Abstract
Background: Liver hydatidosis may lead to serious morbidity due to biliary complications, the management for which endoscopic sphincterotomy (ES) and biliary drainage are very efficient. We evaluated the effectiveness of endoscopic treatment for complications of hepatic hydatid disease.
Methods: We retrospectively reviewed endoscopic retrograde cholangiopancreatography (ERCP) procedures performed between January 2000 and December 2009 and compared laboratory findings, localization of the lesions and ERCP procedures applied between patients with and without jaundice.
Results: In all, 70 ERCP procedures were performed in 54 patients (24 men, 30 women). Of the 70 procedures, 24 were performed to treat jaundice. All patients with biliary fistulas and jaundice were managed with endoscopic procedures. The 70 ERCP procedures included sphincterotomy only (n = 40); sphincterotomy and stent placement (n = 7); stent placement only (n = 4); sphincterotomy and membrane extraction (n = 9); sphincterotomy, membrane extraction and pus drainage (n = 5); and sphincterotomy and pus drainage (n = 5). Laboratory results improved in 3–7 days, and bile leakage ceased in 2–21 days.
Conclusion: Endoscopic retrograde cholangiopancreatography is a safe and effective way to manage biliary complications of hepatic echinococcal disease. In most patients, ES is the most efficient treatment of postoperative external biliary fistulas, jaundice and accompanying cholangitis, as it enables clearing the bile ducts of hydatid remnants; ES should be performed since it accelerates the healing process by decreasing pressure in the choledochus.
Hydatid disease (HD) is a parasitic infection most commonly caused by the larva of Echinococcus granulosus and is a considerable health problem.1 The liver is the most frequently involved organ (75%), followed by the lungs (15%); the remainder of the body is affected 10% of the time.1–5
The disease is endemic in some cattle- and sheep-farming areas of the world and is prevalent in Mediterranean countries, such as Turkey. The main symptoms are related to compression owing to the growing mass. In some endemic regions, patients with hydatid disease may present with hydatid pancreatitis as their sole symptom. Intrabiliary rupture of the cyst can result in subsequent fistula formation in 5%–25% of patients. As a result, complications, such as obstructive jaundice and acute cholangitis caused by hydatid remnants in the biliary tree, can be seen during the pre- and postoperative periods.6–9 If biliary communication persists after the initial surgery, bile collections or fistulas may develop, and persistent postoperative biliary fistula is a serious complication that often necessitates another surgery.
Surgery is indicated for patients with symptoms and complications of hydatid disease, and the principal aim is total excision of the lesion.1,2 The specific operative approach depends on the number and location of the cycts and associated complications. Endoscopic methods are reported to be effective alternatives to surgery for the treatment of such complications owing to lower morbidity and shorter hospital stays. We report our experience with the endoscopic management of biliary complications of hepatic hydatid disease.
Methods
We retrospectively reviewed endoscopic retrograde cholangiopancreatography (ERCP) procedures used to manage the pre- and postoperative complications and outcomes of patients with liver hydatidosis between January 2000 and December 2009. Endoscopic sphincterotomy (ES) was planned for the patients with progressive cholangitis attacks or postoperative external bile leaks to quicken treatment and the healing process. Acute hydatid pancreatitis was also an indication for ES in endemic areas, such as Turkey. Endoscopic sphincterotomy was not performed in patients with transient jaundice and rapidly decreasing postoperative external bile fistulas. We considered patients to have jaundice if their total serum bilirubin was 34.21 μmol/L or greater.
We compared laboratory findings, localization of the lesions and ERCP procedures applied between patients with and without jaundice.
Antibiotics were administered intravenously as a prophylactic measure before the procedure. Patients were sedated by intravenous administration of midazolam and meperidine, and duodenal peristalsis was supressed with hyoscine N-butyl bromide. The ERCP procedure was performed with patients in a prone position with standard video duo-denoscopes (ED250XT-5, ED 200 XT Fujinon), and ES was performed in a standard manner using a variety of papillatomes. If stent insertion was required (e.g., in the case of severe cholangitis, insufficient expansion of the choledochus or unsatisfactory sphincterotomy), a Tannenbaum-type stent was used (10-F, Wilson-Cook, Inc.). A short sphincterotomy was almost always performed as a part of the stent insertion procedure. After ES, either a Dormia basket or an extraction balloon catheter was used to remove the daughter vesicles or infected bile from the biliary tract. Patients in whom remnants of the echinococcal material were removed from the bile duct were also treated with albendazole (10 mg/kg) to prevent the spread of disease. Provided that patients did not have allergic reactions and that there was no risk of scolices settling back in the tissues, remnants of all the material were left in the intestine. Stents were removed after the patients recovered from cholangitis or 6–8 weeks after the external biliary fistula healed. Follow-up consisted of clinical and biochemical monitoring and ultrasonography.
Statistical analysis
We performed χ2 tests and independent samples t tests for statistical analysis. We considered results to be significant at p < 0.05.
Results
During our study period, 70 ERCP procedures were performed in 54 patients (24 men, 30 women; mean age 48.5 [range 18–80] yr). All patients with biliary fistulas and jaundice were managed by endoscopic procedures. None of these patients were operated after ERCP. The 70 ERCP procedures consisted of sphincterotomy only (n = 40); sphincterotomy and stent placement (n = 7); stent placement only (n = 4); sphincterotomy and membrane extraction (n = 9); sphincterotomy, membrane extraction and pus drainage (n = 5); and sphincterotomy and pus drainage (n = 5; Table 1).
List of the procedures performed with endoscopic retrograde cholangiopancreatography
Of the 70 ERCP procedures, 24 were performed for jaundice due to biliary duct–associated hydatidosis: 9 were performed preoperatively in patients with liver hydatidosis and without any history of previous operations, and 15 were performed because of jaundice that occurred postoperatively. The 46 procedures that were not performed to treat jaundice involved ES for bile leakage and the treatment of postoperative external biliary fistulas.
Alanine aminotransferase, aspartate aminotransferase, alkaline phosphatase and γ-glutamyl transferase levels; white blood cell count; and choledochus diameter were significantly higher in patients with elevated total serum bilirubin than patients with normal total serum bilirubin. Age and amilase and lactate dehydrogenase levels did not differ significantly between these 2 groups (Table 2). Patients who met objective clinical criteria for functional biliary obstruction (i.e., dilated bile duct, abnormal liver tests) in particular experienced an improvement in their conditions following ERCP.
Laboratory findings of the patients with normal and high total bilirubin levels
In patients with jaundice cysts were significantly more common in the right than in the left hepatic lobe (χ2 test, p = 0.027; Table 3). Four patients presented with acute hydatid pancreatitis. Bile fistulas healed in 2–21 days after the ERCP procedure, and total serum bilirubin improved in 3–10 days. The drainage was successful with ERCP and stenting in 3 patients who were treated nonoperatively and in 8 patients postoperatively. The rate of ERCP-related complications was 2.8%. Mild pancreatitis (acute edematous pancreatitis) developed in 2 patients and resolved with conservative treatment. In 6 patients amilase levels increased more than 3-fold, but hyperamylasemia was transient. No patients had complications severe enough to necessitate surgical intervention.
Location of the hydatid cysts and correlation with total serum bilirubin
Discussion
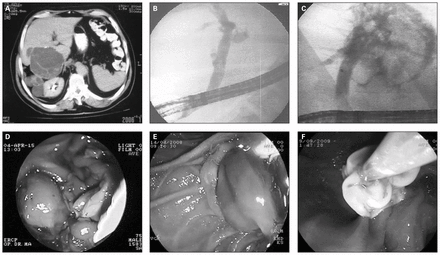
Endoscopic retrograde cholangiopancreatography is an effective and safe method for detecting and treating complications involving the biliary tree in patients who undergo surgery for liver hydatidosis. The most frequent category of complication and adverse effects of hydatid cysts is on the biliary tree (80%–90%). The presenting symptoms in these patients are external biliary fistula, jaundice, cholangitis or biliary colic. Ultrasonography, computed tomography, magnetic resonance imaging and magnetic resonance cholangiopancreatography — especially for cysts ruptured into the biliary tract — are the methods used as diagnostic tools. Although ERCP can be used as a diagnostic method, it is better to use it as a therapeutic method. The type of complications and their frequency vary, but the therapeutic approach is similar and mainly consists of ES and biliary drainage (Fig. 1).
(A) Appearance of hydatid disease of the liver on a computed tomography scan. Endoscopic retrograde cholangiopancreatography view of (B) the hydatid material in the common bile duct, (C) contrast extravasation from the intrahepatic bile ducts to the hydatid cyst cavity, (D) infected hydatid material drained after papillotomy, (E) balloon extraction of the hydatid material after papillotomy and (F) extraction of the germinative membrane from the choledochus.
Before the widespread use of ERCP, the treatment for hydatid disease with rupture into the biliary tract was surgery for exploration of the biliary tract with choledochotomy and placement of a T tube for the cyst remnants. In cases of papillary stenosis, additional manipulation in the form of sphincteroplasty or choledoduodenostomy was necessary.10 Currently, ERCP is the first choice of treatment. In terms of treatment for acute cholangitis caused by choledocholithiasis, ES is superior to emergency surgery.11 The same may be expected for cholangitis caused by hydatid disease. However, to our knowledge, there are no published data to support the routine use of ERCP in the preoperative assessment of patients with hydatid disease without biliary complications; it has been suggested that prior ES minimizes the frequency of fistula formation after surgery.12,13
The most common postoperative complication of surgery for hydatid cysts is persistent external drainage in which there is communication between the residual cyst and biliary tree.14 Surgery has been the traditional treatment for biliary fistulas because of the hydatid cysts that fail to close spontaneously. However, because of the presence of adhesions and inflammation, surgery may be difficult and hazardous.15,16 Endoscopic techniques have been developed to decrease the pressure in the biliary tract and reduce the time for closure of the fistula; the use of biliary ES, nasobiliary drainage and endoprosthesis insertion has been reported.12,13,17,18 In hydatidosis, ES is preferable because of the frequent occurrence of papillary stenosis or associated difficulties with drainage of bile; it is also better tolerated by patients.19 Data from several series indicate that the time frame for closure of external fistulas ranges from 3 to 43 days after ES.20,21 In the present series, all patients with persistent external drainage were treated successfully with ES, and the fistulas closed within 10–20 days.
Biliary stent insertion is known to be highly effective in the treatment of postcholecystectomy biliary fistula, especially in patients with a narrow choledochus and high fistula output. In contrast to postcholecystectomy fistula, which cease rapidly after ES and occasionally even close spontaneously without decompression of the biliary tract, ES is preferable in patients with hydatidosis because of the frequent occurrence of papillary stenosis or associated difficulties with bile drainage. However, stent insertion is expensive and requires further ERCP procedures for exchange and ultimate removal. In most patients, ES is sufficient for the treatment of biliary fistula.
The etiology of postoperative external biliary fistulas may be extremely peculiar. Although uncommon in such patients, echinococcal material or even stones may be present in the bile duct. As suggested by al Karawi and colleagues,22 ERCP enables clearance of such debris from the ducts by using a balloon catheter, Dormia basket or irrigation with hypertonic saline solution by means of a nasobiliary drain. However, because of the risk of sclerosing cholangitis, lavage is not performed with any scolicidal agents. Rather, in these patients, treatment with albendazole (10 mg/kg/d) for 3 months is preferred.
Other common complications associated with hydatid cysts are jaundice and cholangitis caused by obstruction of the bile duct by hydatid remmants. These remnants can also cause acute hydatid pancreatitis.23,24 Endoscopic sphincterotomy, clearance of the biliary tract and stent placement is the treatment of choice in patients with severe cholangitis.22 In the present series, all 7 patients with postoperative obstructive jaundice or cholangitis had cyst remnants in the bile duct. With ES and clearence of the tract, symptoms resolved within 36 hours, and all patients remained asymptomatic during extended follow-up.
An infrequent postoperative complication associated with the treatment of hydatid cysts is secondary sclerosing cholangitis caused by injection of a scolicidal agent into the cyst during surgery.25 Therapy for patients who experience this complication is extremely difficult, and ES often fails to relieve the symptoms; this was the case for 1 patient in the present series.
Conclusion
Endoscopic retrograde cholangeopancreatography is a safe and effective method for the management of the biliary complications associated with hepatic hydatid cysts, either before or after surgery. It should be considered as the treatment of choice for biliary fistulas and hydatid cholangitis both in the preoperative and postoperative periods.
Footnotes
Presented in video form at the 18th World Congress of the International Association of Surgeons, Gastro-enterologists and Oncologists, Oct. 8–11, 2008, Istanbul, Turkey, and at the 8th National Endoscopic–Laparoscopic Surgery Congress, July 1–4, 2007, Turkey
Competing interests: None declared.
Contributors: M. Akaydin, F. Erozgen and Y.E. Ersoy designed the study. M. Akaydin and S. Birol acquired the data, which M. Akaydin, F. Erozgen, Y.E. Ersoy and R. Kaplan analyzed. M. Akaydin, F. Erozgen, Y.E. Ersoy and S. Birol wrote the article. M. Akaydin, F. Erozgen, Y.E. Ersoy and R. Kaplan reviewed the article. All authors approved its publication.
- Accepted January 10, 2011.