Abstract
Background: The effect of hospital specialization on the risk of hernia recurrence after inguinal hernia repair is not well described.
Methods: We studied Ontario residents who had primary elective inguinal hernia repair at an Ontario hospital between 1993 and 2007 using population-based, administrative health data. We compared patients from a large hernia specialty hospital (Shouldice Hospital) with those from general hospitals to determine the risk of recurrence.
Results: We studied 235 192 patients, 27.7% of whom had surgery at Shouldice hospital. The age-standardized proportion of patients who had a recurrence ranged from 5.21% (95% confidence interval [CI] 4.94%–5.49%) among patients who had surgery at the lowest volume general hospitals to 4.79% (95% CI 4.54%–5.04%) who had surgery at the highest volume general hospitals. In contrast, patients who had surgery at the Shouldice Hospital had an age-standardized recurrence risk of 1.15% (95% CI 1.05%–1.25%). Compared with patients who had surgery at the lowest volume hospitals, hernia recurrence among those treated at the Shouldice Hospital was significantly lower after adjustment for the effects of age, sex, comorbidity and income level (adjusted hazard ratio 0.21, 95% CI 0.19–0.23, p < 0.001).
Conclusion: Inguinal hernia repair at Shouldice Hospital was associated with a significantly lower risk of subsequent surgery for recurrence than repair at a general hospital. While specialty hospitals may have better outcomes for treatment of common surgical conditions than general hospitals, these benefits must be weighed against potential negative impacts on clinical care and the financial sustainability of general hospitals.
Inguinal hernia is a common problem, affecting more than one-quarter of men during their lifetime. Surgical repair of inguinal hernia is one of the most frequent surgical procedures performed, with an estimated 800 000 hernia repairs performed in the United States each year.1 Since inguinal hernia repair is usually an ambulatory procedure and complications are uncommon, hernia recurrence is a key quality measure. Hernia recurrence risk can reach up to 15%, depending on a variety of factors, including surgeon expertise,2 and is commonly used as an outcome measure in evaluative studies of hernia repair.3
Ambulatory surgical centres and specialty hospitals provide care to patients with specific problems, such as elective cardiac or orthopedic conditions.4 Proponents of specialty hospitals advocate their potential benefits in terms of quality, efficiency and cost of care. The high volume of procedures performed at specialty hospitals may largely explain why the reported outcomes of care are frequently better than those at general hospitals.5 Critics of specialty hospitals point out their potential to “cream skim” profitable and low-risk episodes of care.4 The Shouldice Hospital in Toronto, Ont., is a surgical specialty hospital focused exclusively on the surgical treatment of abdominal wall hernias, performing thousands of hernia procedures each year and accounting for a large proportion of all such operations performed in Ontario. Surgeons at the Shouldice Hospital typically perform 20 times more hernia repairs than surgeons in general hospitals, making it an extreme outlier in procedure volume. The Shouldice Hospital has been prominently cited as a prototypical surgical specialty facility6 and as a business model for the type of “focused factory” that could translate the efficiencies seen in the manufacturing industry to health care. Although there are reports of low rates of hernia recurrence among patients who had surgery at the Shouldice Hospital, there are no published population-based studies.
The purpose of the present study was to compare hernia recurrence rates among patients having primary elective inguinal hernia repair at the Shouldice Hospital with those having surgery at general hospitals in Ontario. We sought to determine whether surgery at the Shouldice Hospital was associated with a lower risk of hernia recurrence and how the risk of recurrence was influenced by procedure volume among those treated at general hospitals.
Methods
Study overview
We conducted a retrospective cohort study using population-based administrative health data for the province of Ontario. All Ontario residents who underwent primary elective inguinal hernia repair in Ontario between Jan. 1, 1993, and Dec. 31, 2007, were followed until Mar. 31, 2010, to assess for hernia recurrence. We were interested in determining whether the Shouldice Hospital — a specialty hospital for hernia surgery — had a lower rate of inguinal hernia recurrence than general hospitals after accounting for surgical volume.
Data sources
We used encrypted, individual level administrative data from the Ontario Health Insurance Plan (OHIP) physician billing database, the Canadian Institute for Health Information Hospital Discharge Abstract Database (CIHI-DAD) and the Registered Persons Database (RPDB). These data sets were held securely in a linked, deidentified form and analyzed at the Institute for Clinical Evaluative Sciences. These databases are considered to be population-based and valid for the ascertainment of surgical procedures, including inguinal hernia repair.7,8 The research ethics board of Sunnybrook Health Sciences Centre approved our study protocol.
Study participants
We identified Ontario residents aged 18–90 years who underwent primary elective nonrecurrent inguinal hernia repair between Jan. 1, 1993, and Dec. 31, 2007. Inguinal hernia repairs were not eligible for inclusion in the study if they were coded as massive inguinal hernias or strangulated or incarcerated hernias. We included the first eligible inguinal hernia repair for patients who had more than 1 repair during the study period; the data sources did not distinguish whether a hernia repair was a right- or left-sided procedure.
Exposures
For each participant, we measured the volume of elective inguinal hernia surgeries performed at their hospital in the year before surgery and categorized them into 4 equal groups (quartiles). We also identified the hospital where the hernia surgery was done. While the number of hospitals varied during the study period owing to openings, closings and amalgamations, more than 100 general hospitals performed hernia surgery in each year of the study period. Because the volume of hernia repairs done at the Shouldice Hospital was substantially larger than all other hospitals, this hospital was categorized separately.
Several variables that might influence inguinal hernia recurrence were measured. These included age, sex, rurality, health region and median household income in the neighbourhood of residence. We assessed comorbidity using the Johns Hopkins Case-Mix Adjusted Clinical Groups (ADG) comorbidity score.9,10 Overall comorbidity was estimated by summing the presence of each of the 12 Collapsed ADG Clusters (CADG) and further stratified into low and high comorbidity levels, with a score of 7 or greater indicating high comorbidity.
Outcome
The primary outcome of interest was surgical repair of a recurrent inguinal hernia at any hospital in Ontario. We identified recurrence events using OHIP fee codes for recurrent hernia, regardless of whether the repair was uncomplicated or associated with an emergent presentation, such as strangulation. Hernia repair events occurring within 2 days of an earlier primary repair were not considered to indicate hernia recurrence, since bilateral repairs were often performed sequentially.
Statistical analyses
We estimated the rate of recurrent hernia repair per 1000 person-years of follow up as well as the overall crude and age-standardized proportion of participants who had a surgical recurrence. For each participant, we also calculated the time between the date of the initial surgery and the earliest occurrence of recurrent hernia surgery, death, loss of registration for health services, or study end date (Mar. 31, 2010). The time to hernia recurrence was plotted using Kaplan–Meier survival curves and compared between hospital categories using the log rank test. We used Cox proportional hazards models to estimate the effects of the various exposures, including patient and hospital characteristics, on the time to hernia recurrence11 using variance-corrected estimates to account for hospital-level clustering.12
We performed a number of stratified analyses to determine whether the Shouldice Hospital had substantially different outcomes than general hospitals for different subgroups. We used interaction terms to test whether hernia recurrence risk differed according to age, sex, time period of hernia repair (1993–2000 v. 2001–2007), income and comorbidity.
We performed multiple sensitivity analyses to test whether aspects of the study design influenced the study findings. First, we analyzed only the healthiest participants in the cohort according to the CADG score. Second, we performed separate analyses for the periods 1993–2000 and 2001–2007 to account for secular changes in inguinal hernia repair techniques, such as the use of surgical mesh and tension-free repair.13,14 Finally, we tested the extent to which selection of patients with favourable hernias (“cherry picking”) influenced the results of the Shouldice Hospital. We identified patients who had a consultation with a Shouldice Hospital surgeon between 2004 and 2006 to determine what proportion subsequently had surgery at the Shouldice Hospital or a different hospital as well as the rate of hernia recurrence in each group. All statistical analyses were done using SAS version 9.2 (SAS Institute Inc.). We considered results to be significant at p < 0.05.
Results
Participants
A total of 235 192 patients had an eligible inguinal hernia repair in Ontario between Jan. 1, 1993, and Dec. 31, 2007: 170 065 at general hospitals and 65 127 at the Shouldice Hospital. The Shouldice Hospital accounted for 27.7% of all hernia repairs in the study, with annual volumes that were at least 6-fold greater than the highest annual volume of a general hospital (Table 1). The median age of participants was 55 years, and 90% were men. Participant characteristics were similar across volume categories for general hospitals. In comparison, those having surgery at the Shouldice Hospital were more likely to reside in higher-income neighbourhoods and have a lower burden of comorbidity.
Characteristics of patients having primary inguinal hernia repair in Ontario, according to hospital volume and specialty status (Shouldice Hospital v. general hospitals)
Risk of hernia recurrence
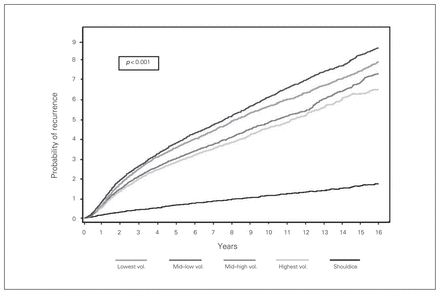
A total of 9020 patients had surgical repair of an inguinal hernia recurrence during the study period (Table 2). The age-standardized proportion of patients who had a recurrence ranged from 5.21% (95% confidence interval [CI] 4.94%–5.49%) among those who had surgery in the lowest volume general hospitals to 4.79% (95% CI 4.54%–5.04%) of those who had surgery at highest volume general hospitals. In contrast, those who had surgery at the Shouldice Hospital had an age-standardized recurrence risk of 1.15% (95% CI 1.05%–1.25%). The cumulative probability of recurrence was significantly lower (p < 0.001) among patients who had surgery at the Shouldice Hospital than at general hospitals, regardless of volume (Fig. 1).
Cumulative probability of repair of recurrent inguinal hernia, according to hospital volume and specialty status of initial hernia repair.
Risk of hernia recurrence according to hospital volume and specialty status (Shouldice Hospital v. general hospitals)
The reduction in recurrence risk observed at the Shouldice Hospital persisted after accounting for potentially confounding variables. Compared with patients who had surgery at the lowest volume hospitals, hernia recurrence among those treated at the Shouldice Hospital was significantly lower after adjustment for the effects of age, sex, CADG and income level (adjusted hazard ratio [HR] 0.21, 95% CI 0.19–0.23, p < 0.001; Table 3). Compared with patients having surgery at general hospitals in the lowest volume quartile, the adjusted relative risk of recurrence for those who had surgery at general hospitals in the highest volume quartile was 0.94 (95% CI 0.89–1.00, p = 0.06). Analyses limited to only patients with low burden of comorbidity showed similar results to the main analysis.
Adjusted risk* of hernia recurrence among persons having primary elective inguinal hernia repair in Ontario
Stratified analyses
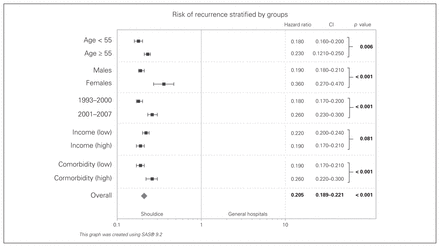
Compared with the risk of recurrence in patients who had surgery at general hospitals, the risk of recurrence was lower in those who had a hernia repair at the Shouldice Hospital for each subgroup examined (Fig. 2). However, the effect on reduction of hernia recurrence was larger among patients younger than 55 years, men and patients with fewer comorbidities. Patients who had surgery between 1993 and 2000 had a larger benefit than those who had surgery between 2001 and 2007 at the Shouldice Hospital.
Hazard ratios for repair of recurrent inguinal hernia, by age, sex, time period, income and comorbidity. CI = confidence interval.
A total of 6566 patients had a consultation with a surgeon at the Shouldice Hospital between 2004 and 2006 and subsequently had an inguinal hernia repair. Of these, 633 (9.6%) had their surgery at a general hospital instead of the Shouldice Hospital; a recurrence later developed in 20 of them (3.2%).
Discussion
In a population-based study of patients having primary elective repair of an inguinal hernia in Ontario, we found that those who had surgery at the Shouldice Hospital — a specialty hospital for hernia repair and an extreme high outlier for surgical procedure volume — had more than a 4-fold lower risk of recurrence requiring subsequent surgical repair than those whose initial surgery was done at a general hospital. This effect could not be explained by differences among patients who had surgery at different types of hospitals or by selection of patients at particularly low risk of hernia recurrence at the Shouldice Hospital. Our findings regarding hernia recurrence, the key outcome measure for hernia repair, suggest that increasing the number of people having inguinal hernia surgery at “focused factories” would result in improved surgical outcomes.
Results in relation to other studies
In randomized trials of hernia repair, the Shouldice technique of hernia repair was associated with fewer recurrences than tissue repairs, but there was no advantage over tension-free repairs using prosthetic mesh.15–24 The reasons why the Shouldice Hospital performed so much better in our study than in the clinical trials is not clear. In addition to performing a specific type of hernia repair in a very reproducible fashion at the Shouldice Hospital,25,26 a variety of processes of care are followed: patients are kept in hospital for several days after hernia repair, strict selection criteria are applied, and the surgeons perform extraordinarily large numbers of hernia surgeries. While we did not identify a statistically significant effect of hospital volume on recurrence among patients treated at general hospitals, our findings did suggest an underlying association, similar to other studies that demonstrated an influence of surgical volume on recurrence and other outcomes of inguinal hernia repair.27–29
Strengths and limitations
The strengths of our study include its large size and population-based sampling, the longitudinal assessment of surgical recurrence regardless of where it was repaired and our ability to identify patients who had surgery at the Shouldice Hospital.
Our study had several limitations. We lacked detailed clinical information on smoking; obesity; and hernia characteristics, such as size, all of which can influence recurrence risk. Although most of the hernia repairs among people who had surgery at the Shouldice Hospital were likely to be Shouldice repairs, we could not determine the specific surgical technique used in other hospitals, including whether repairs were open, laparoscopic, tension-free or “tissue” repairs. Because this study was limited to Ontario residents, we lacked information on procedures and outcome events for people from outside the province who had surgery in Ontario, many of whom would have had surgery at the Shouldice Hospital. We measured only hospital volume and not surgeon volume and therefore cannot exclude the effects of surgeon volume and expertise. Because recurrence was defined as surgical repair of a recurrent hernia, we could not detect subclinical recurrences, nor could we identify recurrences among patients who did not choose to have their recurrent hernia repaired.30 We were not able to measure differences in wound complications, which may occur due to surgical technique and suture materials. Finally, our data did not distinguish between left- and right-sided inguinal hernias. For patients with a surgical recurrence who had 2 prior inguinal hernia repairs, we attributed the recurrence to the hospital where the first primary inguinal hernia was repaired. To the extent that people had 2 inguinal hernias repaired at 2 different hospitals, this error would have falsely attributed the recurrence to the wrong hospital approximately half the time. Since all of these types of misclassification error are nondifferential and would bias our findings toward the null hypothesis of finding no effect of the Shouldice Hospital, it is unlikely that any of these sources of error biased our findings in favour of the results we observed.
Study implications
There are 2 main explanations for our principal findings regarding surgical recurrence. Either surgical care is substantially better at a surgical specialty hospital, or patients at substantially lower risk of recurrence were preferentially selected for surgery. Patients having surgery at the Shouldice Hospital were generally healthier and had a higher household income. There was no evidence that use of local anesthesia at the Shouldice Hospital led to more medically high-risk patients having surgery there. It is possible that the specialty hospital operated on patients with highly favourable hernias, or on minimally detectable hernias on which other surgeons would not operate.31 Our results do not provide support to the hypothesis that patient selection alone can explain the observed results. An estimate of the extent of out-selection is the 10% of patients who had a consultation with a surgeon at the Shouldice Hospital but subsequently had surgery at a general hospital. Only an extraordinarily high recurrence rate among these patients would explain the large effect we observed; the actual recurrence risk of approximately 3% among these patients suggests a very limited effect of patient selection. While our findings suggest that specialty hospitals treat patients with selected and favourable demographic characteristics, we did not find that they preferentially selected patients based on expected treatment outcome. The Shouldice Hospital is unique in that it is not only just a very high-volume specialty surgical hospital, but also the champion of a surgical technique that is rarely used in other hospitals. The favourable results we observed regarding hernia recurrence at the Shouldice Hospital may be associated with surgical volume, surgical technique and processes of care, or with all of these factors.
Our findings raise important questions for future studies. What processes of care explain the striking differences in outcome we observed at the Shouldice Hospital? While it is an extreme outlier in terms of surgical volume, the rate of recurrence after surgery at the specialty hospital was substantially better than that at even the highest volume general hospitals. The importance of factors such as operative technique, patient preparation, postoperative care, or other processes of care are not clear, and better understanding of these issues will determine the extent to which the improved outcomes can be achieved in general hospitals. Finally, if surgical specialty hospitals can achieve substantially better outcomes than general hospitals, does it make sense to encourage more routine surgical care to be provided in these settings? Any potential benefits in clinical outcomes must ultimately be considered in the context of the negative consequences of specialty hospitals, such as maintaining expertise in surgical care at general hospitals and drawing profitable episodes of care away from general hospitals that rely on revenue from elective surgery to subsidize more costly types of hospital care.32
Conclusion
Inguinal hernia repair at a large hernia specialty hospital was associated with a substantially lower risk of subsequent surgery for hernia recurrence than repair at a general hospital. These results could not be explained entirely on the basis of surgical volume, patient selection or confounding factors. While specialty hospitals may have better outcomes for treatment of common surgical conditions than general hospitals, these benefits must be weighed against potential negative impacts on clinical care and the financial sustainability of general hospitals.
Footnotes
This study was supported by the Institute for Clinical Evaluative Sciences (ICES), which is funded by an annual grant from the Ontario Ministry of Health and Long-Term Care (MOHLTC). The opinions, results and conclusions reported in this paper are those of the authors and are independent from the funding sources. No endorsement by ICES or the Ontario MOHLTC is intended or should be inferred. The authors have no conflict of interest related to this research, and have no affiliation with the Shouldice Hospital.
Competing interests: None declared.
Contributors: C. Bell, T. Stukel and D. Urbach designed the study. A. Malik and D. Urbach acquired the data, which all authors analyzed. A. Malik and C. Bell wrote the article, which all authors reviewed and approved for publication.
- Accepted September 18, 2015.