Abstract
Background: A gap exists between the best evidence and practice with regards to surgical site infection (SSI) prevention. Awareness of evidence is the first step in knowledge translation.
Methods: A web-based survey was distributed to 59 general surgeons and 68 residents at University of Toronto teaching hospitals. Five domains pertaining to SSI prevention with questions addressing knowledge of prevention strategies, efficacy of antibiotics, strategies for changing practice and barriers to implementation of SSI prevention strategies were investigated.
Results: Seventy-six individuals (60%) responded. More than 90% of respondents stated there was evidence for antibiotic prophylaxis and perioperative normothermia and reported use of these strategies. There was a discrepancy in the perceived evidence for and the self-reported use of perioperative hyperoxia, omission of hair removal and bowel preparation. Eighty-three percent of respondents felt that consulting published guidelines is important in making decisions regarding antibiotics. There was also a discrepancy between what respondents felt were important strategies to ensure timely administration of antibiotics and what strategies were in place. Checklists, standardized orders, protocols and formal surveillance programs were rated most highly by 75%–90% of respondents, but less than 50% stated that these strategies were in place at their institutions.
Conclusion: Broad-reaching initiatives that increase surgeon and trainee awareness and implementation of multifaceted hospital strategies that engage residents and attending surgeons are needed to change practice.
Surgical site infections (SSIs) are the most common complication following surgery, with reported rates ranging from 5% to 30%.1 The attributable morbidity and mortality is significant, with patients who experience SSIs being 60% more likely to spend time in the intensive care unit, 5 times more likely to be readmitted to hospital and twice as likely to die than patients without SSIs.2 Whereas many risk factors for the development of SSIs are related to patient characteristics that cannot be easily modified, there are a variety of system or hospital factors that can be manipulated. These include improper selection and administration of antibiotic prophylaxis, intraoperative hypothermia and intraoperative hyperglycemia.3
Despite clear evidence and guidelines to direct SSI prevention strategies, compliance is uniformly poor.4 For example, Hedrick and colleagues3 reported baseline compliance with appropriate timing of antibiotic prophylaxis in only 68% of patients having elective colorectal surgery. This same study also revealed that 36% of patients arrived in the postanesthetic care unit with core temperatures less than 36°C.3 Forbes and colleagues5 found that as few as 5% of patients received their preoperative antibiotics within 60 minutes of surgery and that as many as 40% were admitted to the recovery room with core temperatures below 36°C. Another audit of 1763 patients at 13 Dutch hospitals revealed that overall adherence to a hospital guideline for antibiotic prophylaxis was achieved in only 28% of patients.6 These studies are just a few examples that highlight the gap between evidence and practice and emphasize the importance and need for tailored knowledge translation strategies to improve adherence to guidelines.
Knowledge translation has been defined as follows: “the exchange, synthesis and ethically sound application of knowledge (…) to accelerate the capture of the benefits of research, is the field of study which examines the effectiveness of various strategies for achieving quality improvement among different stakeholders in a variety of settings.”7 Unfortunately, this process can be slow, incomplete and faced with many barriers.8 It has been established that educational materials and meetings on their own have unreliable or minimal influence on care delivery, therefore other mechanisms are required to achieve desirable changes in practice.4 Some guidance for strategy selection is provided by the Pathman model, which describes 4 key steps to knowledge translation: awareness, agreement, adoption and adherence.9 While not necessarily a linear process, a different approach may be necessary for each step to influence change.4,9 Hence, to select the most appropriate implementation strategy, it is crucial to perform a needs assessment to identify the level of stakeholders on the knowledge translation continuum for the particular clinical problem of interest.10,11
The present study describes the results of a survey used to gauge awareness, agreement, adoption of and adherence to SSI prevention strategies among general surgeons and general surgery residents. The survey was designed to identify the type of implementation strategies needed to increase adherence to recommended SSI prevention practices. It was part of a more comprehensive initiative designed to improve SSI prevention among teaching hospitals affiliated with the University of Toronto.12
Methods
Participants and environment
All attending general surgeons and general surgery residents affiliated with the University of Toronto were invited to participate in this study. The staff surgeons practised at 1 of 5 academic teaching hospitals or 2 community-affiliated hospitals. The surgical residents typically rotated through all of these sites. The survey was distributed to 59 attending surgeons and 68 residents.
Survey design
A group of experts, including surgeons, residents and knowledge translation experts, designed the survey to assess beliefs, knowledge and practices of attending general surgeons and general surgery residents on issues related to SSI prevention, abdominal wound closure, deep vein thrombosis prophylaxis, mechanical bowel preparation, ventral hernia repair and the use of drains. The present study reports only the results of the 16 questions in 5 domains pertaining to SSI prevention. These 5 domains included methods used to prevent SSIs in general surgery patients, types of SSIs that surgeons believe are prevented by the use of antibiotic prophylaxis, specific factors that are important to consider when making decisions about antibiotic prophylaxis, perceived barriers preventing patients from receiving appropriate timing and duration of antibiotics and strategies already in place or that should be implemented to reduce SSI rates at respondents’ hospitals.13
Survey distribution
The survey was distributed along with an email invitation to participate. A reminder email was sent out 3 weeks after the initial email. A paper copy of the survey was also mailed with a self-addressed, stamped envelope. Finally, another email reminder was sent to all nonresponders 6 weeks after the initial email. Completion of the survey was voluntary. Results were collected and compiled by a web-based program (ASP.NET). Responses were then transferred to a Microsoft Access database for analysis. Ethics approval was granted by the research ethics boards of all participating hospitals.
Results
The overall response rate was 60%. The distribution of response rates is shown in Table 1; the rate was 68% (40 of 59) among attending surgeons and 53% (36 of 68) among residents. There was a higher response rate among residents in postgraduate year (PGY)-3 and above. The response rate of attending surgeons was distributed across the participating hospitals. In general, the responses of the attending surgeons and residents were similar and are therefore aggregated. All respondents answered all of the questions.
Distribution of response rates for survey on SSI prevention
Knowledge and perceptions regarding evidence supporting SSI prevention strategies
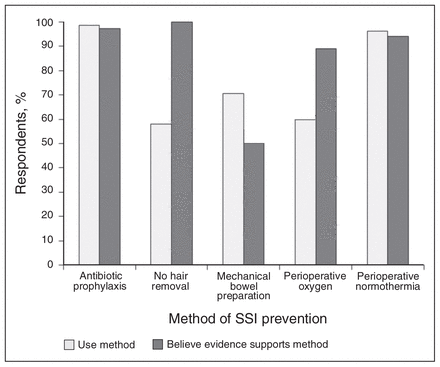
Figure 1 shows evidence-based strategies for preventing SSIs, the perception of the evidence and the extent to which the strategies are used by the respondents. There was inconsistency in some areas between the perception of evidence and the rate of strategy use. For example, more than 90% of respondents believed there was strong evidence to support the use of antibiotic prophylaxis and perioperative normothermia, and consistent with this perception, rates of reported use of this strategy were similarly high. By contrast, there appears to be a gap between perception and practice in the area of preoperative bowel preparation, hair removal and perioperative oxygen supplementation. For example, 71% of respondents reported prescribing preoperative bowel preparation even though less than 50% of respondents believe that evidence supports this practice. Conversely, the responses pertaining to no preoperative hair removal and perioperative hyperoxia indicated that although surgeons are aware of the evidence supporting these SSI preventation measures, they are not being used.
Beliefs and practice patterns regarding methods to prevent surgical site infections (SSIs).
Types of infections that surgeons believe are prevented by the use of antibiotic prophylaxis
Almost 90% of respondents believed that antibiotic prophylaxis is “important” or “very important” in preventing superficial SSIs. However, a much smaller proportion of respondents were aware that antibiotic prophylaxis is important in the prevention of other SSIs (deep or organ space). In addition, there was limited awareness that appropriate antimicrobial prophylaxis reduced rates of hospital readmission and shortened length of stay in hospital (Table 2). Only 8% of respondents felt that antibiotic prophylaxis was “important” or “very important” in preventing death.
Respondents’ ratings of “important” or “very important” for the administration of antibiotic prophylaxis to prevent the adverse postoperative outcomes*
Factors considered to be important in making decisions about antibiotic prophylaxis
When asked how decisions regarding antimicrobial pro-phylaxis were made, respondents reported that published practice guidelines were “important” or “very important” in influencing practice (Table 3). By contrast, hospital policies or protocols, computerized decision-support tools and standard pharmacy medication sets were considered to be less important by most respondents.
Respondents’ ratings of “important” or “very important” for factors to consider when making decisions about antibiotic prophylaxis*
Perceived barriers preventing patients from receiving appropriate timing and duration of antibiotics
As shown in Table 4, most respondents felt that performing concurrent tasks and lack of verbal communication among staff were the most common reasons for failing to administer antimicrobials within the effective time window. However, the range of responses suggests that multiple factors contribute, including a lack of clarity on who is responsible for administering the antibiotics, unanticipated changes in cases and the inconvenience of mixing antibiotics.
Respondents’ ratings of “important” or “very important” for factors influencing the timing of initiation and duration of antibiotic prophylaxis administration*
Implementation of strategies to reduce SSI rates
This aspect of the survey demonstrated a large disparity between existing practices and strategies that are thought to be helpful in reducing SSIs. Operating room checklists, standardized written orders, departmental protocols or clinical pathways and formal surveillance programs were felt to be the most useful strategies for reducing SSI rates. More than 75% of respondents felt these should be implemented, yet less than half indicated that these strategies were already in place at their hospitals. Two-thirds of respondents felt that provider-specific feedback should be implemented at their hospitals, but only 10% reported that a mechanism for feedback was currently in place. These responses are summarized in Table 5.
Proportion of respondents who believe the following strategies are in place or should be implemented at the hospital level to reduce SSI rates*
Discussion
Although strong evidence and guidelines exist that recommend a variety of SSI prevention strategies, compliance with this evidence has generally been described as poor.14–17 We performed a needs assessment to understand the context within which surgeons make decisions and to identify potential barriers of evidence adoption. Our results can be used to select and tailor strategies that may improve SSI prevention.
Despite awareness of evidence supporting the effectiveness of best practices, many academic surgeons and trainees fail to implement them, especially with regards to no hair removal before surgery, omission of mechanical bowel preparation and perioperative hyperoxia. When focusing specifically on antibiotic prophylaxis, it appears that whereas most surgeons are aware that antibiotic prophylaxis is important in preventing SSIs, they are less clear about its role in preventing other adverse sequelae, including deep and organ space SSI, prolonged length of stay in hospital, readmissions and death.
The knowledge translation literature has shown that uptake and compliance with passively disseminated guidelines is poor.18 In contrast, our survey respondents believed that it is important to consult practice guidelines when making decisions regarding antibiotic prophylaxis. Although guidelines exist in areas such as antibiotic prophylaxis, surgeons may not be aware of their existence. Fewer surgeons indicated that computerized decision aids or standard pharmacy sets were important in their decision-making. This may, however, be a reflection of the resources available to surgeons in our setting. For example, only 2 of 7 participating hospitals have computerized order entry and support. Therefore, it is not surprising that many respondents did not believe that this is an important resource as they have not had an opportunity to experience the potential benefits.19
Furthermore, the results of our study demonstrated that barriers to appropriate timely administration of antibiotic prophylaxis are multifactorial. About 50% of respondents believe that the competing priorities in the operating room, lack of communication and lack of responsibility are all important barriers for appropriately administered antibiotic prophylaxis. These factors can all be classified as barriers at the hospital or system level. Therefore, proposed implementation strategies will require tremendous institutional commitment for coordinated quality improvement. We used a workshop to unite stakeholders from various specialties, such as anesthesiology, nursing, pharmacy, surgery and infectious disease, at each hospital. They reviewed our study data, and discussed the merits and challenges associated with various knowledge translation strategies. Subsequently these health professionals have focused on specific implementation strategies that may be most beneficial at their hospital. These include the use of operative checklists, standardized written orders and departmental protocols, increased resources toward surveillance and audit and feedback programs to monitor SSI rates.
Limitations
This study has several limitations. First, our response rate was only 60%. It is likely that respondents differed from nonrespondents in their knowledge and understanding of SSI prevention strategies. Thus, if anything, our results overestimate knowledge. Second, the responses were self-reported and might not be consistent with practice. Self-reporting has been shown to overestimate performance considerably, suggesting that compliance with guidelines is poorer than reported. The disparity is potentially significant. Adams and colleagues20 conducted a review of the literature to determine the utility of self-reports as a measure of guideline adherence and identify the effect of response bias on the validity of self-reports. In 87% of 37 comparisons, self-reported compliance measures consistently exceeded objective measures, with a median difference of 27%. As an example, an audit of more than 700 patients at the University of Toronto during this same time period revealed that only 80% of patients undergoing elective colorectal surgery received preoperative antibiotics in a timely fashion. Furthermore, this audit demonstrated that up to 50% of these same patients were leaving the operating room with core temperatures less than 36ºC (D.S.F., unpublished data, 2008). These results are in contrast to our survey responses, which indicate that 99% and 96% of surgeons use antibiotic prophylaxis and perioperative normothermia, respectively. Despite this discordance, our survey results provide important insights into knowledge and beliefs, which might guide better implementation strategies. Finally, the generalizabilty of our results may be limited, as they represent findings from institutions associated with only 1 academic centre. However, there is strong evidence from other studies illustrating a lag in adoption of evidence into practice.4
Conclusion
Taken together, our data suggest that gaps in the translation of evidence into practice are pervasive, even within academic environments. To demonstrate change, implementation strategies must focus not only on the care providers, but also on the environments in which they practise. Finally, our study emphasizes the value of a structured knowledge translation framework before attempting changes in practice.
Footnotes
Presented at the Surgical Infection Society Annual Meeting, May 8, 2008, Hilton Head, South Carolina
Competing interests: S. Forbes declares having received speaker fees from Merck on the topic of the surgical management of intra-abdominal sepsis. None declared for the other authors.
Contributors: C. Eskicioglu, A. Gagliardi, D. Fenech, S. Forbes, R. McLeod and A. Nathans designed the study. C. Eskicioglu, M. McKenzie and R. McLeod acquired the data, which C. Eskicioglu, A. Gagliardi and A. Nathans analyzed. C. Eskicioglu wrote the article, which all authors reviewed and approved for publication.
- Accepted December 5, 2011.