Fifteen (75%) felt that the SCT did test their intraoperative decision-making skills, while 1 resident felt that it did not test these skills. Fourteen (70%) of respondents rated the test difficult or very difficult. Only 40% of residents found the format of the SCT easy to understand. The majority (70%) of respondents felt the format was easier to understand as more questions were answered. Forty-five percent thought that the SCT was more difficult than an oral exam; 35% thought that the SCT was easier than an oral exam. In general, 55% would prefer to take an oral exam.
Residents agree that SCTs can be designed to assess intraoperative decision-making skills. Due to a lack of previous exposure, most residents have difficulty with the format of the exam. As residents gain experience by answering more questions, however, these difficulties are reduced. The lack of experience with SCTs may have a negative influence on residents’ attitudes toward SCTs.
23. Minimally invasive surgery in community hospitals: a single centre’s experience from 1999 to 2004 in establishing an advanced MIS program
The objective of this study is to describe the stages involved in establishing successful minimally invasive surgery (MIS) programs in community hospitals.
Over a 6-year period, we observed the transformation of the smallest surgical program in Nova Scotia into the first fully equipped MIS centre in Atlantic Canada, offering advanced procedures usually performed in university centres.
We described the following 4 phases: (I) pre-MIS (before 1999), (II) introduction of advanced MIS (1999–2000), (III) establishing advanced MIS (2000–2002) and (IV) innovation (2002–2004). One full-time surgeon and 2 locum surgeons were mainly performing open procedures in phase I. In phase II, executive decisions were made to establish a centre of excellence for MIS; a general surgeon with advanced laparoscopic skills was recruited; laparoscopic instruments were introduced during open cases; several basic MIS procedures were introduced; and 7 nurses were trained. In phase III (2000–2002), the program was successfully established with a single laparoscopic tower, 2 laparoscopic sets, 1 ligasure generator and the assistance of 2 surgeons from McGill University. Large bowel resection for benign and malignant diseases, anterior resection, abdomino-perineal resection (APR), lysis of adhesions, small bowel resection, inguinal hernia repair, ventral and incisional hernia repair, Nissen fundoplication, splenectomy, repair of perforated peptic ulcer, and repair of iatrogenic perforation of large bowel were some of the procedures introduced in phase III. During phase IV, we introduced innovative techniques to perform advanced MIS procedures without any surgical assistant.
We concluded that, with the right personnel, appropriate training, support from the administrators and the use of relatively inexpensive appropriate technology, advanced MIS procedures can be performed safely and effectively even in a community hospital with 1 surgeon.
24. Careers and lifestyles of women surgeons: a Canadian population study
A Web-based survey of Canadian women surgeons will be undertaken to evaluate if women surgeons are able to combine productive careers with rewarding family lives and if the ability to do so varies with the surgical specialty being practised.
The results of this study will be compared with a similar study carried out in 1993 to see how career and lifestyle characteristics of women surgeons have changed over the past decade. The study population includes women surgeons in the surgical specialties of cardiovascular and thoracic surgery, general surgery, obstetrics and gynecology, ophthalmology, orthopedic surgery, otolaryngology, neurosurgery, plastic surgery and urology. The questions cover the following areas: demographics, surgical training, current professional activities (including academic rank and tenure), childbearing experiences and household or child-rearing responsibilities, satisfaction with career and home life, and personal experiences with sexual discrimination and sexual harassment. Results and conclusions are pending.
25. Exploration of a physician report card for quality improvement in breast cancer
Individual surgeon performance across multiple measures of breast cancer treatment was determined and allowed for exploration of outlier definitions, a physician report card and provincial quality improvement strategies.
A population-based cohort of Manitoban woman diagnosed with breast cancer from 1995 to 2001 was used. The provincial cancer registry provided demographic, tumour and treatment information. Medical claims data were used for provider information. The measures examined were based on the availability of a published Canadian clinical practice guideline and reliable data for evaluation. Selected were rates of breast conserving surgery, axillary assessment in invasive and noninvasive disease and the adequacy of axillary node dissection (AND). Low-volume surgeons (< 12 breast cancer surgeries/yr) were evaluated together, while the remaining high-volume surgeons were examined individually. A measure outlier was defined as a surgeon with a rate whose 95% confidence interval was outside the provincial average and/or outside guidelines. Provincial rates with low-volume surgeons or outliers excluded were calculated to inform on quality improvement strategies.
Forty-three surgeons treated 4094 women. The 22 low-volume surgeons performed 15.1% of procedures. Each measure showed a wide variation in individual surgeon rates. A clear outlier definition could not be found for axillary assessment. Low-volume surgeons were outliers in 2 of 3 of the remaining measures, while 10 (47.6%), 6 (28.6%) and 5 (23.8%) of high-volume surgeons were never, once and twice or more times identified as outliers. Except for axillary node dissection in noninvasive disease, exclusion of low-volume surgeons or outliers did not meaningfully affect provincial rates.
A physician report card for breast cancer surgery is challenging in both creation and interpretation. Quality improvement strategies in Manitoba need to focus on all surgeons, rather than just low-volume surgeons or outliers in order to make meaningful improvements in provincial breast cancer care.
26. Endoscopic sphincterotomy in the management of complications of liver hydatid disease
The aim of this study was to evaluate the effectiveness of endoscopic sphincterotomy for complications of liver hydatid disease.
Eleven patients underwent endoscopic treatment for complications of hepatic hydatid disease. Indications for endoscopic retrograde cholangiography (ERCP) were: obstructive jaundice (1 case) and postoperative persistent external biliary fistula (10 cases). All patients were treated with albendazole, 400 mg daily, for 3 months. In the first patient, endoscopic retrograde cholangiography detected hydatid membranes in the common bile duct, and he underwent endoscopic sphincterotomy with no complications. The outcome was favourable. In 10 patients, closure of the biliary fistula was observed from 3 to 10 days after endoscopic sphincterotomy. During 15 months of followup, all patients remained asymptomatic.
Endoscopic sphincterotomy is safe and effective for the treatment of biliary complications of hepatic hydatid disease.
27. Conservative management of non-cecal diverticulitis found incidentally at laparotomy
The conservative management of patients found to have non-cecal diverticulitis at laparotomy for another suspected diagnosis is presented in a series of 13 patients accrued over the 5-year period from 1998 to 2002 at 2 separate institutions. The Hinchey classification system was used to grade all cases. Of the 13 cases, 11 were class I, 1 was class II and 1 was class III. Aside from 1 case of transverse diverticulitis, all cases involved the sigmoid colon. The average age of patients was 48.4 with a range of 36–80. All cases were treated with antibiotics following surgery and avoided both a resection and a stoma. Primary end points included resolution of acute symptoms and successful discharge from hospital. None of the patients required another operation in the acute setting. Although follow-up is ongoing, 5 of 13 (38.5%) patients required elective resections for recurrence of symptoms. This study suggests that it is safe to treat mild to moderate cases of acute diverticulitis discovered unexpectedly at laparotomy with conservative measures. Given the high rate of recurrent symptoms, it also raises the controversy of whether or not it would be prudent to resect the diseased segment at the time of the first OR.
28. Laparoscopic wedge gastrectomy esophageal lengthening procedure: clinical and physiological followup
Various methods of Collis gastroplasty have been described to lengthen the esophagus. In this series of 8 patients, we describe early outcomes following a laparoscopic wedge gastrectomy (LWG) esophageal lengthening procedure.
Between January 2004 and August 2004, patients with PEH were assessed preoperatively with GERD symptom scores, upper endoscopy, barium swallow, 24-hour pH monitoring and esophageal manometry. Intraoperatively, after reduction of the PEH and mobilization of the esophagus, patients with less than 2 cm of intraabdominal esophagus underwent LWG. A 52 French bougie was advanced, and the wedge gastrectomy was performed using a 45-mm ENDO GIA linear-cutting stapler. A loose fundoplication was then performed.
Eight patients (5M:3F) with a mean age of 66.9 ± 11.6 years underwent LWG. Six patients (75%) had a PEH (5 type III, 1 type IV); 2 patients (25%) had previously failed fundoplications. Mean OR time was 188.1 ± 51.9 minutes. Mean LOS was 3.9 ± 2.0 days. Mean time to start of oral diet was 1.25 ± 0.7 days. All patients had a gastrograffin swallow on POD one. All were normal except one, which showed a narrowing at the level of the diaphragm. The only minor complication was postoperative dysphagia in this same patient. This resolved without dilatation. There were no major complications. Follow-up upper endoscopy at 6 months revealed 1 patient’s wrap was partially undone. Another patient had a loose wrap with a hiatal hernia. Only 1 patient required postoperative antacid medication. Comparison of pre- and postoperative investigations revealed the following:
| Investigation | Time; mean (and SD) value | p | |
|---|---|---|---|
| Preop | 6 mo postop | ||
| GERD symptom score off meds | 27.25 (5.53) | 13.60 (6.63) | 0.0742 |
| 24-h pH | 4.45 (2.39) | 4.16 (1.68) | 0.4621 |
GERD = gastroesophageal reflux disease; meds = medications; postop = postoperative; preop = preoperative.
LWG esophageal lengthening procedure is a safe technique for dealing with a shortened esophagus. Larger studies with longer follow-up are still needed.
29. Laparoscopic surgery for colorectal cancer: a systematic review
Colorectal cancer is the second leading cause of cancer-related death in western countries. Surgeons have been reluctant to embrace laparoscopic techniques in colorectal cancer mainly due to concerns of inferiority. The objective of this systematic review is to show non-inferiority of laparoscopic-assisted colorectal resection for colorectal cancer compared with open colectomy.
A very comprehensive review of literature was performed using standard searching techniques for available literature on the topic. The following inclusion criteria were therefore used to select studies for inclusion into the overview: adults over 16 years of age with colorectal resection for documented colorectal cancer; randomized controlled trials with patients’ resections done either laparoscopic-assisted or open. We excluded studies that did not have the outcome of recurrence of colorectal cancer documented in their article. Data extraction and study quality were assessed, and finally data analysis was performed in a quantitative matter.
We identified 6 published and 4 not yet published studies that fulfill our inclusion criteria. The total number of patients between the studies was 1262. The methodologic quality was presented in its transparency. All primary and secondary outcomes showed good homogeneity except for morbidity, which was described heterogeneously between the studies. We can clearly see that there was no disadvantage to laparoscopic colorectal resection in any of these primary and secondary outcomes compared with the conventional open technique.
The results of this study suggest that although the definitive answer is not clear, the overwhelming evidence presently indicates that laparoscopic colorectal cancer resection is as safe and efficacious as the conventional open technique.
30. Diverticulitis: Do you know what causes it to be severe?
The causes of acquired diverticular disease of the colon are incompletely understood. In patients who become symptomatic, even less is known about factors relating to the severity of their illness.
This review endeavours to determine if differences exist between patients with mild and complicated diverticulitis.
A single teaching hospital experience with diverticular disease was reviewed: 281 admissions involving 261 individuals with acute diverticulitis from 1991 to 1997 were reviewed. Patients were divided into 2 groups according to severity of their illnesses. The “uncomplicated” group comprised 152 patients with acute diverticulitis. They required only conservative management. The “complicated” group comprised 109 patients in whom acute diverticulitis was associated with local or remote abscess formation, purulent or fecal peritonitis, colon fistulas or complete large bowel obstruction. Current medication exposures and medical conditions were identified for purposes of comparison between the groups. The Charlson index was calculated for each patient and was used as global measure of comorbidity. Logistic regression (SAS, 9.1 NC) was used to analyze the data.
There did not appear to be any difference in sex distribution. Patients admitted with complicated disease were older as determined by a mean of 63.7 (12.8) versus 58.1 (15.3) years for patients with uncomplicated diverticulitis (p = 0.002). Complicated patients were less likely to have a history of previous treatment for acute diverticulitis but were more likely to be on NSAIDs and to have a higher Charlson comorbidity index score. Patients with a history of chronic pulmonary disease and end-stage renal disease were associated with “complicated” diverticulitis.
Complicated diverticulitis was often seen in individuals already compromised by other major illness and by patients that were on NSAIDs. Previous episode of diverticulitis is a strong protective factor against severe diverticulitis.
31. Withdrawn
32. Laparoscopic donor nephrectomy: the pediatric recipient in a dual-site program
The purpose of this study was to evaluate the safety of a dual-site pediatric renal transplantation program by comparing the outcomes of pediatric recipients of laparoscopic donor nephrectomy (LDN) versus open donor nephrectomy (ODN).
This is a retrospective study of consecutive pediatric recipients (n = 9) of LDN between June 2002 and June 2004. This group was compared with the 9 most recent pediatric recipients of ODN (March 2001 to July 2004). Renal function was assessed with calculated creatinine clearance (Schwartz formula). Graft complications were recorded. Data are expressed as medians (range) or absolute number (percentage) and were analyzed using Mann–Whitney U test and Fisher’s exact test, respectively.
When comparing the laparoscopic versus open group, there were no significant differences in recipient age (10 [2–16] v. 9 [2–17] yr, p = 0.8), height (1.30 [0.85–1.90] v. 1.35 [0.81–1.73] m, p = 0.7), weight (30.6 [12.2–60.0] v. 33.0 [13.0–59.1] kg, p = 0.6), preoperative calculated creatinine clearance (10.1 [6.1–37.7] v. 10.1 [9.2–18.4] mL/min/1.73m2, p = 0.8) and warm ischemia time (50 [35–59] v. 38 [27–98] min, p = 0.06). There were 2 grafts with multiple arteries in each group. Differences in graft complications were not significant (see Table). Six-month postoperative calculated creatinine clearance was higher in the laparoscopic group (103.5 [87.2–122.2] v. 77.4 [30.7–85.5] mL/min/1.73m2, p < 0.001).
A dual-site laparoscopic donor nephrectomy program is not associated with adverse pediatric recipient outcomes when compared with a same-site open donor approach.
| Group | Graft complication; no. (and %) | |||
|---|---|---|---|---|
| Delayed graft function | Acute rejection | Graft failure | Ureteral complications | |
| Laparoscopic | 0 (0) | 2 (22) | 0 (0) | 2 (22) |
| Open | 1 (11) | 4 (44) | 0 (0) | 3 (33) |
| p value | 1.0 | 0.6 | 1.0 | 0.6 |
33. Margin status following breast-conserving surgery for ductal carcinoma in situ
Margin status is considered one of the most important factors in determining the risk of local recurrence following breast-conserving surgery (BCS) for ductal carcinoma in situ (DCIS). The optimal margin for local control is controversial with suggested standards ranging from microscopically negative to > 2 mm. Reported rates of positive margins range from 36% to 64% when the > 2-mm standard is employed. Routine intraoperative margin assessment has been demonstrated to reduce the need for reoperation by up to 50%.
The purpose of this study was to determine if routine intraoperative assessment of margins should be considered following BCS for DCIS in our own practice. The Manitoba Cancer Care Registry and an electronic medical record (OpTx) were used to retrospectively identify 111 women with DCIS seen at the Winnipeg Regional Health Authority Breast Health Centre in whom BCS was attempted between 2000 and 2004. Assessment of margin status intraoperatively was not routinely performed by any of the 10 surgeons involved.
Microscopically positive margins were found in 14 (12.6% ± 6%, 95% CI) patients. A further 28 (25.2% ± 8%, 95% CI) patients had 0- to 2-mm margins. Thus in our study 37.8% (± 9%, 95% CI) of patients had < 2-mm margins. As 10 of 14 (71%) patients with microscopically positive margins were re-excised, while only 13 of 28 (46%) with 0- to 2-mm margins were re-excised, the acceptable standard in our community appears to be microscopically negative margins.
The overall incidence of positive margins at our institution was lower than the rates published in most large institutional reviews. Assuming microscopically negative margins are acceptable, the benefit of routine intraoperative margin assessment by our surgeons does not appear warranted. Examination of recurrence rates may provide further insight into what is an acceptable margin.
34. Chest tube complications: How well are we training our residents?
The primary objective of this study was to define the incidence and risk factors for complications in chest tube thoracostomy performed exclusively by resident physicians. The secondary objective was to outline the rate of complications occult to post-insertional supine anteroposterior chest radiographs (AP CXRs).
All severely injured trauma patients (ISS ≥ 12) who underwent tube thoracostomy over a 12-month period at a regional trauma centre were retrospectively reviewed. Insertional, positional and infective complications were identified. Patients were assessed for complications based on resident operator characteristics, patient demographics, associated injuries and outcomes. Thoracoabdominal CT scans and corresponding CXRs were used to determine the rate of complications occult to post-insertional CXR.
Forty-four percent (338/761) of patients (99% blunt trauma) had CXR and CT imaging. Seventeen complications were present among 76 (22%) resident-placed chest tubes in 61 (28%) patients: 6 (35%) were insertional, 9 (53%) were positional and 2 (12%) were infective. Tube placement outside of the trauma bay (p = 0.049) and non-surgical resident operators (p = 0.03) were independently predictive of complications. The rate of complications according to training discipline were general surgery (7%), internal and family medicine (13%), other surgical disciplines (25%) and emergency medicine (40%). Resident seniority, time of day and other factors were not predictive. Six of 11 (55%) positional and intraparenchymal lung tube placements were occult to post-insertional supine AP CXR.
Chest tubes placed by resident physicians are commonly associated with complications that are not identified by post-insertional AP CXR. Thoracic CT is the only way to reliably identify this morbidity. The differential rate of complications according to resident specialty suggests that residents in non-general surgical training programs may benefit from more structured instruction and closer supervision in tube thoracostomy.
35. An intervention to improve do-not-resuscitate (DNR) orders in general surgery
There is increasing interest in the quality of care provided near the end of life. The timing and quality of DNR orders have been used as a marker of quality palliative care in other studies; generally, DNR orders were obtained poorly and too late for patients to advocate for themselves. We examined whether discussing DNR orders at weekly morbidity/mortality (M&M) rounds improved the quality and timing of DNR orders on a general surgery service. In July 2003, M&M rounds were altered to include a discussion of DNR orders. The charts of all patients who died in hospital while admitted to a general surgeon 1 year pre- and post-intervention were reviewed to collect data on admitting diagnosis, surgical procedure, cause of death, timing and wording of DNR, and who participated in the discussion.
One hundred and four of 128 deaths were reviewed. Pre-intervention, 51 of 61 (83.6%) had DNR orders, 29 (56.8%) within 1 day of death, and 11 (21.5%) of the discussions included patients; post-intervention, these were 33 of 42 (78.5%), 16 (48%) and 2 (6%), respectively. Of the patients admitted with a terminal illness, 20 (74.0%) and 7 (70.0%) had a DNR order written before death, on average 5 and 4 days before death, and only 4 (14.8%) and 2 (20.0%) involved the patient in the discussion, pre- and post-intervention, respectively. There were no significant differences pre- and post-intervention.
DNR orders were obtained late, and few discussions included the patient. A discussion of DNR orders at M&M rounds did not improve the timing or patient involvement in the DNR discussion. However, these data demonstrate the need for additional work to improve quality and timing of DNR discussions.
36. Incidence and outcomes of Clostridium difficile colitis in solid organ transplant recipients
At present, Clostridium difficile colitis (CDC) is a common nosocomial infection in hospitals in the province of Québec. Limited data exist about the incidence and outcomes of CDC in solid organ transplant patients. Patients with CDC after solid organ transplants were identified from a prospective transplant database. From March 1999 to March 2003, 714 patients were transplanted: 322 kidney (K), 244 liver (L), 50 pancreas (P), 71 heart (H), 20 kidney–pancreas (KP), 2 kidney–heart (KH) and 5 kidney–liver (KL) allografts. The mean age was 48.6 years old and 66% were male. The overall incidence of CDC (positive stool toxin assay) was 14.1%. The yearly incidence of CDC has increased over the study period, in parallel to a pandemic in Québec (see Figure).
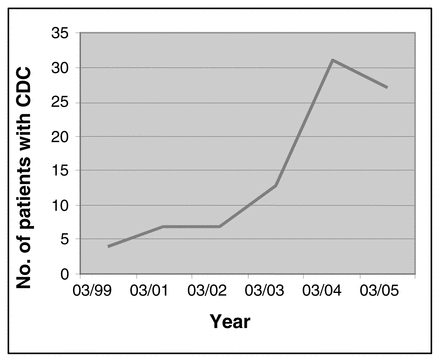
Forty-three patients were diagnosed with CDC within the perioperative period (30 d) and 6 patients within 2 months of transplantation. The all-cause mortality associated with CDC was 13%. The incidence of complicated CDC (defined as requiring colectomy or associated with graft loss) was 9%. The majority of complicated CDC occurred in the perioperative period. Among these, 5 patients underwent subtotal colectomy for complicated CDC, all of whom survived, and there was 1 graft failure. CDC is a serious and growing complication in solid organ transplant recipients. The aggressive management of CDC presenting in the post-transplant period, particularly early subtotal colectomy can be associated with improved outcomes.
37. What is the evidence base for the management of inguinal hernia?
To better understand the evidence base for the management of adults with inguinal hernias, we systematically searched MEDLINE, EMBASE and Cochrane Reviews for the 10-year period 1995–2004 for reports of prospective studies.
One thousand and three unique citations were identified and their abstracts reviewed, yielding 219 reports of randomized clinical trials (RCTs) published in English or French in 63 journals. No journal contained more than 19 RCTs (9%), and 46 journals contained 3 or fewer reports. Two of the 5 most cited journals are oriented to anesthesiology and contained 24 RCTs; overall, 49 RCTs (22%) were reported in 12 anesthesiology journals. Ninety-eight RCTs (45%) evaluated the choice of operation in terms of clinical outcomes: in 65, the comparison was between laparoscopic and another repair. Six additional reports were economic analyses of RCTs involving laparoscopic repair. Forty-seven RCTs (22%) evaluated pain management (e.g., adjunctive local anesthesia, NSAIDs, music) and 31 (14%) anesthetic techniques. Questions of surgical technique (e.g., suture material) were addressed in 23 RCTs (11%) and perioperative care in 8 RCTs (4%), including 4 primarily pertaining to prevention of wound infection. No RCT evaluated expectant or non-surgical management or questions related to postoperative follow-up. Twenty-three systematic reviews were identified, with a similar distribution of topics.
Questions related to inguinal hernia repair are of enduring interest to surgeons, but the large number of RCTs and their disparate locations underscore the challenge of transferring this knowledge to clinical practice. Observational studies remain common. New RCTs may be being undertaken without full consideration of existing data. In addition, important questions in the management of inguinal hernia remain to be addressed.
38. Melanoma in the elderly: differences in primary site and depth adversely affect female outcomes
Women tend to present with more extremity melanomas and thinner primary lesions when compared with men. This translates into an overall survival advantage for women. That survival advantage is lost in the elderly population. This study looks for differences in presentation that could account for the altered outcome and alert physicians to a different pattern of presentation in elderly women.
Patients were identified from a database of sequential referrals to plastics and surgery through a multidisciplinary melanoma clinic. Age, sex, primary site, Breslow and Clark levels, TNM staging, therapy, follow-up and recurrence were all recorded. Two hundred and thirty-two patients with a mean age of 59.4 years were identified. Elderly was defined as being more than 1 standard deviation above that mean and included patients aged 75 and over. Mean follow-up was 24.9 months.
Males accounted for 60% of the reference and 59% of the elderly 75+ group (no difference). Men presented with deeper lesions overall but this was only significant in the under 75 group. The 75 and over female population had thicker melanomas (4.0 mm v. 2.3 mm), more T4 (30% v. 8.2%, p = 0.025), fewer T1 melanomas (6% v. 26%, p = 0.050), fewer extremity primaries (29% v. 8.2%, p = 0.005) and more recurrences (47% v. 14%, p = 0.050) when compared with the younger cohort. No such differences were demonstrated between the elderly and reference male population.
Elderly women tend to present with thicker, non-extremity melanomas. Their presentation and recurrence rates are significantly different from younger women and resemble the patterns seen in men.
39. Laparoscopic adrenalectomy, a safe and effective therapy for the management of pheochromocytoma: a review of 20 cases
A retrospective cohort study was conducted to determine if laparoscopic adrenalectomy (LA) was a safe and effective therapy for the management of pheochromocytoma, as compared with open adrenalectomy (OA). Comparison was also made between 2 α-blocker regimens, phenoxybenzamine (PB) versus competitive α blockers (CAB) (doxazosin, prazosin and terazosin), in terms of intraoperative blood pressure control. Pertinent data were collected on 28 resections for pheochromocytoma, between 1998 and 2005, from 26 patient charts. Perioperative outcomes of 20 LAs were compared with 8 OAs. Rates of intraoperative hypertensive episodes (SBP > 180 and/or DBP > 90) and hypotensive episodes (SBP < 100 and/or DBP < 60) were compared between the PB (n = 20) and CAB (n = 7) groups. Mean (± SD) length of postoperative stay was less in the LA group (3.1 [1.5] v. 6.3 [1.0] days, p < 0.01), as was mean (± SD) tumour size (4.8 [3.0] cm v. 7.3 [2.5] cm, p < 0.05). No statistically significant differences were found for operative time or rate of postoperative complications. There were no statistically significant differences in intraoperative hypertensive or hypotensive episodes between the α-blocker groups. There were no intraoperative complications related to extremes of blood pressure, and no perioperative mortalities occurred in either group.
In conclusion, laparoscopic adrenalectomy is a safe and effective therapy for the management of pheochromocytoma. Effective preoperative α blockade can be achieved with either phenoxybenzamine or competitive α-blocker regimens.
40. Waiting times and conversion rates in urgent laparoscopic cholecystectomy
The aim of this study was to assess the impact of waiting time on conversion-to-open rates in urgent laparoscopic cholecystectomy.
A retrospective review was performed for all patients receiving urgent laparoscopic cholecystectomy at one institution between January 2001 and April 2003. Operating room booking forms and patient records were reviewed to determine time of presentation to the emergency department, time of booking for surgery and the time that surgery commenced. Only patients undergoing laparoscopic cholecystectomy as the primary procedure were included in the study. Patients with incomplete booking times were excluded.
Complete waiting time data were available for 156 patients. Sixteen required conversion to an open procedure (10.3%). The majority of patients requiring urgent laparoscopic cholecystectomy (146/156) were designated as requiring surgery within the next 24 hours. Half of all study patients did not meet this objective. Mean waiting time from booking for surgery to initiation of surgery was 37.5 hours in patients who were converted to open versus 27.8 hours for patients who were not converted to open (p = 0.11). For patients diagnosed with acute cholecystitis, mean waiting time from emergency department presentation to booking for OR was 28.03 hours. Waiting time was not related to duration of surgery or postoperative length of stay.
Patients wait longer than expected for urgent laparoscopic cholecystectomy. We were unable to demonstrate a statistically significant impact on conversion rates.
41. Province-wide survey of appendicitis in Québec. New twists to an old disease
This study, sponsored and conducted by Le Collège des Médecins du Québec, audited the management of acute appendicitis in Québec during 1 year (April 2002–March 2003). A questionnaire was sent to the Health Records Department of all hospitals treating appendicitis in the province. Data from 85 (100%) hospitals were received and reviewed.
During the study period, 7599 appendectomies were performed and 5707 (75%) were selected for study (55% men). The rate of normal and perforated appendix was 5.4% and 15.9%, respectively. Median hospital stay for simple and perforated appendicitis was 2.6 and 5.8 days, respectively. At least 1 imaging procedure was done in 86% of cases (54% CT scans, 55% ultrasounds).
Antibiotics were not given in 7% of cases and in 8% of patients with a perforation. Seventeen percent of patients did not receive preoperative or intraoperative doses, and, postoperatively, 58% of patients received unnecessary doses.
Laparoscopy was used in 35% of cases and was associated with a reduction in postoperative stay for simple (2.6 v. 2.9 d, p < 0.001) and perforated appendicitis (5.4 v. 5.9 d, p = 0.004). A low rate of laparoscopy (< 20%) was found in 66% of teaching and 37% of non-teaching institutions. Conversion to open surgery was necessary in 9.7% of simple appendicitis and 29.3% of perforated ones (p < 0.001).
Although results of this survey compare with similar published series, a few concerns emerge. Many have to do with noncompliance with recommended antibiotic usage for acute appendicitis. Although laparoscopy seems to be slowly making its way into the surgical armamentarium, the low rate of laparoscopic appendectomies in teaching hospitals raises the issue of appropriate resident training.
42. Intraoperative laparoscopic skills assessment: direct observation versus blinded video rating
A reliable and valid global operative assessment of laparoscopic skill (GOALS) has been developed for direct evaluation of intraoperative technical skill. Direct observation, however, may be biased. The purpose of this study was to investigate the reliability and validity of GOALS when applied to blinded, videotaped performances.
A global rating scale of 5 items (depth perception, bimanual dexterity, efficiency, tissue handling and autonomy) has previously been found to be reliable and valid for evaluation of laparoscopic skill by direct observation. Laparoscopic cholecystectomies performed by 5 novice (PGY 1 and 2) and 5 experienced (PGY 5 and attendings) surgeons were videotaped and evaluated by 2 direct observers during dissection of the gallbladder from the liver bed. Subsequently, 4 experienced laparoscopists (V1–V4) blindly evaluated the videotaped procedures using GOALS. Two of the video raters (V1, V3) had prior experience using GOALS in the operating room. The interrater reliabilities between video raters (VR) and between VRs and direct raters (DR) were calculated using the intraclass correlation coefficient (ICC). Construct validity was assessed using a 2-way ANOVA with Fisher post hoc analysis.
Interrater reliability for the 4 VRs (V1–V4) and the DRs (total GOALS score) was 0.72. The ICC for all 4 VRs was 0.68. The interrater reliabilities for VRs compared with DRs were 0.86, 0.39, 0.94 and 0.76, respectively, for raters V1–V4. All raters, except V2, differentiated between novice and experienced groups (p values ranged from 0.01 to 0.05).
These data suggest that GOALS can be used to assess laparoscopic skill based on videotaped performances, but that rater training may play an important role in ensuring the reliability and validity of the instrument. Experience using the tool in the operating room may improve the reliability of video rating and could be of value in training evaluators.
43. Is a formal data registry for the trauma unit in Cape Town, South Africa feasible?
The primary objective of this study was to assess the feasibility of creating a formal patient data registry for the trauma program at Groote Schuur Hospital (GSH) in Cape Town, South Africa. The secondary objective was to assess the program’s ability to maintain this database on a long-term basis.
GSH is a tertiary care trauma referral centre receiving approximating 12 000 cases per year (35% penetrating, 22% operative). This is among the largest experiences in the world. Records detailing all severely injured trauma patients presenting to GSH between 2003 and 2004 were included in a retrospective review. A formal economic analysis was also completed.
Three thousand seven hundred and fifteen severely injured patients were admitted to the GSH over the 12-month period. Forty-nine percent were victims of penetrating trauma. Based on a Canadian trauma program model with comparable overall volumes, the economic cost of creating a formal patient registry over the first year is $400 000. The cost of maintaining a registry approaches $370 000 annually. This includes computer hardware, registry software, database technicians and a resource manager. By minimizing redundancy and using cost-control methods, including lower labour costs, the creation of a trauma registry for $27 200 is feasible in South Africa. While software servicing and employee salaries represent significant long-term costs, this database could be maintained for $16 800 annually.
Trauma registries represent the standard measure of quality of care and the pre-eminent hypothesis-generating data source for innovative research. This is particularly important in critical care where acute treatment algorithms rely on large-scale patient outcomes and clinical experiences. While the cost of a trauma registry is significant, the tangible benefits to patient care are immeasurable. Furthermore, these costs can be reduced, and in some cases eliminated, in unique settings such as GSH. A formal GSH registry would prove invaluable to trauma care throughout the world.
44. Laser-enhanced digital imaging of gross breast specimens: an adjunct to margin assessment and quick confirmation of resected microcalcifications
Non-palpable breast lesions can often be mammographically detected by identifying a suspicious pattern of microcalcifications. During breast surgery, the intraoperative confirmation of these microcalcifications in the resected specimen and the real-time assessment of surgical margins are important but time-consuming endeavours. This study looks at enhancing the process with the use of laser light-induced specimen fluorescence, captured with digital imaging.
Breast surgery specimens were circumferentially inked and then cut longitudinally through the area of suspected abnormality. Prior to further processing, the cut surface was bathed in blue wavelength laser light for up to 30 seconds. A prolonged exposure digital image captured specimen fluorescence for immediate interpretation. A control photograph was taken in ambient light from the same camera position for comparison.
Paired photographs demonstrated non-visualization of microcalcifications in ambient light and readily apparent microcalcifications in laser-enhanced images. Fluorescence of connective tissue structures and small vessels improved the visualization of the entire specimen and facilitated surgical margin assessment around the areas of concern.
This method of digitally recording laser-induced specimen fluorescence provides immediate confirmation of the presence of microcalcifications in resected breast specimens and allows for improved gross assessment of surgical margins.
45. Neck masses referred to community general surgical practice
Neck masses are commonly seen in general surgical practice. The differential diagnosis varies depending on age, sex and anatomic location. We set out to assess the referral pattern of neck masses to community general surgical practice.
A retrospective chart review was performed on neck masses referred to 3 community general surgeons in Prince George over a 2-year period. Age, gender, location and diagnosis were assessed.
The records of 116 patients, ranging from 2 to 83 years (average 45 yr), were reviewed. Eighty-four (72.41%) were female and 32 (27.59%) were male. The thyroid was the most frequent site of neck mass (55.11%). This was followed by lymph nodes (15.13%), salivary (6.89%), congenital (6.03%) and other (3.45%). Non-malignant neck masses were present in 77.38% of females and 71.88% of males. Of these, thyroid adenomas were more common in females, whereas reactive lymph nodes were more common in males. Dividing patients by age, inflammatory masses were most common in the 0–15 year old age group (88.89%). Benign neoplasms were more common in the 16–40 and over 40 age groups (54.55% and 64.86%). But malignant masses increased in prevalence with age (> 25% in age > 16 yr). A higher percentage of neck masses found in the lateral position were malignant compared with those found in the central position (34.78% v. 16.36%, p < 0.05).
Neck masses are a common referral to general surgical practice. Non-malignant neck masses are more common than malignant neoplasms. However, increased age and lateral location should increase the surgeon’s suspicion for a malignant cause.
46. The timing of surgical management in acute colitis
In the absence of a clear indication for emergency surgery, the optimal timing for surgical management of acute colitis is not clearly defined. Acute colitis is initially managed conservatively with bowel rest, steroids and other pharmacologic intervention. Some physicians feel that if there is no significant clinical improvement within 5 days, operative intervention is indicated. Others feel that a 7- to 10-day course of medical management is warranted. This study compares the outcome of patients treated with early operative intervention versus those with late surgical intervention.
A retrospective chart review examining all cases of acute colitis from January 1995 to June 2003 was undertaken. Data regarding patient demographics, Truelove criteria, timing and indication for surgery, type of surgery, length of stay, complications and mortality were collected.
A total of 42 patients were identified. None of the patients died during the initial admission or in follow-up. Analysis of the Truelove scores revealed that all patients with a score of 2 or more after 7 days of conservative treatment required surgical management. Of those patients with a Truelove score of 3 or more at admission, 57% required surgical management during that admission and an additional 17% (total 74%) required surgery in the follow-up period.
A comparison of patients with early surgery (within 7 days of presentation) and those with late surgery (> 7 d) showed a higher postoperative complication rate in the early surgery group. However, 45% of the late surgery group developed further preoperative complications (perforation, toxic megacolon) while undergoing medical management. Hospital length of stay was longer for patients with late surgical intervention.
Truelove criteria can serve as an objective guide in determining the need for surgical intervention. This study does not show a clear advantage between early or late surgical intervention. A larger, prospective trial is necessary to determine the optimal timing of surgical intervention.
47. Clinical judgement remains of great value in the diagnosis of acute appendicitis
Observation and repeated examination may lead to favourable clinical outcomes in the ever-challenging diagnosis of appendicitis. The goal of this study was to evaluate the clinical performance of the diagnosis of suspected appendicitis in a centre with limited access to medical imaging technologies and to identify factors associated with complicated cases.
A retrospective review of the medical records of 211 consecutive surgical cases of suspected appendicitis, spanning an 11-year period, was performed. The delays before treatment and the subsequent patient outcomes were evaluated.
There were 8.1% of cases with negative appendicitis, 75.8% with non-complicated appendicitis, 12.3% with complicated appendicitis and 3.8% with other surgical conditions. The delay before the first medical consultation was significantly longer in patients with complicated appendicitis. The various delays after the first medical consultation were not significantly different between groups.
Based on the results of this study, in the context of limited medical imaging modalities available, observation was not associated with an increased incidence of complicated appendicitis. The presence of complicated appendicitis was associated with the delay before the patient’s first medical consultation. Clinical judgement can be prioritized and can lead to a good clinical performance in the management of patients with a suspected appendicitis with no significant increase in complicated appendicitis and negative appendectomy rates.
*Paper published in CJS.
48. Laparoscopic cannulation: development and validation of a new simulator task
A panel of experts identified 3 basic skills not addressed in the simulator component of the SAGES FLS (the Society of American Gastrointestinal and Endoscopic Surgeons’ Fundamentals of Laparoscopic Surgery) curriculum, one of which was cannulation. The purpose of this study was to create a cannulation task and to evaluate its reliability, validity and internal consistency.
Intravenous tubing with a premade defect is suspended in the endotrainer box. After viewing an instructional video, the operator is asked to introduce a cholangiogram catheter into the box, thread it into the tubing and then remove it. Scores are based on a cut-off time and normalized using the best performance of the sample. Participants (n = 38) at all levels of training were timed and videotaped (n = 34) during 2 iterations of the task by 1 of 2 examiners. Participants (n = 30) were also tested in the FLS tasks. Interrater reliability was assessed by having the other examiner score the taped performances (intraclass correlation coefficient [ICC]). Internal consistency was estimated using Cronbach’s α. Construct validity was evaluated by comparing novice (medical student–PGY2, n = 22) to experienced (PGY3–attending, n = 16) operators (t test). Cannulation scores were correlated with total FLS scores (manual component) to estimate concurrent validity.
The interrater reliability between examiners was 0.99 (ICC). Cronbach’s α with the addition of cannulation to the other tasks was 0.91 and did not improve with deletion of the new task. The mean score for novices was 37 (95% CI 24–50) and for experienced operators was 86.2 (80.5–91.9, p < 0.001). The correlation coefficient for the 30 participants who performed the other FLS tasks was 0.79 (p < 0.001).
This cannulation task meets the high standards established by the other components of the FLS system. It reflects an important skill that is not currently addressed and may be a valuable addition to the FLS program.
49. Minimally invasive surgical management in the setting of locally advanced colorectal cancer
Randomized trials have demonstrated the safety and efficacy of minimally invasive surgery (MIS) for colorectal cancer. The outcomes of MIS in the setting of locally advanced disease (LAD) remain unclear. In this study we analyze patients with LAD in a prospective database from a centre specializing in MIS and compare results to historical, open outcomes.
Review of a prospective database identified 14 patients with T4 lesions. All patients received standard preoperative staging, including imaging (CT or US), and were not felt to have LAD. Seven of the patients with T4 lesions underwent MIS resections. Of these LAD MIS resections, 1 was an anastomotic recurrence with associated carcinomatosis, 3 developed a distant metastasis at 0, 8 and 12 months, and 3 showed no clinical evidence of recurrence during the follow-up period (mean 17, range 5.5–29 mo). Six had node-positive disease and 4 underwent mulitvisceral resection.
A literature review identified 42 studies of MIS for colorectal cancer with 3252 patients. There were 101 patients with LAD identified at surgery, of which 8 had completed MIS resections. In 8 studies of open surgery for LAD, en bloc resection resulted in 5-year survival of 22% (node positive) and 71% (node negative).
Accepted guidelines for LAD mandate en bloc resection of involved organs. There are no reports describing the feasibility and outcomes of MIS for locally advanced colorectal cancer. Data from a single centre seem to indicate that MIS outcomes for LAD are comparable to similar stage historical controls. Experienced MIS surgeons may consider selecting patients for MIS based on careful consideration of preoperative imaging and intraoperative findings using a low conversion threshold and maintaining oncologic principals. However, given the additional technical challenges and higher conversion rates for these patients, an MIS approach to locally advanced disease cannot be recommended at this time.
50. Role of FNAC in investigation of parotid lesions, relation revisited
Fine needle aspiration cytology (FNAC) is a quick, minimally invasive, low morbidity procedure that could aid in diagnosis of parotid lesions, thus allowing consideration of non-surgical management or preoperative planning. We were interested in the relative accuracy of FNAC in the diagnosis of pleomorphic adenomas and Warthin’s tumours.
Using the Saskatoon Health Region pathology database, we reviewed 190 cases of parotid gland FNAC with available histopathological follow-up between 1997 and 2005. The sensitivity, specificity and accuracy were determined with respect to final histopathological diagnosis for all specimens, and for pleomorphic adenomas and Warthin’s tumours.
Of the 190 cases examined, the histopathological diagnoses were: benign (n = 138), malignant (n = 52), Warthin’s tumours (n = 34) and pleomorphic adenomas (n = 72). On FNAC, 123 cases were benign, 32 were malignant, 26 were non-diagnostic, 9 indeterminate, 27 Warthin’s tumours and 67 were pleomorphic adenomas. Out of 67 FNAC diagnoses of pleomorphic adenoma, 4 were mistaken for cancer (5.9%). Comparing FNAC with histologic diagnoses, the results were:
| Points of comparison, % | Overall | Pleomorphic | Warthin’s |
|---|---|---|---|
| Sensitivity | 61 | 89 | 78 |
| Specificity | 94.5 | 92 | 96 |
| Accuracy | 85 | 95 | 96 |
| False-negatives | 10 | 10 | 4.6 |
| False-positives | 4.5 | 7.9 | 4.6 |
While the overall sensitivity of FNAC for malignant tumours was low, the sensitivity and specificity for pleomorphic adenomas and Warthin’s tumours was quite high. In the appropriate clinical setting, this could allow for conservative management with close follow-up. However, one should be cautious when interpreting FNAC results other than pleomorphic adenoma or Warthin’s tumour and consider the complete clinical situation in further management.
51. Peri- and preoperative use of adhesive skin expanders can facilitate resection and improve cosmesis in the management of selected cutaneous malignancies
Resections of primary and recurrent cutaneously based malignancies require wide excision of skin. Areas of the scalp, extremity and upper back often require reconstructive flaps or skin grafting for closure. Recurrences may occur in radiated fields that limit the mobility of surrounding skin for flap construction.
Superficially applied adhesive skin expanders have been successfully employed to close granulating wounds after extensive debridement or fasciotomy. This study applies the same principle of gradual skin advancement to the preoperative setting to facilitate the closure of later planned resections.
Seven primary or recurrent cutaneously based malignancies are described, including scalp, chest wall, upper back, lower leg, calf and elbow locations. All had application of adhesive skin expanders in the pre- and perioperative setting. Wide excisions were all completed without skin graft or flap construction, with good cosmesis. Photo documentation of the technique and results are included in the poster.
Pre- and perioperative use of adhesive skin expanders facilitate the wide excision and primary closure of primary and recurrent cutaneous based malignancies in selected difficult cases.
52. “First, do no harm” — monitoring outcomes during the transition from open to laparoscopic live-donor nephrectomy
This study was undertaken to validate the multidisciplinary and dedicated-team approach to the introduction of laparoscopic live-donor nephrectomy (LLDN) by comparing donor and recipient outcomes during the transition from open to LLDN.
Seventy-five donor nephrectomies were performed for adult recipients between January 1998 and November 2003. Open nephrectomy (n = 31) was performed between January 1998 and November 2003, while LLDN (n = 44) was performed from December 2000 to November 2003. Data were collected prospectively, with supplemental retrospective chart review. Donor outcomes and recipient graft function were compared in the 2 groups.
Fifty out of the 75 (67%) procedures were performed since the introduction of LLDN, with 44 of 50 (88%) done laparoscopically. All LLDN were left nephrectomies, compared with 63% in the open group. There were no conversions from LLDN to open. Donor age, gender, BMI and operating time were similar in the 2 groups. Multiple arteries were found in 27% of donors in each group. Intraoperative urine output was lower in the LLDN donors (2.3 ± 2.5 v. 3.6 ± 3.0 mL/kg/h, p = 0.06), and serum creatinine was higher in the LLDN donors on postoperative day one (122 ± 21 v. 105 ± 27 μmol/L, p < 0.01). Complications requiring intervention occurred in 1 LLDN donor (pulmonary edema) and in 5 open donors (bleeding requiring transfusion in 2, pulmonary edema in 2, and pneumonia). Median length of stay was shorter after LLDN (3 v. 6 d, p < 0.01). In the recipients, there were no differences in ureteral complications, incidence of delayed graft function, length of hospital stay, postoperative creatinine levels up to 1 year, acute rejection, or cumulative patient and graft survival between the 2 groups.
At our institution, a team approach has allowed for the safe introduction of LLDN. This has been associated with an increase in the number of cases performed and a decrease in donor hospital stay.
53. Anti-reflux surgery for GERD: a small area variation analysis
No recent epidemiologic study of gastresophageal reflux disease (GERD) has been performed. Our objective was to describe population trends in the use of anti-reflux surgery across Ontario and identify variations in the rate of GERD surgery in relation to geographic area.
We identified all 10 899 primary anti-reflux procedures performed on persons aged 18 years or older in Ontario, between 1991 and 2002, using the provincial administrative health databases. Anti-reflux procedure rates, standardized for age and sex, were measured for each of the 49 counties in Ontario. Small-area variation was quantified using 4 measures of variation: the extremal coefficient (EQ), a third quartile to first quartile ratio (Q3:Q1), the coefficient of variation (CV) and the systematic component of variance (SCV). Chi-square tests were performed to identify those counties significantly differing from the remainder of the province.
The provincial crude rate of anti-reflux procedures was 11.6 per 100 000 adults over the duration of the study. Annual rates were relatively stable over the 10-year period; however, there appears to be a recent trend upward. Patients between the ages of 45 and 64 had the highest rates of surgery. Women underwent anti-reflux surgery more frequently than men (13.6 v. 9.4 per 100 000). Adjusted surgical rates by county ranged from 5.0 to 28.7 per 100 000 persons. The EQ, Q3:Q1, CV and SCV were 5.7, 1.8, 52.1 and 175.8, respectively.
Significant regional variation exists for anti-reflux surgery across Ontario, suggesting that anti-reflux surgery is a highly “discretionary” procedure. Therapeutic preference and the widespread availability of proton pump inhibitors likely contribute to this variation.
54. Can the esophageal Doppler be used to guide fluid administration during pneumoperitoneum in pigs?
During laparoscopic live-donor nephrectomy, aggressive fluid hydration is recommended to prevent the decrease in renal blood flow associated with pneumoperitoneum (PP). However, overhydration can also be detrimental. The objective of this study was to assess the effectiveness of goal-directed fluid administration to maintain renal cortical perfusion (RCP) during PP in a porcine model.
Seven 35-kg pigs were studied for 30 minutes prior to, 80 minutes during and 60 minutes after release of 15 mm Hg CO2 PP. Measurements were taken of stroke volume (SV) and cardiac output (CO) using an esophageal Doppler probe, RCP using a laser Doppler probe placed on the right kidney, renal function by the fractional excretion of sodium (FeNa) and urine output every 10 minutes. During PP, intravenous boluses of NS 5 mL/kg were given as needed to maintain SV within 10% of baseline. Data are expressed as mean (SD). Statistical analysis was performed with ANOVA; p < 0.05 was considered significant.
Mean fluid administered was 364 (239) mL. The mean number of boluses administered was 2.4 per pig (range 0–5). Using this strategy during PP, mean RCP, SV, CO, urine output and FeNa were not significantly different from baseline.
| Measurement | Time; mean (and SD) value | ||
|---|---|---|---|
| Baseline | Pneumoperitoneum | Postpneumoperitoneum | |
| Cardiac output, L/min | 5.1 (1.4) | 4.8 (1.2) | 4.3 (1.3)* |
| Stroke volume, mL | 53 (14) | 50 (12) | 45 (12)* |
| Renal cortical perfusion, cc/100-g tissue | 41 (7) | 39 (7) | 45 (8)*† |
| Urine output, cc/kg/h | 1.4 (0.2) | 1.3 (0.5) | 1.1 (0.6) |
| Fractional excretion of sodium, % | 0.31 (0.24) | 0.13 (0.1) | 0.22 (0.24) |
SV-guided fluid administration prevented the decrease in RCP and urine output normally seen during pneumoperitoneum, without requiring the administration of large volumes of crystalloid.
55. Prevention of bleeding after islet transplantation — lessons learned from a multivariate analysis of 128 cases at a single institution
Islet transplantation is being offered increasingly as an alternative to insulin for selected patients with unstable type 1 diabetes. Percutaneous transhepatic portal access avoids a need for surgery but is associated with potential risk of intraperitoneal bleeding.
Between 1999 and 2005, we performed 128 percutaneous transhepatic islet transplants in 66 patients. We encountered severe post-transplant bleeding in 18 of 128 cases (14.1%). In univariate analysis, the risk of bleeding was associated with an increasing number of procedures (2nd and 3rd procedures with an odds ratio [OR] of 10.0 and 20.7, respectively), platelets count < 150 000 (OR 4.2), elevated portal pressure (OR 1.1 per mm Hg) and heparin dose exceeding 42 U/kg (OR 10.4). A multivariate analysis further confirmed the cumulative transplant procedure number (p < 0.001) and heparin dose ≥ 42 U/kg (p = 0.02) as independent risk factors for bleeding.
Effective mechanical sealing of the intrahepatic portal catheter tract with thrombostatic coils and tissue fibrin glue and omission of ASA pre-transplant completely prevented bleeding in all subsequent procedures (n = 22, p = 0.04).
We conclude that bleeding after percutaneous islet implantation is an avoidable complication with effective sealing of the intraparenchymal liver tract combined with judicious use of anticoagulation therapies.
56. Treatment of the primary tumour in patients with incurable stage IV colorectal cancer: a survey of general surgeons and medical oncologists
The objectives of this study were: (1) to determine whether clinical equipoise exists with respect to resecting the primary tumour electively in the setting of incurable stage IV CRC (colorectal cancer), (2) what physicians think the most important outcome would be for a randomized controlled trial (RCT) and (3) what the minimally clinically important difference (MCID) would be if the primary outcome were survival.
Two hundred and eighty academic general surgeons and medical oncologists across Canada were surveyed. The questionnaire was composed of (1) a vignette of a healthy patient with CRC and incurable liver metastases followed by questions about the best treatment for the patient in a variety of scenarios and (2) questions regarding the design of an RCT.
One hundred percent of the medical oncologists and 81% of the surgeons surveyed reported having seen more than 11 patients with CRC in the past 2 years. The first scenario was a man with incurable stage IV CRC with an asymptomatic mid-sigmoid tumour. Fifty-three percent of surgeons and 50% of oncologists said they would recommend/refer the patient for resection of the primary tumour. Ninety-one percent of surgeons and 83% of oncologists said they would consider offering such a patient the opportunity to participate in an RCT. The majority of surgeons and oncologists thought that 3–6 months would be the MCID, in median survival, which would justify a change in their current practice. Fifty percent of oncologists and 69% of surgeons thought quality of life should be the primary outcome for an RCT. Conversely, 50% of oncologists but only 16% of surgeons thought survival should be the primary outcome.
Clinical equipoise exists in the setting of whether to resect the primary tumour electively in incurable asymptomatic stage IV colorectal cancer. While an RCT may be difficult, it seems feasible.
57. Erythropoeitin can reduce the need for transfusion in anemic patients undergoing surgery for gastrointestinal-tract malignancy — a meta-analysis
To assess the effect of erythropoietin (EPO) on perioperative transfusions in anemic gastrointestinal tract cancer patients undergoing surgery.
Randomized clinical trials in which patients received perioperative EPO versus placebo or no treatment were identified using MEDLINE. Using RevMan (Version 4.2, Oxford, England, 2003), odds ratio (OR), risk reduction (RR) and number needed to treat (NNT) were calculated for the administration of EPO as it relates to transfusion of packed red blood cells. Anemia, in the studies, was defined as hemoglobin < 130 g/L.
Six trials were included in the analysis. A total of 152 patients received EPO, with 153 patients receiving placebo. Transfusions were received by 50 (32.3%) and 69 (45.1%) patients, respectively. This was a statistically significant difference (OR 0.58, 95% CI 0.36–0.93). Relative RR was 71% (95% CI 53%–96%). This yields an absolute RR of 12.2% (95% CI 1.34%–23.1%) and an NNT of 9 (95% CI 4.3–73).
The available evidence suggests perioperative administration of EPO reduces the likelihood of transfusion in anemic patients undergoing surgery for gastrointestinal-tract malignancies.
58. Protein carbonyls as a measure of oxidative stress in trauma patients
Trauma is the most common cause of oxidative stress. Carbonyls are products of oxidative protein degradation and may be early indices of oxidative stress.
The aim is to determine the relationship between changes in plasma and urine protein carbonyl levels and trauma severity.
A prospective study on 30 trauma patients evaluating serum and urine samples over 7 days was conducted. Plasma protein carbonyls were measured spectrophotometrically at wavelength of 370 nm using a modification of the calorimetric method described by Levine. Total protein concentration was measured against bovine serum albumin standards using bicin-choninic acid assay. Urine carbonyl precipitate was also measured using DNPH. The 2 main ISS groups (minor and major trauma) were equally matched in age and sex.
The average carbonyl content on admission was 0.87 ± 0.2 nmol carbonyl/mg total protein and 0.93 nmol/mg over the study period for minor trauma. In the major trauma group, mean carbonyl content on admission was 1.95 ± 0.38 nmol carbonyl/mg total protein and 1.86 nmol/mg over the study period. The individual peak carbonyl levels occurred at the time of hospital admission and on day 7. Day 7 levels were higher than admission levels in the 2 groups although more marked in severe trauma. The carbonyl content was significantly higher in major trauma than in minor throughout the study period (p < 0.001). The same trend was noticed on admission, and the difference between the 2 groups was also significant (p = 0.025). A positive correlation was observed between the presence of urine carbonyl precipitate and trauma severity (p = 0.000).
Protein degradation is an early effect of oxidative damage in trauma, and protein carbonyl levels could be used as to monitor patients. Protein carbonyl levels also correlate with trauma severity.
59. CAGS Basic Science Award: Fluid management strategies to maintain renal perfusion and function during pneumoperitoneum
Although pneumoperitoneum decreases renal blood flow, it remains unclear whether this impacts renal function. Our aim was to characterize the effects of pneumoperitoneum on renal perfusion and function and to evaluate 2 different strategies for fluid management.
Twelve 30-kg pigs were randomized into 2 groups: group 1: maintenance (3 cc/kg/h of NaCl) and group 2: bolus (15 cc/kg/h and a 20 cc/kg NaCl bolus before induction of pneumoperitoneum). Pigs were studied in a blinded fashion for 30 minutes prior to, 60 minutes during and 30 minutes after release of 15 mm Hg CO2 pneumoperitoneum. Renal cortical perfusion (RCP) was measured using a laser Doppler probe placed on the right kidney. Renal function was assessed using the fractional excretion of sodium (FeNa). Data are expressed as mean (and SD). Statistical analysis was done with ANOVA (*p < 0.05).
There were no differences between groups at baseline. Compared with baseline, RCP decreased in the maintenance group during and after release of pneumoperitoneum. This drop in RCP was not seen in the bolus group. No change in renal function (as measured by the FeNa) was noted in either group at any time.
Pneumoperitoneum of 15 mm Hg CO2 causes a decrease in renal blood flow but has no effect on renal function as measured by the FeNa. Administration of a fluid bolus reverses the hemodynamic effects of pneumoperitoneum on renal blood flow. Fluid administration may be an important factor to overcome the effects of pneumoperitoneum during laparoscopy in humans.
60. The role of ciprofloxacin in prolonging polyethylene biliary stent patency: a multicentre, double-blinded effectiveness study
Plastic stents are the mainstay of the palliation of malignant jaundice but are complicated by recurrent obstruction. Previous trials have failed to demonstrate any improvement in patency with the use of antibiotics. Patients with malignant jaundice were randomized in a double-blind fashion, after polyethylene stent insertion, to receive ciprofloxacin or placebo. After successful stent decompression, there were 50 patients in the treatment arm and 44 in the placebo. There were 14 (33%) episodes of stent occlusion in the ciprofloxacin group versus 23 (49%) in placebo (χ2 test, p = 0.115). There was no significant difference in patency (log-rank test, p = 0.17). There were significantly fewer episodes of cholangitis with ciprofloxacin: 10 (23%) versus 21 (42%) in the placebo (p = 0.047). The ciprofloxacin group also demonstrated a significant improvement in the Social Function domain of the SF-36 Quality of Life Survey at 1 month (paired t test, p = 0.03). The other domains of the SF-36 were not different, nor was survival (log-rank, p = 0.80). There is insufficient evidence to show that prophylactic ciprofloxacin can prolong plastic biliary stent patency. The observed trends suggest that ciprofloxacin significantly decreases the incidence of cholangitis and results in improvements in certain aspects of quality of life.
61. Natural history of choledocholithiasis in gallstone pancreatitis
Standard management of gallstone-associated acute pancreatitis calls for cholecystectomy with cholangiography to be performed during the same hospitalization after acute symptoms have subsided. No previous studies, however, have objectively addressed the usefulness of intraoperative cholangiography in management of these patients.
Our goal is to determine the incidence of common bile duct stones following an acute episode of gallstone pancreatitis.
Medical records of all patients who underwent a cholecystectomy and intraoperative cholangiography following an episode of gallstone pancreatitis on the same admission between 1999 and 2004 at University of Alberta and Royal Alexandra hospitals were examined to determine the incidence of common bile duct stones after resolution of gallstone pancreatitis.
A series of 86 patients’ charts were reviewed. Sixty-three patients met the inclusion criteria. All except for 1 patient underwent successful intraoperative cholangiography (98%). Among patients who had no evidence of CBD obstruction based on preoperative imaging and laboratory work, 3 patients were found to have filling defect on intraoperative cholangiography and stones on their postoperative ERCP 3/63 (5.0%). This is not significantly different than the 4.6% incidence of CBD stones in patients with cholelithiasis with normal preoperative imaging and blood work (p = 0.994).
In the setting of normal preoperative imaging and laboratory work, the incidence of CBD stones in patients recovering from acute mild–moderate gallstone pancreatitis is not significantly higher than the patients with no history of pancreatitis. Studies should be performed to assess whether routine cholangiography in gallstone pancreatitis changes patient outcome.
62. Fast-track advanced laparoscopic surgery in an ambulatory surgery centre. A 4-hour stay
This is a review of advanced laparoscopic procedures performed on an outpatient basis in the ambulatory campus of an academic health sciences centre. Charts and the follow-up call log by nursing were reviewed.
Over 3 years, 55 patients (71% male; median age 41, range 18–72 yr) underwent 50 Nissen fundoplication (NF) and 5 adrenalectomies (ADR). Selection criteria included absence of significant comorbidities and patients’ presence in town for 48 hours postoperatively. Comorbidities were present in 18 patients (32%), and 13% had previous upper abdominal surgery. Discharge criteria were based on hemodynamic stability, ability to ambulate and absence of nausea, pain or bleeding.
Median operative time was 85 minute (NF, 80 min; ADR, 140 min). There were 2 intraoperative complications (partial splenic infarction, bleeding). There was no mortality or conversion to open surgery.
The median postoperative stay was 4.5 hours (range 2.4–7.5). Two patients (3.6%) were transferred to an inpatient site for admission (see intraoperative complications above). Five patients (9%) visited the emergency department of the in-patient sites in the month following their surgery. Four needed admission (dysphagia, slipped Nissen, dehydration, pain). Readmission rate at 1 month was thus 11%. One patient (1.8%) needed remedial surgery for a slipped Nissen.
Data on the day-one nursing postoperative telephone follow-up was available for 50 patients (91%); 34 were successfully contacted. Twenty-four (70.5%) had no complaint. Symptoms reported were: pain (7), dysphagia (1), dysuria (1), sore throat (1), hiccup (1) and nausea (1).
Successful fast-track outpatient surgery for some advanced laparoscopic procedures is achievable. Precise selection and discharge criteria combined with appropriate follow-up should decrease readmission rate and patient discomfort.
63. The impact of the current epidemic of Clostridium difficile in Montréal on 2 general surgery units
Recently, the number of severe cases of C. difficile associated diarrhea (CDAD) has increased significantly in Montréal. We analyzed the impact of this epidemic on the gastrointestinal (GI) and hepatopancreatobiliairy (HPB) surgical services in our hospital. Data were collected in a prospective infection control surveillance program based on positive CD cytotoxin assay results. Cases were classified according to the clinical manifestations. CD rates were calculated per 4-week period and per medical and surgical services. In addition, from June 28 to October 11, 2004, the prevalence of CD colonization at admission and the incidence of CD acquisition during the hospital stay were established for all patients admitted to the GI and HPB services. From January 2004 to January 2005, there were 276 nosocomial cases of CD identified in the hospital: 88 (31.9%) asymptomatic carriers, 108 (39.1%) patients with diarrhea, 50 (18.1%) with colitis, 17 (6.2%) with pseudomembranous colitis, 4 (1.4%) with toxic colitis and 9 (3.3%) indeterminate. Complications included admission to ICU (8), deaths (40) including 4 attributed to CDAD. The global hospital rates per 4-week period for symptomatic cases varied from 6.4 to 39.1/1000 admissions (mean 16.4) and from 7.8 to 42.6/10 000 patient-days (mean 20.4): the annual rates were 18.3 and 44.6/1000 admissions and 17.3 and 37.2/10 000 patient-days for GI and HBP, respectively. The prevalence rate of CD colonization at admission was 4.6% (18 patients) and the incidence rate of CD colonization during hospitalization was 10.8% (35 patients). Hence, the nosocomial acquisition and transmission of CD appeared to be important factors in the development of CDAD in GI and HPB patients who, in our hospital, are at a significant higher risk for CDAD considering their pathologies, surgeries and adjuvant treatments.
64. Correlation of benign hyperplastic lesions found on ultrasound-guided needle biopsy with excisional biopsy specimens
This study correlates benign hyperplastic pathology (atypical ductal hyperplasia [ADH], papillary lesions, florid ductal hyperplasia and sclerosing adenosis) found on ultrasound-guided needle biopsy (USB) with pathology of excisional biopsy (EB) specimens. All USBs at the Cedar’s Breast Clinic between June 2003 and October 2004 (n = 534) were reviewed; cases with the above pathologies (n = 48) were investigated by chart review, examination of ultrasound images with a breast imaging radiologist, and review of biopsy slides with 2 pathologists. Twenty-three lesions underwent EB. Ten of 23 (43%) of lesions were in situ or invasive cancer: 5 of 12 ADH lesions were ductal carcinoma in situ (DCIS) and 2 of 12 were invasive cancer; 2 of 9 papillary lesions were DCIS and 1 of 9 was invasive cancer. No statistical difference between benign versus pre-malignant/malignant lesions on EB were observed with regard to both clinical parameters (age, family history, past breast cancer and history of hormone replacement therapy) and ultra-sonographic features (size, echogenicity, microcalifications, posterior acoustic properties, depth of lesion greater than width, irregular margins, Doppler signal and cystic component). The concordance among radiologist, pathologist and surgeon to recommend EB once USB pathology result was obtained was 11 of 23 (48%, 7/10 malignancies) in the lesions that were excised and 11 of 25 (44%) in lesions that did not undergo excision. On review of the USB pathology, 5 cases were upgraded, of which 2 warrant further investigation. After at least 6 months follow-up, 12 of 25 lesions that did not undergo EB had follow-up radiology studies: 3 cases were recommended to undergo further investigations. ADH and papillary lesions may carry a higher risk of associated pre-malignancy and malignancy than previously reported. Further verification of this finding is needed. The radiologist, pathologist and surgeon should confer to appropriately manage these high-risk lesions.
65. The role of advanced radiological imaging using the modified Alvarado Score in the investigation of patients with suspected appendicitis
Using a 7-item clinical checklist (modified Alvarado Score [MAS]) we determined the clinical value and accuracy of imaging in patients with possible appendicitis. We hypothesize that imaging will be of greater value in patients with equivocal presentation (low MAS).
A retrospective review of patients at 2 adult hospitals who underwent appendectomy over a 2-year period was undertaken. The MAS was assessed, and patients were separated into high-suspicion (MAS 7–9) and low suspicion (MAS 1–6) of appendicitis. Use of CT or US was noted, and the rates of negative appendectomy (NA) were determined through confirming pathological diagnosis. Statistical analysis was performed using SAS output with χ2 calculation.
Two hundred and twelve patients were included for analysis. The overall NA rate was 9.4%. One hundred and twenty-seven patients presented with a high clinical suspicion of appendicitis (MAS 7–9), 7 of which had an NA (5.51%). Eighty-five patients presented with equivocal findings of appendicitis (MAS 1–6), 13 of which had an NA (15.3%).
Patients in the high MAS group were imaged in 48.8% of cases. Of those imaged, 2 of 62 had an NA while in the unim-aged group there were 5 of 65 NAs. Imaging improved the positive predictive value (PPV) in the high MAS group from 92.3% to 96.7%, p = 0.69. In the low MAS group, 72.9% were imaged. Of those imaged, 6 of 62 had an NA. In the patients without imaging, 7 of 23 had an NA. Imaging improved the PPV from 69.6% to 93.1%, far more than the high MAS group, p = 0.005.
Our results suggest that radiological imaging significantly improves diagnostic accuracy in patients with an equivocal clinical presentation of appendicitis as represented by a low MAS. Diagnostic imaging did not significantly change the PPV of correctly diagnosing appendicitis in patients with a high MAS.
66. Shared general surgery call between 2 hospitals — Does delay of care increase complications?
Regionalization and manpower issues have led to the establishment of “shared call” (SC) between hospitals in Canada. Such a system was implemented within the Division of General Surgery in London, Ontario, between London Health Sciences Centre’s University Campus (LHSC-UC) and St. Joseph’s Health Centre (SJHC) in 2000. Under this system, patients requiring general surgery consultation may be assessed in one emergency department (SJHC) and transferred to another hospital for care (LHSC-UC).
We hypothesized that the SC system may produce delays that result in adverse outcomes.
A retrospective case–control study of appendectomy cases at LHSC-UC under the SC model from July 2002 to June 2004 was performed. End points studied included time from presentation to intervention (appendectomy), investigations performed, surgical pathology, morbidity and mortality.
One hundred and twenty-six cases were reviewed. Seventy-two LHSC-UC patients identified (control) were compared with 38 patients whose care originated at SJHC (case). Time to intervention appeared excessive in both groups and was longer in patients whose care originated at SJHC (961 min) compared with LHSC-UC (844 min). Due to the delay observed in both groups the difference detected was not statistically significant (p > 0.05). There was no difference in final pathology in LHSC-UC versus SJHC cases (normal 7% v. 3%, appendicitis 76% v. 84%, perforated 17% v. 13%), morbidity (8% v. 5% wound complications) nor mortality (none in either group). Rate of imaging for both groups was high 72% (UC) versus 55%. Delay to intervention appeared to be greater in patients who underwent imaging (738 min v. 958 min).
SC at LHSC-UC and SJHC does not appear to adversely affect the care of patients with appendicitis in London, Ontario. Further analysis is required to determine other factors (such as medical imaging) that may be producing excessive delay in intervention of appendicitis at our centre.
67. A population-based review of severe cyclist trauma in British Columbia
The popularity of cycling is increasing for recreation as well as a mode of transportation, with a corresponding increase in injuries. This population-based study analyzes the pattern and trends of severe injuries and deaths from cycling in British Columbia.
All cycling injuries captured by the British Columbia Trauma Registry (BCTR) over a 10-year period (1993–2003) were reviewed. Patients from the 3 most populated health regions of the province (approximately 3 million inhabitants), each with designated trauma centres contributing to the BCTR, formed the study cohort.
During the study period, 1476 cyclists sustained injury meeting BCTR criteria, annual incidence rate of 4.55 per 100 000. This represents 2.89% of the total trauma population admitted to these trauma centres (n = 51 150). The male to female ratio was 4:1. Mean age was 33.87 ± 17.49 years; 40% were between 25 and 40 years. Lone crashes made up 67.55% of those injured, compared with 30.70% versus a motor vehicle. Helmet use increased throughout the study period with a utilization rate rising to approximately 55% in injured cyclists by the end of the study. There was a corresponding drop in head injury rate during the study from 23% to 17%. Head injury and death were less common in cyclists wearing helmets than those who did not (14.89% v. 39.09%, p = 0.001). There were 40 deaths (mortality 2.71%), 80% were males, mean ISS was 39.51 ± 17.75, and mean TRISS was 0.456 ± 0.022. Head injuries and thoracic trauma were more common in non-survivors.
Cycling-related injuries continue to pose a small but significant public health concern. We recommend that prevention initiatives be broadened to include the adult population between 25 and 40 years old. Enforcement of mandatory helmet laws and education initiatives are needed to improve helmet utilization and decrease head injury morbidity and mortality.
68. Early removal of post-mastectomy drains is not beneficial: results from a halted randomized controlled trial
Drainage of mastectomy sites with closed suction drainage to avoid seromas is standard in the treatment of breast cancer. The optimal time to remove these drains has not been well defined. This study evaluates whether surgical drains can be removed on postoperative day 2 following mastectomy, without increasing the need for seroma treatment.
Women undergoing mastectomy for malignancy, with either sentinel lymph node biopsy or complete axillary dissection, were enrolled at a single site over a 4-month period. After mastectomy, patients were randomized to early drain removal 2 days postoperatively (early removal) or standard drain removal (< 30 cc drainage in 24 h or 2 wk postoperatively, whichever came first) (standard treatment). All medical contacts after discharge were recorded for a period of 1 month.
Twenty-seven of the anticipated 80 women were recruited before an interim analysis was mandated to address patient safety concerns expressed by enrolling physicians. Of these patients, 3 withdrew before completion of the trial. Of the remaining 24 patients, 14 had been randomized to the standard treatment group and 10 were in the early removal group. Patients in the standard treatment group had significantly fewer seroma aspirations (0 v. 2, p = 0.0004), fewer drain reinsertions (0 v. 5, p = 0.004) and fewer physician visits (1.5 v. 3, p = 0.004). These results demonstrate a significantly higher risk to patients in the early removal group and this trial was therefore stopped early due to concerns over patient safety.
Surgical drains cannot be safely removed on postoperative day 2 after mastectomy. Early removal significantly increases the occurrence of seromas requiring additional treatment.
69. CAGS Clinical Research Award: Stapled hemorrhoidopexy is associated with a higher long-term recurrence rate of internal hemorrhoids compared to conventional excisional hemorrhoid surgery: a meta-analysis
The purpose of this systematic review is to compare the long-term results of stapled hemorrhoidopexy (SH) with conventional excisional hemorrhoidectomy (CH) in patients with internal hemorrhoids.
A systematic review of randomized controlled trials (RCTs) comparing SH and CH with long-term results was performed. The EMBASE, MEDLINE and CENTRAL databases were searched for relevant trials. Included studies had a minimum follow-up of 6 months and compared circular stapled hemorrhoidopexy to excisional hemorrhoidectomy (Milligan–Morgan, Ferguson, diathermy and Hospital Leopold Bellan procedure). Studies were analyzed for clinical and statistical heterogeneity. Primary outcomes were hemorrhoid recurrence, hemorrhoid symptom recurrence, complications and pain. Trials were subdivided into studies with follow-up less than 1 year or those with follow-up of 1 year or more. A random effects model was used to calculate a meta-analysis.
Thirteen RCTs were included in the analysis. Follow-up ranged from 6 months to 4 years. The results show that patients who had SH are more likely to have long-term recurrence of hemorrhoids compared with CH at all time points (OR 3.85, 95% CI 1.47–10.07, p < 0.006) and in studies with follow-up of 1 year or more (OR 3.60, 95% CI 1.24–10.49, p < 0.02). SH results in more patients complaining of prolapse at all time points (OR 2.96, 95% CI 1.33–6.58, p < 0.008) and in studies with follow-up of 1 year or greater (OR 2.68, 95% CI 0.98–7.34, p < 0.05). Non-significant trends favouring CH are seen in the proportion of asymptomatic patients, bleeding, soiling/difficultly with hygiene/incontinence, the presence of perianal skin tags and the need for further surgery. Non-significant trends favouring SH are seen in pain, pruritis ani and symptoms of anal obstruction/stenosis.
Stapled hemorrhoidopexy is associated with a higher long-term recurrence rate of internal hemorrhoids compared with conventional excisional hemorrhoid surgery. More patients receiving SH complain of hemorrhoidal prolapse in long-term follow-up compared with CH.
70. Surgeon volume and technical factors influence positive margin rates after breast conservation surgery for early stage breast cancer
Positive surgical margins are a predictor of local recurrence after breast conservation surgery (BCS) in early stage breast cancer. Most early stage breast cancers are managed with BCS. However, few studies have examined the relationship between technical factors and margin status. Furthermore, while some studies have suggested a relationship between specialization and outcome in breast cancer, the relationship between surgeon volume and margin status has not yet been evaluated. The objectives of this study were to determine whether specific surgical factors and volume of breast cancer cases affect margin status.
The study was a retrospective, cohort analysis of 584 patients with clinical stage I or II breast cancer seen at a regional cancer centre from 2000 to 2002. Logistic regression was performed to determine the best independent predictors of positive margins. Factors with p < 0.1 were entered into the final model.
Thirty-eight percent of tumours were nonpalpable (NPT) and 62% were palpable (PT). Overall, 24.7% had positive margins. Ninety-eight percent of cases were performed under general anesthetic. In univariate analysis, performance at an academic (versus community) hospital, specimen radiography and use of a rigid versus flexible wire for needle localization were not significant. A confirmed preoperative diagnosis, specimen orientation labelling, cavity margin dissection, increased volume of surgical specimen and increased volume of surgeon cases (> 10 cases per year) were associated with clear margins in univariate analysis (p < 0.05). In logistic regression, multifocality (OR 9.74, 95% CI 2.74–34.61), increased tumour size (OR 3.15, 1.64–6.20), absence of cavity margins (OR 3.06, 1.22–7.65) and low-volume surgeon (OR 2.72, 1.12–6.21) were independent predictors of positive margins. Seventy-eight percent of surgeons were “low-volume,” and 38.4% of the cases were performed by “low-volume” surgeons.
This study has demonstrated that specific surgical factors are associated with the generation of positive margins after BCS of palpable and nonpalpable tumours in early stage breast cancer. Along with tumour factors (size and multifocality), low-volume surgeons and absence of cavity margin dissection were independent predictors of positive margins in this cohort of patients.
71. Feasibility and outcomes with cytoreduction surgery and hyperthermic intraperitoneal chemotherapy
Carcinomatosis of gastrointestinal (GI) origin is usually fatal within 6–8 months. Cytoreduction surgery and hyperthermic intraperitoneal chemotherapy (CS/HIPEC) with curative intent was undertaken to assess feasibility and short-term outcomes and to collect long-term recurrence and survival data.
Patients without distant metastases and good functional status were offered CS/HIPEC. If all macroscopic cancer was removed at laparotomy, hyperthermic (40–42°C) intraperitoneal mitomycin C (12–15 mg) was circulated for 1 hour via Coliseum technique. 5 Fluorouracil (5FU 1 g) was given on postoperative days 1–4. Short-term outcomes including tumour extent (peritoneal carcinomatosis index [PCI]) and resectability, operative times, transfusion rates, perioperative complications and in-hospital mortality were recorded. Standardized follow-up (fu) for recurrence and survival data are ongoing.
Twenty-seven patients with mean age of 47 (30–76) were treated. Primary GI pathology included cancers of the appendix (13), colon (6), primary peritoneal (5), terminal ileum (2) or mesothelioma (1). Tumour was extensive in the majority (85% had high PCI scores > 203) yet 81% (22/27) underwent complete cytoreduction (CCR). Median operating time was 396 minutes (133–509) and median transfusion requirements were 2 units (0–17). One patient died (3.7%) secondary to hemorrhage/DIC. Reoperative rate was 18% (5/27). Patients required ICU monitoring/intervention in one quarter (26%) of cases and median overall length of stay was 19 days (10–46).
Median fu for the group is limited at 8 months (1–55 mo), but 10 patients have had more than 24 months fu. Of 21 patients undergoing CCR, 1 died perioperatively, 3 died of recurrent disease, 3 are alive with recurrence and 14 are alive without recurrence. Of the 10 patients with more than 24 months fu, 50% remain alive without recurrence.
CS/HIPEC for carcinomatosis of GI tract origin is feasible. Furthermore, disease-free and overall survival data are promising for a disease with a previously limited survival time and supports the conclusion of the prospective RCT for colorectal carcinomatosis.
72. Institutional quality assurance and outcome evaluation for sentinel lymph node biopsy in melanoma patients
With the introduction of new technologies, institutional quality assurance (QA) and patient outcome evaluation (OE) become essential components of patient care. This study retrospectively evaluated these issues, using a newly developed melanoma database, for patients undergoing sentinel lymph node biopsy (SLNB) for primary cutaneous melanoma.
Patients with primary cutaneous melanoma having a SLNB at our institutions between January 1998 and December 2002 were identified from a review of our billing database. Their office charts were retrospectively reviewed and the pertinent data entered into an Access database. When necessary, further data were obtained from their Cancer Agency records.
There were 115 patients identified (62 male and 53 female), with a mean age of 51 years at diagnosis. Lesions were most commonly located on the extremities (52%) or trunk (43%), followed by the head and neck (6%). All patients were stage I or II (stage IA 2.6%, IB 41.7%, IIA 27%, IIB 18.3%, IIC 9.6%). The mean melanoma thickness was 2.49 mm (range 0.8–12 mm). The surgical technique involved both radionuclide and vital dye mapping in all cases, with standard hematoxylin and eosin staining of pathology specimens. More than 1 sentinel node (SN) was found in 23% of patients with an average of 1.5 SN per patient. Mean follow-up was 11 months (range 1–72). Our SN identification rate was 98%. The positive SLNB rate was 18%, and 20% of those patients had additional positive nodes found at the time of formal node dissection. There have been 4 local recurrences in our node negative group giving a false-negative rate (FNR) of 16.7%.
Our results generally concur with established oncology literature, though the FNR is slightly high and requires further evaluation. The database allowed easy access to the data needed for this analysis. We will be expanding this study provincially to evaluate the outcomes for all patients having SLNB during this time period to evaluate the consistency of care throughout the province. We propose that in the future patients be prospectively entered into our database for ongoing quality assurance and outcome evaluation.
73. Melanoma recurrence in the era of sentinel node biopsy: predictors and patterns of failure
Sentinel lymph node (SLN) biopsies have been demonstrated to accurately reflect the status of a draining nodal basin in melanoma. Despite a low nodal failure rate after sentinel biopsy, in-transit and distance recurrences still occur. This study examines the failure rate in melanoma patients, focusing on patterns and risk factors after a negative SLN biopsy.
A prospective database identified 156 patients undergoing sentinel node assessment for clinical stage I/II melanoma. Age, sex, Breslow depth, pathological features, TNM staging and primary site were all recorded. Follow-up (mean 25 mo) was conducted in a multidisciplinary clinic setting. Categorical data were analyzed with χ2 and Fisher’s exact tests and parametric data with Student’s t test.
SLN negatives accounted for 76% of all cases, with 3 basin failures in the node negative group. Overall recurrence, including in-transit, nodal and distant disease was markedly higher in the node positive group (44% v. 8.4%, OR 8.7, p = 0.000003). Sixty percent of failures in the node negative group recurred with evidence of in-transit disease. Fifty percent of node negative T4 patients experienced in-transit or distant failure versus only 4.6% of the remaining SLN negative population (OR 17.0, p = 0.0005). Ulceration was also more common in the recurrence group (p = 0.003).
In-transit recurrence is the most frequent manifestation of failure in the SLN negative group. T4 and ulcerated lesions are at particular risk, even in the face of a negative SLN biopsy.
74. Withdrawn
75. Parathyroidectomy and chronic renal failure: factors influencing success
The aim of this study was to identify factors predicting success after surgery on patients with hyperparathyroidism and chronic renal failure.
We reviewed retrospectively all patients treated by parathyroidectomy for secondary and tertiary hyperparathyroidism from 1986 to 2004 in a single institution. Data were collected for patients’ demographics, preoperative and intraoperative variables and at the follow-up.
Ninety-seven patients were surgically treated for secondary and tertiary hyperparathyroidism and 7 of those were excluded because of incomplete information. Ninety patients remained for the final analysis. The mean age was 42.4 ± 15.0 years. There were 48 men (53.3%). The mean dialysis time was 4.6 ± 5.0 years with a preoperative intact parathyroid hormone (iPTH) of 907.5 ± 417.9 ng/mL. The main surgical indications were osteodystrophy, hypercalcemia and calciphylaxy in 32.4%, 16.2% and 13.5%, respectively. Thirty-three (36.6%) patients had resection of 3 or less parathyroid glands while 57 (63.3%) had resection of more than 3 glands. The success rate, defined by a iPTH of ≤ 200 ng/mL after 6 months, was 57.8% (n = 48). The causes of treatment failure were persistence and recurrence in 33.7% and 8.4%, respectively. Among the variables of multivariate analysis (sex, age, dialysis status, hyperparathyroidism type, number of gland resected, preoperative and postoperative calcemia and preoperative iPTH), only resection of more than 3 parathyroid glands (p = 0.0018) and tertiary hyperthyroidism (p = 0.0454) were statistically significant predictive factors of surgical success.
Resection of more than 3 parathyroid glands and tertiary hyperparathyroidism were positive factors for predicting success after parathyroidectomy on chronic renal failure population.
76. Oxistress assay: novel bedside technique for measuring oxidative stress in surgical patients
Oxidative stress has been associated with many clinical conditions, and trauma is the commonest cause. Most techniques for measurement are very technically involved and not easy to use in a clinical setting. This may explain the current gap in knowledge of the natural history in humans as most studies have been post mortem or in animals. We evaluated the novel Oxistress assay (Obayan et al, 2005, US Patent # 6 852 541) in the clinical setting as a method for measuring oxidative stress in biological fluids.
The aim of the study was to develop an easy clinically applicable technique for measuring oxidative stress and to evaluate its efficacy.
The principle of the assay is based on the rapid reaction of deoxyglucose in the presence of hydroxyl ion or peroxyl radical to produce a distinct colour change in thiobarbituric acid. It is presently being developed into a dipstick.
Preliminary testing was done on urine samples from stressed rats and plasma from blood-bank blood to determine its ability to measure peroxides. A blind study comparing urine samples in 61 patients and 50 controls was done to evaluate the accuracy of the assay as a screening test. A prospective study was also conducted on all trauma patients (n = 120) over 15 years of age assessed and admitted by the trauma team between April and September 2000.
A significant difference (p = 0.0001) was observed between the mean urine peroxide levels in the patient population (674 μM/l) and the controls (196 μM/l).
Trauma resulted in more than 2-fold the normal urine excretion of oxidants.
Results correlated with those of the plasma antioxidant (FRAP), erythroctye GSH (modified Brigelius’) and protein carbonyl (modified Levine’s) methods.
We recommend the novel Oxistress assay as a bedside test for oxidative stress because it has proven to be a reliable clinical screening and diagnostic tool.
77. Clinical practice guidelines for the care and treatment of breast cancer: Have they made a difference?
A major objective of the Canadian Clinical Practice Guidelines for the Care and Treatment of Breast Cancer was to reduce variation in treatment by provider. In order to evaluate if that objective was achieved, we examined provincial rates of surgical care, as well as the variation in rates of surgical care by surgeon pre- and post-guideline publication in 1998.
This study drew from a population-based cohort of 5429 Manitoban woman diagnosed with breast cancer from 1995 to 2001. The provincial cancer registry provided demographic, tumour and treatment information. Medical claims data were used for provider information. The measures examined were based on the availability of both a published Canadian Guideline and reliable data for evaluation. Specifically, the 4 measures evaluated were: breast conserving surgery, axillary assessment in invasive and noninvasive disease and the adequacy of axillary node dissection. Provincial rates and the variation in rates by surgeon over time pre- and post-guideline publication were plotted and examined for inflection points. Multivariate analysis with nested modelling was used to determine if these rates differed statistically (p < 0.05) by time period.
Despite the presence of important differences between actual and ideal rates of care for the surgical measures reviewed, the Canadian Clinical Practice Guidelines for the Care and Treatment of Breast Cancer showed no clinically or statistically significant effects on provincial rates or variation in rates by surgeon. New strategies in guideline dissemination and/or implementation may be required.
78. Preoperative radiotherapy and radical resectional surgery in the treatment of retroperitoneal sarcoma
Surgery alone fails to provide long-term local control in a large proportion of patients with retroperitoneal sarcoma (RPS). Over the last 15 years, we have developed a novel protocol for the treatment of RPS, using tissue expanders to displace the bowel from the field of preoperative external beam radiation therapy (PEBRT) before surgery. Thirty-eight consecutive cases of RPS were treated: 28 of these were primary and 10 recurrent. Twenty of the primary cases were treated using the following protocol: 1) staging laparotomy and placement of saline-filled tissue expanders, 2) PEBRT (5000 cGy) and 3) radical resectional surgery 6–8 weeks later. There was minimal morbidity associated with expander placement, and 19 patients completed a full course of PEBRT with no severe adverse effects. R0 resection was achieved in 12 of the 20 primary cases, and R1 in 6. A mean of 2.5 additional organs was resected per patient (range 0–5). Seventeen patients remain disease-free at a median follow-up of 39 (14–65) months. Disease recurred in 3 (15%) at a median of 22 months, and 2 of these died at 32 and 112 months after surgery. Overall median survival for these 20 patients was 40 (18–76) months, and the median disease-free interval was 35 (18–67) months. Of the 10 recurrent cases, median survival was 25 (9–29) months in 6 treated with palliative radiotherapy alone and 57 (39–93) months in 4 treated with combined radiotherapy and resectional surgery.
We conclude that a low recurrence rate can be achieved in RPS using radiation combined with radical surgery and that the use of intra-abdominal tissue expanders is safe and effective and may facilitate the delivery of full-dose PEBRT. These findings are in keeping with preliminary results from ongoing randomized trials on the use of PEBRT in the treatment of RPS. Statistics: median (25th percentile–75th percentile).
79. Medical management of chronic anal fissures: a meta-analysis
To assess the efficacy and morbidity of various medical therapies for healing of chronic anal fissure as compared with placebo or lateral sphincterotomy.
Literature search of all randomized controlled trials published in English in the EMBASE and PubMed databases was performed. Search terms included “fissure-in-ano, glyceryl trinitrate (GTN), calcium channel blockers (CCB), botulinum toxin (Botox) and randomized controlled trials (RCT).” Acute anal fissures and fissures in children were excluded. Each study was reviewed by 2 reviewers, and discrepancies were resolved by discussion. REVMAN 4.2.7 was used for statistical analysis.
Thirty-nine studies were identified; of those, 21 were eligible for entry. Eleven studies with 985 participants compared GTN with placebo. GTN was superior (OR 2.38, 95% CI 1.81–3.03). Headache was the main side effect (OR 4.06, 95% CI 2.56–6.43). GTN was compared with lateral sphincterotomy in 5 studies (n = 303). Healing was superior with surgery and headache more common with GTN (OR 8.91, CI 4.77–16.62; OR 31.01, CI 9.3–103.04, respectively). Surgery was associated with higher risk of minor incontinence (OR 6.25, CI 1.11–33.33).
Three studies (n = 136) compared Botox with placebo, OR 2.63, CI 2.70–5.26 in favour of Botox. Fifteen studies (n = 1231) comparing placebo with various medical therapies were pooled. Healing was in favour of active treatment (OR 2.38, CI 1.81–3.03). Likewise, 6 trials (n = 414) compared medical treatment (5 GTN and 1 Botox) with surgery. Surgery was superior for healing (OR 8.07, CI 4.59–14.2). Sphincterotomy was more likely to cause minor incontinence (OR 10, CI 2.22–50).
We concluded that compared with placebo, medical treatment is superior. Despite an increased risk of minor incontinence, lateral sphincterotomy remains the gold standard for treating chronic anal fissures.
80. Conservative management for well differentiated thyroid cancer
A retrospective study was performed of all patients with well differentiated thyroid cancer between 1982 and 2002 operated upon by a single general surgeon at our centre. One hundred and eighty patients were identified. All patients were seen regularly with none lost to follow-up. This consisted of a 6 monthly neck examination ± ultrasound together with maintenance of full thyroid suppression status. There were 136 patients (75.5%) TNM stage I and II, and 44 (24.5%) in higher stages with no mortality in the low-risk group over the 20 years and 4 in the high-risk group. A total of 97 patients (54%) had a lobectomy and isthmusectomy; 31 patients (18%) had an extended hemithyroidectomy (medial aspect opposite lobe) for a total of 128 patients (72%) who had conservative surgery (Gp A).
Twenty-seven patients (15%) underwent near total thyroidectomy, and 25 patients (14%) had a total thyroidectomy for a total 52 patients (29%) with more extensive surgery (Gp B). In Gp A, no patients had a recurrence within the residual thyroid gland. Only 4 required reoperation to resect a recurrence in lymph nodes, usually a single node, and no distant metastases occurred. There was no recurrent nerve paresis and no mortality related to the disease. Gp B accounted for 4 mortalities and 17 recurrences despite more radical initial surgery. Postoperative unilateral recurrent laryngeal nerve paresis occurred in 6 of these patients (3.4%); of these, 2 (1.1%) were permanent. Twelve cases (6.7%) were complicated by postoperative hypocalcemia in which 2 (1.1%) with total thyroidectomy were permanent.
Conservative surgery for low-risk patients with well differentiated thyroid cancer is sufficient and adequate surgery which avoids complications without significant risk for recurrence local, regional or distant. Higher-risk patients may need more aggressive surgery but with higher morbidity and despite the more aggressive surgery with significant risk for local recurrence. Biological factors and initial risk stratification are the important determinants of outcome and not the extent of surgery.
93. Evaluation of BAX, BCL-2, cytochrome C and caspase 8 expression in breast cancer patients: Is there a prognostic role in early stage cancers?
Breast cancer exhibits a wide spectrum of biological behaviour, even in the same stage of disease. Furthermore, apoptosis has been shown to be intimately involved in carcinogenesis and metastasis. The purpose of this study was to determine the prognostic value of the apoptotic machinery involved proteins, namely BAX, BLC2, cytochrome C and caspase 8 in breast cancer patients.
Seventy-six patients with breast cancer diagnosed from 1988 to 1991 were identified retrospectively. Clinicopathological parameters such as age, tumour size, estrogen receptor status, lymph node status, disease-free survival and overall disease-specific survival were obtained. Paraffin-embedded formalin-fixed tissues were immunostained with BAX, BLC2, cytochrome C and caspase 8 antibodies using a standard avidin biotin reaction. Stained slides were evaluated by a pathologist for staining intensity and percentage of cells staining positively. Kaplan–Meier and Cox regression were used for uni- and multivariate survival analysis.
Mean patient age was 59 years with a mean follow-up of 5.4 years from the time of surgery. Infiltrating ductal adenocarcinoma was the most common pathology. Neither expression nor coexpression of the proteins of interest was associated statistically with pathological characteristics, disease-free or overall survival. In patients with T1 tumours, coexpression of BAX and caspase 8 was associated with worse survival (100% v. 50%, p = 0.027). In patients with N0 disease, BAX expression was associated with worse survival (100% v. 70%, p = 0.021). Finally, in stage IIA patients, BAX expression with or without caspase 8 coexpression led to worse disease-free and disease-specific survival (100% v. 65%, p = 0.01, for disease-specific survival).
These results indicate that BAX expression or BAX and caspase 8 coexpression are associated with worse disease-free and disease-specific survival in patients with early stage breast carcinoma (T1 or N0 or IIA). Prospective validation of these results is warranted.
81. Cyclin D1 polymorphism G870A and risk for Barrett esophagus and esophageal adenocarcinoma
To investigate individual susceptibility to gastresophageal reflux disease (GERD), Barrett esophagus (BE) and esophageal adenocarcinoma (EADC), we studied the frequency of the common G870A polymorphism of CCND1, which encodes cyclin D1, a key cell cycle regulatory protein.
The study population comprised 307 patients enrolled in a prospective case–control study to evaluate lifestyle risk factors and molecular alterations in GERD (n = 126), BE (n = 125) and EADC (n = 56), defined according to strict clinico-pathologic criteria. Controls comprised 95 strictly asymptomatic individuals. Genomic DNA was extracted from cases and controls, and polymerase chain reaction was used to amplify exon 4 of CCND1. After digestion with BsrI, acrylamide gel electrophoresis was used to identify wild-type and the G870A polymorphic allele. The frequency of alleles (G/G, G/A, A/A) was compared between cases and controls. Immunohistochemistry, using the monoclonal antibody DCS-6, was used to study cyclin D1 protein distribution in cases.
The observed distribution of CCND1 genotypes in controls was as predicted from Hardy–Weinberg equilibrium theory. Compared with asymptomatic controls, and adjusted for age and gender, increasing frequencies were seen for the A/A genotype in patients with GERD (odds ratio [OR] 2.83; 95% confidence interval [CI] 1.09–7.34), BE (OR 3.69; 95% CI 1.46–9.29) and EADC (OR 5.99; 95% CI 1.86–18.96). Although significant differences for cyclin D1 overexpression were found between cases with GERD-induced esophagitis (20%; 15/74), Barrett metaplasia (11%; 14/125) and EADC (25%; 14/56) (p = 0.001), no association was seen between genotype and cyclin D1 overexpression.
The CCND1 A/A genotype is associated with increased risk for GERD, BE and EADC. The contribution of this polymorphism to susceptibility of defined stages of progression to esophageal adenocarcinoma suggests the incorporation of CCND1 genotype analysis in endoscopic Barrett surveillance programs may allow better stratification of individuals at increased risk for malignant progression.
82. Minimally invasive esophagectomy
Between February 2004 and March 2005, 54 patients (pts) underwent operative exploration for planned esophagectomy. Forty-eight pts (35 males, 13 females, median age 67) were approached with minimally invasive techniques. Twenty pts had previous open abdominal surgery. With laparoscopy, 5 were found unresectable, had a mini-laparotomy and feeding tube placement. Five pts were converted to laparotomy and underwent a gastrectomy. Of the remaining 38 pts, 26 had a laparoscopic-assisted transhiatal esophagectomy (LTE), 4 had a right thoracotomy and laparoscopic-assisted esophagectomy (T-LE), 8 had a right video-assisted thoracic esophageal mobilization and LE (V-LE). Twenty-three percent were converted to laparotomy, for assessment of resectability (4 pts), adhesions (4 pts) or spleen injury (1 pt). Major complications leading to reoperation occurred in 2 LTE pts (port site hernia, colon herniation), 1 T-LE pt (chylothorax) and 5 V-LE pts (3 chylothorax, 1 empyema, 1 bronchial injury). Median LOS was 10 days. There were no postoperative deaths. Anastomotic stricture occurred in 5 patients after discharge. Three pts had benign disease, 1 severe dysplasia, 10 squamous cell carcinoma and 24 adenocarcinoma. Sixteen pts had T1–T3 N0 disease, 16 had T2–T3 N1 disease and 2 pathologic stagings are pending. Up to 30 lymph nodes per resected specimen were identified and histologically examined. Most patients with N1 disease underwent adjuvant treatment. Two of 38 pts died within 3 months of surgery from metastatic disease. With a mean follow-up of 4 (0–12) months, all surviving pts are currently disease-free. Laparoscopic assisted esophagectomy is technically feasible in most patients. Early experience suggests LTE is associated with low morbidity. Further follow-up is required to determine oncological outcomes.
83. Evolution to video-assisted thoracic surgery (VATS) lobectomy after training and the initial results of the first twenty cases
The operative experience leading to the first lobectomy by video-assisted thoracic surgery (VATS) along with the outcomes of the initial 20 cases of a new graduate were examined.
The data were collected prospectively from a single surgeon who completed thoracic surgery training certified by the Royal College of Physicians and Surgeons of Canada. Mortality was defined as death within 30 days or death in hospital. Morbidity was defined as any complication requiring intervention or prolonging hospital stay.
Prior to performing the first VATS lobectomy, 94 major pulmonary resections were performed by open thoracotomy (10 pneumonectomy, 2 sleeve resection, 8 bilobectomy, 72 lobectomy and 2 segmentectomy). In this group, experience with the lateral muscle sparing incision increased from 17% (8/47) to 70% (33/47) when comparing the approach used for the initial half of this group with the latter half.
The morbidity for the first 20 cases of VATS lobectomy was 25%, and the mortality was 5%. Mean operative time was 170 minutes, median blood loss was 200 mL, and median length of stay was 6 days. There were 3 conversions to open (15%), all due to bleeding from the pulmonary artery. The single death was due to pneumonia. There were no intraoperative deaths or deaths directly related to the VATS technique. Of the 19 patients who survived surgery, all are alive and disease-free after short-term follow-up.
New graduates of thoracic surgery training programs in Canada can safely perform VATS lobectomy with acceptable morbidity and mortality rates. Experience with pulmonary resection by lateral muscle sparing thoracotomy is important as this approach is similar to that used during pulmonary resection by VATS. Data from other new graduates are needed to confirm these results. Long-term disease-free and overall survival data from this current series are needed to evaluate the oncological outcomes of this procedure performed by a new graduate.
84. The evolution of distant thoracic surgical patient assessment in British Columbia, 1985–2005: from on-site outreach clinic to videoconferencing
In 1985, we began the process of enhancing access to thoracic surgical assessment by establishing distant outreach clinics, recognizing that patient access to tertiary services decreases as travel distance increases.
As technology has progressed, the process of patient assessment has evolved from on-site outreach clinic to videoconferencing. With the on-site clinic, the surgeon travels to distant communities where local patient assessment occurs. With the advent of videoconferencing, the surgeon from his home-based hospital conducts the assessment with the patient and the thoracic oriented nurse attending at their distant site.
In both circumstances, surgery occurs at the surgeon’s base hospital. A patient satisfaction tool was developed to evaluate acceptance of videoconferencing.
Between 1985 and 1998, outreach clinics were held in Kelowna, Trail and Prince George at times when no thoracic surgeon was available in these communities. Data were not kept.
Between May 1998 and April 2005, on-site clinics occurred in Prince George, Kamloops, Cranbrook, Trail and Nelson:
| 100 clinics | (1.2 clinics/mo) |
| 1890 patients | (18.9/clinic) |
| 602 consultations | (6.0/clinic) |
| 1288 follow-ups | (12.9/clinic) |
Between December 2003 and April 2005, videoconferencing clinics have been held in Kamloops, Cranbrook, Nelson, Trail and Grand Forks:
| 52 clinics | (3.3 clinics/mo) |
| 449 patients | (8.6/clinic) |
| 152 consultations | (2.9/clinic) |
| 297 follow-ups | (5.7/clinic) |
For the past 20 years, we have successfully conducted more than 2000 distant patient assessments through on-site and videoconferencing clinics. Since 2003, the rapid evolution of videoconferencing has further improved access to the distant thoracic surgical patient by increasing both frequency of clinics and the number of sites reached by the clinics.
85. Impact of a change in anastomotic technique for esophagectomy
Clinical outcomes after a stapled cervical anastomosis were compared with those obtained following traditional handsewn technique after esophagectomy.
A review of an esophageal cancer database (2001–2004) identified patients who underwent cervical esophagogastric anastomosis following esophagectomy. Beginning in the fall of 2002, the stapled technique for cervical esophagogastric anastomosis was introduced (n = 20). Clinical outcomes were compared with a group of patients in whom a hand-sewn technique was used (n = 72). Outcomes related to cervical anastomotic leak, length of stay and the need for postoperative dilatations were compared. Student’s t tests (length of stay) and χ2 tests were used with significance at p < 0.050.
As early as the first year after introduction of the stapled technique, a trend toward decreased anastomotic complications could already be observed. Cervical anastomotic leaks complicated 5% of stapled as compared with 26% of handsewn anastomoses. This difference approached statistical significance despite the recent introduction of this technique and the small number of patients treated (p = 0.063). Patients who underwent stapled anastomosis tolerated earlier oral feeds and had a significantly decreased hospital length of stay (20.9 ± 14.6 d v. 10.8 ± 5.4 d [mean ± SD], p < 0.001). Significant quality of life improvements were associated with the stapled anastomosis. Dysphagia related to stricture was markedly diminished as was the need for postoperative dilatations (15% of stapled v. 46% of hand-sewn, p = 0.018).
A stapled cervical esophagogastric anastomosis after esophagectomy is superior to the traditional hand-sewn cervical anastomosis. Differences were apparent within 1 year following the introduction of the stapled technique. We anticipate that these differences will become more evident as this institution gains experience with this technique with greater number of patients over time.
86. Increased expression of inducible nitric oxide synthase, nitrotyrosine and p53 mutations in the molecular pathogenesis of esophageal adenocarcinoma
To investigate critical early molecular alterations in the pathogenesis of esophageal adenocarcinoma (EADC), we studied the expression of inducible nitric oxide synthase (iNOS) and nitrotyrosine (NTS), a stable reaction product of chronic nitric oxide (NO) exposure and a marker for cellular protein damage, in a well-defined series of patients with gastresophageal reflux disease (GERD), Barrett esophagus (BE) and EADC. As NO has been implicated as a potential causative factor for endogenous p53 mutations, a subgroup of EADCs were characterized for p53 alterations.
RNA was extracted from esophageal tissues comprising GERD-induced esophagitis (n = 76), BE (n = 119) and EADC (n = 54). Reverse transcription polymerase chain reaction (RT-PCR) was used to study iNOS expression in each esophageal tissue type, relative to matched normal epithelia (internal control). Immunohistochemistry was used to study NTS expression in corresponding formalin-fixed tissue sections. p53 mutations were characterized in 32 EADCs by DNA sequencing.
A progressive increase in iNOS mRNA overexpression was seen in tissues from patients with GERD (4%; 3/76), BE (20%; 24/119) and EADC (35%; 19/54) (p < 0.0001). NTS expression was significantly more common in EADC (43%; 23/54) when compared with GERD (24%; 18/76) and BE (22%; 26/119) (p = 0.013). p53 mutations were found in 21 of 32 (66%) EADCs; 11 mutations were at CpG dinucleotides. NTS overexpression was significantly more frequent in tumours with p53 mutations at CpG dinucleotides (10/11) compared with non-CpG mutations (3/10) (91% v. 30%, p = 0.008).
The increasing frequency of iNOS mRNA overexpression in GERD, BE and EADC supports the hypothesis that an active inflammatory process, most likely a consequence of GERD, underlies molecular progression to EADC. The highly significant association between NTS, reflecting chronic NO-induced cellular protein damage and endogenous p53 mutations at CpG dinucleotides, provides further evidence for a molecular link between chronic inflammation and the development of EADC.
87. Endoscopic cricopharyngeal myotomy and Zenker’s diverticuloplasty
A prospective study evaluating the effectiveness of the operating diverticuloscope in the surgical management of Zenker’s diverticulae was undertaken at LHSC. Between November 2002 and March 2005, 16 patients underwent surgery for a symptomatic Zenker’s diverticulum. Ages ranged from 44 to 89 years of age. Nine patients (60%) were successfully treated with endoscopic repair (ER). Operative time was less than 1 hour in all ER cases. LOS was 24 hours. Four patients were converted to open repair after attempted endoscopic repair because of poor visualization of the diverticulum. Open repair was the initial surgery in 3 patients because of the presence of a very small diverticulum. The only complication was a suspected mucosal tear in an ER patient (sutured endoscopically). Good to excellent relief of all preoperative symptoms was seen in all ER patients 6 weeks postoperatively. Longer ER followup (up to 2.5 yr) was available in 6 patients. Two patients remain symptom free, 2 patients have minimal symptoms, and 2 patients have recurrence of some dysphagia requiring further investigation.
Endoscopic treatment of a Zenkers’s diverticulum is a safe, minimally invasive procedure, requiring short length of hospital stay and operating time. There appears to be a significant relief of symptoms in most patients.
88. A retrospective analysis of the clinical performance of anterior mediastinoscopy
The objective of this study is to examine the role of anterior mediastinoscopy in staging of patients with left-sided lung cancer. All patients with left-sided lung lesions and otherwise normal CT scans referred to a tertiary care university hospital thoracic surgery service between 2001 and 2004 were reviewed. Two hundred and twenty-six (226) patients were stratified into 2 groups: those having undergone cervical and anterior mediastinoscopy and those having undergone cervical mediastinoscopy only (controls). Eighty-three patients (83) were excluded because they had clinically unresectable disease (advanced disease or not fit for surgery). Unnecessary thoracotomy rates (thoracotomy for benign disease or advanced, unresectable cancer) were compared in the remaining 143 patients. In the anterior mediastinoscopy group, 18 of 80 (22.5%) had an unnecessary thoracotomy compared with 17 of 63 (27.0%) for controls (p = 0.54 χ2 analysis). Furthermore, in 24 of 80 patients who had an anterior mediastinoscopy, no lymph nodes were sampled. Only 3 of 80 patients were spared an unnecessary thoracotomy by the identification of metastatic disease to either anterior mediastinal or aortopulmonary lymph nodes. In patients with left-sided lung cancer and otherwise normal CT scans, anterior mediastinoscopy does not significantly reduce the rate of unnecessary thoracotomy.
89. Development of a lung tumour model for validating 3-dimensional thoracoscopic ultrasound imaging
We developed a lung tumour model, using excised porcine lung and agar tumours, to provide a means of verifying 3-dimensional ultrasound (3D US) images and to provide a teaching tool for intraoperative lung ultrasound techniques.
Spherical tumours were made from agar with diameters ranging from 9.5 mm to 25.4 mm and were inserted through incisions on the underside of an excised porcine lung. The lung was placed in a box with ports, and the thoracoscopic US probe was inserted through a port for imaging, in a similar fashion to introperative US imaging of lung nodules during VATS (video-assisted thoracoscopic surgery). Multiple 2-dimensional (2D) US images of the subpleural tumours were reconstructed into 3D images. We coupled the HDI 5000, LapL9-5 thoracoscopic probe to a rotational mover driven by a computer. During data acquisition, the ultrasound probe was held by a stabilizing system, while the probe rotated 100° about its long axis for approximately 6 seconds. One observer measured the tumour image volumes 5 times, once every 2 days. Using software developed in our laboratory, the tumour boundaries were outlined in image slices 3° apart.
The 3D US images of the lung model tumours were very similar in appearance to those obtained intraoperatively. The coefficient of variation (COV = standard deviation / mean) and tumour volume error decreased as the tumour size increased. The average COV and volume error were 11.2% and 12.9%, respectively.
3D thoracoscopic US can be used accurately and reproducibly to measure tumour volumes in vitro; thus it may also be useful for radiation dose planning in minimally invasive lung cancer therapies such as brachytherapy. Although many of our lung ultrasound techniques were developed in the operating room, there is a need for teaching tools to provide a practical means for becoming accustomed to this imaging technology.
90. Post-pneumonic empyemas in southwestern Ontario: A new crisis!
A retrospective review of adult post-pneumonic empyemas requiring decortication (n = 211) in London from April 1997 to December 2004 was undertaken. We excluded charts containing incomplete data (n = 45), pediatric cases (≤ 16 years of age), non-infectious causes (esophageal perforations, esophageal anastomotic leaks, hemothorax, trauma) (n = 55). These data (n = 111) were compared with the total number of patients with a discharge diagnosis of empyema (ICD-10 code J86 and ICD-9 code 510).
The annual number of cases with a diagnosis of empyema from April 1997 to December 2004 was 44, 35, 36, 42, 75, 68, 72 and 55. Correspondingly, the annual number of empyemas requiring decortication was 0, 0, 6, 9, 20, 22, 30 and 24. When the first 4 years were compared with the last 3 years and 9 months, this represented a 74% relative increase in the number of patients discharged with a diagnosis of empyema, with a corresponding 540% relative increase in number of empyemas requiring decortication. The mean age of these adults was 56, 77% of whom were male. Ninety-one percent of cases obtained pleural fluid cultures that grew Streptococcus species (α-hemolytic streptococcus, S. anginosus, pneumoniae or viridans) in 31%, Staphylococcal species (S. aureus or epidermidis) in 16% and were culture negative in 42%. Outpatient antibiotics prescribed before transfer were known for 58 patients included levofloxacin (22%), azithromycin (10%) and clarithromycin (9%). The most common in-hospital antibiotics prescribed were levofloxacin (16%), cefotaxime (12%) and clindamycin (12%).
Since 1997, there has been an alarming increase both in the number of patients with empyemas admitted to hospital, as well the number of post-pneumonic empyemas that required operative intervention. The etiology remains unclear.
91. A prospective assessment of the impact of lower esophageal sphincter tone on achalasia symptoms
Although the absence of peristalsis is the sine qua non of achalasia, a hypertensive lower esophageal sphincter (LES) is often included in the definition of this motility disorder. However, the influence of LES tone on symptoms of achalasia is not well documented.
All patients referred for esophageal motility for an assessment of dysphagia from February 2004 to March 2005 were asked to participate. The Achalasia Symptom Questionnaire (ASQ), a structured 11-question survey (score: 0–best, 67–worst), was completed by all consenting patients. Those with achalasia (manometric absence of peristalsis) were divided into 2 groups: group A = hypertensive LES (> 26 mm Hg) and group B = normal/hypotensive LES (< 26 mm Hg). Patient characteristics, manometric data and symptoms scores were compared between the 2 groups. Data presented as mean ± SD; t test or χ2 determined significance (*p < 0.05).
Fifty-three patients with newly diagnosed achalasia were identified in the study period: 8 patients were excluded because of prior treatment; complete data were available in 38 of 45 (group A, n = 22; group B, n = 16). LES tone (A = 42.6 ± 10; B = 18.8 ± 4)* and % of LES relaxation (A = 50.2 ± 20%; B = 66.7 ± 18%) differed significantly between the 2 study groups. Compared with group A, group B had less dysphagia (0–4 Likert scale) to liquids (A = 2.8 ± 1.2; B = 2.1 ± 1.3)* and soft food (A = 2.8 ± 2; B = 1.8 ± 1)* but not solids (A = 3.2 ± .9; B = 2.6 ± 1.1). ASQ was less in group B (A = 42.9 ± 15; B = 29.7 ± 14).* No difference in age or gender was noted.
Normal or low LES pressure is present in a large proportion of patients with achalasia and imparts significantly less dysphagia and fewer symptoms. Given that a reduction in sphincter tone is the primary goal of most therapeutic modalities of achalasia, the initial LES pressure may impact the success rate of treatment for this disease.
92. Repair of esophageal perforation: a diversified approach
Outcomes in esophageal perforation (EP) have been linked to timing of diagnosis and location and extent of injury. We believe that accurate assessment and appropriate application of the initial approach to repair is critical to improved outcomes.
Records were reviewed for all patients admitted with EP to Virginia Mason Medical Center (VMMC) from 1989 to 2002. Patients with fistulization and non-iatrogenic perforation secondary to a malignancy were excluded.
Forty-six patients with a mean age of 64.7 (30–86) years were treated at VMMC in the study period. Perforations were iatrogenic (n = 31), barogenic (n = 14) and unknown (n = 1). Thirty-four patients had an upper gastrointestinal (UGI) contrast study personally reviewed by the surgical team that was either performed initially or repeated at VMMC after transfer from a referring institution. Ten patients were managed nonoperatively: 8 had parenteral antibiotics and 2 also had endoscopic stent placement. Mean ASA for all patients was 3.0. Of patients managed operatively, 20 underwent primary repair, 6 underwent resection (3 primary and 3 delayed), 6 had primary repairs in addition to intraoperatively placed stents (4) and T-tubes (2), and 4 underwent operative drainage alone. Mean time from perforation to operative intervention was 29.8 hours (2 h–10 d). Intraoperative endoscopy was selectively used in 12 patients to guide treatment planning. Twenty-seven complications occurred in 17 patients. One death in the nonoperative group and 1 death in the operative group resulted in mortality rate of 4.3%. Complications but not mortality were increased in patients with delayed treatment (> 24 h).
UGI contrast studies personally supervised by this surgical team and intraoperative endoscopy are important components of the initial assessment. Appropriate utilization of primary repair, intraoperative stents, T-tubes, drainage alone and resection in selected patients will improve outcomes and decrease the requirement for defunctioning procedures.






