Compliance and barriers to postoperative colorectal cancer follow-up in a tertiary care cancer centre
Introduction:
The primary aim of patient follow-up (FU) after curative-intent treatment for colorectal cancer (CRC) is to identify patients who have resectable disease. Three recent meta-analyses have suggested that close surveillance can improve long-term survival. Our multidisciplinary team adopted a stringent CRC FU strategy in 2000. The purpose of this study was to assess adherence and barriers to FU for CRC.
Methods:
Patients aged 19–75 years who had curative intent surgery from July 2000 to Dec. 2002 were identified from a prospective CRC database at a tertiary care cancer centre. Compliance with FU was assessed by chart review. We surveyed patients and providers to explore barriers to FU adherence.
Results:
Of 149 patients, 93 with no metastases who were appropriate for FU were identified. Median FU was 34 months. Guideline targets were met for 70% of clinic visits, 49% of CEA and 62% of abdominal imaging studies. Perioperative colonoscopy occurred in 56% of patients, and 71% of patients had a postoperative colonoscopy. Seventy percent of health care providers and 55% of patients completed a barriers survey. Access to physicians and tests were identified by both groups as the most important barriers to FU.
Conclusion:
CRC FU is widely variable despite implementation of guidelines set by a multidisciplinary team at our centre. By surveying providers and patients, we have identified barriers to CRC FU. In response, we have designed and instituted a novel, patient-centred intervention: a patient passport.
A population-based assessment of adequacy of surgical resection for T4 colorectal cancer
Introduction:
Inadequate resection of pT4 colorectal cancer (CRC) may result in increased local recurrence and reduced survival.
Methods:
We analyzed the clinical, pathological and follow-up data of resected pT4 CRC in the Ontario Familial Colorectal Cancer Registry from 1997 to 2000. Rates of positive surgical margins, lymph node assessment and local recurrence were assessed. Two surgical oncologists examined the operative and pathology reports, and cases with suspected violation of surgical oncologic principles were identified.
Results:
Seventy-six cases from 45 hospitals were documented. Median follow-up was 4 years. Median patient age was 58 years; 68 (89%) had primary colon cancer. Median number of lymph nodes reported was 9 (range 0–44). Thirty-six (47%) tumours were N0 and, of these, 19.4% and 2.8% of patients had a R1 and R2 resection, respectively. Median survival following R0 was better than after R1 or R2 resection (71 v. 31 mo, p = 0.03). Incomplete resection (R1/2) was associated with increased disease recurrence. Examples demonstrating violation of surgical oncologic principles relevant to achieving R0 excision were demonstrated in 6 operative reports.
Conclusion:
Variation exists in the surgical treatment of pT4 CRC in Ontario. The median number of lymph nodes retrieved and/or reported was below recommended guidelines. Approximately 1 in 5 pT4 lesions were resected with an R1/2 excision, and disease recurrence was more frequent in this group. Suboptimal resections occurred at the same frequency in N0 and N+ patients. Excerpts from operative and pathology reports suggest suboptimal application of critical surgical oncologic principles.
A qualitative assessment of the Quality Initiative in Rectal Cancer trial
Introduction:
The Quality Initiative in Rectal Cancer (QIRC) trial randomized 16 hospitals across Ontario to the QIRC strategy versus minimal intervention. The strategy included a workshop, use of an opinion leader (OL), operative demonstrations, postoperative checklists and audit/feedback. Surgeons at each intervention hospital used a standardized approach to select an OL from their ranks. We assessed the experiences of OL and non-OL surgeons in the QIRC strategy.
Methods:
Semi-structured qualitative telephone interviews were completed with the 8 OLs and 8 non-OL surgeons. Interviews were guided by grounded theory. Initial interviews were assessed to ensure that domains of interest were fully explored. Two investigators (F.W., M.F.) independently reviewed all final transcripts and identified themes. Consensus among all investigators was achieved for final themes.
Results:
All approached surgeons participated in interviews. Seven themes were identified: limited role for local OL on changing physician practice in rectal cancer surgery; limited effect of identifying OL on group dynamics; operative demonstrations supported positive response from surgeons; characteristics of operative demonstrator are important; positive effect of the trial on practice; surgical OL requires technical expertise and subspecialist OL concept supported.
Conclusion:
The experience of local OLs in this trial appears to be mixed. While some of the themes support the concept of a local OL, other themes suggest the selected OL had a limited role and effect. However, the overall QIRC strategy and, in particular, the operative demonstration intervention, was viewed positively and was felt to have a positive long-term effect on participants’ practice.
Trends in rectal cancer survival in relation to the local control strategy.*
Introduction:
Improved rectal cancer survival has been credited to improved local control obtained from quality-assurance programs involving surgery, with or without radiotherapy, in several population-based studies. Local control was suboptimal in Manitoba in the mid-1990s despite adoption of the 1991 National Institutes of Health (NIH) chemo-radiotherapy guidelines. We were interested in exploring trends in rectal cancer survival in Manitoba, particularly in patients where local control is an issue.
Methods:
Patients with rectal or rectosigmoid adenocarcinoma from 1985 to 1999 were identified from the provincial cancer registry. Demographic, treatment and mortality information were also abstracted from the registry. Manitoba population and death counts for the calculation of age-specific relative survival probabilities were obtained from Statistics Canada. Survival was examined for all patients for the periods 1985–89, 1990–94 and 1995–99 and subsequently limited to those who underwent major surgery (Hartmann’s, anterior and abdominal perineal resection). The Ederer II method was used for survival probabilities.
Results:
Three-thousand and twenty-one patients were identified with 1723 (57.0%) having major surgery. Five-year relative survival was 48.7%, 49.6% and 56.2% for all patients for the 3 periods, respectively; major surgery results were 56.9%, 58.1% and 59.7%. Perioperative radiotherapy was used in 38% of the 1995–99 major surgery group, twice the rate of 1985–89; perioperative chemotherapy was used in 41%, a 10-fold increase.
Conclusions:
Consistent with other studies, overall rectal cancer survival in Manitoba has improved since 1985. Better local control, as suggested in other studies, or increased adjuvant chemotherapy utilization, were not major factors in that improvement. Future work should include review of the local control strategy and factors to explain the improved survival. *This abstract has been previously cited in the ASCO 2006 Proceedings, Abstract #13536, with the full text available online through asco.org.
Diffusion of intraoperative demonstrations in the Quality Initiative in Rectal Cancer (QIRC) trial
Introduction:
Accrual to the QIRC trial has recently closed. The trial is testing the efficacy of the QIRC strategy and will provide insights on knowledge translation among surgeons. The key innovation of the strategy was an intraoperative demonstration of total mesorectal excision (TME), a new gold standard for rectal cancer surgery. The classic S-shaped diffusion-innovation curve suggests an initial slow uptake of an innovation followed by an acceleration at the 20%-participation level.
Methods:
For the trial, surgeons at 16 high-procedure volume hospitals across Ontario were cluster-randomized to the experimental (QIRC strategy) or control arms. Strategy interventions included workshops, audit and feedback, opinion leaders, postoperative checklists and intraoperative demonstrations. For this last intervention, surgeons could invite to their operating rooms an expert surgeon to demonstrate TME. Surgeons were encouraged to participate in 2 demonstrations. We measured participation over time in 1 or 2 demonstrations.
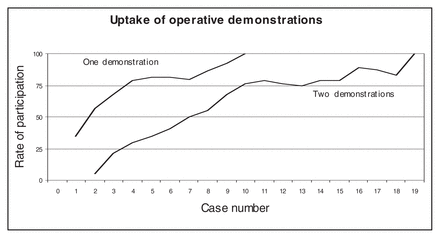
Results:
The 37 eligible surgeons in the experimental arm had case volumes varying from 6 to 34 cases. Thirty-five percent of surgeons had a demonstration on their first case. By case 5, 81% of surgeons had participated in 1 demonstration. Among surgeons with 10 or more cases, by case 10, 76% of surgeons had participated in 2 demonstrations. The slopes of both curves suggest a very early acute accelerated uptake unlike the classic S-shaped diffusion-innovation curve.
Conclusions:
Ontario surgeons participated with enthusiasm in a new surgical innovation, which required a marked change in their usual practice.
Treatment of peritoneal carcinomatosis arising from the appendix
Introduction:
Peritoneal carcinomatosis (PC) arising from the appendix is a rare disease for which the long-term prognosis is poor. The aim of our study was to evaluate the results of an aggressive treatment approach used in our institution in the last decade.
Methods:
Data from all patients with a PC arising from the appendix were prospectively collected and analyzed. Treatment consisted of a complete surgical cytoreduction of the tumour followed by intraperitoneal chemotherapy. Chemotherapy consisted either of early postoperative intraperitoneal chemotherapy (EPIC) or intraperitoneal chemohyperthermia (IPCH). Ronnett’s histologic classification was used for tumour grading: disseminated peritoneal adenomucinosis (grade 0), peritoneal mucinous carcinomatosis with intermediate features (grade 1) and peritoneal mucinous carcinomatosis (grade 2).
Results:
From Sept. 1997 to June 2005, 37 patients underwent laparotomy with curative intent. There were 13 patients treated with EPIC and 12 with IPCH. The estimated 5-year overall survival (OS) was 56% (95% confidence interval [CI] 34–77) for all patients, 58% (95% CI 30–86) for EPIC patients and 60% (95% CI 10–100) for IPCH patients. There was no statistically significant difference between these groups with regards to survival. Histologic grade was an important prognostic indicator since all grade 0 patients survived while none of grade 2 patients did (p < 0.0001). Patients with grade 1 tumour had an estimated 87% (95% CI 64–100) 5-year OS. There was no postoperative mortality. The overall complication rate for treated patients was 36%, including fistulas (16%) and intra-abdominal abscesses (12%).
Conclusion:
Although these results are preliminary, this therapeutic approach seems both feasible and safe in selected patients. Patients with high-grade tumours are poor candidates for this treatment.
Development of a standards document for laparoscopic colorectal cancer resection in Ontario
Introduction:
Laparoscopic resection (LR) has emerged as an option for the curative treatment of colorectal cancer. Adoption of LR across Ontario may cause patient morbidity. A clinical practice guideline (CPG) was initiated between the Surgical Oncology Program of Cancer Care Ontario (CCO) and the McMaster University Program in Evidence-Based Care (PEBC).
Methods:
An expert panel comprised of representatives of both CCO and the PEBC, general and colorectal surgeons from university and community hospitals in Ontario, and representatives of other related specialties and the Ontario Association of General Surgeons was formed to produce an endorsable CPG along with clinician and institutional standards. The draft document was sent out to Ontario clinicians in a 2-part structured feedback process targeting all Ontario general surgeons and a sample of medical and radiation oncologists.
Results:
The standards document outlines patient, clinician and institutional criteria for the conduct of LR. Practitioner feedback was obtained through a mailed survey of 440 stakeholders (319 clinicians and 121 administrators [hospital CEOs]). Respondents who indicated that the report was relevant to their clinical practice (n = 186) overwhelmingly (89% or higher) agreed with the report’s relevance, development methodology and recommendations. Issues raised in the written comments included concerns with the 20 supervised procedures recommended, issues with the mentoring process and issues related to implementing the recommendations, including time constraints.
Conclusion:
A standardized methodology was used to develop a CPG and standards document on LR in Ontario. Although widely supported by practitioner feedback, implementation issues will present a challenge.
A multi-faceted approach to facilitating quality improvement in Ontario
Introduction:
Provincial cancer quality data collected by Cancer Care Ontario (CCO) show practice variation in cancer surgery across the province which has a direct impact on patient outcomes. With over 1000 surgeons in Ontario practising in over 150 hospitals, the Surgical Oncology Program at CCO has sought to facilitate improvement in cancer surgery by initiating a multifaceted approach to improving quality.
Methods:
Over the past 3 years, CCO has developed a provincial surgical program that focuses on 4 facets: 1) developing and transferring knowledge on guidelines and standards, 2) facilitating communities of practice, 3) improving access through wait-time investments and 4) fostering an academic fellowship program and surgical stipends. These facets have functioned in a synergistic fashion to facilitate quality improvements.
Results:
Preliminary results have shown that this model has: enabled better adherence to quality guidelines; promoted skill development and enhanced capacity; strengthened local relationships; improved access to care; and empowered surgeons (and other clinicians) to collectively define quality issues and develop realistic local solutions.
Conclusions:
This presentation will illustrate current progress in rethinking the design and delivery of provincial surgical oncology quality improvement initiatives. A key focus will be sharing how we understand the impact of our efforts and translating their implications into program shifts. This process is iterative, and we endeavour to flex our approach to encompass new ways of thinking. We look forward to continuing to inform and enrich our understanding of the issues impacting our goal of improving quality in cancer surgery.
Evaluation of the risk factors for surgical site infection in breast cancer surgery
Introduction:
The surgical site infection (SSI) rate in breast cancer surgery (7.3%) is higher than the usually accepted infection rate for clean surgery (about 3%). There is controversy surrounding the use of prophylactic antibiotics in breast surgery, and certainly there is no clear existing guideline favouring its routine use. To be able to diminish the infection rate, it is therefore important to identify modifiable risk factors for SSI of the breast.
Methods:
We prospectively followed 186 patients operated (for a total of 200 interventions) for a period of 6 months for investigation or treatment of breast disease. Suspected SSI risk factors were sought. A complementary retrospective analysis of the medical records was made. A univariate and a multivariate analysis of the data were done.
Results:
Axillary dissection (odds ratio [OR] 3.81, 95% confidence interval [CI] 1.19–12.27) and hospitalization time (33.13 v. 22.84 h, p = 0.024) were both statistically significant on univariate analysis. Infection rates also varied significantly between surgeons (Fisher exact test, df = 3, p = 0.042). Multivariate analysis identified axillary dissection (OR 3.82, 95% CI 1.19–12.27, p = 0.025) as the only independent variable. Hospitalisation time was not retained at multivariate analysis because of heavy interaction with axillary dissection. This was confirmed by χ2 analysis of association.
Conclusion:
These results suggest that it could be possible to diminish the surgical site infection rate by establishing practice guidelines between the surgeons that would propose increasing ambulatory surgery as well as lowering the number of axillary dissections. This has been made possible by the advent of the sentinel node biopsy technique. In the future, it would be interesting to determine if substituting an axillary dissection by a sentinel node biopsy will reduce the incidence of SSI of the breast.
Women with locally advanced breast cancer are not at higher risk for contralateral synchronous breast cancer
Background:
Breast magnetic resonance imaging (MRI) may provide a more accurate assessment of synchronous contralateral breast cancer in select cohorts of patients. The utility of this imaging technique for detecting synchronous contralateral breast cancers in patients with locally advanced breast cancer (LABC) has not previously been described. We report our experience in assessing contralateral disease in a cohort of women with LABC who had clinical assessment, mammography, ultrasound and MRI before neoadjuvant therapy.
Methods:
Patients who presented with LABC, stage IIB (T3N0), stage III A/B, were identified from a prospectively kept database at a single tertiary care centre between Nov. 2001 and Nov. 2004. Charts were reviewed retrospectively, and demographic, imaging and pathologic variables were abstracted.
Results:
One-hundred and one female patients with LABC were identified who had a median age of 49 (range 27–83) years. One hundred of 101 patients presented with a clinically obvious LABC. Three patients had LABC that was not visualized mammographically but was detected on ultrasound and MRI. The majority (81%) of the LABC were invasive ductal carcinomas. Sixteen of 101 patients (16%) had contralateral imaging findings that required biopsy for diagnosis. Of the contralateral biopsies, 44% (7/16) were malignant (n = 2 ductal carcinoma in situ, n = 4 invasive ductal, n = 1 invasive lobular). These malignant lesions were identified clinically in 4 of 7 patients, on 7 of 7 ultrasounds, 7 of 7 mammograms and 5 of 5 MRI. Overall, 7% (7/101) patients had malignant synchronous contralateral disease.
Conclusions:
In our LABC cohort, 7% presented with malignant contralateral disease. The incidence of contralateral disease in women with LABC is comparable to patients who present with early-stage breast cancer. No single screening technique, ultrasound, mammogram or MRI appeared to be superior for identifying contralateral synchronous malignancy. It is unclear as to the significance of identifying synchronous contralateral disease in patients with LABC.
Improving the quality of surgery for gastric cancer: Are surgeons aware of the relevant quality indicators?
Background:
Gastric cancer survival in the West is inferior to that achieved in Asian centres. While differences in tumour biology may play a role, poor quality surgery contributes to understaging. The standard proximal margin of resection is recommended to be ≥ 5 cm; revision based on intraoperative frozen section is of benefit, and ≥ 15 lymph nodes is an adequate lymph assessment. We hypothesize that the majority of surgeons performing gastric cancer surgery in a North American setting are unaware of the recommended standards.
Methods:
Using the Ontario College of Physicians and Surgeons registry, surgeons who potentially include gastric cancer surgery in their scope of practice were identified. A questionnaire was mailed to 559 surgeons; 55% responded and 203 surgeons reported managing gastric cancer. Results were evaluated by χ2 and logistic regression; p < 0.05 was considered significant.
Results:
Eighty-six percent of respondents were male; 59% in urban nonacademic practice and 30% in academic practice. Forty-two percent of surgeons operate on 2–5 cases/year and 18% on > 5. One third of surgeons identified ≤ 4 cm to be the desired proximal margin. Frozen section is used by 52% to evaluate proximal margin status. Twenty percent were unsure of the number of lymph nodes needed to accurately stage; the median number reported by the remainder was 10 (range 0–30). Overall, only 16 of 203 identified the need for both a ≥ 5-cm proximal margin and ≥ 15 lymph nodes; this was too small a group to analyze for demographic associations. Surgeons who do > 5 gastric resections/year were more likely to report performing a D2 resection (p = 0.008).
Conclusions:
The majority of surgeons operating on gastric cancer in Ontario did not identify standard quality indicators of gastric cancer surgery. A continuing medical education program should be designed to address the knowledge gap, aiming to improve the quality of surgery and outcome of multidisciplinary management.
Defining the chemoresistant molecular profile of colorectal liver metastases: microarray analysis of stromal cells and tumour cells
Introduction:
The chemotherapeutic options for metastatic colorectal cancer are expanding, and it is currently difficult to predict which individuals would benefit from a particular regimen. Moreover, the role of tumour stroma in chemoresistance is poorly understood.
Methods:
As part of a phase II clinical trial of neoadjuvant 5-fluorouracil, leucovorin and CPT-11, core biopsies of colorectal liver metastases were taken before administration of chemotherapy. Tumours from patients who had partial responses (n = 4) were compared with those from patients who had progressive disease (n = 4). Laser capture microdissection (LCM) enabled separation of tumour cells and stromal cells, which were separately analyzed. Samples were pooled and hybridized on a 14k chip for cDNA micorarray analysis. To avoid dye bias, analysis was repeated following reverse labelling. Transcripts were considered to be differentially abundant if covariance was ≤ 0.5 and if the absolute value of the mean log ratio was ≥ 0.85 (i.e., > 1.8-fold change).
Results:
In chemoresistant tumour cells, 21 transcripts were more highly expressed, and 23 transcripts were less abundant. Interestingly, the molecular profile of stroma in chemoresistant tumours was similar to that of tumour cells, with some notable exceptions. There were 9 genes that were differentially expressed in tumour cells that were not found to be differentially expressed in stromal cells. Additionally, there were 7 transcripts that were upregulated specifically in stromal cells, including MMP7, apolipoproteins 1 and A1, early growth factor response I and left–right determination factor I.
Conclusion:
Stromal cells as well as tumour cells influence chemosensitivity. These initial results will be confirmed by replicative analysis of a larger data set. Definition of a reliable genetic signature that predicts chemoresistance will ultimately enable individualization of systemic therapy of metastatic colorectal cancer.
Identification of human colon cancer initiating cells
Introduction:
It has been shown that acute myeloid leukemia, breast and brain cancers contain a small subset of cancer stem cells (CSC) that drive tumour growth. Although CSC form a small proportion of the total tumour, they are the only cells able to initiate and sustain tumour growth. Our interest was to determine whether human colon cancers are driven by a subset of cancer stem cells.
Methods:
Using a xenotransplant assay, human colon cancer cells were implanted under the renal capsule of NOD/SCID mice at doses ranging from 2 × 106 to 1 × 104. To characterize the phenotype of the colon CSC, we separated cancer cells based on CD133 expression. The CD133− cells were injected at doses ranging from 5 × 104 to 2.5 × 105, and CD133+ cells were injected at doses ranging from 1 × 102 to 2 × 104. To determine the frequency of the colon CSC limiting dilution analyses were completed for both the bulk and CD133+ colon cancer cells.
Results:
Tumours developed in 6–21 weeks following the injection of bulk colon cancer cells and demonstrated histological features similar to the original tumour. Limiting dilution analysis showed that the frequency of colon CSC is 1 in 5.68 × 104 (95% confidence interval [CI] 1 in 3.4 × 104 – 1 in 9.3 × 104) bulk colon cancer cells. Following separation of the colon cancer cells based on CD133 expression we found that injection of as few as 100 CD133+ cells resulted in tumour formation. In contrast, despite the injection of large numbers of CD133− cells we only observed tumour growth in 1 out of 25 mice. Limiting dilution analysis demonstrated that the frequency of the CSC is 1 out of every 262 CD133+ cells (95% CI 1/129–1/534). This represents a 216-fold enrichment of the CSC fraction, as compared with bulk colon cancer cells. The expression of CD133 ranged from 5% to 32%, as assessed by flow cytometry, and the level of expression in xenografts was similar to that seen in the original tumours.
Conclusions:
We have established a xenotransplant model of human colon cancer. Using this model we have identified that colon cancers have a subset of CD133+ cells that possess the ability to initiate and sustain tumour growth. These findings provide strong support for the idea that colon cancer contains a CSC population. This may lead to the development of new therapeutic strategies directed specifically against the cells responsible for sustaining tumour growth.
Surgical oncology care: How adequately are Canadian general surgery programs training their residents?
Introduction:
The adequacy of training in surgical oncology during Canadian general surgery (GS) residency has not been formally studied. We developed a series of national surveys in an attempt to address this question.
Methods:
Four comprehensive surveys addressing knowledge, skills and attitudes in oncologic care were developed and sent to all Canadian graduating general surgery residents in 2005, recently graduated general surgeons (2003/2004) and program directors. Non-responders were contacted twice in follow-up.
Results:
Response rates were 18.3% from the residents and 23% from program directors. All of the directors stated their program had formal oncology training, while only 70% of residents stated the same. Residents reported low numbers of ambulatory skill exposure during their training that correlated with the directors’ results. Thirty-eight percent of residents felt uncomfortable performing hepatobiliary surgery, having performed < 5 surgeries as first assist and none as primary operator. All the directors believed this area should be a required competency of GS training and residents should complete a threshold number of cases. Relatively common procedures such as total thyroidectomy and ilioinguinal node dissection were performed infrequently, and 23% of residents stated they were uncomfortable doing these procedures. Directors overestimated the number of procedures being done. Of a comprehensive list of oncologic procedures compiled by the authors, residents felt 68% should be a required part of GS training, whereas directors felt only 59% would be appropriate. Low response rates by new graduates do not permit evaluation of how this training affects subsequent practice.
Conclusions:
This preliminary study would suggest that that GS residency programs do not provide adequate exposure for comfort and competency in “specialty surgery.” Ongoing assessment of new graduates is needed to further evaluate how this affects practice and if surgical oncology fellowship training corrects these deficiencies.






