Abstract
Background: Olecranon fractures represent 10% of upper extremity fractures. There is a growing body of literature to support the use of plate fixation for displaced olecranon fractures. The purpose of this survey was to gauge Canadian surgeons’ practices and preferences for internal fixation methods for displaced olecranon fractures.
Methods: Using an online survey tool, we administered a cross-sectional survey to examine current practice for fixation of displaced olecranon fractures.
Results: We received 256 completed surveys for a response rate of 31% (95% confidence interval [CI] 30.5–37.5%). The preferred treatment was tension band wiring (78.5%, 95% CI 73–83%) for simple displaced olecranon fractures (Mayo IIA) and plating (81%, 95% CI 75.5–85%) for displaced comminuted olecranon fractures (Mayo IIB). Fracture morphology with a mean impact of 3.31 (95% CI 3.17–3.45) and comminution with a mean impact of 3.34 (95% CI 3.21–3.46) were the 2 factors influencing surgeons’ choice of fixation method the most. The major deterrent to using tension band wiring for displaced comminuted fractures (Mayo IIB) was increased stability obtained with other methods described by 75% (95% CI 69–80%) of respondents. The major deterrent for using plating constructs for simple displaced fractures (Mayo IIA) was better outcomes with other methods. Hardware prominence was the most commonly perceived complication using either method of fixation: 77% (95% CI 71.4–81.7%) and 76.2% (95% CI 70.6–81.0%) for tension band wiring and plating, respectively.
Conclusion: Divergence exists with current literature and surgeon preference for fixation of displaced olecranon fractures.
Olecranon fractures are a common injury representing 10% of upper extremity fractures.1 The standard treatment for displaced olecranon fractures is open reduction and internal fixation (ORIF), with typical methods including tension band wiring or plating.1–4 The chosen method of surgical intervention depends on many factors, including the amount of bone loss, the amount of comminution, the stability of the joint and the ability to reduce the articular surface.3
Displaced noncomminuted olecranon fractures were traditionally treated using tension band wiring, which was first described by Weber and Vasey.5 This method was designed with the theory that early mobilization would create tensile forces across the fracture that would be converted to compression forces and prevent nonunion, while minimizing the loss of range of motion.6 It has recently been shown that this principle is applicable only during active extension through a range of 30–120° of elbow flexion.7 However, tension band wiring remains a popular method of internal fixation of olecranon fractures.6 The advantages of tension band wiring compared with plate fixation include shorter surgery4 and lower cost.8 Surgeons who use this technique have shown good fracture healing and acceptable range of motion.4,9–12 However, the rates of hardware removal following tension band wiring are significant and reported to be as high as 80%.13–16
Plating techniques have been used for both comminuted1,17 and noncomminuted fractures of the olecranon.4 Plating offers the advantage of increased stability4,18 and may be associated with lower rates of hardware prominence.1,4,6,17,19 However, such a construct may be considered too bulky for simpler noncomminuted fractures, be associated with longer surgery and be more costly.15
There is controversy about which internal fixation method for displaced olecranon fractures provides optimal stability, range of motion and lack of complications (e.g., hardware prominence). There are clear advantages and disadvantages to each method, but owing to variability in patient population and injury pattern (simple v. comminuted), determining the best method presents a challenge. We administered a survey to gauge Canadian surgeons’ practices and preferences for internal fixation methods for displaced olecranon fractures. The survey results will help elucidate how surgeons are making treatment decisions and what factors are perceived to be important in choosing an appropriate fixation construct and the complications they experience with them.
Methods
Survey design
We created a 10-item survey to assess the preferences and practices of Canadian orthopedic surgeons for the internal fixation of displaced olecranon fractures in adults. The questionnaire addressed surgeons’ preference of methods for internal fixation of displaced noncomminuted versus displaced comminuted fractures as well as the factors dictating their choice of method using a scale from 0 (no impact) to 4 (most impact). The survey differentiated fracture type using the Mayo classification of olecranon fractures,20 with type IIA described as simple displaced and IIB as comminuted displaced fractures. Notably, type IIA includes both simple transverse and simple oblique fractures, which may be managed differently. Question 5 of the survey asked surgeons to comment on the impact of fracture morphology on treatment decisions in order to account for the broad classification system. Respondents were also surveyed on the factors that deterred them from using a given fixation method for a specific fracture type as well as the most frequently encountered complication with such methods. The questions were closed-ended with multiple-choice options or Likert scales.21 An “other” option was included when applicable to allow respondents to specify the answer most appropriate for them. The demographic information that we collected included practice setting (academic v. community) and the number of olecranon fractures treated in 1 year. All response data were collected anonymously, with no monetary incentives or prenotification telephone calls. The Ethics Review Board in association with Hamilton Health Sciences approved this study. Responses were required for all questions; however, participants were able to opt out of completing the survey at any point. We used SurveyMonkey to create the survey. The full questionnaire is provided in Appendix 1, available at canjsurg.ca.
All questions were vetted by experts in the field (B.R, B.P) for clarity and comprehensiveness. In addition, 3 surgeons piloted the survey (face validity), and revisions were made according to their feedback on fixation methods, complications and classification (content validity).
Survey distribution
The survey was distributed to orthopedic surgeons belonging to the Canadian Orthopaedic Trauma Society (COTS) and Canadian Orthopaedic Association (COA). An email was sent to all members of COTS and COA (833 in total) with a cover letter describing the objectives of the study and providing a link to the survey. We sent 2 follow-up emails, approximately 5 weeks apart, to all nonresponders to remind them to complete the survey.
Sample size calculation
To sufficiently power our analysis, we assumed that approximately 75% of surgeons surveyed used tension band wiring or plating for fixation of displaced olecranon fractures. It was calculated that 125 completed questionnaires would be required to produce a 95% confidence interval (CI) of ± 7% for the use of tension band wiring or plating, with an α level of 0.05.
Statistical analysis
We calculated relative frequencies of the survey questions with their corresponding CIs. We used the Wilson method to calculate CIs for the proportions. We calculated the means and the CIs for the questions that participants were asked to rank on a scale of 0 to 4. We reported percentages and means with their corresponding CIs for survey questions. We used SPSS and Confidence Intervals Analysis software (www.som.soton.ac.uk/research/sites/cia/) for data analysis.
Results
Respondents
There were 833 registered members of the COA and the COTS eligible to participate in this survey. Overall, 256 members responded to our email invitation to complete our survey yielding a response rate of 31% (95% CI 30.5–37.5%). The sample size of 256 completed surveys allowed a 95% CI of ± 4.4%. Of those who completed the survey 55.5% had an academic practice and 46.5% had a community practice. Of the surgeons surveyed, 94.9% performed 0–20 olecranon surgeries a year (65.6% performed 0–10, and 29.3% performed 10–20).
Management preferences and factors influencing choice
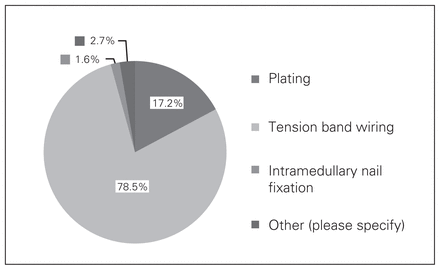
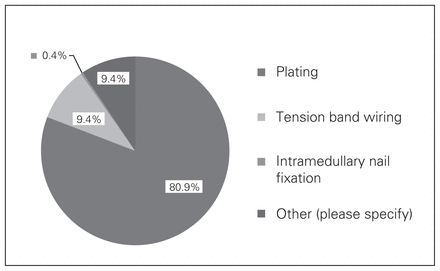
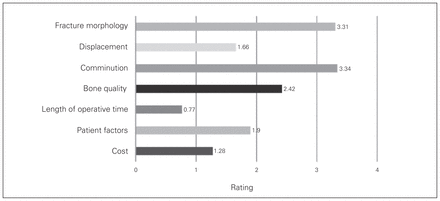
The preferred treatment for simple displaced olecranon fractures (Mayo IIA) according to the surgeons surveyed was tension band wiring (frequency 78.5%, 95% CI 73–83%; Fig. 1). The preferred treatment for displaced comminuted olecranon fractures (Mayo IIB) was plating (frequency 81.0%, 95% CI 75.5–85%; Fig. 2). The 2 most important factors (on a scale of 0 to 4, where 0 indicates no impact and 4 indicates major impact on management) influencing the decision of which fixation method to use were fracture morphology (mean impact 3.31, 95% CI 3.17–3.45) and comminution (mean impact 3.34, 95% CI 3.21–3.46; Fig. 3).
Responses to the question, “What is your preferred method for the internal fixation of a displaced noncomminuted (Mayo Class IIA) olecranon fracture?”
Responses to the question, “What is your preferred method for the internal fixation of a displaced comminuted (Mayo Class IIB) olecranon fracture?”
Responses to the item, “Please rate the following factors according to their impact on your preferred management of olecranon fractures. Please specify how each factor impacts your management decisions.”
Deterrents to choosing fixation construct
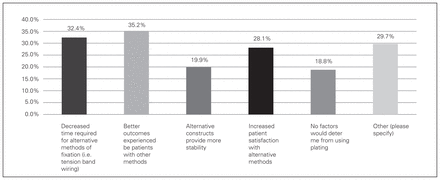
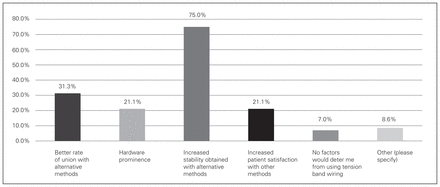
The major deterrents to using plating constructs for simple displaced fractures (Mayo IIA) were decreased time required for alternative methods, as reported by 32.4% (95% CI 27.0–38.4%) of respondents; 35.2% (95% CI 29.6–41.2%) of respondents felt that they had better outcomes with other methods (Fig. 4). “Other” was selected by 29.7% (95% CI 24.4–35.6%) of respondents, who listed cost (n = 43), hardware irritation (n = 20), simplicity/speed (n = 6) and no difference with tension band wiring (n = 7) as deterrents. The major deterrent to using tension band wiring for displaced comminuted fractures (Mayo IIB) was increased stability obtained with other methods of fixation, as described by 75% (95% CI 69–80%) of respondents (Fig. 5).
Responses to the question, “Which factors would deter you from using plating for displaced noncomminuted (Mayo Class IIA) olecranon fractures?”
Responses to the question, “Which factors would deter you from using tension band wiring for the fixation of displaced comminuted (Mayo Class IIB) olecranon fractures?”
Complications
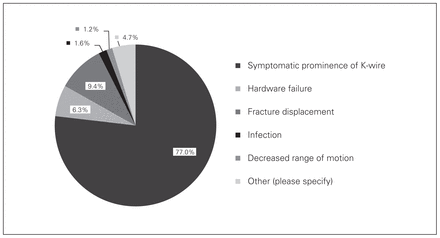
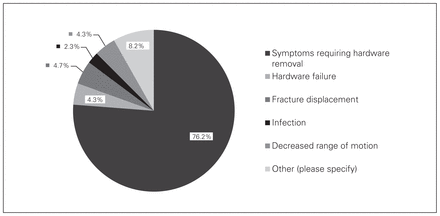
Out of all the surgeons surveyed, 77% (95% CI 71.4–81.7%) reported symptomatic hardware prominence as their patients’ major perceived complication with tension band wiring, followed by fracture displacement at 9.4% (95% CI 6.4–13.6%; Fig. 6). For plating, 76.2% (95% CI 70.6–81.0%) of surgeons surveyed stated that symptomatic hardware prominence was the most frequent patient-perceived complication (Fig. 7); approximately 8.2% (95% CI 5.4–12.2%) of surgeons stated “other” as being the most frequent. Specified complications were skin breakdown (n = 3) and longer duration of surgery (n = 3). Eight respondents stated there were no major perceived complications when using plating for displaced olecranon fractures.
Responses to the question, “What is the most frequently perceived complication you experience when using tension band wiring fixation?”
Responses to the question, “What is the most frequently perceived complication that you experience when using plating?”
Community versus academic setting
Surgeons in academic settings were more likely than those at community hospitals to use plating for noncomminuted (Mayo class IIA) olecranon fractures (22.5% v. 10.1%). For the treatment of comminuted fractures (Mayo class IIB), in the academic setting 83.1% chose plating and 7.8% chose tension band wiring versus 77.3% and 11.8%, respectively, in the community.
Discussion
There is controversy regarding which internal fixation method provides optimal stability, range of motion, cost and lack of complications, including hardware prominence, for displaced olecranon fractures. There are clear advantages and disadvantages to each method, but owing to variability in patient population (age, bone quality), relying on fracture pattern and surgeon preference to determine the best method of fixation presents a challenge. Our survey aimed to gauge surgeons’ practices and decision-making on internal fixation methods for displaced olecranon fractures and compare these practices to the current trends reported in the literature.
According to the literature, many surgeons believe tension band wiring may not be as easy as previously thought, given the high rate of loss of reduction and overall hardware prominence, which has been reported to be as high as 80%.4,14,15,22 This belief is also reflected by our survey results, which showed the 2 most commonly perceived complications were symptomatic hardware prominence and fracture displacement. Moreover, in our survey the majority of surgeons responded that the optimal fixation of simple displaced olecranon fractures is with an “easy” and “time efficient” construct: tension band wiring. Authors such as Mullett and colleagues,23 have emphasized that technical considerations (e.g., engaging the anterior cortex of the ulna using a transcortical approach) of tension band wiring compared with intramedullary wiring help to prevent pin migration and hardware prominence. Interestingly, the major deterrent for using tension band wiring for comminuted fractures was that other constructs, such as plating, were deemed more stable for those patterns.
Proponents of plating state that although it requires more time — it was shown in 1 study to be 25 minutes longer than tension band wiring — plating is generally better at achieving and maintaining anatomic reduction.3,4,17 In our survey, the majority of surgeons responded that the optimal fixation of displaced comminuted olecranon fractures is with plating. Although variability exists in the type of plate and technique used, overall patient satisfaction is high.1,4 Many surgeons feel plating is a good fixation method for olecranon fractures, yielding acceptable range of motion, minimal discomfort and good results when used for simple and comminuted olecranon fractures.1,3,17,19,24 According to our survey results, reluctance to use plating for simpler fractures was driven by cost, equivalent or better outcomes with other simpler constructs and longer duration of surgery (including more extensive dissections). In a randomized controlled trial comparing tension band wiring to plating, authors reported no difference in range of motion but significantly more hardware prominence in the tension band wiring group than the plating group (42% v. 5%).4 There was also measurable loss of reduction in the tension band wiring group compared with essentially none in the plating group.4 It was concluded that “settling” of the fracture reduction occurs in many cases with tension band wiring and that, overall, plating should be strongly encouraged when fixing displaced olecranon fractures.4 Close to 10% of surveyed surgeons stated that when fixing comminuted displaced olecranon fractures they preferred to use tension band wiring. As a principle, tension band wiring is relatively contraindicated when there is comminution of the articular surface.3,6 In these cases, a higher degree of stability is required to maintain integrity of the articular surface and in turn maximize functionality of the joint, suggesting the use of plate fixation.3 Therefore, this indicates a discrepancy between the literature and current practice.
Based on the current evidence, we believe that plating techniques should be used for both displaced noncomminuted and displaced comminuted fractures.1,3,4,15,17,19,24 However, based on our survey, 78.5% of surgeons use tension band wiring for simple displaced olecranon fractures and believe this technique is more stable (20%), produces better outcomes (35.2%) and requires less time to perform (35.2%). Thus, the beliefs and practices of the Canadian surgeons surveyed may not be completely supported by the existing evidence. In our survey 17% of surgeons felt plating was too expensive for use in simpler fractures. But according to the literature, rates of surgical removal for hardware prominence are significantly higher when using tension band wiring than when using plating,4 contributing to a higher overall cost. Interestingly, most surgeons (> 75%) felt that when using either construct, the complication most often experienced by patients was hardware prominence. As a result of the substantial rate of hardware prominence requiring surgical removal, as seen in our survey and in the literature, critical evaluation of all options for olecranon fixation is warranted.15 Only 4% of those surveyed used screw fixation or intramedullary fixation. An economic analysis evaluating cost differences between plating and tension band wiring taking into account additional surgeries should be undertaken, keeping in mind different institutional costs.
Limitations
A limitation of our study was the reliance on surgeons to recall the most frequently experienced complications, which may have led to bias.
Conclusion
Our survey shows that surgeons prefer to fix simple displaced olecranon fractures using tension band wiring and displaced comminuted fractures with plating. Furthermore, the percentage of surgeons preferring tension band wiring was higher in the community than in academic settings for both noncomminuted and comminuted fractures. Fracture morphology and comminution were most influential for guiding their treatment. The major deterrent to using plating for simple fractures was the perception of increased cost, longer duration of surgery and equivalent outcomes using other methods. Likewise, deterrents for using tension band wiring for displaced comminuted fractures were that other constructs available provided better stability. The most common perceived complication experienced using either method was hardware prominence. Our survey results demonstrate that surgical decision-making, in regards to fixation of displaced olecranon fractures, may not be supported by the literature and suggests a discrepancy between Canadian surgeons’ beliefs and practices and the current evidence.
Footnotes
Competing interests: None declared.
Contributors: T. Wood, K. Thomas and F. Farrokhyar designed the study. T. Wood and K. Thomas acquired the data, which all authors analyzed. T. Wood and K. Thomas wrote the article, which all authors reviewed and approved for publication.
- Accepted January 16, 2015.