Multidisciplinary cancer conferences: exploring obstacles and facilitators to their establishment and function
Introduction:
There is increasing international evidence supporting the use of a multidisciplinary approach to cancer management to improve the quality of patient outcomes. The multidisciplinary cancer conference (MCC) provides an opportunity for key cancer professionals to evaluate and to discuss diagnosis and treatment options with the goal of providing optimal patient care. There have been no prior studies exploring the experiences of adopting and implementing MCCs in Canada.
Methods:
Using a grounded theory approach, this exploratory study triangulates the qualitative methods of interviews, participant observation and document analysis to explore the experiences of adopting and implementing MCCs in 4 hospitals in Ontario, Canada. Common themes emerging from the data were systematically coded using constant comparative analysis. Dominant concepts were assimilated to create a conceptual theory of the policy, administrative/organizational and participant level experiences of implementing MCCs.
Results:
Thirty-seven MCCs were observed across 3 hospital sites, and 48 interviews were conducted across a range of clinical specialists and administrators. The core conceptual category was the perceived value for time balance, which was variably influenced by policy factors, institution-based administrative factors and themes directly related to MCC structure and to participant interaction.
Conclusions:
Variation exists in the enthusiasm of cancer professionals and in the administrative capacity of institutions to adopt and routinely implement MCCs. Recognition of barriers identified in this study is important for creating provincial and hospital-based strategies to facilitate widespread dissemination of MCCs and to monitor their ongoing growth.
Staged liver resection for extensive bilobar colorectal liver metastasis
Introduction:
Liver resection offers the only potential for cure in patients with colorectal cancer liver metastasis (CRCLM). By present standards, 20% of patients are eligible for resection. Staged resection allows for liver regeneration and permits more extensive resection. This increases the number of patients eligible for resections with a curative intent.
Methods:
Patients who required staged resection for CRCLM at our institution were identified. The resection strategy is based on preservation of the middle hepatic vein and a liver remnant consisting of segments 1 and 4. All patients received neoadjuvant chemotherapy before the initial hepatic resection, as well as adjuvant chemotherapy following each liver resection. Ten patients (41.7%) underwent portal vein embolization.
Results:
Twenty-three patients were identified between January 2003 and April 2007. Sixteen patients (69.6%) completed the staged resections. The average number of lesions was 5.5, and the median clinical risk score was 3 (Fong et al. Ann Surg 1999;230:309–21). In the group that had a complete resection, the median disease-free survival was 1.6 years. The overall 1- and 4-year survivals were 93.3% and 78.8% in the completed resection group, and 57.1% and 28.6%, respectively, for the group that did not complete the staged procedure. The difference in survival was statistically significant (p = 0.01). There were no cases of liver failure.
Conclusions:
Staged liver resection based on preservation of the middle hepatic vein increases the number of patients eligible for resection with curative intent in patients presenting with initially unresectable CRCLM.
Getting from Dx to Sx: multivariate analysis of access to surgical care in a Canadian cohort of colorectal cancer patients
Background:
Current Canadian benchmarks for the time interval between diagnosis and surgery for cancer patients are 2 and 4 weeks. This study aimed to explore patient and system factors influencing the time interval between diagnosis and surgery in a Canadian cohort of colorectal cancer (CRC) patients.
Methods:
Between Feb. 15, 2002, and Feb. 15, 2004, all patients undergoing nonemergent surgery for primary CRC within a single health district were enrolled in a prospective consecutive cohort study. A standardized method was used to collect data. Associations between patient and health system factors, and the time interval between diagnosis and surgery, were analyzed using multivariate logistic regression.
Results:
The study cohort consisted of 362 patients, and the median time from diagnosis to surgery was 27 days. Overall, 55% of the cohort achieved the 4-week benchmark, and 25% achieved the 2-week benchmark. On multivariate logistic regression, patients with colon cancer (relative risk [RR] 2.7–4.0, p < 0.001), patients with stage II–IV tumours (RR 2.1–6.6, p < 0.05) and patients who did not undergo preoperative ultrasound or CT imaging (RR 2.3–3.3, p < 0.001) were more likely to achieve the 2- and 4-week benchmarks. Female patients were more likely to achieve the 2-week benchmark (RR 1.7, p = 0.04). Otherwise, no significant associations were identified between any patient or health system factors and the interval between diagnosis and surgery in this cohort.
Conclusions:
The majority of colorectal cancer patients may not be achieving benchmarked time intervals from diagnosis to surgery. Rectal cancer patients warrant particular attention, as does the relationship between preoperative imaging and the interval to surgery.
Hyperthermic intraperitoneal chemotherapy with oxaliplatin for peritoneal carcinomatosis arising from the appendix: preliminary results of a phase II study
Background:
Peritoneal carcinomatosis (PC) arising from the appendix is a rare disease for which the long-term prognosis is poor. The aim of this study was to evaluate the results of an aggressive treatment approach used in our institution in the last 5 years.
Methods:
Data from all patients with a PC arising from the appendix were prospectively collected and analyzed. Treatment consisted of complete surgical cytoreduction of the tumour followed by hyperthermic intraperitoneal chemotherapy (HIPEC) with oxaliplatin (460 mg/m2) in 2 L/m2 of dextrose (5%) in water at 43°C over 30 minutes. Ronnett’s histologic classification was used for tumour grading: disseminated peritoneal adenomucinosis (DPAM), peritoneal mucinous carcinomatosis with intermediate features (PMCA-I) and peritoneal mucinous carcinomatosis (PMCA).
Results:
From February 2003 to March 2007, 38 patients underwent laparotomy with curative intent. Mean follow-up was 23 months. Twenty-three patients received HIPEC, but 10 patients could not have complete cytoreductive surgery and received no HIPEC. Five patients with a negative second-look surgery also received no HIPEC. The 3-year overall survival (OS) was 100% for the negative second-look patients, 86% for the HIPEC patients and 29% for the unresectable patients (p = 0.0098). The 3-year disease-free survival (DFS) was 49% for the HIPEC patients. Histologic grade was a prognostic factor with regard to DFS for the HIPEC patients (p = 0.011). There was 1 postoperative mortality. The overall complication rate for treated patients was 39%, including intra-abdominal abscess (22%), hemorrhage (18%) and anastomotic leak (9%).
Conclusion:
Although these results are preliminary, this therapeutic approach seems both feasible and safe in selected patients.
Radiotherapy in rectal cancer can be limited to the minority of patients with a threatened or involved mesorectal margin
Introduction:
Current standards recommend radiotherapy for patients with stage II or III rectal cancer to decrease the risk of local tumour recurrence. But with good quality surgery this risk is largely driven by the presence of tumour at the mesorectal margin. We describe results of limiting radiotherapy to patients with a threatened or involved mesorectal margin.
Methods:
We reviewed the charts of consecutive patients treated with major resection by 1 surgeon (M.S.) for primary rectal cancer from 1999 to February 2006. Patient, tumour, treatment and outcome measures were compared for patients who did and did not receive radiotherapy. The main outcome of interest was local tumour recurrence. The mesorectal margin was assessed using a digital rectal exam — especially important for low lesions — and CT or MRI of the pelvis. A threatened margin demonstrated tethering on physical exam or inflammation on scan, while an involved margin demonstrated fixation on physical exam and direct involvement on scan.
Results:
There were 97 cases, and median follow-up was 2.7 years. Most cases were referrals from other surgeons. There were 52 (54%) nonradiated patients, and 56% of these had at least a stage II tumour. Radiated versus nonradiated patients were more likely to be younger (63 y and 73 y, respectively), and their tumours were more likely to be closer to the anal verge and fixed (p < 0.05 for all). While rates of wound infection were greater for radiated and nonradiated patients (22% and 8%, p < 0.05, respectively), colostomy rates, anastamotic leak rates and hospital length of stay were similar. In the radiated and nonradiated groups there were only 3 and 1 case of local recurrence (7% and 2%, p > 0.05), respectively.
Conclusions:
Radiotherapy in rectal cancer can be limited to the minority of patients with a threatened or involved mesorectal margin.
Treatment of colorectal cancer relapse in Ontario — a population-based analysis
Introduction:
Colorectal cancer (CRC) is one of the most common cancers in Ontario. Although surgical resection is the primary curative treatment modality, up to half of all patients are expected to have disease relapse. We sought to examine the use of surgery for disease relapse using Ontario administrative databases.
Methods:
CRC patients aged 18–80 years diagnosed between 1996 and 2001 were identified from the Ontario Cancer Registry. Patients with other primary cancers and those with relapse within 1 year were excluded. Linked hospital discharge abstracts and physician billings were examined for evidence of disease relapse, hepatic resections and pulmonary resections in 5 years of follow-up. Logistic regression analysis was used to explore factors associated with surgical resection.
Results:
Out of 12 804 patients who were disease-free 1 year after resection, 3316 patients had evidence of relapse by year 5 of follow-up. Overall, 234 (7.1%) of relapsed patients received a liver metastectomy, while 143 (4.3%) of patients received a lung metastectomy. The majority of liver and lung resections were performed in regions with academic centres. In the multivariable model, advanced age (p < 0.01) and increasing comorbidity (p < 0.01) were negatively associated with surgical resection. Higher socioeconomic status (p < 0.01), high-risk primary tumour (p < 0.01), body imaging frequency (p = 0.02) and diagnosis between 1999 and 2001 (p = 0.02) were positively associated with surgical resection for relapse.
Conclusions:
Lung and liver resections are performed in a minority of CRC relapses. Further study is needed to elucidate factors that further enable eligible patients to receive potentially curative surgery.
Germline genomic copy number variations in familial pancreatic cancer
Introduction:
The genetic basis of familial pancreatic cancer (FPC) is largely unknown. Germline genomic copy number variation (CNV) is a widespread form of human genetic variation. Germline CNVs affecting tumour suppressor genes or oncogenes may influence cancer risk. High-resolution single nucleotide polymorphism (SNP)–based DNA arrays can be used for genome-wide detection of CNVs in germline DNA. We hypothesize that discovery of FPC gene(s) is facilitated by identification of novel CNVs.
Methods:
Lymphocyte DNA was extracted from 47 FPC patients and assayed on the Affymetrix GeneChip® Human Mapping 500K SNP array (Affymetrix, Santa Clara, Calif.), consisting of 2 chips. Raw intensity data were analyzed with 2 algorithms using a hidden Markov model to estimate CNVs, with 25 healthy controls as reference. Only deletions were examined. Cases with CNV calls greater than 2 standard deviations (SD) from the mean number of calls were excluded. All single-SNP CNVs, and 2-SNP CNVs less than 1 kilobase in size, were excluded. CNVs overlapping by 20% or more between 2 algorithms and/or 2 chips were combined. Results were compared with CNVs previously identified in 1000 healthy controls.
Results:
Two cases had more than 2 SD CNV calls; in the remaining 45 cases, 100 unique CNVs were detected, with a mean size of 91 kilobases. Seventeen of 100 CNVs occurred on both chips, and 11 of 17 were detected by both algorithms. Eleven of 100 CNVs were present in more than 1 patient. Importantly, 37 CNVs were not present in any control samples, of which 22 contained known genes.
Conclusions:
Unique or rare germline copy number losses in FPC patients may lead to the discovery of putative tumour suppressor genes predisposing to FPC. Further annotation of these CNVs is in progress.
Patterns of invasive palliative interventions in patients with advanced hepatobiliary and pancreatic cancers
Introduction:
Invasive palliative interventions (IPIs) have been well described, however their frequency and timing near the end of life is poorly documented. This study examines the patterns of IPIs in palliative pancreatic and hepatobiliary cancer patients.
Methods:
The medical records of 295 patients referred to palliative care (PC) with advanced pancreatic (n = 161), biliary (n = 37), gallbladder (n = 27) and hepatic (n = 70) cancer between Jan. 2001 and Dec. 2004 were reviewed for IPIs. IPIs were classified as open/laparoscopic, endoscopic and interventional radiology (IR).
Results:
IPIs were required by 47.5% of patients. Indications for IPIs included biliary obstruction (n = 180), ascites drainage (n = 152), bowel obstruction (n = 25), pleural effusion (n = 8), urinary obstruction (n = 3) and pain (n = 3). Of the 385 IPIs, 268 (69.6%) were performed by IR, 61 were endoscopic and 44 were open/laparoscopic. Mean time from IPI to death was 5.6 (standard deviation [SD] 7.0) months; 58% of IPIs occurred before PC referral, and mean time from PC referral to death was 3.0 (SD 5.0; median 1.0) months. The means of IPI proximity to the end of life were 10.4 (open/laparoscopic), 6 (endoscopic) and 2.8 (IR) months, respectively (p < 0.001). Procedures in liver and gallbladder patients occurred closer to death relative to pancreatic and biliary patients (means 2.3 and 3.6 v. 6.5 and 6.6 mo; p = 0.022, respectively).
Conclusions:
Recognizing patterns of IPIs can optimize quality of care and is essential to understanding symptomatic disease trajectories at the end of life. Interesting findings include late referral to PC, and the various specialists performing these interventions. This exploratory study demonstrates the importance of IPIs in palliation and provides incentive for further study.
Prophylactic total gastrectomy (PTG) for hereditary diffuse gastric cancer (HDGC): the Newfoundland experience
Introduction:
Hereditary diffuse gastric cancer (HDGC) is an autosomal-dominant condition associated with germline mutations in the e-cadherin/CDH1 gene. Currently, it carries about an 80% lifetime risk of developing gastric cancer.
Methods:
We performed a retrospective chart review of 17 mutation-positive individuals who underwent prophylactic total gastrectomy (PTG) with Roux-en-Y reconstruction. This constitutes the largest reported series worldwide.
Results:
Median length of hospital stay was 13 (mean 25, range 10–107) days. Major complications included 3 patients with intra-abdominal abscesses: 2 associated with anastomotic leak requiring operative drainage and 1 from hematoma requiring percutaneuous drainage. One patient required surgery for small bowel obstruction 3 weeks after the initial surgery. Three patients had pulmonary emboli despite prophylaxis. There were no perioperative deaths. Extensive pathologic examination of the gastrectomy specimens revealed 7 of the 17 patients (41%) had microscopic foci of invasive signet-ring adenocarcinoma. All 7 patients were staged as T1NOMO, and none were offered adjuvant therapy.
Conclusions:
In our series, we found that PTG can be performed with an acceptable rate of major morbidity, although long-term outcomes and quality of life measures are currently lacking.
Thyroid PETomas: incidental thyroid focal uptake on PET/CT
Introduction:
Recent series of incidental thyroid activity on fluoro-2-deoxy-D-glucose and positron emission tomography (FDG-PET) in patients evaluated for non–thyroidal malignancy, which we refer to as a ‘PEToma,’ have suggested that such lesions are associated with a significant incidence of primary thyroid malignancy. We have reviewed our experience with PETomas of the thyroid.
Methods:
A total of 6457 FDG-PET scans performed on 4726 patients from May 2004 to March 2007 were retrospectively reviewed. The current study population included all those with focal activity described in the thyroid gland.
Results:
One-hundred and sixty patients (2.5%) were found to have incidental, abnormal FDG uptake in the thyroid gland, of whom 103 patients (118 lesions) had focal uptake, the PEToma group. Of these patients, 50 (48%) underwent further investigation including ultrasound (US) in 48, FNB in 38 and CT scan in 3. Ten patients underwent surgery, and differentiated thyroid cancer (DTC) was identified in 8, 3 of whom had micropapillary cancers. The remaining 53 PEToma patients underwent no further investigation. Interestingly, 6 patients who had focal uptake showed either resolution of the FDG-PET activity or no identifiable lesion on US.
Conclusions:
In those patients who underwent thyroidectomy, the incidence of DTC is similar to that in the literature. Although some patients will have falsely positive focal thyroid uptake on FDG-PET, we believe that evaluation of patients with focal activity within the thyroid on FDG-PET, at a minimum, requires ultrasonographic confirmation and FNB whenever a true lesion is documented.
Analysis of clinical applicability of the Breast Cancer Nomogram for positive sentinel lymph node: the Canadian experience
Introduction:
Completion axillary dissection is sometimes controversial after a positive sentinel lymph node (SLN). A model for predicting non–sentinel lymph node (NSLN) involvement has been developed and prospectively tested in several series. However, its clinical applicability has never been tested among surgeons.
Methods:
The Breast Cancer Nomogram (BCN) developed by the Memorial Sloan–Kettering Cancer Center was applied to a consecutive series of 209 SLN-positive patients. The performance of the BCN was assessed by the area under the receiver operating characteristic (ROC) curve. Surgeons in Quebec were surveyed to determine the predicted NSLN positivity below which they would not dissect the axilla. The accuracy of the BCN was determined in this clinically relevant range.
Results:
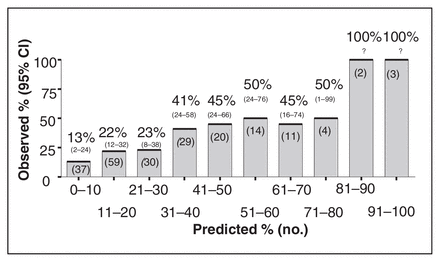
The predictive accuracy of the BCN had an area under the ROC curve of 0.687, matching other reported series. Almost half of interviewed surgeons treat over 20 breast cancer patients per year. Fourteen out of 82 surgeons questioned would never leave the patient without a completion axillary dissection after a positive SLN, regardless of the BCN result, while 71% of them would not complete axillary dissection if the prediction of a positive NSLN was 10% or less. However, only 37 of the 209 (18%) patients were in this 10% or less category, with a mean observed rate of positive NSLN of 13% (95% confidence interval 2%–24%). The false-negative rate among these 37 patients was 14%.
Conclusions:
The BCN performed fairly well in the whole cohort of patients. Prediction of a positive NSLN must be 10% or less to be clinically applicable and acceptable by the majority of our surgeons. Although useful, the BCN data should be used with caution at the low end of the scale. Because of some limitations in the performance in this category, other clinical factors and judgment must accompany its use.
IS A Level III axillary nodal dissection in malignant melanoma necessary following positive sentinel lymph node biopsy?
Introduction:
In malignant melanoma, level III axillary node dissection is the standard of care in treating sentinel lymph node (SLN)–positive disease. The curative intent of extensive nodal dissection has not been demonstrated in prospective randomized studies and is associated with considerable morbidity. The purpose of this study is to evaluate the involvement of level III nodes in both SLN-positive disease (subclinical nodal involvement) and clinically palpable disease. We hypothesize that a conservative nodal dissection (level I and II) would be of equal benefit in patients with SLN-positive disease as the current radical approach.
Methods:
All axillary dissections for melanoma undertaken at our institution were collected over an 8-year period (1999–2007). Forty-one axillary specimens were identified, presenting with positive SLN biopsy or with clinically palpable disease. Each was analyzed for the number of positive level III lymph nodes and for prognostic features.
Results:
A single positive level III lymph node was found in a patient with clinically palpable disease (p = 0.02). Ulceration, female patients and a preoperative nodal status of clinically palpable disease showed a high likelihood of having positive lymph nodes within the dissected basin. Breslow depth was found to be inversely related.
Conclusion:
The presence of a single positive level III node in 41 dissections (in a patient with clinically palpable disease) suggests that these nodes have limited involvement. Key prognostic indicators varied considerably with the established literature, and may be related to small sample size. The extensive level III axillary dissection for melanoma in patients with SLN-positive disease may not be necessary. In the absence of prospective randomized data, patients may be equally well served with a more limited (level I/II) axillary dissection.
The double-edged sword: preoperative MRI in early breast cancer
Introduction:
Preoperative breast MRI has been suggested as an adjunct to conventional imaging in early-stage breast cancer. The objective of this study is to determine the impact of preoperative bilateral breast MRI on perioperative and surgical management.
Methods:
This study is a retrospective review of a prospective database. Two-hundred and seventy (270) female patients with early breast cancer presented to the Princess Margaret Hospital from January to December 2006. Onehundred and thirty-six (136) patients underwent routine preoperative bilateral breast MRI (MRI group), and 134 did not (controls). For each patient in the MRI group, an assessment was made whether their MRI results affected their management and whether this change was beneficial.
Results:
MRI resulted in a change in management in 56 of 136 patients (41%). Thirty-six patients in the MRI group (26%) had additional preoperative imaging, 25 patients (18%) had additional biopsies, and 44 patients (32%) had a change in their planned surgery. MRI correctly identified a second focus of occult invasive cancer in 15 patients (11%) and ductal carcinoma in situ in 5 patients. The change in management was considered beneficial in 20 patients (removed occult cancer or prevented second surgery), detrimental in 12 patients (unnecessary surgery or biopsy) and neither detrimental nor beneficial in the rest. Median time to surgery was not significantly longer in the MRI group compared with controls (25 v. 23 d). With a median follow-up of 13.5 months, there has been 1 local recurrence in the MRI group.
Conclusions:
Preoperative MRI detects additional breast cancers but at the cost of unnecessary interventions.
Quality indicators for sentinel lymph node biopsy: development through a multidisciplinary consensus process
Introduction:
Sentinel lymph node biopsy (SLNB) is rapidly becoming the preferred method for axillary staging in the treatment of invasive breast cancer. The quality of training and implementation, however, has been inconsistent and may be influencing patient outcomes. Currently, there are no performance measures or “quality indicators” from which SLNB can be evaluated. The aim of this study was to establish consensus on quality indicators in SLNB through a multidisciplinary expert panel.
Methods:
A literature search using MEDLINE was performed independently by 2 investigators for studies evaluating SLNB training, practice, performance measures or outcomes published in English between 1996 and August 2007. Concepts from the literature review were abstracted and transposed into quality indicators. Development and consensus on quality indicators was performed using a modified Delphi process and a nominated multidisciplinary expert panel. Input from the panel was provided through 2 survey iterations followed by an in-person meeting where consensus on the final quality indicators was reached.
Results:
A total of 22 potential quality indicators were abstracted from the literature review. Panelists suggested 2 additional potential indicators. The in-person consensus meeting of the entire expert panel resulted in 11 final quality indicators for SLNB (Table 1).
Conclusions:
A modified Delphi consensus process was used successfully to develop meaningful, clinically relevant quality indicators for SLNB. Future evaluation of SLNB in practice can now be performed to assist clinicians in providing care of the highest standard to women with breast cancer and to identify areas where improvements can be made.






