Abstract
Background: Parathyroid dysfunction leading to symptomatic hypocalcemia is not uncommon following a total or completion thyroidectomy and is often associated with significant patient morbidity and a prolonged hospital stay. A simple, reliable indicator to identify patients at risk would permit earlier pharmacologic prophylaxis to avoid these adverse outcomes. We examined the role of intact parathormone (PTH) levels 1 hour after surgery as a predictor of post-thyroidectomy hypocalcemia.
Methods: We prospectively reviewed the cases of consecutive patients undergoing total or completion thyroidectomy. Ionized calcium (Ca2+) and intact PTH levels were measured preoperatively and at 1-, 6- and 24-hour intervals postoperatively. The specificity, sensitivity, negative and positive predictive values of the 1-hour PTH serum levels (PTH-1) in predicting 24-hour post-thyroidectomy hypocalcemia and eucalcemia were determined.
Results: We reviewed the cases of 149 patients. Biochemical hypocalcaemia (Ca2+ < 1.1 mmol/L) developed in 38 of 149 (25.7%) patients 24 hours after thyroidectomy. The sensitivity, specificity, positive and negative predictive values of a low PTH-1 were 89%, 100%, 97% and 100%, respectively.
Conclusion: We found that PTH-1 levels were predictive of symptomatic hypocalcemia 24 hours after thyroidectomy. Routine use of this assay should be considered, as it could prompt the early administration of calcitriol in patients at risk of hypocalcemia and allow for the safe and timely discharge of patients expected to remain eucalcemic.
Parathyroid dysfunction leading to hypocalcemia is not uncommon after total or completion thyroidectomy and, if symptomatic, is often associated with significant patient morbidity and a prolonged hospital stay.1 Often, parathyroid tissue is deliberately or inadvertently resected with the surgical specimen. When recognized intraoperatively, normal, devitalized glands should be autotransplanted into the surrounding skeletal muscle. More often though, the observed fall in parathormone (PTH) levels is a result of traumatic injury to the parathyroids during thyroidectomy leading to either transient ischemia or even frank infarction of the glands. Thus, the hyposecretion of PTH may be relatively transient (1.6%–68%) or may be permanent (0.4%–33%).2,3
Intact PTH is secreted by the parathyroid glands in response to serum ionized calcium levels. Intact PTH in an 84-amino acid protein and control of its release is under direct feedback from extracellular calcium ions, as mediated through the cell surface calcium receptor of the parathyrocyte.4 The half-life of intact PTH is measured in minutes and can be reliably assayed.5,6 It is degraded into several smaller proteins with variable half-lives and biologic activity.6 The appearance of postoperative hypocalcemia may be delayed up to 48 hours depending on the levels of such biologically active peptides as well as the patient’s vitamin D and electrolyte status and the presence or absence of “hungry” bone, among other factors.4,5
Because of the lag between the hyposecretion of PTH and the development of symptomatic hypocalcemia, early pharmacologic support with calcium, magnesium and calcitriol can potentially keep high-risk patients eucalcemic and asymptomatic, thereby avoiding morbidity. Early prophylactic administration of calcitriol is important in maintaining eucalcemia in high-risk patients because, as a fat-soluble vitamin, its pharmacokinetics are such that an increase in serum calcium may take 24–48 hours. Thus, the early identification of post-thyroidectomy patients at risk of hypoparathyroidism and hypocalcemia would allow for the early introduction of calcitriol.7 Conversely, patients at low risk of post-thyroidectomy hypocalcemia can be spared the discomfort of excessive blood tests and can reliably be discharged without fear of symptomatic hypcocalcemia.
The present study correlates preoperative serum PTH and ionized calcium (Ca2+) levels with those obtained at 1, 6 and 24 hours after total thyroidectomy with an emphasis on the 1-hour PTH (PTH-1) and the subsequent development of hypocalcemia.
Methods
We retrospectively reviewed the cases of consecutive patients undergoing total or completion thyroidectomy at a single institution (Montreal General Hospital) between July 2009 and February 2011. No patients with coexisting parathyroid or renal pathology were included. The data were generated as part of our adopted thyroidectomy care pathway. We recorded the following information: age, sex, indication for surgery (benign v. malignant lesion) and type of surgery (completion v. total thyroidectomy). Preoperative serum ionized calcium (Ca2+) levels and preoperative PTH (PTH-P) levels were recorded; we also recorded PTH levels determined 1, 6 and 24 hours postoperatively (PTH-1, PTH-6 and PTH-24, respectively). Ionized calcium was measured on a blood gas machine, the ABL800 Flex (Radiometer). Normal Ca2+ ranged from 1.10–1.32 mmol/L. Serum intact PTH was measured using the Roche Elecsys 2010 System electrochemiluminescence immunoassay (Roche Diagnotics). The normal PTH level in our laboratory ranges from 1.5–6.9 pmol/L. Hypocalcaemia was defined as at least 1 ionized serum calcium measurement below 1.10 mmol/L (normal range: 1.1–1.32 mmol/L). Oral calcium supplementation with or without calcitriol was given to patients in whom symptomatic hypocalcemia developed or when the serum calcium level was less than 1.0 mmol/L. Patients with acral numbness, paresthesias, a positive Chvostek or Trousseau sign, cardiac arrhythmias or muscular spasms with or without stridor were considered symptomatic.5,6 Severe hypocalcemia was defined as Ca2+ of 0.9 mmol/L or less. An intravenous calcium gluconate (10%) infusion was reserved for patients with severe, symptomatic hypocalcaemia.
Statistical analysis
We calculated Pearson correlation coefficients. All statistical analyses were performed using Microsoft Excel 2011.
Results
We reviewed the cases of 149 patients (14 [9.4%] men and 135 [90.6%] women). The mean age of the entire cohort was 57.8 years and the median age was 58 years. Of the entire cohort, 136 (91.3%) patients underwent total thyroidectomy and 13 (8.7%) underwent completion thyroidectomy for malignancy. On final histologic review, 140 (94%) patients had diagnoses of primary thyroid cancer, whereas the 9 (6%) remaining patients had benign lesions.
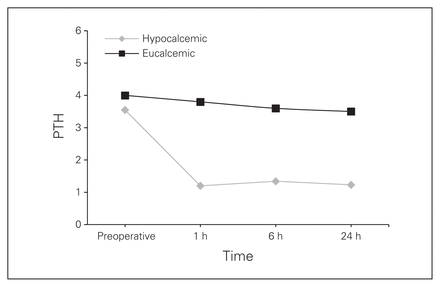
A significant number of patients had hypoparathormonemia (as defined by a PTH < 1.5 pmol/L (normal range: 1.5–6.9 pmol/L). The incidence at 1, 6 and 24 hours postoperative was 34 (22.8%), 36 (24.2%) and 38 (25.5%), respectively (Table 1). The incidence of hypoparathormonemia at 1, 6 and 24 hours postoperative seemed to plateau early and changed little. Furthermore, the mean PTH levels in hypocalcemic patients also attained an early plateau (Fig. 1). In eucalcemic patients at 24 hours postoperative, the mean PTH levels, although significantly higher, tended to decrease slightly by PTH-24 (Fig. 1). The Pearson r coefficients comparing PTH-1 and PTH-6 with PTH-24 were 0.80 and 0.95, respectively, thus reflecting the relative stability of PTH measurements within the first 24 hours postoperative.
Mean postoperative parathormone (PTH) in hypocalcemic and eucalcemic patients.
Incidence of hypoparathomonemia and hypocalcemia after total or completion thyroidectomy, n = 149
Hypocalcemia, as defined by Ca2+ less than 1.1 mmol/L (normal range: 1.1–1.32 mmol/L) at 1, 6 and 24 hours postoperative was documented in 3 (3.5%), 8 (5.4%) and 38 (25.5%) patients, respectively (Table 1). To assess the ability of Ca2+-1 measurements to predict hypocalcemia 24 hours postoperative, we performed sensitivity and specificity analyses. Of 149 patients, only 3 (3.5%) had low Ca2+-1; Ca2+-24 was low in 38 (25.5%) patients. Thus, the sensitivity of a low Ca2+-1 in predicting a low Ca2+-24 was only 11%. The specificity, however, was 100%. The negative (NPV) and positive predictive values (PPV) were 76% and 80%, respectively. Thus, Ca2+-1 is of limited use in predicting hypocalcemia 24 hours post-thyroidectomy. This is reflected in the Pearson r coefficients comparing Ca2+-1 and Ca2+-6 with Ca2+-24 of only 0.33 and 0.41, respectively. Unless they are low, Ca2+-1 levels are a poor predictor of hypocalcemia at 24 hours postoperative.
Of the 38 patients in whom hypocalcemia developed 24 hours post-thyroidectomy, PTH-1 levels less than 1.15 pmol/L (normal range: 1.5–6.9 pmol/L) in 34. Thus, the sensitivity of the PTH-1 in predicting the incidence of hypocalcemia at 24 hours postoperative is 89%. The specificity of PTH-1 less than 1.5 pmol/L in predicting hypocalcemia at 24 hours postoperative is 100%. The NPV and PPV were 97% and 100%, respectively (Table 2). Thus, PTH-1 is highly reliable in predicting which patients are at risk of hypocalcemia and which will remain eucalcemic the day after surgery.
Sensitivity and specificity analysis of PTH-1 measurement comparing Ca2+-24 and hypocalcemia
Of our entire cohort, 30 patients were discharged on oral medication consisting of combinations calcium, calcitriol and magnesium.
Discussion
Hypocalcemia post-thyroidectomy is the most common postoperative complication, with a reported incidence of 1%–50%.1,6 In the present study, the percentage of hypocalcemic patients reached 25.5% at 24 hours postoperative. Early identification of patients at risk of hypocalcemia would allow for prophylactic treatment, thus avoiding the development of symptomatic hypocalcemia.8 Conversely, patients who are not at risk can be spared repeated blood work and can safely be discharged without fear of returning with hypocalcemia.9
Early postoperative calcium monitoring, although important, is a poor predictor of subsequent symptomatic hypocalcemia. Despite the fact that the slope of postoperative serum calcium levels correlates with the development of symptomatic hypocalcemia, its utility is limited as the results are not available until 24–48 hours post-thyroidectomy.8,9 Combined with the lag between oral calcitriol and its onset of action, the delays in achieving calcium homeostasis become excessive. The routine administration of calcitriol and/or calcium to all patients either pre- or postoperatively are strategies that have been advocated.10,11
Other approaches to monitor and predict postoperative parathyroid function and subsequent hypocalcemia have been described in the literature. These include PTH assayed either intraoperatively or in the early postoperative period.10–13 These approaches are based on the fact that intact PTH has a short half-life of 1–4 minutes,14,15 thus allowing detection of its fall early in the perioperative period. Early diagnosis of hypocalcemia and the relevance of PTH levels for enabling an earlier diagnosis after total thyroidectomy have been the subject of numerous studies and several authors.14–19 These studies vary widely in terms of trial type, methodology, measurement technique, timing of measurement, protocols and thresholds maintained.
Pattou and colleagues3 found that a postoperative PTH level of 12 pg/mL or less was a good predictor of hypocalcemia, but they did not state how long after surgery PTH values were obtained.15 Lombardi and colleagues15 found greater precision with measurements taken at 4 and 6 hours, with an overall accuracy of 98%. Lam and Kerr16 reported that all patients with a PTH level less than 8 pg/mL measured 1 hour after the surgery became hypocalcemic, and all patients with a PTH level greater than 9 pg/mL did not. Higgins and colleagues17 demonstrated that 64% of those patients who subsequently required calcium supplementation had a decrease in PTH levels greater than 75% from baseline 20 minutes after surgery, and 74% of those who did not need calcium supplementation demonstrated a decrease of less than 75% from baseline. The Australian Endocrine Guidelines,18 published in 2007, adopted the recommendations of Lombardi and colleagues15 to standardize obtaining a PTH level 4 hours after a thyroidectomy. The wide variability of the predictors for the development of hypocalcemia across centres suggests that the measurement of PTH at any time in the postoperative period may be a reliable predictor of hypocalcemia.19 We believe that obtaining a PTH level 1 hour after an operation is the optimal time to predict the need for calcium and/or calcitriol supplementation after discharge from the hospital.
The present study demonstrates that PTH-1, PTH-6, and PTH-24 assays are good predictors of hypocalcemia 24 hours post-thyroidectomy. A PTH-1 assay alone is predictive of the development of postoperative hypocalcemia at 24 hours, with a sensitivity of 89% and an NPV of 97%. Practically, we found no significant advantage in determining PTH-6 and PTH-24 in asymptomatic patients with a PTH-1 greater than 1.5 pmol/L.
Should PTH-1 be greater than 1.5 pmol/L, asymptomatic patients can be discharged without the need for further routine calcium monitoring. Should PTH-1 be less than 1.5 pmol/L, patients can be administered a “loading dose” of calcitriol early in the recovery room. This is of practical importance given a lag of 24–48 hours before calcitriol exhibits its clinical effects.
The purpose of the present study was to identify a simple predictor of early postoperative hypocalcemia, which may either be transient (lasting weeks–months) or may persist. Factors other than PTH-1, such as extent of dissection, number of parathyroids visualized intraoperatively, number of parathyroids identified in the pathologic specimen, and vitamin D levels, should be taken into account to predict chronic hypoparathyroidism and the need for calcitriol and calcium for longer than 6 months after surgery.
Conclusion
Our results suggest that PTH-1 is an excellent predictor of patients who are at risk for hypocalcemia 24 hours postoperatively. Should PTH-1 be less than 1.5 pmol/L, prophylactic pharmacotherapy with calcitriol should be started to avoid the development of symptomatic hypocalcemia.
Footnotes
Competing interests: None declared.
Contributors: A. Alqahtani and R.J. Tabah participated in all manuscript preparation activities. A. Parsyan and R. Payne designed the study and reviewed and approved the final version for publication.
- Accepted November 11, 2013.