Intravascular knotting of Swan–Ganz catheters (SGCs) is a rare complication, with fewer than 100 reports in the literature. Knotted SGCs usually require special surgical or interventional radiologic techniques for safe removal.1
We report a case of successful transfemoral removal of a knotted SGC that had been inserted through the subclavian vein. This avoided a transthoracic surgical procedure.
Case report
A 79-year-old woman was admitted to our intensive care unit (ICU) because of end-stage heart failure accompanied by respiratory insufficiency. On the seventh day, routine radiography revealed a “bow-tie” knot near the distal end of an SGC that had been inserted through the right subclavian vein. We were able to pull the knot back into the subclavian vein, but attempts to undo the knot and remove the catheter were unsuccessful. An open surgical approach was deemed necessary.
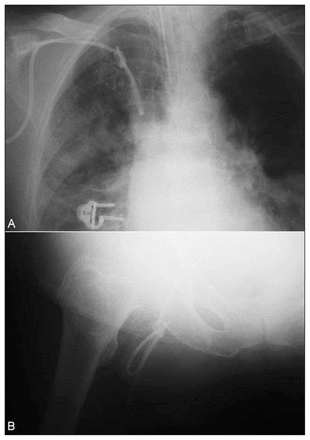
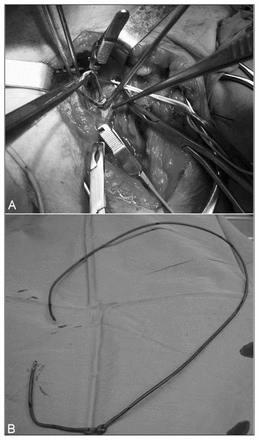
To avoid a stressful transthoracic procedure for removing the catheter, we chose an alternative route through the right common femoral vein. Under fluoroscopic guidance, the catheter was relocated from the superior vena cava through the right atrium into the inferior vena cava and forwarded to the right common femoral vein (Fig. 1). The vein was exposed surgically in order to capture the catheter. Thereafter, the proximal segment of the catheter at the subclavian entry point was cut, and the catheter was heterotopically pulled out through the femoral vein (Fig. 2). The heart was monitored throughout the procedure, and broad-spectrum antibiotics were given. The patient returned to the ICU where cardiac monitoring was continued. No cardiac or other surgery-related complications were recorded.
(A) Radiograph showing the Swan–Ganz catheter inserted through the right subclavian vein with a “bow-tie” knot near its distal end, which is at the level of the superior vena cava. (B) Radiograph showing the catheter relocated in the right common femoral vein.
(A) Surgical exposure of the right common femoral vein and removal of the knotted distal end of the Swan–Ganz catheter from the vein. (B) The knotted catheter after its removal.
Discussion
Knotting of SGCs is rare. Pulmonary artery catheters seem to be responsible for more than two-thirds of knotted intravascular catheters.1 The reason for this complication is not clear. The fact that SGCs are thin-walled, long and soft, and are usually placed without fluoroscopic control, and that there is turbulent blood flow in the cardiac cavities, may contribute to knot formation. Once knotting occurs, the catheter is almost impossible to remove without surgical or radiologic intervention. The latter has been reported to resolve the problem in up to 62% of cases.1
When interventional radiologic techniques have failed to undo the knot, aggressive surgical techniques are required for orthotopic catheter removal. In such cases, the standard surgical procedure to obtain adequate proximal control of the vein to allow a safe venotomy and knot removal requires clavicle disarticulation and in many cases additional median sternotomy.2 However, this procedure is stressful and dangerous when the patient is already critically ill. There are reports in the literature in which the knotted catheters were left in situ instead of being removed, but this option predisposes to undesirable complications such as venous thrombosis or septic complications and may lead to increased mortality.1,3 To avoid the risks of major surgery for SGC removal and without leaving the SGC in situ we proposed an alternative approach: heterotopic transfemoral surgical removal of the SGC after it had been guided to the femoral vein with interventional radiologic assistance.
Although the alternative removal method was successful and uncomplicated in our patient, several risks exist. In particular, special attention should be paid during relocation of the knot to the inferior vena cava through the right atrium, in order to avoid myocardial or tricuspid valve damage or trapping the knot in the cardiac cavities. Also, navigation of the knot into the veins should be performed gently to avoid lacerating major veins. Finally, intensive cardiac monitoring should be provided intraoperatively and postoperatively to detect and treat any arrhythmias provoked by the passage of the catheter through cardiac cavities.
In our opinion, heterotopic transfemoral removal of a knotted SGC inserted through the subclavian vein is a viable alternative to an orthotopic transthoracic surgical approach, when interventional radiologic techniques have failed to resolve the problem.
Footnotes
Competing interests: None declared.
- Accepted May 10, 2007.