Gastrointestinal stromal tumours (GISTs) are found most commonly in the stomach (60%–70%), followed by the small bowel (20%–30%), and the colon and rectum (5%).1 We describe a case of GIST in an unusual location (perianal) and highlight how both imaging and histology are essential in diagnosing and managing this tumour.
Case report
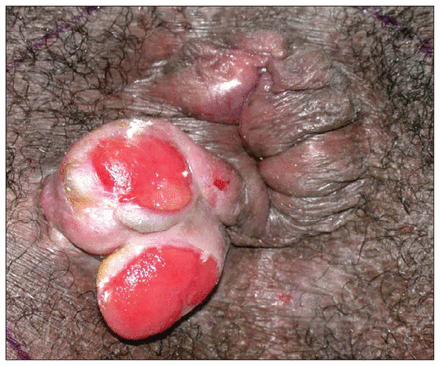
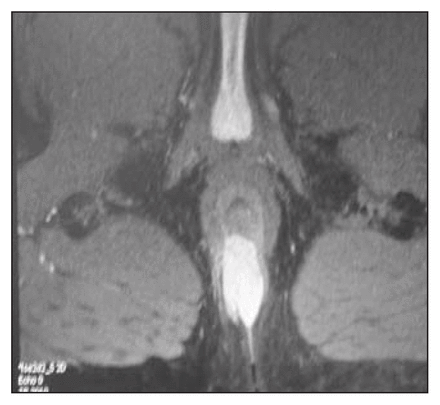
A 30-year-old man presented with a history of rectal bleeding and an associated cutaneous perianal lesion. Examination of the perianal area revealed a 2 × 4-cm lesion in the right posterior position (Fig. 1). Initial biopsies showed only nondysplastic epithelium (likely owing to sampling error). Because a malignant lesion was suspected, the man underwent a repeat biopsy. The pathologic findings suggested a spindle cell mesenchymal tumour suspicious for hemangiopericytoma or GIST. Rigid sigmoidoscopy to 10 cm was normal. A pelvic MRI demonstrated a heterogeneous, lobulated, solid mass of 1.7 × 3.1 × 4.6 cm, centred at the posterior midline of the external sphincter involving the internal sphincter (Fig. 2). The tumour, removed at abdominoperineal resection, was described as a spindle cell tumour (3.5 × 3 × 2 cm) extending into the perirectal soft tissue. The mitotic rate was < 1 in 10 high-power fields and immunohistologic stains were negative for c-Kit and positive for CD34. Despite negative c-Kit staining, the lesion was thought to be consistent with a GIST.
Perianal cutaneous extension of the tumour immediately before surgical resection.
MRI image illustrating tumour involvement of both internal and external sphincters.
Discussion
GISTs display a wide variety of malignant behaviours, and none of these tumours can be considered completely benign. A National Institutes of Health consensus statement ranks these tumours into 4 categories of risk of aggressive behaviour based on the tumour size and mitotic count.2 According to this classification, our patient’s tumour was low-risk; however, his young age at presentation may moderately increase the risk for aggressive tumour behaviour.3
These tumours are rarely found in the anus and rectum.1 What makes this patient’s rectal lesion even more unusual is the associated perianal skin lesion. Since these tumours arise from the muscularis propria and grow intramurally, the true extent of the tumour is best assessed by either CT or MRI. In this case, MRI was critical to our surgical planning; it changed our approach from a simple wide local excision of the apparent skin lesion to the abdominoperineal resection necessary to include the involved anal sphincters and perirectal soft tissue.
Traditionally GISTs have been resistant to conventional chemo- and radiotherapy. However, imatinib mesylate is a new agent that selectively inhibits the tyrosine kinases associated with the c-Kit protein. Patients with high-risk tumours should receive imatinib therapy, but its role in the treatment of intermediate and low-risk tumours is undefined. 4 Our patient’s tumour fell into the low-risk category and, uncharacteristically of GISTs, did not express the mutant c-Kit protein, making its response to imatinib uncertain.
Footnotes
Competing interests: None declared.
- Accepted September 25, 2006.