Summary
Between September 2014 and December 2015, 32 patients with inguinal hernia were treated using a new 3D mesh in our department. This mesh is characterized by a multilamellar flower-shaped central core with a flat, large-pore polypropylene ovoid disk that has to be implanted preperitoneally. Compared with the traditional Lichtenstein procedure, we observed a shorter mean duration of surgery and a significantly lower mean visual analogue scale (VAS) postoperative pain score recorded immediately after the procedure in the 3D mesh group. The mean VAS score recoded after 4 and 8 postoperative days showed better results in the 3D mesh group than the control group. Moreover, there was reduced postoperative morbidity in the 3D mesh group than the control group, even if no patients experienced severe complications.
The use of a polypropylene mesh during a tension free repair of an inguinal defect represents the standard of care in the majority of centres.1 However, in the last few decades, prosthetic hernia techniques have been implemented through the use of different types of mesh, including those with 3D structures.
A deep fixation of the mesh is well accepted as a cause of many common complications, including chronic pain.2 Owing to these considerations, several types of mesh that eliminate the need for fixation have been produced and studied; one of these is the Freedom ProFlor Inguinal Hernia Implant (Insightra Medical Inc.), a large, porous polypropylene mesh that uses the flexible properties of polypropylene to form an additional multilamellar flower shape similar to a radial spring. This 3D mesh is characterized by a dual system that involves a synthetic and permanent polypropylene implant and a reusable dilation and deployment tool made from plastic tubing. Attached to the central core there is a flat, large-pore polypropylene ovoid disc measuring 8 × 10 cm that has to be implanted preperitoneally into the defect to protect the repair and stabilize the device.3,4
Between September 2014 and December 2015, 32 patients with inguinal hernia were treated using the 3D mesh in our department. A 1:1 ratio retrospective case–control analysis was performed with a control group of patients treated with a traditional large-pore polypropylene mesh during the same period. The description of the study and our results are reported in Appendix 1, available at canjsurg.ca.
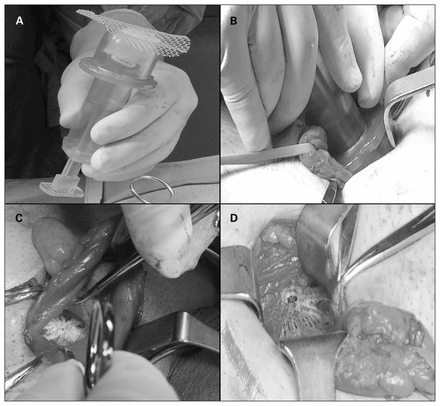
A Lichtenstein technique was used in all controls treated with standard polypropylene mesh. For the 3D mesh, 2 different sizes of central core were used (2.5 cm and 4 cm), depending on the width of the hernia opening. After the opening of the external oblique aponeurosis, the hernia sac was isolated from the spermatic cord. Then a careful and gentle dissection of parietal peritoneum from the posterior abdominal wall was performed using the specific device. In this phase accurate control of the hemostasis is a crucial step to place the mesh safely. The width of dissection has to be appropriate to achieve a preperitoneal free space large enough to allow positioning of the implant’s disc. The mesh was then compressed and loaded into the tube system (Fig. 1A). Subsequently, the tube system was inserted into the hernia defect to release the mesh into the preperitoneal space (Fig. 1B). The tube was then pulled back, taking care that the polypropylene disc remained beyond the posterior abdominal wall.5 After delivery, the flower shape multilamellar core fully obliterated the hernia defect (Fig. 1C–D). In cases of indirect hernia, the mesh was placed from the internal inguinal ring, and the spermatic cord’s structures were not compressed by the lamellas (Fig. 1C). For direct hernias the mesh was directly placed into the preperitoneal space from the hernia opening (Fig. 1D). No stitches were necessary to stabilize the mesh or reduce the hernia opening. Closure of the external oblique fascia was routinely performed using absorbable running sutures. Skin closure was performed with separate intradermal monofilament absorbable stitches.
(A–B) The 3D mesh is inserted in the tube system and placed into the preperitoneal space. (C) For indirect hernias, the mesh is placed into the internal inguinal ring without compression on the spermatic cord. (D) For direct hernias, the mesh is placed directly from the hernia opening.
Even if the use of polypropylene mesh allows the development of a tension-free technique, a high level of postoperative discomfort and chronic pain is still described. Several studies developed a new type of implant to eliminate the necessity of fixation, improving scar tissue formation within the mesh.
Based on these considerations we moved to the use of this new type of mesh, reconsidering our standard technique with the polypropylene implant following the traditional Lichtenstein procedure.
In our experience, the use of this new fixation-free 3D multilamellar mesh substantially reduced the duration of surgery compared with traditional techniques, such as the Lichtenstein procedure. This result should be related to the absence of the fixation phase of the operation. The 3D mesh is placed in the preperitoneal space after the preparation of the layer that is facilitated by using the specific device. In our experience this procedure is easy and short to perform; furthermore, we speculate that the learning curve for this procedure would be short. Despite this report representing our first experience using this 3D mesh, no complications related to the technique were observed, highlighting the safety and feasibility of this procedure.
Our most important result was the substantially lower postoperative pain and discomfort recorded in the 3D mesh group than the Lichtenstein group. This was further confirmed after 4 and 8 postoperative days. These outcomes could be related to the absence of stitches needed to fix the mesh, which can be one of main causes of postoperative patient discomfort. Certainly every preperitoneal mesh is placed far from the nerve, reducing the possible risk of postoperative pain. Nevertheless, owing to its peculiar 3D structure, this type of mesh results in no dislodgement and apparently less or no pain and discomfort. However, the absence of recurrence and chronic pain in both groups shows the efficacy and validity of the traditional technique.
Conclusion
In our initial experience, the use of this new fixation-free 3D multilamellar mesh can be considered a safe and viable option for inguinal hernia repair, resulting in a shorter duration of surgery and substantially less postoperative pain and lower morbidity than traditional polypropylene mesh.
Footnotes
Competing interests: None declared.
Contributors: All authors contributed substantially to the conception, writing and revision of this article and approved the final version for publication.
- Received December 1, 2016.
- Accepted July 12, 2016.