Abstract
Introduction: The impact of local provision of specialty service on patients’ access to care was studied in Canada’s 13 health care jurisdictions where distance may be a barrier limiting access.
Methods: A cross-sectional study of routinely collected registry data in Ontario and Nova Scotia was performed. Liver transplant was chosen as an indicator service. Transplant rate, disease severity, urgency and outcome were studied in adult recipients of first liver transplants from 1993 to 2002. Provinces that provided liver transplants were compared with those that did not; Ontario regions that provided the service were compared with those that did not; and the period of time when liver transplants were available in Nova Scotia was compared with the time when they were not.
Results: Use varied widely between jurisdictions but was consistently higher in provider provinces, at 10.9 per million population (pmp) compared with 8.9 pmp in nonprovider provinces (p < 0.005). Use was higher in district health councils of Ontario that provided transplantation. A larger proportion of patients in provider regions had viral or alcoholic etiologies of disease than did those from nonprovider regions, who tended to have superior survival after transplant. Service interruption in Nova Scotia did not change use rates, with transplant rates remaining above average, at 12.0 pmp.
Conclusions: Differences in use between provider and nonprovider regions may reflect local service availability as well as local patterns of disease and patient referral. Expectations of patients that are established by local service availability persist after service is removed.
Travel time for patients to the point of care has been shown to affect access to care in England.1 The National Health Service (NHS) is the sole public provider of health care in Great Britain and northern Ireland. Currently, the principle means of NHS reform is to provide patients who require elective specialty care with more choices, in the hope that competition among providers will drive improvements in effectiveness and efficiency.2 In Canada, there are 13 health care jurisdictions, each responsible for the development, provision and regulation of health care delivery in their own region. Provinces or territories meet the challenge of changing health care requirements by setting their own priorities. One of the purposes of the Canada Health Act is to ensure that service is available to all residents of Canada.3 Portability provisions in the Act allow patients to seek treatment in another jurisdiction if services are not available in their own. A case can be made that, a single-payer system allows health services to grow more easily than with national health services with centralized care delivery systems.4 However, distance from a patient’s residence to the point of service, either within a jurisdiction or between provinces, may be so large in Canada that it becomes a barrier to health care.
Liver transplantation was chosen as an indicator to test the impact of a patient’s place of residence on access to specialty health care service in Canada. This procedure has evolved from an experimental service that was infrequently available on a compassionate basis to become standard therapy for a broad range of conditions that affect patients, without geographical limitations. Surgical liver transplant services are available at comparatively few sites in Canada and worldwide. Both elective travel and urgent travel from the patient’s residence to the transplant centre are required for successful completion of the entire transplantation process. In addition, distances between the centre and the site of organ donation vary according to population density. The indications and outcomes of transplant have been standardized, and data, which are collected comprehensively on a national basis, include the location of the donors, recipients and transplantation. Thus liver transplantation is an evolving travel-dependant service with high-quality clinical and geographical data. The prevalence of liver disease surpasses the ability to provide liver transplantation with up to 20% of transplant candidates dying before a suitable donor is located. This suggests that liver transplant would be an indicator more of service access than of disease prevalence.
Methods
Access to and outcome of liver transplant in Canada from January 1, 1993 through December 31, 2002 was assessed using data from the Canadian Organ Replacement Register. This registry, which resides at the Canadian Institute for Health Information, collects information on all liver transplants performed in Canada.5 Data analyzed related to the following: the patient at the time of transplant (sex, age, area of residence, cause of liver disease and severity of liver disease); organ donation (living v. deceased, location); and liver transplant (location, urgency, graft survival and patient survival at 1 year after transplant). Disease severity was calculated with the Model for End-stage Liver Disease (MELD), using creatinine, bilirubin and international normalized ratio of prothrombin time.6 In Canada, organ allocation is made according to a nationally agreed algorithm based on clinical need. Patients are assigned to 1 of 4 priority groups (designated 1–4), with a subcategory prioritization for fulminant liver failure (designated F).7 For the purposes of this review, urgent transplants referred to those in patients assigned a Canadian wait-list status of 3F, 4 or 4F; those in status 1, 2 or 3 were classified as nonurgent.
Rates and recipient characteristics (sex, age) were based on all recipients receiving first transplants within the period. Recipients (aged 18 years or older) of first liver transplants were allocated by location of residence to a province or territory and to a health care district that were determined to be providers or nonproviders of surgical liver transplant services. Retransplants and combination transplants were excluded. Yearly and cumulative analyses allowed for the following 3 comparisons: provider versus nonprovider provinces; provider versus nonprovider districts in Ontario and provider period versus nonprovider period in Nova Scotia. In Nova Scotia, surgical liver transplant services were provided until June 1, 2001, after which, patients received their liver transplant in London, Ontario. Nova Scotia was included as a provider province from the beginning of the study until June 1, 2001 and was ranked with the nonprovider provinces thereafter. In a separate analysis of Nova Scotia residents, the 18-month period before June 1, 2001 was designated as a provider period, and data were compared with the subsequent 18-month period, which was designated as a nonprovider period.
Statistical analyses were performed with SAS Enterprise Guide (version 2.05). Categorical data were compared with the chi-square test, and the Tukey’s t test was used for continuous data. A paired t test assuming different variances compared annual use rates during the period of interest. Differences between multiple groups were assessed with analysis of variance, and statistical significance was set at p < 0.05.
Results
Over the decade studied, 3 548 liver transplants were performed in Canada, for an annualized rate of 11.8 per million population (pmp). During the same time, the rate of liver transplant was 16.2 and 12.0 pmp in the United States and France, respectively.8,9 Liver transplant recipients came from all-over Canada, and the distribution of recipients mirrors the location of Canada’s population. Looking at first transplants only, there was a marked variation in transplant rates across provinces, from 4.1 pmp in the territories to 14.1 pmp in Nova Scotia (Table 1). Only 4 patients were resident in the territories at the time of transplant, so that comparison is not appropriate. However, the transplant rate in Nova Scotia was over 60% higher than 5 other provinces whose rates were less than 9 pmp in that time period. No differences were seen in the sex, age, or cause or severity of disease between the provinces.
Access to liver transplantation according to Canadian province of residence, 1993–2003
British Columbia, Alberta, Ontario, Quebec and Nova Scotia provided surgical liver transplant services. During the study period, there were 2865 deceased liver donors who had been resident in provider provinces and 340 in nonprovider provinces, giving equivalent donor rates (11.4 pmp for the provider group and 11.6 for the nonprovider group). The proportion of liver transplants from live donors was not statistically different in provider and nonprovider provinces (3.5% v. 1.5%, respectively).
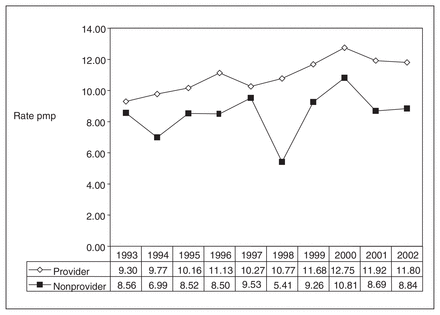
The cumulative transplantat rate was 22.5% less in patients from nonprovider provinces (8.9 pmp v. 10.9 pmp, p < 0.05). For each of the 10 years, there was a higher rate of liver transplant among residents of provider provinces, compared with those who lived in nonprovider provinces (Fig. 1). These differences were statistically significant (p < 0.05) for 1998 and 2002, and a paired analysis over the entire 10-year period was significant (p < 0.005).
Rate of first liver transplants per million population (pmp) by provider and nonprovider provinces for each year between 1993 and 2003. Provider provinces offer surgical liver transplantation services. Nonprovider provinces refer their patients to programs outside their province or territory.
Recipients from provider provinces were more likely to have viral or alcoholic cirrhosis, but liver disease severity was similar to recipients from nonprovider provinces (Table 1). Patient and graft survival at 1 year after transplantation was superior in the patients from nonprovider provinces (89% and 85%, respectively), compared with provider provinces (85% and 81%, respectively; p < 0.05).
Seventy percent of the population in Ontario lives outside of the Toronto and Thames Valley district health councils (DHCs), which provide surgical liver transplant services. The rate of liver transplant is significantly lower in nonprovider DHCs, compared with provider DHCs, even though differences in sex, age, diagnosis or disease severity are not seen (Table 2). Graft and patient survival rates at 1 year after transplant were similar in both groups.
Access to liver transplantation comparing District Health Councils in Ontario that provide surgical liver transplantation services and also comparing periods of provision and nonprovision of service in Nova Scotia
Interruption of surgical liver transplantation services was not associated with a reduction in the Nova Scotia liver transplant rate, with use during both provider and nonprovider periods (12.7 and 12.0 pmp, respectively) being above the national average (Table 2). One-year graft and patient survival rates were also similar during each period in Nova Scotia.
Conclusions
Access to care remains a concern in spite of substantial investment in health care delivery in Canada. For some, this is a result of the single-payer structure of health care. Although the recipient constituency offers an almost unanimous endorsement for the single-payer system, those working within it require frequent encouragement.10 Debate is essentially political, with limited data to support opinions. The Canadian Medical Association’s Physician Resource Survey 2000 shows a decline in satisfaction with access to specialist medical care.11 Regional differences were evident in the survey.
Despite the expensive, travel-dependant, and evolutionary nature of liver transplant and the extraordinary distances between Canadian communities, access to care is available everywhere in the country. The same is probably true of all acute care hospital services. Even with centralization and loss of local expertise, more “routine” services, such as maternity care, are available to residents of remote communities. In this respect, the goals of the Canada Health Act are fulfilled to a remarkable extent. This success comes at substantial personal inconvenience and nonmedical cost, but such barriers are overcome by patients accessing nonlocal services through a combination of government, community and family support.
In this study, differences were seen in the use of liver transplants by patients from provider provinces, compared with those from nonprovider areas. The apparent advantage of local service provision was not restricted to interprovincial comparisons but could also be seen in Canada’s largest province. Although some of these differences did not reach statistical significance, a higher rate of access was repetitively found over each time period in provider areas. Indications for liver transplant and protocols for organ allocation, which are shared and transparent across Canadian transplant programs, do not discriminate on the basis of patient residence. Donor location should not matter, and donor rates were found to be the same in provider and nonprovider regions.
Service interruption in Nova Scotia was not associated with a decrease in the rate of use. This suggests that, once patients’ expectations are established by the local provision of services, these expectations persist, at least in the short-term, despite service withdrawal. It is also possible that factors other than local service are related to the differences observed in this study. Such factors might include disease prevalence and etiology, physician referral pattern and patient relocation. The higher prevalence of viral and alcoholic causes of liver disease in recipients from the provider regions, which probably reflects the greater urban concentrations in these areas, may result in a different requirement for transplantation. The higher survival rate after transplantation in patients from nonprovider regions may reflect different referral patterns that favour patient referal at an earlier stage of liver disease. In a clinical needs-based priority system of transplant allocation, such a strategy would result in lower transplant rates. Although these factors may not completely explain a gap in the rate, higher rates of survival after transplant partially offset its impact, so that the potential gap in end-stage liver disease survival is smaller. This study does not document whether patients with liver disease move from nonprovider provinces or districts to be closer to the place of transplantation. Short-notice transplants using time-limited liver grafts that would otherwise have to be discarded are available only to local candidates.
The principal message in the data may not be that service use varies with distance from service provision but that considerable geographical challenges are overcome in Canada to provide access to specialty health care, regardless of the remoteness of residence. Portability provisions of the Canada Health Act are operational, so that access is available to evolving specialty services even if the service is not provided locally. This study does not deal with the financial impact of specialty heath care provision. In Canada, out-of-province care is provided on a full-cost recovery basis. Nonetheless, transfer of care to another jurisdiction has implications for local employment. It also has consequences for revenue collection that can amount to a provincial loss equivalent to 60% of the actual cost of care when income and consumption taxes are accounted for.12 Jurisdictional reviews regarding the impact of local versus distant care on the welfare of its citizens and on the cost of their health care will continue to stimulate evolution of health care within Canada’s single-payer system.
Footnotes
Competing interests: None declared.
- Accepted January 27, 2006.