Abstract
Background: In previous studies, 50%–70% of patients referred to orthopedic surgeons for total knee replacement (TKR) were not surgical candidates at the time of initial assessment. The purpose of our study was to identify and cross-validate patient self-reported predictors of suitability for TKR and to determine the clinical utility of a predictive model to guide the timing and appropriateness of referral to a surgeon.
Methods: We assessed pre-consultation patient data as well as the surgeon’s findings and post-consultation recommendations. We used multivariate logistic regression to detect self-reported items that could identify suitable surgical candidates.
Results: Patients’ willingness to undergo surgery, higher rating of pain, greater physical function, previous intra-articular injections and patient age were the factors predictive of patients being offered and electing to undergo TKR.
Conclusion: The application of the model developed in our study would effectively reduce the proportion of nonsurgical referrals by 25%, while identifying the vast majority of surgical candidates (> 90%). Using patient-reported information, we can correctly predict the outcome of specialist consultation for TKR in 70% of cases. To reduce long waits for first consultation with a surgeon, it may be possible to use these items to educate and guide referring clinicians and patients to understand when specialist consultation is the next step in managing the patient with severe osteoarthritis of the knee.
Worldwide estimates indicate that approximately 10%–20% of people older than 60 years have symptomatic osteoarthritis (OA).1 Currently, 4.4 million, or 1 in 8, Canadians are living with OA, and this number is expected to increase to 10.4 million by the year 2040.2 Because of its substantial direct and indirect costs, OA is a growing public health care concern.3,4 The annual economic burden of OA is expected to reach $405 billion by the year 2020 in Canada alone, emphasizing the need to spend health care dollars wisely.2
Total joint replacement (TJR) is an effective intervention for patients with moderate to severe OA in their lower limbs.5 According to the Arthritis Alliance of Canada, TJRs could avert more than 72 000 cases of severe OA over the next 30 years while also improving the symptoms and physical functioning of individuals living with the disease.2 However, provincial and nationwide reports indicate that wait times for Canadians to see an orthopedic surgeon are longer than acceptable.6
Total knee replacement (TKR) accounts for the majority of joint replacement surgeries in Canada,7 therefore targeting a reduction in wait times for TKRs will have the greatest impact in wait time statistics. Despite the growing concern regarding wait times for TKR, current efforts focus on reducing wait times for total joint replacement; there is a limited amount of research that specifically targets improvements in the wait from referral to initial consultation with an orthopedic specialist.8
Interestingly, current evidence suggests that nearly 50%–70% of patients referred to an orthopedic surgeon for TKR are not scheduled for surgery.9,10 In a public health care system, ensuring that patients are seen by the appropriate specialist at the right time is key to ensure efficient allocation of health care resources and timely access to care.
A proposed solution to help mitigate the demand for orthopedic specialist care is to establish central intake and assessment centres (CIACs), where other allied health professionals (physical therapists, nurse practitioners) screen, triage and provide nonoperative care to patients referred for TKR. Although a CIAC may help alleviate excessive wait times for surgical consultations, they may not represent an efficient model of care, given that anecdotally it is reported that most patients referred for TKR eventually undergo surgery and that CIACs mandate an additional costly point of care.11 Ensuring the majority of patients referred to orthopedic specialists for TKR are interested in and eligible candidates for surgery could be achieved through simpler, less costly means than CIACs, such as nonoperative management at the discretion of the family physician and appropriate education for family physicians regarding surgical candidacy.
Thus, the purpose of the present study was to identify the reasons patients are classified as nonsurgical candidates after consultation with an orthopedic surgeon, identify and validate patient-reported predictors of being offered and electing to undergo TKR during the initial consultation, and determine the clinical utility of a predictive model to guide the referral to a surgeon for TKR.
Methods
Study design and setting
This study took place in a clinic that specializes in joint replacement at University Hospital, London Health Sciences Centre, London, Ont., Canada. The centre performs 1700 TKR surgeries per year, which accounts for approximately 3% of all joint replacement surgeries performed annually in Canada.12 This study used a single-centre prospective cohort design conducted with patients who were attending their first consultation for their knee with 1 of 7 fellowship-trained arthroplasty surgeons. Prior to meeting with the surgeon, patients completed a series of questionnaires. Following the consultation, the attending surgeon completed a form detailing their findings and recommendations for treatment. The study was approved by the Health Sciences Research Ethics Board at Western University.
Participants
Patients aged 18–100 years who were referred by their primary health care providers for their first consultation for surgical treatment of knee OA were eligible to participate in this study. Patients were ineligible if they did not speak English; if they were deemed by the orthopedic surgeon to be a complex case; if they were not a new referral; if they had previously undergone a TKR; or if they were unable to complete the questionnaire because of psychiatric, cognitive, visual or physical impairment.
All newly referred patients were identified by the study coordinator before their surgical consultation and were registered into a secure web-based data management system (www.empowerhealthresearch.ca; EmPower Health Research Inc.). Participants were provided a unique username and password that allowed them to login and complete the questionnaires before their appointment. Several studies support the validity of online data collection.13–15 Patients who chose not to complete questions online were provided a paper copy of the questionnaires to complete in the waiting room before meeting with the surgeon.
Outcome measures
We developed a patient demographic and OA questionnaire. The selection and content of the initial patient questionnaires was informed by a thorough literature review followed by a meeting of the participating arthroplasty surgeons who discussed (until consensus) the expected strength of association between collected information and likelihood that patients reporting those characteristics would be scheduled for TKR by the end of the consultation. Because we were interested in identifying items that did not require interference or interpretation by a clinician (in the interest of removing the need for a CIAC), only patient-reported items were included.
Specifically, we included demographic information including age, sex, body mass index (BMI), employment status, presence/absence of bilateral symptoms, previous use of allied health (i.e., physiotherapy, chiropractor, massage therapy), use of intra-articular injections, use of walking aids, and willingness to undergo surgery. Patients indicated their willingness by selecting 1 of 5 response options; a participant was considered “willing” if they selected the response “definitely willing” or “probably willing,” or “unwilling” if they selected the response “unsure,” “probably unwilling,” or “definitely unwilling.”
Patients also completed the Short Form 12-item survey (SF-12)16 and a global rating of knee pain on a numeric scale from 0 to 10, where 0 represents no pain. We also used the Patient Acceptable Symptom State questions (PASS 1 and 2) for OA (in relation to activities of daily living [ADLs], pain and function). The PASS 1 asks, “Taking into account all the activities you have during your daily life, your level of pain, and also your functional impairment, do you consider that your current state is satisfactory?”. The PASS 2 asks, “Considering all the different ways in which your disease affects you, if you were to remain in this state for the next few months, would you consider your current state to be satisfactory?”.17 The response options were yes/no.
After the orthopedic surgeon performed the usual initial consultation with the participant, the surgeon completed a form detailing their findings and recommendations. The surgeons were blind to participant outcome measures, as only the primary data collector retained access to this information. The form asked the surgeon to indicate whether the participant was an appropriate candidate for TKR. If yes, the surgeon indicated whether the consultation resulted in a booking for TKR; if no, the surgeon was asked to indicate the reason(s) via a standard checklist, which was determined a priori by all participating surgeons.
We constructed a simplified algorithm based on model findings and our recommendations for clinicians.
Statistical analysis
Based on the literature and surgeon expertise, we identified 9 items that were most likely to identify surgical candidates: age, BMI, unilateral/bilateral symptoms, willingness to undergo surgery, previous use of allied health, use of injections, use of walking aids, SF-12 Physical Composite Scale (PCS), and global rating of knee pain. We then set out to determine whether we could use patient responses to questionnaire items to identify patients who are scheduled for TKR during their initial consultation (dependent variable).
Our sample size was calculated based on the formula used by Peduzzi and colleagues:18 (n = 10 × k ÷ p), where p was the limiting event rate or the proportion of referrals deemed to be nonsurgical candidates (47%)9 and k was the number of predictors. This yielded a sample size requirement of approximately 200 individuals.
Since our intention was to run both a model development analysis (training sample) and a validation analysis (testing sample) we required approximately 400 individuals randomly divided into 2 equally sized groups. We used an all enter method of multivariate logistic regression analysis where we pared down our model by eliminating any predictors with an α > 0.20 and used the Hosmer–Lemeshow test to confirm the model fit. Model diagnostics were performed following Menard’s method.19
Next, we performed additional analyses with predictors that assessed similar constructs, such as those measuring pain and function. Specifically, we repeated our analysis by replacing global rating of pain and SF-12 PCS with the PASS 1 and PASS 2 questions, respectively, in both the training and validation models.
Last, we identified a final clinical model encompassing terms that were significant in both the training and test models that considered the results of our additional analyses. We calculated the sensitivity and specificity of this model to correctly identify patients booked for TKR following first consult using a standard cut-off value of 0.5. We then adjusted the cut-off value in increments of 0.5 to determine whether we could improve the sensitivity of our model.
All data analyses were performed using SPSS version 22.0 (SPSS Inc.).
Results
Study population
Of the patients who consented to participate, demographic characteristics were similar between those who completed all questionnaires and those who did not. Patients who refused consent tended to be older than those who consented (Table 1).
Patient demographic characteristics
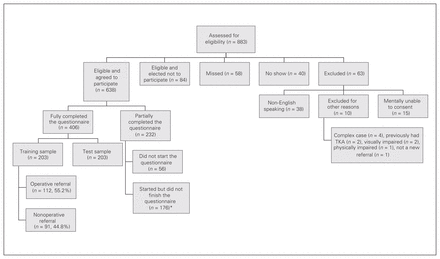
From Apr. 17, 2013, to Feb. 19, 2014, a total of 883 patients were consecutively screened for eligibility. Of these, 63 did not meet eligibility requirements, 40 patients did not attend their appointment, 58 were missed, and 84 refused consent. Of the 638 eligible patients who gave their consent, 406 patients fully completed the study protocol (Fig. 1). Using the American Association for Public Opinion Research (AAPOR) standard,20 our response rate was 72%. Our training and testing samples each comprised 203 patients.
Flow of participants through the study. TKA = total knee arthroplasty
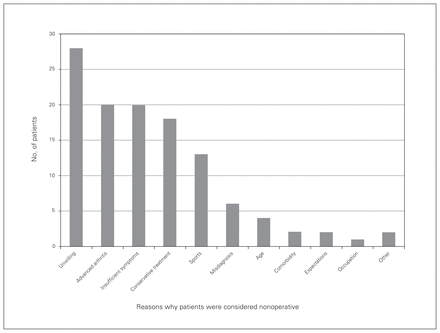
Assumptions of the logistic model were confirmed. Within our training sample, 91 of 203 participants (44.8%) were not scheduled for surgery during the initial consultation with the orthopedic surgeon. Figure 2 describes the reasons why patients were considered nonoperative, as indicated by their surgeon.
Reasons why patients were considered nonoperative, as indicated by their surgeon.
The final training and validation logistic regression models are shown in Table 2. Five variables were identified in the training model as being significant contributors to identifying surgical candidates: age, global rating of pain, SF12 PCS, willingness to undergo surgery, and previous injections. All of these variables were significant in the validation model in addition to BMI, bilateral symptoms and previous use of allied health care. Thus, the original model was validated, as all of the predictors identified as significant in the training model were also significant in the validation model, with odds ratios of similar magnitudes.
Training and validation, final models
We found that willingness to undergo surgery was the strongest predictor of being scheduled for TKR during the initial consultation. In the training sample, patients who were willing to undergo surgery were approximately 4.5 times more likely to be scheduled for TKR (95% confidence interval [CI] 1.64–12.08, p = 0.003). This was further confirmed by the validation sample, in which patients who were willing to undergo surgery were approximately 10 times as likely to be scheduled for TKR (95% CI 3.01–31.71, p < 0.001).
Several other variables were identified as significant predictors in both the training and validation samples. Specifically, the greater the pain reported by the patient, the more likely they were to be scheduled for TKR (i.e., for every 1 unit increase on the 0–10 global rating of pain numeric rating scale, patients were 20% more likely to be scheduled for TKR). The higher a patient scored on the SF-12 (i.e., better function), the less likely they were to be scheduled for TKR. Patients who had tried injections were 1.5 times more likely to be scheduled for TKR than those who had not tried injections. Finally, age was a significant predictor in both models.
Additional analyses
In the training model, when we removed the global rating of pain variable and replaced it with the PASS 1, patients who answered “yes” (i.e., they felt that their current level of pain and functional impairment was acceptable) were approximately 75% less likely to be scheduled for TKR than those who answered “no.” When we replaced the SF-12 PCS with the PASS 2 question, patients who answered “yes” (i.e., they felt that their current disease state was acceptable) were approximately 50% less likely to be scheduled for TKR than those who answered “no.” Results of these additional analyses revealed that the model fit improved in both the training and validation models when PASS 1 (Table 3) and PASS 2 (Table 4) were substituted into the model, whereas the other terms remained relatively stable.
Additional analysis (PASS 1): training and validation, final models
Additional analysis (PASS 2): training and validation, final models
Final clinical model
In formulating the final clinical model, the PASS 2 is preferable based on the clinical utility of a single question versus a 12-item questionnaire. Although the additional analyses evaluated similar constructs with different measures, we cannot compare them directly because they are scaled differently. To avoid collinearity between PASS 1 and PASS 2 statements, it is more suitable to include the global rating of pain in a final predictive model that includes the PASS 2. Thus, our final clinical model includes the following predictor variables: age, willingness to undergo surgery, global rating of pain, PASS 2 and previous injections (Table 5). Cut-off values of 0.5 and 0.35 were used to compute the sensitivity and specificity and overall percentage correct of the final clinical models (training and validation; Table 6). In the training sample, using a cut-off value of 0.5 this model would have correctly screened out 57 of 91 (62%) patients who were not surgical candidates at the time of first consultation, while correctly identifying 87 of 112 (77%) patients scheduled for TKR. Using a cut-off value of 0.35, this model would have correctly screened out 40 of 91 (44%) nonoperative patients, while correctly identifying 104 of 112 (92%) patients scheduled for TKR.
Final clinical models, including the intercept*
Sensitivities and specificities of the final model
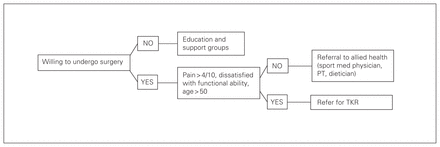
Based on model findings and clinical experience a simplified algorithm for referring physicians is described ( Fig. 3).
Algorithm for patient referral to total knee replacement (TKR). Based on model findings, willingness to undergo surgery should be determined before a referral to TKR is made. Physicians should direct unwilling patients to education and support groups. In patients who are willing to undergo surgery, pain, function and age should be further considered before referral. In patients whose symptoms are mild, referral to allied health may be the most appropriate avenue. Physicians should follow up with these patients regularly to monitor and reassess status for referral to TKR. PT = physiotherapy.
Discussion
We found that a large proportion of referrals for TKR (approximately 45%) were not suitable or “ready” candidates for joint replacement at the time of their initial surgical consultation (i.e., the patient was unwilling to proceed with surgery; lacked advanced OA; was only mildly symptomatic; or had not yet tried or exhausted conservative therapies, such as physical therapy or injections, to manage their OA). The application of the model developed in this study would reduce the proportion of nonsurgical referrals by 25%, while identifying the vast majority of surgical candidates (> 90%). It may be useful for referring physicians to consider the predictors identified in our model when deciding if a referral for TKR is the most appropriate avenue for patients with knee OA. While not every patient referred to an orthopedic surgeon will be a candidate for surgical intervention, improving education for patients and practitioners regarding the timing of referral and conservative options may introduce a more efficient care pathway.
Limitations
A limitation of the present study is that the results may be specific to the study centre and its patient population. Our centre is located within an academic institution and is a high-volume joint-replacement centre whose surgeons operate almost exclusively within their designated specialty. Although there are similar centres in larger urban areas, the rate of referrals that are nonsurgical at their initial consultation may be slightly overestimated in comparison to referrals to an orthopedic surgeon whose practice includes nonsurgical interventions and/or a broader spectrum of diagnoses.
Conclusion
Before making a referral, physicians must ask patients about their willingness to undergo joint replacement surgery. If the patient is unwilling, but meets all other criteria for referral, the physician should investigate reasons for unwillingness (e.g., uncertain about what to expect during the recovery period, lack of support for ADLs during recovery period) and perhaps provide educational material and information about available support groups. Patients who are willing to undergo joint replacement, whose pain is greater than 4/10, who are dissatisfied with their current ability to function, and who are older than 50 years should be referred for TKR.
For patients with mild symptoms, the physician may offer pharmacological pain relief (e.g., acetaminophen, nonsteroidal anti-inflammatory drugs/COX inhibitors) with referrals made to clinicians with expertise in administering intra-articular injections (e.g., sports medicine physicians), physical therapy, nutrition and weight loss (Fig. 3).
Physicians should follow up with the patient regularly to identify changes in pain and function to reassess eligibility and willingness for joint replacement. Finally, physicians should use radiography (bilateral weight-bearing films) as a modifier to decision-making, where patients with severe degenerative changes are more likely to benefit from TKR. Magnetic resonance imaging should not be used to diagnose the degree of degenerative changes or meniscal pathology because it is expensive and provides minimal diagnostic benefit over plain films even in patients with mild to moderate knee OA.
Our study showed that 45% of patients referred to an arthroplasty surgeon are not suitable or “ready” surgical candidates at the time of initial consultation. A patient’s willingness to undergo surgery, previous injections, significant pain, physical disability and older age can correctly predict whether a patient is scheduled for TKR in 70% of referrals. Given long wait times for initial consultation and the potential additional costs to the patient and health care system, joint replacement represents an area where education to optimize referrals may better optimize patient care.
Footnotes
Competing interests: None declared.
Contributors: L. Churchill, S. Malian, B. Chesworth, D. Bryant, S. MacDonald and J. Giffin designed the study. L. Churchill, S. Malian, S. MacDonald and J. Giffin acquired the data, which L. Churchill, S. Malian, B. Chesworth, D. Bryant, J. Marsh and J. Giffin analyzed. L. Churchill, S. Malian, B. Chesworth, D. Bryant, S. MacDonald and J. Giffin wrote the article, which all authors reviewed and approved for publication.
- Accepted July 12, 2016.