Hemobilia is a rare and potentially life-threatening cause of upper gastrointestinal bleeding.1 We describe the unusual case of a patient in whom massive hemobilia occurred after Roux-en-Y hepaticojejunostomy.
Case report
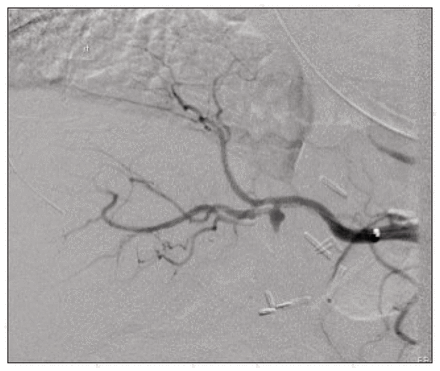
A 68-year-old man taking anticoagulants who had previously undergone an ileal conduit urinary diversion for remote bladder cancer presented with acute cholecystitis. He underwent laparoscopic converted to open cholecystectomy. The postoperative pathology report revealed gallbladder adenocarcinoma (pT1a) extending into the cystic duct margin. The patient underwent subsequent cystic stump and total bile duct excision, with portal and retroduodenal lymph node dissection and Roux-en-Y hepaticojejunostomy. Surgeons used a 5–0 polypropylene stitch to control a short-lived arterial bleeder caudal and to the left of a scarred porta hepatis. He was discharged on postoperative day 15 after an episode of pyelonephritis and minor wound infection. Four days later, the patient presented with chest pain, tachycardia (121 beats/min) and hypotension (95/67 mm Hg). Blood test results revealed normal hemoglobin and serum total bilirubin levels but an elevated troponin level, and his international normalized ratio was 2.3. An electrocardiogram showed evidence of acute coronary syndrome. He received intravenous heparin and clopidogrel bisulfate; we conducted urgent cardiac catheterization, and his heart appeared normal. However, the patient’s blood pressure dropped substantially, and his level of consciousness deteriorated (Glasgow Coma Scale score 6), requiring urgent mechanical ventilation. After transfer to the coronary unit, massive hematemesis ensued. Subsequently, the patient’s hemoglobin level was 33 g/L and total bilirubin 86 mg/dL (1471 μmol/L). Urgent gastroscopy revealed massive nasopharygeal bleeding flowing to the esophagus and stomach, which we treated with nasopharyngeal packing. Owing to persistent bleeding, we ordered a triphasic computed tomography (CT) scan of his liver, which showed normal results, and a repeat endoscopy, which revealed mild nasogastric tube trauma to the esophagus and stomach and a small duodenal ulcer with no active bleeding. The patient’s total bilirubin level continued to rise in association with his decreasing hemoglobin level. He underwent abdominal angiography, which showed no active bleeding. The next day, however, review of the films suggested a 1.5-cm pseudoaneurysm at the origin of the right hepatic artery (Fig. 1). We conducted an urgent angiography and deployed a balloon-expandable stent; follow-up images showed resolution of the pseudoaneurysm (Fig. 2) with decreased left hepatic artery flow. We discharged the patient on day 30 with no sequelae, and he remained well 26 months later with patent right and left hepatic arteries shown on Doppler ultrasound.
Angiogram showing an aneurysm of the common hepatic artery.
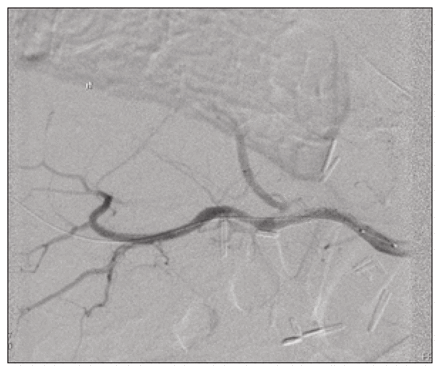
Angiogram showing the aneurysm after insertion of a stent.
Discussion
Hemobilia is caused by a communication between the splanchnic circulation and the biliary tree. The classic triad of symptoms are biliary colic, melena (or hematemesis) and jaundice. The most common cause is liver biopsy, but it may also follow parenchymal liver intervention.2 Other etiologies include trauma, malignancy, arteriobiliary or arterioportal fistula and pseudoaneurysm of the hepatic arteries. The literature highlights that a high degree of suspicion is always required, and the same can be concluded in our report. The development of an acute coronary syndrome, anticoagulation and massive nasopharyngeal bleeding clearly contributed to a delay in diagnosis in our patient. Nevertheless, the association of massive bleeding with increasing total bilirubin in the face of a recent hepatobiliary procedure should have prompted earlier angiography. Hepatic triphasic CT was not helpful, but abdominal angiography ruled out bleeding from either the hepatic or enteral anastomoses of the Roux-en-Y reconstruction. It also allowed for both accurate diagnosis of the right hepatic artery pseudoaneurysm and successful treatment by insertion of an expandable covered metal stent. We believe this aneurysm to have been a direct result of arterial iatrogenic injury incurred during the second operation. Although pseudoaneurysms of the cystic artery3 and the right hepatic artery4 after cholecystectomy have been reported, to our knowledge ours is the first report of hemobilia after Roux-en-Y reconstruction.
This case report illustrates that, no matter the context, clinicians should have a high index of suspicion when a patient presents with massive gastrointestinal bleeding, a climbing total bilirubin level and recent hepatobiliary intervention or manipulation. This is especially true if gastroscopy offers no clear cause. We suggest that both diagnosis and treatment can be achieved with early visceral angiography.
Footnotes
Competing interests: None declared.