Abstract
Background: Nondisplaced or minimally displaced clavicle fractures are often considered to be benign injuries. These fractures in the trauma patient population, however, may deserve closer follow-up than their low-energy counterparts. We sought to determine the initial assessment performed on these patients and the rate of subsequent fracture displacement in patients sustaining high-energy trauma when a supine chest radiograph on initial trauma survey revealed a well-aligned clavicle fracture.
Methods: We retrospectively reviewed the cases of trauma alert patients who sustained a midshaft clavicle fracture (AO/OTA type 15-B) with less than 100% displacement treated at a single level 1 trauma centre between 2005 and 2010. We compared fracture displacement on initial supine chest radiographs and follow-up radiographs. Orthopedic consultation and the type of imaging studies obtained were also recorded.
Results: Ninety-five patients with clavicle fractures met the inclusion criteria. On follow-up, 57 (60.0%) had displacement of 100% or more of the shaft width. Most patients (63.2%) in our study had an orthopedic consultation during their hospital admission, and 27.4% had clavicle radiographs taken on the day of admission.
Conclusion: Clavicle fractures in patients with a high-energy mechanism of injury are prone to fracture displacement, even when initial supine chest radiographs show nondisplacement. We recommend clavicle films as part of the initial evaluation for all patients with clavicle fractures and early follow-up within the first 2 weeks of injury.
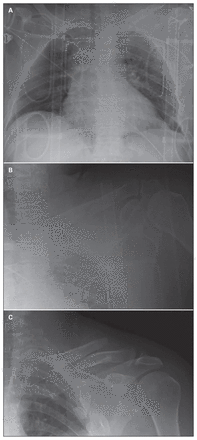
Minimally displaced clavicle fractures are considered to be benign injuries that usually do well with nonoperative treatment.1 In contrast, prospective studies have shown the benefits of open reduction and internal fixation of midshaft clavicle fractures with 100% or greater displacement.2,3 Most studies on clavicle fractures have involved patient populations who have sustained a low-energy fall or sporting accident.1–4 It has been our experience that minimally displaced clavicle fractures on initial supine chest radiographs in patients sustaining high-energy trauma are often not worked up appropriately with dedicated clavicle films as part of the initial evaluation and frequently present with 100% fracture displacement to our orthopedic clinic for follow-up (Fig. 1). This study was performed to determine the percentage of patients who received orthopedic evaluation and dedicated clavicle films as part of the initial assessment after sustaining high-energy trauma when a supine chest radiograph revealed a well-aligned clavicle fracture and to determine whether there was subsequent fracture displacement over time.
(A) Initial presenting chest radiograph, (B) clavicle radiograph on date of injury and (C) follow-up radiograph at 3 weeks after left clavicle fracture.
Methods:
We performed a retrospective review of trauma alert patients who sustained a midshaft clavicle fracture (AO/OTA type 15-B) and were treated at a single level 1 trauma centre between 2005 and 2010 to compare fracture displacement on initial supine chest radiographs to follow-up radiographs. In addition, we reviewed the rate of orthopedic consultation and the type of imaging studies obtained. To be included in our study, patients had to be 18 years or older, have a midshaft clavicle fracture (AO/OTA type 15-B) present on the initial supine chest radiograph, have initial fracture displacement of less than 100% of the clavicle shaft width, and have follow-up radiographs clearly showing the clavicle taken 2 or more days postinjury. Our Institutional Review Board approved this study.
The initial supine chest radiograph taken in the trauma bay was used as the index radiograph. The date and type of radiograph (chest radiograph or dedicated clavicle series) were noted for subsequent radiographs. For the purposes of this study, fractures were categorized on follow-up films as either displaced or nondisplaced. We considered fractures with less than 100% translation to be nondisplaced, and we considered those with 100% or more translation (including fractures with overlap) to be displaced. This definition was based on prior studies showing displacement of 100% in clavicle fractures to be predictive of nonunion.2,3 In addition, fracture displacement was measured quantitatively as the distance (in millimetres) between adjacent cortices at the fracture site on the radiograph showing the greatest fracture displacement.
We performed initial analyses to determine the rate of 100% fracture displacement on follow-up radiographs and the rate of orthopedic consultation and procurement of dedicated clavicle films both initially and during follow-up. We performed subgroup analyses to evaluate the rates of 100% fracture displacement for fractures among 2 arbitrarily determined groups: group A had initial displacement of 3 mm or less and group B had displacement greater than 3 mm but less than 100%.
Statistical analysis
We report descriptive statistics using mean or frequency as appropriate. We used the Fisher exact test to compare the percentage of patients who had a dedicated clavicle film taken on the day of admission and at any time during follow-up depending on whether or not they had an orthopedic consultation and the percentage of those who had fracture displacement of 100% or more of the shaft width on the follow-up radiograph depending on whether or not a dedicated clavicle film was taken. The α-level was set at 0.05 for statistical significance.
Results:
A total of 310 adult trauma alert patients sustained a clavicle fracture and were brought to our emergency department during the study period. Eleven patients (3.5%) were found to have fractures of the medial 1/5 (AO/OTA type 15-A) and 40 (13%) were found to have fractures of the lateral 1/5 (AO/OTA type 15-C) and were excluded from the study. Twenty-seven patients (9%) had midshaft clavicle fractures but had presenting chest radiographs that did not include the clavicle. Ninety-three patients (30%) did not have a follow-up radiograph 2 or more days after the initial film and were excluded. Finally, 44 (14%) patients had displacement with 100% or more translation at the fracture site on initial presentation and were excluded from this study.
The final study group consisted of 95 patients: 66 men and 29 women with an average age of 40 (range 19–89) years. The mechanism of injury was considered high-energy in all patients and involved motor vehicle collision in 41 (43.2%); motorcycle collision in 36 (37.9%); fall from a height in 8 (8.4%); pedestrian–automobile collision in 5 (5.3%); gunshot wound in 2 (2.1%); and all-terrain vehicle, boating and skateboarding accident in 1 (1.1%) patient each.
Initial clavicle displacement on the supine trauma bay chest radiograph averaged 5.8 (range 0–12.2) mm, with 31 of 95 fractures (32.6%) having 3 mm or less of displacement and the remaining 64 (67.4%) having more than 3 mm but less than 100% displacement. On the day of admission, 26 of 95 (27.4%) patients had dedicated clavicle films. Two of 26 (7.7%) showed 100% or more fracture displacement. Sixty (63.2%) patients had an orthopedic consultation on the day of admission, and they had a significantly higher rate of dedicated clavicle films taken on the day of admission than the remaining 35 patients who did not have orthopedic consultations (23 [38.3%] v. 3 [8.6%], p < 0.002).
All 95 patients had repeat radiographs taken 2 or more (range 2–33) days postinjury. Twenty-nine (30.5%) patients had a dedicated clavicle radiograph taken after the day of admission; the remainder had only serial chest radiographs. Receiving an orthopedic consultation at any point during hospital admission did not increase the likelihood of having dedicated clavicle films for follow-up (27 of 79 [34.1%] v. 2 of 16 [12.5%], p = 0.14).
Fifty-seven (60.0%) patients had 100% or more displacement of the shaft width on follow-up radiographs (Table 1). Forty-six (80.7%) of them had the displacement noted on films taken during their hospital admission, whereas the remaining 11 (19.3%) were taken during out-patient follow-up. The subsequent displacement from initial chest radiograph to follow-up radiograph averaged 7.6 (range 0–25) mm. Of these 57 patients with subsequent fracture displacement of 100% or more of the shaft width, 12 (21.1%) underwent surgical stabilization; they accounted for 12.6% of the entire cohort.
Frequency of clavicle displacement
We assessed subsequent fracture displacement between 2 subgroups of patients based on the initial displacement on admission supine chest radiographs. The percentage of patients with follow-up fracture displacement of 100% or more of the shaft width was significantly lower in patients with initial fracture displacement of 3 mm or less than in those with an initial displacement of more than 3 mm (10 of 31 [32.3%] v. 47 of 64 [73.4%], p < 0.001).
Discussion
We found a low incidence of dedicated clavicle films taken on the day of admission and during follow-up of patients with high-energy trauma, regardless of whether they received an orthopedic consultation. In addition, there was a high incidence (60.0%) of 100% fracture displacement on follow-up radiographs; most (80.7%) were noted on films taken during the hospital admission. We also found a lower (although still substantial) incidence of 100% fracture displacement in patients who had initial fracture displacement of 3 mm or less on supine chest radiographs than in those who had more than 3 mm of displacement (32.3% v. 73.4%).
Although it is accepted practice to obtain biplanar films on any fracture, we found that dedicated clavicle radiographs were obtained for only 27.4% of patients on the day of admission and for 30.5% of patients during follow-up. While orthopedic consultation did increase the likelihood of having biplanar radiographs of the clavicle taken on the day of admission, the frequency remained low (38.3%). When a clavicle fracture appears nondisplaced on the initial supine chest radiograph, it is not uncommon for further diagnostic imaging to be deemed unnecessary and for nonoperative treatment to be provided to the patient.5 We suspect that this situation is replicated at many hospitals. This may be in part because of a historical viewpoint that midshaft clavicle fractures are a benign entity that can almost always be treated nonoperatively with “good” results.1 The low rate of biplanar imaging and orthopedic consultation in combination with the high rate of delayed fracture displacement highlights the need for a more diligent approach toward the evaluation and treatment of midshaft clavicle fractures.
We found that 60.0% of midshaft clavicle fractures with less than 100% displacement on the initial supine chest radiograph in patients sustaining high-energy trauma had subsequent 100% fracture displacement, despite the fact that only 30.5% had a dedicated clavicle radiograph during follow-up. Furthermore, as many as one-third of fractures with initial displacement of 3 mm or less had 100% or more displacement on follow-up. This late displacement may indicate greater soft tissue stripping in patients who have sustained a high-energy injury compared with a low-energy fall. The subsequent displacement that occurred in our patient population changed fracture management from nonoperative to surgical in 21.0% of patients.
Much of the orthopedic literature over the past several years regarding midshaft clavicle fractures has attempted to identify which patients would benefit most from surgical intervention. In a retrospective study by Hill and colleagues,4 242 consecutive fractures of the middle third of the clavicle were treated nonoperatively. Initial shortening of the fracture site of 20 mm or more was found to be associated with nonunion; final shortening of 20 mm or more was associated with an unsatisfactory result.4 Robinson and colleagues2 reported the results of a prospective observational cohort study of 868 patients. They found a 4.5% rate of nonunion after midshaft clavicle fracture. Independent predictors of nonunion were advanced age, female sex, fracture displacement of 100% or more and the presence of comminution.2 This degree of displacement, therefore, provides an operative indication for midshaft clavicle fractures and changes fracture management when recognized. The Canadian Orthopaedic Trauma Society reported a multicentre, prospective randomized trial of 132 patients who sustained a displaced midshaft clavicle fracture.3 Patients were randomly assigned to plate fixation or to non-operative treatment with a sling. Because patient outcome scores, time to union and union rates were significantly improved in the operative fixation group when 100% fracture displacement was present, we used this displacement as our end point in the current study.
Limitations
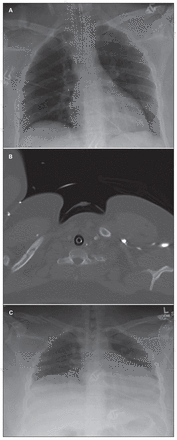
Limitations of the present study include the variation in the time interval between initial and follow-up radiographs. Owing to the retrospective nature of the study, radiographs were not taken at predetermined times. However, given our outcome measure, the time from injury to follow-up radiograph was not important as long as enough time was given to allow a fracture to displace if it was going to do so. Furthermore, the duration of follow-up for some patients in this study was as little as 2 days. Patients were included with this brief follow-up for 3 reasons. First, we observed before conducting this study that in many of our trauma patients who sustained a high-energy injury and had a minimally displaced clavicle fracture, complete displacement developed at the fracture site as little as 2 days after injury (Fig. 2). Second, given that our study cohort was composed of trauma alert patients with high-energy injuries, most patients were admitted to hospital for at least 2 days, during which time follow-up radiographs could have been taken. The minimum of 2 days of follow-up gave us the largest possible cohort while allowing reasonable time for the clavicle to displace. Third, with our primary outcome measure being the rate of displacement, we felt that even patients with relatively short follow-up should be included. Any fracture displacement in patients with a short follow-up that occurred during this short follow-up period would not have changed our outcome. However, in patients with short follow-up whose fractures did not show displacement at that time, the fractures may have gone on to displace before union. This would have led our overall rate of subsequent fracture displacement (60.0%) to be even higher.
(A) Initial chest radiograph and (B) computed tomography scan showing nondisplaced clavicle fracture. (C) Follow-up radiograph at 4 days showing displacement greater than 100%.
When a single view (supine chest radiograph) is the only view used for measurement of the initial displacement, the angle of the radiograph may underestimate the true degree of displacement. However, a chest radiograph was often the only image obtained to evaluate and follow the clavicle fracture in this series of patients until follow-up in the orthopedic clinic. We believe that it is not uncommon for the supine chest radiograph taken upon presentation in the trauma bay to be used to manage initial treatment until outpatient follow-up; our results highlight the importance of closer orthopedic follow-up in patients with high-energy clavicle fractures as well as the importance of obtaining and reviewing the appropriate images.
Finally, our study is limited in the number of patients lost to follow-up beyond the 2-day minimum. Unfortunately, poor follow-up among trauma patients as a whole is quite common. The patients lost to follow-up could have changed the results of this study if they had completed follow-up. We cannot be certain that these 2 cohorts would have had the same rate of fracture displacement, and fractures in the group lost to follow-up could have displaced at a lower or higher rate. However, we believe that the cohort lost to follow-up is similar to our final cohort. The 2 groups (those with follow-up and those without) were similar demographically, in initial displacement of the fracture and with respect to injury mechanism. In addition, many of the patients in our final cohort did not seek orthopedic follow-up for their clavicle fractures, much like our excluded patients. Many of our follow-up radiographs showing displacement came from chest radiographs obtained by the general trauma surgeon or primary care physician. The clavicle was not the reason for many of our follow-up radiographs, and yet still showed a high rate of displacement. Therefore, were it not for other reasons for obtaining radiographs, these patients would not have been included in the final cohort either.
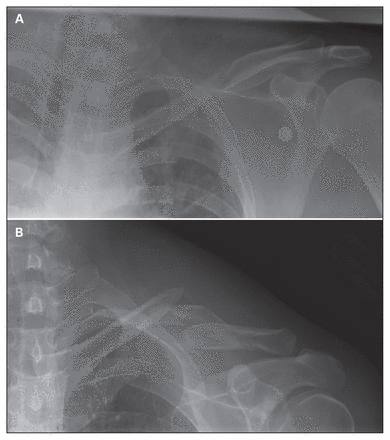
It is our experience that some patients who sustain a high-energy injury and have a well-aligned clavicle fracture on the initial supine radiograph will have marked fracture displacement on follow-up radiographs and, owing to this displacement, will benefit from surgical correction. When this early follow-up has not been completed, patients have returned to the orthopedic clinic weeks after their injuries with displacement or even malunion of fractures that had initially been diagnosed as nondisplaced (Fig. 3).
(A) Presenting clavicle radiograph and (B) follow-up radiograph at 2 days demonstrating displacement greater than 100%.
We have now changed orthopedic protocol at our institution. Trauma patients who have a clavicle fracture are evaluated with dedicated clavicle radiographs as part of their initial workup. We recommend obtaining dedicated clavicle films initially and follow-up clavicle films within 2 weeks for all patients with midshaft clavicle fractures. An additional follow-up radiograph is taken after 6 weeks in clinic. We obtain these images with the patients in the upright position when they are medically able.
Conclusion:
Clavicle fractures in patients who sustain high-energy injuries have a high propensity to displace on follow-up radiographs, even when they are minimally displaced initially. This displacement can go unnoticed when fracture evaluation has not occurred with dedicated clavicle views, orthopedic consultation and early follow-up. It is not uncommon for clavicle fractures to be treated without this protocol. We found that 60.0% of minimally displaced fractures on the initial supine chest radiograph had more than 100% displacement at early follow-up in this study. One-third of fractures with initial displacement of 3 mm or less had later displacement of more than 100%. This displacement may change subsequent fracture management in order to provide optimal patient outcomes. We recommend dedicated clavicle radiographs and close follow-up of all patients with clavicle fractures to assess for subsequent fracture displacement.
Footnotes
This work was performed at Orlando Regional Medical Center.
This study was presented at the 2012 OTA Annual Meeting, Minneapolis, MN, and at the 2013 AAOS Annual Meeting, Chicago, IL.
Competing interests: G. Haidukewych has received royalties and has consulted for Biomet, Depuy, Synthes, and Smith and Nephew, and owns stock in the Institute for Better Bone Health and Orthopediatrics. K. Koval has received royalties and has consulted for Biomet and Stryker. J. Langford has consulted for Stryker and owns stock in the Institute for Better Bone Health. M. Munro has consulted for Smith and Nephew. The Orlando Regional Medical Center has received funding for fellowship support from Synthes. No other competing interests declared.
Contributors: J.T. Riehl, M.W. Munro, J.R. Langford, G.J. Haidukewych and K.J. Koval designed the study. J.T. Riehl, B.J. Athans, M.W. Munro, S.J. Kupiszewski acquired and analyzed the data, which J.R. Langford, G.J. Haidukewych and K.J. Koval also analyzed., J.T. Riehl, B.J. Athans and K.J. Koval wrote the article, which all authors reviewed and approved for publication.
- Accepted June 5, 2013.