Schwannoma is a benign tumour arising from Schwann cells of the peripheral nerve sheath; histologic predominance of degenerative findings is typical of a rare variant, the “ancient” schwannoma.1–3 Retroperitoneal pelvic localization of these tumours is quite rare.4,5 Even more exceptional is development in the perineal area, which we report here.4
Case report
A 64-year-old man complained of a painless mass in the perineum, giving rise to discomfort in a certain sitting position and to mild dysuria. On physical examination there was an irreducible, hard, thick mass in the anterior perineal area, on the left of the raphe.
Sonography revealed a large, solid mass in the urogenital triangle, extending from the membranous urethra to the perianal area and compressing the corpus spongiosum of the urethra and the fixed portion of the left corpus cavernosum.
Computed tomography (CT) confirmed a solid, bilobate, well-demarcated mass, measuring 15 × 9 cm, in the left ischiorectal fossa, with heterogeneous contrast enhancement in the arterial phase. The mass caused compression on the left corpus cavernosum, at the radix penis level, laterally on the internal obturator muscle and medially on the levator ani muscle.
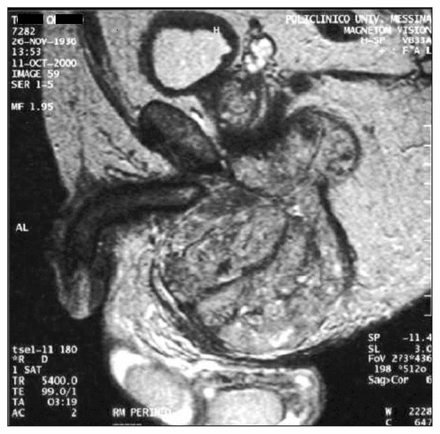
Magnetic resonance imaging (MRI) confirmed the presence of a well-encapsulated mass in the left perineum, with dishomogeneous signal intensity both on T1- and T2-weighted sequences (Fig. 1). Retrograde urethrocystography revealed compression on the proximal portion of the urethra and mild urinary retention on the postvoiding study.
Magnetic resonance imaging sagittal T2-weighted image (repetition time 5400 ms, echo time 99 ms). The bilobate perineal mass appears well encapsulated and not homogeneous. Compression without infiltration of the left corpus cavernosum is clearly visible.
Histologic examination of the echo-guided needle biopsy specimen revealed that the lesion was composed of spindle cells with elongated nuclei without atypias.
Through an arcuate incision in the urogenital triangle, a capsulated mass was excised that was attached, in the upper pole, to the tendinous arch and iliococcygeus portion of the levator ani muscle.
The tumour, weighing 300 g and measuring 17 × 9.5 cm, was ellipsoid in shape, of hard elastic consistency and exhibited a pseudocapsule.
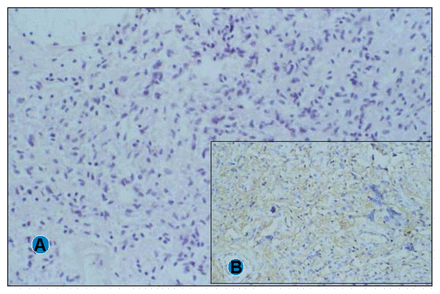
Microscopically, the neoformation was characterized by the classic biphasic pattern of Antoni A and B areas (Fig. 2), with fairly closely packed spindle cells having tapering elongated nuclei; infrequent but distinctive Verocay bodies were present. Focal degenerative changes, including microcystic formation and hemosiderin deposits with occasional calcification, were not uncommon. The neoformation was composed predominantly of Schwann cells as shown by immunoreactivity in neoplastic elements for S-100 antibody (Fig. 2); all other antibodies tested were negative. The histopathological diagnosis was “ancient” schwannoma.
Microscopic examination of the tumour shows (A) a biphasic pattern of Antoni A and B areas and infrequent but distinctive Verocay bodies (hematoxylin–eosin stain, original magnification × 40). (B) There is immunoreactivity in neoplastic elements for S-100 antibody (hematoxylin–eosin stain, original magnification × 10).
The patient was discharged on the seventh postoperative day, with normal urine test results. At 48 months’ follow-up, the patient showed no evidence of recurrence.
Discussion
Perineal tumours are uncommon and are malignant in 66% of cases.2–4 Preoperative diagnosis is difficult since both benign and malignant tumours typically present as an asymptomatic enlarged perineal mass.4
Benign schwannoma is an encapsulated nerve-sheath neoplasm originating from Schwann cells. These tumours are more frequently located in the head, neck, upper and lower extremities and trunk; retroperitoneal localization is unusual,4 and development in the perineal area is extremely rare.4
Perineal schwannoma, like schwannomas occurring in the retroperitoneal space, are of considerable dimensions and may exhibit areas of spontaneous degeneration and hemorrhage, typical of the “ancient” variant.
A MEDLINE search showed that very few cases have been reported in the literature. In most of the cases described, symptoms are related to compression on the close structures; a giant ancient schwannoma located in the perineal space may lead to compression on the adjacent organs, especially the urethra and rectum, with onset of related symptoms.
In the presence of a large well-encapsulated expansive mass in the perineal region without CT or MRI findings of infiltration of the surrounding structures, a diagnosis of neurinoma, even if rare, should be considered.1,2
Magnetic resonance imaging, with multiplanar images, is particularly valuable not only in predicting the feasibility of tumour resection, but also for long-term follow-up.
The treatment of choice for benign schwannoma is complete excision; relapse appears to be associated with incomplete resection.4,5
Partial resection may be preferred when the mass is in close proximity to other organs to avoid iatrogenic damage (neural deficit, vessel lesions) that has been reported in 10% of cases.4
The benign or malignant nature of perineal tumours can be established only on definitive histologic examination; percutaneous biopsy may be useful for classifying the lesion.1,3
The expression of high concentrations of S-100 protein in the cytoplasm of tumour spindle cells on immunostaining is useful in the differentiation of a benign schwannoma from a malignant peripheral nerve sheath tumour and from other benign spindle cell tumours. Schwannomas rarely undergo malignant transformation, for which the prognosis is poor.1,3,5
Footnotes
Competing interests: None declared.