Summary
Studies have shown that a number of women do not receive adjuvant radiation therapy following breast-conserving surgery; the reasons have not been well investigated. We reviewed the charts of 267 patients in our institution who did not receive radiation therapy following surgery in order to determine patient-stated reasons for nonreceipt. We found that 43% of patients did not receive radiation because they received a completion mastectomy. Excluding these patients, reasons for nonreceipt of radiation therapy were sorted into 9 categories. Most patients declined radiation therapy (against physician advice). We identified 3 major barriers to receipt of radiation therapy: improper patient selection, transportation or ambulatory issues and patient fear surrounding radiation toxicity. All of these reasons are surmountable barriers to radiation receipt.
Numerous studies have established that not all women opting for breast-conserving therapy (BCT) for early-stage breast cancer actually receive appropriate adjuvant radiation therapy (RT). Studies have reported rates of RT receipt around 85%, meaning that 15% (or more than 1 in 8) of these women do not receive standard of care treatment.1,2 Such studies have identified patient, disease and environmental factors associated with nonreceipt of RT; however, few have investigated what patients perceive as barriers to RT receipt, and none have investigated this question in a single-payer health care system. Knowledge of factors associated with nonreceipt may help elucidate the problem and could help with patient selection. Specifically, learning about patient-perceived barriers to RT can help clinicians to identify important discussion points and help researchers and policy-makers to address these barriers directly, thereby improving health care delivery.1
We identified a cohort of 1722 consecutive patients in London, Ont., who received breast-conserving surgery (BCS) between 2006 and 2013. Patients were divided into groups based on whether or not they received RT. We reviewed the charts of the 267 patients who did not receive RT. Clinical records were investigated for the patients’ stated reasons for RT nonreceipt. Reasons were collected and sorted into 1 of 10 categories:
Completion mastectomy
Patient declined owing to perceived ability to manage transportation/mobility
Patient declined owing to personal preference
Patient declined without giving a reason
Patient was lost to follow-up
Patient was restaged (metastasis)
No records of RT referral
RT not offered owing to previous RT
RT not offered owing to patient comorbidity, age or frailty
Other
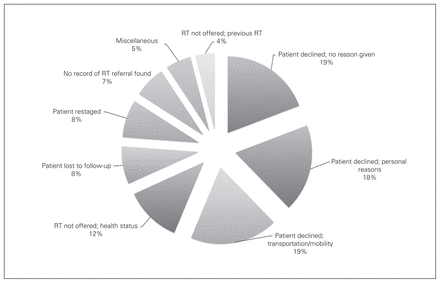
The most common reason that lumpectomy patients did not receive RT was because they received a completion mastectomy (116 patients, or 43% of the total reasons for nonreceipt of RT). Other reasons for nonreceipt of RT are shown in Figure 1.
Proportional representation of reasons for nonreceipt of radiation therapy (RT), as stated in chart notes (completion mastectomy excluded).
Breast-conserving therapy is not recommended in patients with multicentric disease, in those with persistent positive resection margins, in those who have received RT previously, or in patients with a high risk of recurrence (e.g., BRCA positive status).3 The most common reason for RT nonreceipt was because the patient received a completion mastectomy; this describes patients who received BCS then later received a mastectomy. Mastectomy was most commonly performed because patients had positive margins after BCS, because of multicentric disease, or because the patient was found to be BRCA positive. For the majority of these patients, completion mastectomy represents appropriate treatment, although also included here are cases where the need or preference for completion mastectomy should have been predicted.
Of those remaining, 12% of patients were not offered RT because of a coexisting health problem, and 4% were not offered RT because of previous RT receipt. These are BCT contraindications that would have been present at initial consultation and, therefore, represent problems of patient selection, as these women should have received mastectomy initially. Although recent evidence suggests that patients may safely undergo RT for a second time, the data are preliminary, and guidelines have not changed.4 To deliver appropriate care to these patients, treatment should be selected based on medical evidence, rather than patient preference.
The next 3 most common reasons for nonreceipt of RT were nonmedical: the patient declined RT for personal reasons, for reasons of transportation and ambulation, or for no given reason. In total, 8% of patients were lost to follow-up (i.e., the patient did not attend follow-up appointments). We hypothesize that at least a portion of these patients were noncompliant with RT because of the intensive schedule to which they had to adhere, because of an a priori reluctance to undergo radiation, or because of transportation/ambulation-related challenges. These patients may benefit from a hypofractionated schedule of RT or should be offered up-front mastectomy. In cases where patients declined to offer reasons for their refusal of radiation, further interrogation revealed that they were fearful of radiation dosages and risks to healthy tissues.
Thus, 3 major barriers to RT exist: improper patient selection, transportation or ambulatory issues, and patient fear surrounding radiation toxicity. These represent surmountable barriers to appropriate treatment for breast cancer.
Fear of RT has challenged physicians owing to patients’ preconceived notions largely based on inadequate or inaccurate information, and this fear has been described as a barrier to selection of BCT as a treatment modality. This fear can be managed with counselling and patient education at the radiation consultation. The challenge remains ensuring that patients have the opportunity to voice their concerns and have their questions answered by a radiation oncologist.5
The problem of patient selection has been addressed in recent literature suggesting the use of a nomogram to predict a patient’s likelihood of receiving RT and basing treatment decisions on the result.1 Patients unlikely to want or receive RT may benefit from preoperative counselling/education and might then be advised to receive a mastectomy rather than BCT. Transportation and ambulation are difficult barriers to address because physicians cannot directly change these factors. One method that may address this concern is the provision of hypofractionated RT for patients who live at great distances, or who have difficulty with the logistics of attending daily RT for weeks at a time. Intraoperative RT is becoming more common in the United States; it allows patients to forego traditional RT by delivering radiation in a single large dose at the time of surgery. Similar hypofractionation schedules using current external beam technology are being investigated widely. This may provide a solution to barriers presented by transportation and ambulation.
Conclusion
Barriers to RT can be divided into 3 categories: improper patient selection, transportation or ambulatory issues and patient fear regarding radiation toxicity. All of these barriers are potentially surmountable. Patient fear of radiation therapy can be allayed during consultation, patient selection may be improved with the use of nomograms or similar tools recently proposed in the literature, and transportation and ambulation problems may be solved if new hypofractionated treatment modalities prove to be safe and effective.1 By addressing these barriers, we may improve health care delivery to patients with breast cancer.
Footnotes
Competing interests: None declared.
Contributors: All authors contributed substantially to the conception, writing, and revision of this article, and approved the final version for publication.
- Accepted July 17, 2017.