The local form of hepatic tuberculosis with no clinical extrapulmonary manifestations is relatively rare. Hepatic tuberculosis lesions that appear as masses larger than 2 mm in diameter are referred to as macronodular and pseudotumoural tuberculosis. In individual patients, lesions may be single or multiple. On the basis of imaging examinations alone, these lesions are virtually indistinguishable from many other focal lesions of the liver, such as hepatocellular carcinoma, metastases and Hodgkin’s disease, so pathological examination is necessary for diagnosis.1
Case report
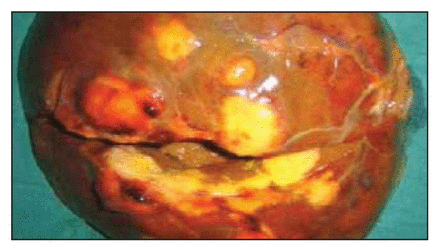
A 30-year-old man presented with complaints of upper abdominal pain for 1 month and significant weight loss. He denied drinking alcohol and smoking. He was thin and anicteric. No abnormality was seen on abdominal examination, esophagoduodenoscopy or colonoscopy. His hemoglobin was 11.8 g/L, total count 9.5 × 109/L, the differential count showed 65% polymorphs, 38% lymphocytes and 2% eosinophils; liver function test findings were within normal limits. The serum α-fetoprotein was 2.31 ng/mL (normal range 0–9.0 ng/mL), the carcinoembryonic antigen level was 1.47 ng/mL (normal range 0–3.0 ng/mL); and viral markers for hepatitis B and hepatitis C were negative. Ultrasonography showed a solid-appearing confluent hypoechoic mass lesion in segments 6 and 7 of the right hepatic lobe, measuring 8 × 5 cm. Contrast-enhanced CT showed a hypodense lesion with marginal nodular enhancement after intravenous injection of contrast in the arterial phase and filling of the pattern of enhancement with persistent opacification in venous and delayed phases, involving segments 6 and 7. MRI showed multiple, rounded, discrete and confluent space-occupying lesions that were hypointense in T1-weighted images and isointense to liver parenchyma on T2-weighted images. Lesions demonstrated a peripheral rim on T2-weighted images. On heavilyweighted images, the lesions did not demonstrate increased signal intensity, which was similar to conventional T2-weighted images. Fine-needle aspiration of the lesion gave inconclusive results. Diagnostic laparoscopy revealed a nodular lesion 5 × 3 cm in size in segment 6 and another nodular lesion 3 × 3 cm in segment 5 in the right hepatic lobe. A classical right hepatectomy was performed (Fig. 1). Histopathological examination of the excised specimen showed multiple foci of epitheloid granulomata with necrosis bordered by multinucleate giant cells (Fig. 2). The surrounding liver parenchyma showed lymphocytic infiltration within the portal tracts with occasional eosinophils. The findings were consistent with hepatic tuberculosis.
Hepatectomy specimen.
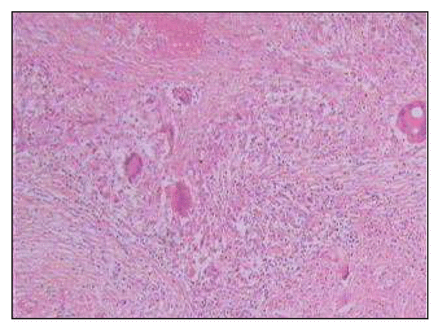
Multiple foci of epitheloid granulomata with necrosis bordered by multinucleate giant cells (hematoxylin–eosin stain).
Discussion
Liver involvement in tuberculosis, although common in both pulmonary and extrapulmonary tuberculosis, is usually clinically silent. Isolated hepatic tuberculoma (syn. nodular hepatic tuberculosis, macronodular hepatic tuberculosis) is perhaps the rarest form of local hepatic tuberculosis.2
Imaging techniques (ultrasonography, CT and MRI) are useful in making the diagnosis of tuberculoma or tubercular abscess. On CT, the liver tuberculoma appears as an unenhancing, central, low-density lesion owing to caseation necrosis with a slightly enhancing peripheral rim corresponding to surrounding granulation tissue.3 One of the typical CT features of hepatic tuberculosis might be multiple lesions of varying density, indicating that there are lesions in different pathologic stages coexisting in hepatic tuberculosis, including tuberculous granuloma, liquefaction necrosis, fibrosis or calcification.4 These findings, although suggestive of tuberculosis, have also been seen in necrotic tumours such as metastatic carcinoma and hepatocellular carcinoma.
MRI of hepatic tuberculosis shows a hypointense nodule with a hypointense rim on T1-weighted imaging and hypointense, isointense or hyperintense with a less intense rim on T2-weighted imaging, and peripheral enhancement or internal septal enhancement on postcontrast MRI.3,5 In our patient, lesions were hypointense in T1-weighted images and isointense to liver parenchyma on T2-weighted images. Lesions demonstrated a peripheral rim on T2-weighted images.
This report illustrates the difficulty in reaching a correct preoperative diagnosis of nodular hepatic tuberculosis that presents as a space-occupying lesion. It is usually unsuspected and confused with primary or metastatic carcinoma of the liver and, as in our case, it has necessitated hepatic resection. Acute awareness is required for diagnosis, which can be made only by histologic examination and polymerase chain reaction analysis. Such awareness may prevent needless surgical intervention.
Footnotes
Competing interests: None declared.
- Accepted May 17, 2006.